Top videos
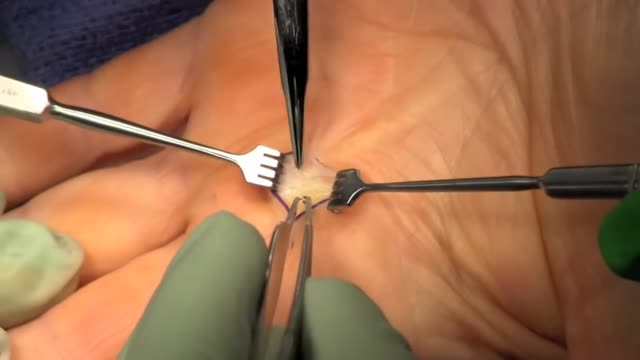
Trigger finger, also known as stenosing tenosynovitis (stuh-NO-sing ten-o-sin-o-VIE-tis), is a condition in which one of your fingers gets stuck in a bent position. Your finger may straighten with a snap — like a trigger being pulled and released. Trigger finger occurs when inflammation narrows the space within the sheath that surrounds the tendon in the affected finger. If trigger finger is severe, your finger may become locked in a bent position. People whose work or hobbies require repetitive gripping actions are at higher risk of developing trigger finger. The condition is also more common in women and in anyone with diabetes. Treatment of trigger finger varies depending on the severity.
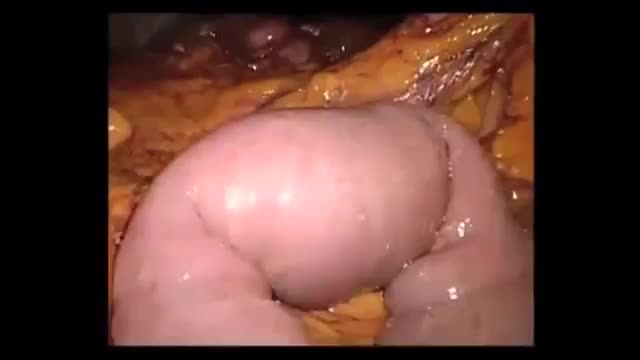
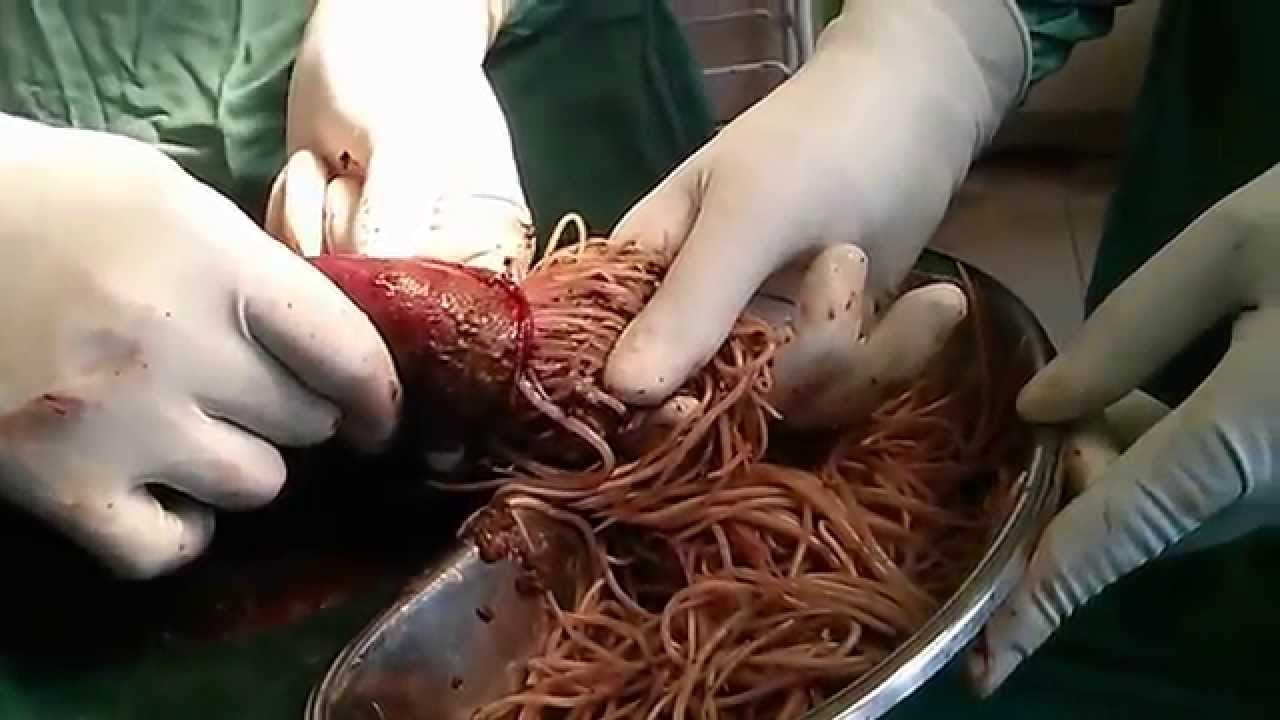
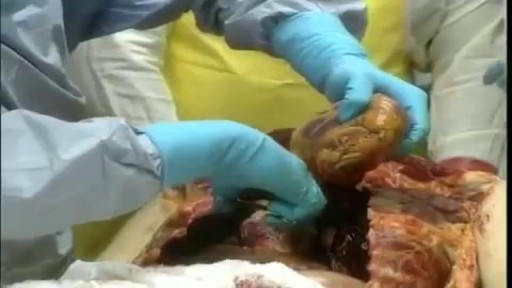
Gallstone ileus is an important, though infrequent, cause of mechanical bowel obstruction, affecting older adult patients who often have other significant medical conditions. It is caused by impaction of a gallstone in the ileum after being passed through a biliary-enteric fistula. The diagnosis is often delayed since symptoms may be intermittent and investigations fail to identify the cause of the obstruction. The mainstay of treatment is removal of the obstructing stone after resuscitating the patient. Gallstone ileus continues to be associated with relatively high rates of morbidity and mortality.
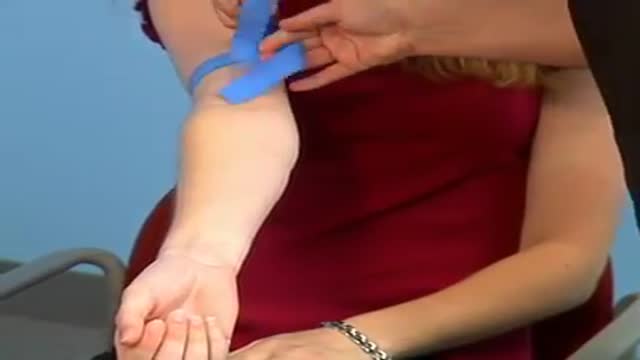
What is Venipuncture? While venipuncture can refer to a variety of procedures, including the insertion of IV tubes into a vein for the direct application of medicine to the blood stream, in phlebotomy venipuncture refers primarily to using a needle to create a blood evacuation point. As a phlebotomist, you must be prepared to perform venipuncture procedures on adults, children, and even infants while maintaining a supportive demeanor and procedural accuracy. Using a variety of blood extraction tools, you must be prepared to respond to numerous complications in order to minimize the risk to the patient while still drawing a clean sample. In its entirety, venipuncture includes every step in a blood draw procedure—from patient identification to puncturing the vein to labeling the sample. Patient information, needle placement, and emotional environment all play a part in the collection of a blood sample, and it's the fine details that can mean the difference between a definite result and a false positive. After placing the tourniquet and finding the vein, it's time for the phlebotomist to make the complex choice on what procedure will best suit the specific situation. Keeping this in mind, it should be noted that the following information is not an instructional guide on how to perform these phlebotomy procedures. Rather, the information