Top videos

Reactive arthritis can affect the heels, toes, fingers, low back, and joints, especially of the knees or ankles. Though it often goes away on its own, reactive arthritis can be prolonged and severe enough to require seeing a specialist. Effective treatment is available for reactive arthritis. Reactive arthritis tends to occur most often in men between ages 20 and 50. Most cases of reactive arthritis appear as a short episode. Occasionally, it becomes chronic. Reactive arthritis is a painful form of inflammatory arthritis (joint disease due to inflammation). It occurs in reaction to an infection by certain bacteria. Most often, these bacteria are in the genitals (Chlamydia trachomatis) or the bowel (Campylobacter, Salmonella, Shigella and Yersinia). Chlamydia most often transmits by sex. It often has no symptoms, but can cause a pus-like or watery discharge from the genitals. The bowel bacteria can cause diarrhea. If you develop arthritis within one month of diarrhea or a genital infection – especially with a discharge – see a health care provider. You may have reactive arthritis. - See more at: http://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Reactive-Arthritis#sthash.VNgDSOOY.dpuf
Here are 10 lifestyle changes you can make to lower your blood pressure and keep it down. Lose extra pounds and watch your waistline. Blood pressure often increases as weight increases. ... Exercise regularly. ... Eat a healthy diet. ... Reduce sodium in your diet. ... Limit the amount of alcohol you drink.

Bartter syndrome has traditionally been classified into three main clinical variants, as follows: Neonatal (or antenatal) Bartter syndrome Classic Bartter syndrome Gitelman syndrome Advances in molecular diagnostics have revealed that Bartter syndrome results from mutations in numerous genes that affect the function of ion channels and transporters that normally mediate transepithelial salt reabsorption in the distal nephron segments. Hundreds of mutations have been identified to date. Such advances may result in the development of new therapies (see the image below). [2] (See Pathophysiology and Etiology.)

TPE removes large-molecular-weight substances such as harmful antibodies from the plasma. It is usually carried out using an automated blood cell separator to ensure fluid balance and maintain a normal plasma volume. This may require the insertion of a femoral or jugular line to allow adequate blood flow. Typically, 30–40 mL/kg of plasma (1–1.5 plasma volumes) are removed at each procedure and replaced with isotonic 4.5 or 5.0% human albumin solution (some services substitute 25–50% of replacement volume with 0.9% saline). Exchange with fresh frozen plasma (FFP) is reserved for the replacement of ADAMTS13 in thrombotic thrombocytopenic purpura (see below) or to replace clotting factors. A one plasma volume exchange removes about 66% of an intravascular constituent and a two plasma volume exchange approximately 85%. TPE is normally combined with disease modifying treatment, such as immunosuppressive drugs, for the underlying condition.
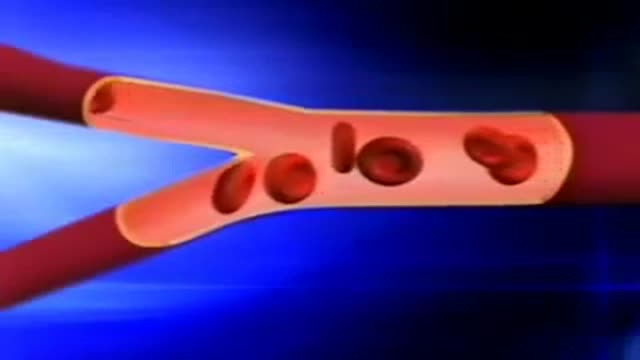
This video: Sickle cell anemia is an inherited form of anemia which is a condition in which there aren't enough healthy red blood cells to carry adequate oxygen throughout your body. Normally, your red blood cells are flexible and round, moving easily through your blood vessels. In sickle cell anemia, the red blood cells become rigid and sticky and are shaped like sickles or crescent moons. These irregularly shaped cells can get stuck in small blood vessels, which can slow or block blood flow and oxygen to parts of the body. There's no cure for most people with sickle cell anemia. However, treatments can relieve pain and help prevent further problems associated with sickle cell anemia.

