Top videos
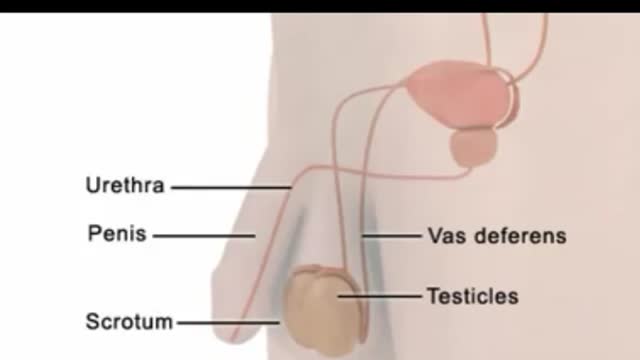
An egg cannot be fertilized when there are no sperm in the semen. The testicles continue to produce sperm, but the sperm are reabsorbed by the body. (This also happens to sperm that are not ejaculated after a while, regardless of whether you have had a vasectomy.) Sperm are made in the testicles. They pass through two tubes called the vasa deferentia to other glands and mix with seminal fluids to form semen. Vasectomy blocks each vas deferens and keeps sperm out of the seminal fluid. The sperm are absorbed by the body instead of being ejaculated.
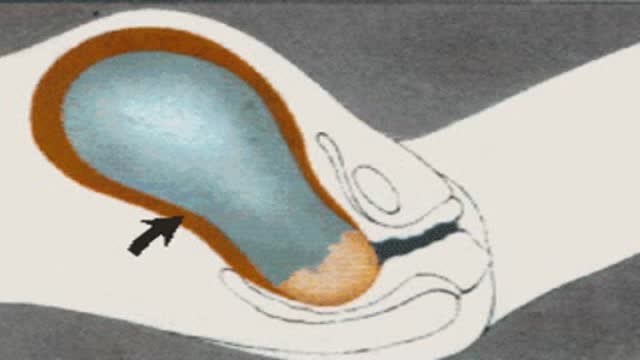
Childbirth (also called labour, birth, partus or parturition) is the culmination of a human pregnancy or gestation period with birth of one or more newborn infants from a woman’s uterus. The process of normal human childbirth is categorized in three stages of labour: the shortening and dilation of the cervix, descent and birth of the infant, and birth of the placenta. In some cases, childbirth is achieved through caesarean section, the removal of the neonate through a surgical incision in the abdomen, rather than through vaginal birth

Tongue and lip-tie are common causes of nipple pain, uneven breast drainage, slow weight gain and low milk supply. Many physicians do not properly assess for tongue or lip-tie or recognize their impact on the breastfeeding relationship, leaving babies vulnerable to early weaning. Ultrasound studies have shown that the tongue movements used by tongue-tied babies are qualitatively different from those used by by babies who are not tongue-tied. These movements are not as effective at removing milk from the breast and can cause significant pain and nipple damage. In these studies, tongue-tied babies also did not draw the nipple as deeply into the mouth as babies who were not tongue-tied.

Symptoms of liver failure include vomiting, diarrhea and fatigue as well as the symptoms from stage 3. While the progression from cirrhosis to failure can take years, the damage is irreversible and leads to eventual death. The key to treating liver disease is to diagnose the condition as early as possible.

Healthcare providers are in the best position to assess for domestic violence, yet have obstacles to doing so. See the benefits to moving beyond these obstacles for those you serve. And discover an accurate, convenient and confidential way to assess for domestic abuse.
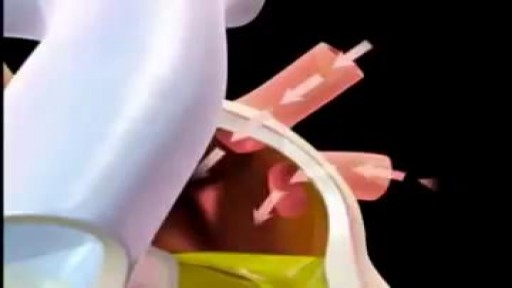
The cardiac cycle is the sequence of events that occurs when the heart beats. As the heart beats, it circulates blood through pulmonary and systemic circuits of the body. There are two phases of the cardiac cycle. In the diastole phase, the heart ventricles are relaxed and the heart fills with blood

Vaginal prolapse (also called vaginal vault prolapse) is quite common after a hysterectomy (surgery to remove the uterus), but not everyone who has a hysterectomy experiences POP. Without the uterine attachments to hold it up, the top of the vagina can drop into the vaginal canal.
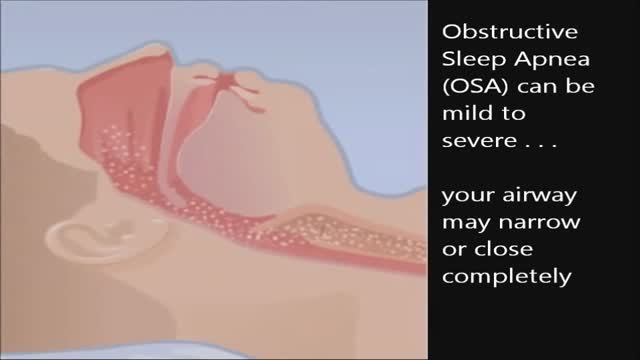
CPAP, or continuous positive airway pressure, is a treatment that uses mild air pressure to keep the airways open. CPAP typically is used by people who have breathing problems, such as sleep apnea. CPAP also may be used to treat preterm infants whose lungs have not fully developed.
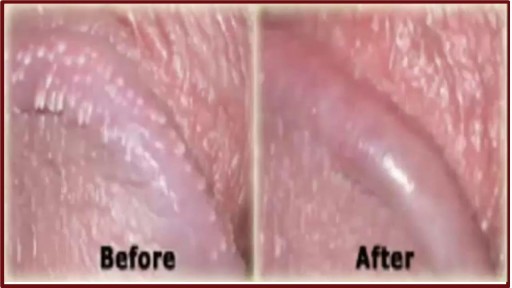
http://penilepapules.plus101.com/ ----- White Spots On Shaft, Pearly Penile Papules Treatment Cream, Single Red Bump On Shaft, Ppp Surgery. Common Home Made Remedies for Pearly Penile Papules. When it comes to treating pearly penile papules many people find it very difficult to reach one of the medical treatments. This is mainly because they are highly expensive and not many people can afford spending large amounts of money on surgery and recovery. In addition to that, these procedures have been reported as being quite risky, which make the men suffering from pearly penile papules think twice before going for one of the available surgeries. This is why, along the time, many homemade, natural treatments have been experienced, so that a cheaper and less risky way of curing pearly penile papules would be found. Some of the methods which have been tried proved to be very less effective, while some did not have any effect at all. Yet, there have also been methods which not only proved to be effective, but they were also considered to be much better than the medical treatment. Most of those who have tried the tea tree oil treatment reported significant diminish of the number of the papules from their penises. In addition to the clearing of the skin, they have also noticed that there were no side effects and the skin remained soft after the papules were removed. As the method was quite simple to put in practice (it requires the application of tea tree oil on the affected area with a cotton swab for three or four times per day), many men decided this was indeed a great solution to their problem.

Lupus is an autoimmune disease that can affect almost any part of your body, most often your joints, skin, kidneys, heart, lungs, blood, or brain. Your two kidneys are part of your renal system, which also includes two ureters, the bladder, and the urethra. As the primary organs of the renal system, your kidneys are responsible for: Maintaining the correct amount and type of body fluids Removing waste products and toxic substances Regulating the hormones (chemical messengers) that help control blood pressure and blood volume