below is intended to serve as an educational resource to inform you of the equipment and procedures you will use. Venipuncture Technqiues Venipuncture with an Evacuated or Vacuum Tube: This is the standard procedure for venipuncture testing. Using a needle and sheath system, this procedure allows multiple sample tubes to be filled through a single puncture. This procedure is ideal for reducing trauma to patients. After drawing the blood, the phlebotomist must make sure the test stopper is correctly coded and doesn't contact exposed blood between samples. Venipuncture with a Butterfly Needle : This is a specialized procedure that utilizes a flexible, butterfly needle adaptor. A butterfly needle has two plastic wings (one on either side of the needle) and is connected to a flexible tube, which is then attached to a reservoir for the blood. Due to the small gauge of the needle and the flexibility of the tube, this procedure is used most often in pediatric care, where the patients tend to have smaller veins and are more likely to move around during the procedure. After being inserted into a vein at a shallow angle, the butterfly needle is held in place by the wings, which allow the phlebotomist to grasp the needle very close to the skin. Phlebotomists should be careful to watch for blood clots in the flexible tubing. Venipuncture with a Syringe: This technique is typically only used when there is a supply shortage, or when a technician thinks it is the appropriate method. It uses the classic needle, tube, and plunger system, operating in a similar manner to the vacuum tube but requiring multiple punctures for multiple samples. Additionally, after the blood is drawn it must be transferred to the appropriate vacuum tube for testing purposes. If you choose to use this method, remember to check for a sterile seal, and use a safety device when transferring the sample. Fingerstick (or Fingerprick): This procedure uses a medical lance to make a small incision in the upper capillaries of a patient's finger in order to collect a tiny blood sample. It is typically used to test glucose and insulin levels. When performing a Fingerstick, the phlebotomist should remember to lance the third or fourth finger on the non-dominant arm. Never lance the tip or the center of the finger pad; instead, lance perpendicular to the fingerprint lines. Heelstick (or Heelprick): Similar to the Fingerstick procedure, this process is used on infants under six months of age. A medical lance is used to create a small incision on the side of an infant's heel in order to collect small amounts of blood for screening. As with a Fingerstick, the incision should be made perpendicular to the heel lines, and it should be made far enough to the left or right side of the heel to avoid patient agitation. Before performing a Heelstick, the infant's heel should be warmed to