Sickle cell anemia is an inherited form of anemia: This is a condition in which there aren't enough healthy red blood cells to carry adequate oxygen throughout your body. Normally, your red blood cells are flexible and round, moving easily through your blood vessels. In sickle cell anemia, the red blood cells become rigid and sticky and are shaped like sickles or crescent moons. These irregularly shaped cells can get stuck in small blood vessels, which can slow or block blood flow and oxygen to parts of the body. There's no cure for most people with sickle cell anemia. However, treatments can relieve pain and help prevent further problems associated with sickle cell anemia.
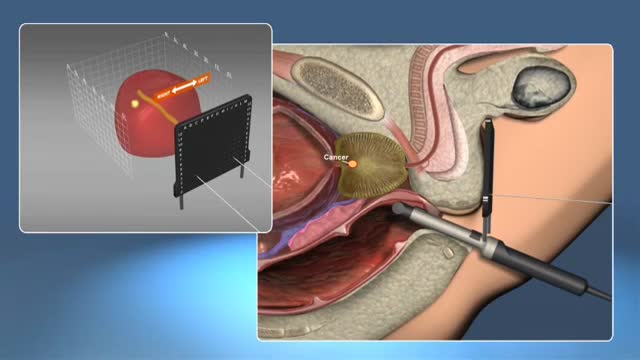
A prostate gland biopsy is a test to remove small samples of prostate tissue to be looked at under a microscope. ... For a prostate biopsy, a thin needle is inserted through the rectum (transrectal biopsy), through the urethra, or through the area between the anus and scrotum (perineum).
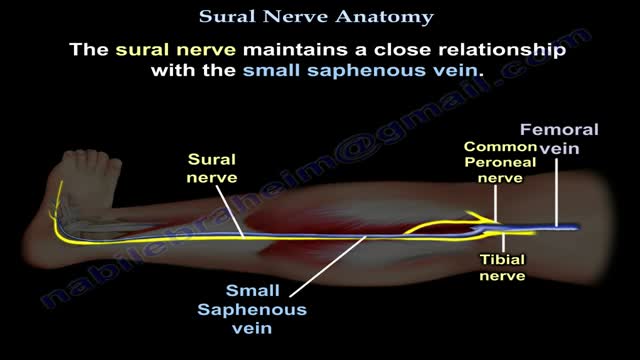
Nerves are the organs that make up the peripheral nervous system (PNS). They serve as information pipelines that allow the brain and spinal cord to communicate with other tissues and organs. Inside the nerves are the axon processes of sensory and motor neurons (nerve cells).

A prenatal ultrasound (also called a sonogram) is a noninvasive diagnostic test that uses sound waves to create a visual image of your baby, placenta, and uterus, as well as other pelvic organs. It allows your healthcare practitioner to gather valuable information about the progress of your pregnancy and your baby's health. During the test, an ultrasound technician (sonographer) transmits high-frequency sound waves through your uterus that bounce off your baby. A computer then translates the echoing sounds into video images that reveal your baby's shape, position, and movements. (Ultrasound waves are also used in the handheld instrument called a Doppler that your practitioner uses during your prenatal visits to listen to your baby's heartbeat.) You may have an early ultrasound at your practitioner's office at 6 to 10 weeks to confirm and date the pregnancy. Or you may not have one until the standard midpregnancy ultrasound between 16 and 20 weeks. That's when you may learn your baby's sex, if you like. (The technician will probably present you with a grainy printout of the sonogram as a keepsake.) You may also have a sonogram as part of a genetic test, such as the nuchal translucency test, chorionic villus sampling, or amniocentesis, or at any other time if there are signs of a problem with your baby. You'll have more frequent ultrasounds if you have diabetes, hypertension, or other medical complications.
The cell membrane is selectively permeable to ions and organic molecules and controls the movement of substances in and out of cells. The basic function of the cell membrane is to protect the cell from its surroundings. It consists of the phospholipid bilayer with embedded proteins.

Three cholinesterase inhibitors are commonly prescribed: Donepezil (Aricept) is approved to treat all stages of Alzheimer's. Rivastigmine (Exelon) is approved to treat mild to moderate Alzheimer's. Galantamine (Razadyne) is approved to treat mild to moderate Alzheimer's. Currently, there is no cure for Alzheimer's. But drug and non-drug treatments may help with both cognitive and behavioral symptoms. Researchers are looking for new treatments to alter the course of the disease and improve the quality of life for people with dementia. ... Medications for Memory Loss.

Superior vena cava syndrome (SVCS) is obstruction of blood flow through the superior vena cava (SVC). It is a medical emergency and most often manifests in patients with a malignant disease process within the thorax. A patient with SVCS requires immediate diagnostic evaluation and therapy.

Wilson's disease is a rare inherited disorder that causes too much copper to accumulate in your liver, brain and other vital organs. Symptoms typically begin between the ages of 12 and 23. Copper plays a key role in the development of healthy nerves, bones, collagen and the skin pigment melanin. Normally, copper is absorbed from your food, and any excess is excreted through bile — a substance produced in your liver.