about 42 degrees Celsius in order to stimulate capillary blood and gas flow. Therapeutic Phlebotomy: This involves the actual letting of blood in order to relieve chemical and pressure imbalances within the blood stream. Making use of a butterfly needle, this therapy provides a slow removal of up to one pint of blood. Though the blood removed is not used for blood transfusions, the procedure and concerns are the same as with routine blood donation. As with any phlebotomy procedure, one should pay close attention to the patient in order to prevent a blood overdraw. Bleeding Time: A simple diagnostic test that is used to determine abnormalities in blood clotting and platelet production. A shallow laceration is made, followed by sterile swabbing of the wound every 30 seconds until the bleeding stops. Average bleed times range between one and nine minutes. As a phlebotomist, you should familiarize yourself with the application and cross-application of these procedures in order to recognize when a procedure is necessary, and what the risks are for each.
Purpose: To evaluate the results of LASIK and IntraLASIK treatment in myopic patients with nystagmus. Methods: Eight patients with congenital nystagmus (16 eyes), from 23 to 49 years of age, underwent LASIK surgery. Corneal flaps were created using either the Hansatome microkeratome or the Intral...ase femtosecond laser. The ablations were performed with the Bausch & Lomb excimer laser with an active tracking system. In some patients, the eyes were fixated with forceps or a fixation ring during the laser ablation. Results: The refractive errors were corrected in all cases. There was no decentration or loss of best corrected visual acuity greater than 1 line. In 56% of the eyes, the post-operative uncorrected visual acuity was better than the best spectacle corrected-visual acuity (BSCVA). 62.5% of the eyes improved their BSCVA. The overall visual performance was improved in all the patients. One patient that did not not drive before become eligible to get a driver license after the surgery. Conclusions: Selected patients with myopia and congenital nystagmus may benefit from laser refractive surgery. Laser refractive surgery may be safely and accurately performed by using either the Hansatome microkeratome or the Intralase femtosecond laser and an active tracking system with or without mechanical fixation. Certain patients improve their BSCVA post-operatively.

Mouth ulcers are sores that appear in the mouth, often on the inside of the cheeks. Mouth ulcers, also known as aphthous ulcers, can be painful when eating, drinking or brushing teeth. Occasional mouth ulcers are usually harmless and clear up on their own. Seek medical advice if they last longer than 3 weeks or keep coming back. Mouth ulcers cannot be caught from someone else. Up to 1 in 5 people get recurrent mouth ulcers.

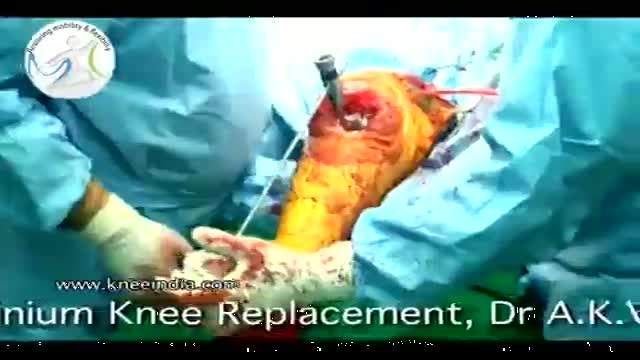
plantar fasciitis and calcaneal spur can be treated by EPFR with calcanean drilling - endoscopic plantar fascia release علاج الشوكة العظمية للكعب بالمنظار د. أسامة الشاذلي مدرس جراحة العظام واستشاري جراحات و مناظير القدم والكاحل كلية الطب جامعة عين شمس

When diving into a Breast Reduction procedure, there are many things to consider. Even as a patient, being aware of any concerns and how the procedure works is important. Therefore, when a plastic surgeon operates on a patient, the results are clear. Dr. Linder, a Breast surgeon specialist in Beverly Hills, helps explain what goes into a Breast Reduction Procedure.

complications from using a urinary catheter include: allergic reaction to the material used in the catheter, such as latex. bladder stones. blood in the urine. injury to the urethra. kidney damage (with long-term indwelling catheters) septicemia, or infection of the urinary tract, kidneys, or blood.

Mysterious massage from East Asia(CHINA).it can cure cure Erectile dysfunction,can let their life better.This video from mainland of China,so the language is Chinese mandarin.but you can see English show on the video too.Tiedang gong means kongfu of Iron penis&balls.
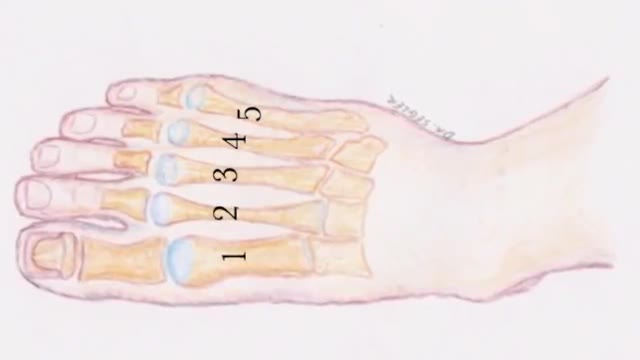
A stress fracture typically feels like an aching or burning localized pain somewhere along a bone. Usually, it will hurt to press on it, and the pain will get progressively worse as you run on it, eventually hurting while walking or even when you're not putting any weight on it at all.
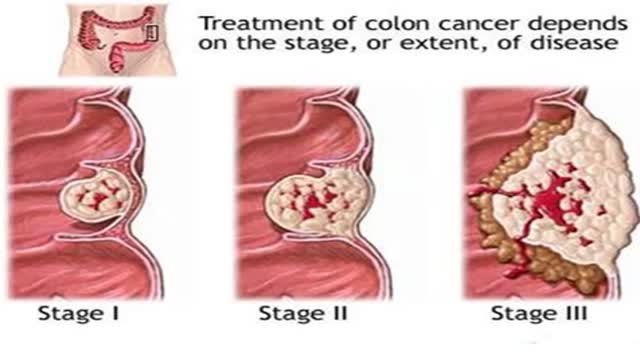
Signs and symptoms of colon cancer include: A change in your bowel habits, including diarrhea or constipation or a change in the consistency of your stool, that lasts longer than four weeks Rectal bleeding or blood in your stool Persistent abdominal discomfort, such as cramps, gas or pain A feeling that your bowel doesn't empty completely Weakness or fatigue Unexplained weight loss Many people with colon cancer experience no symptoms in the early stages of the disease. When symptoms appear, they'll likely vary, depending on the cancer's size and location in your large intestine.