Top videos
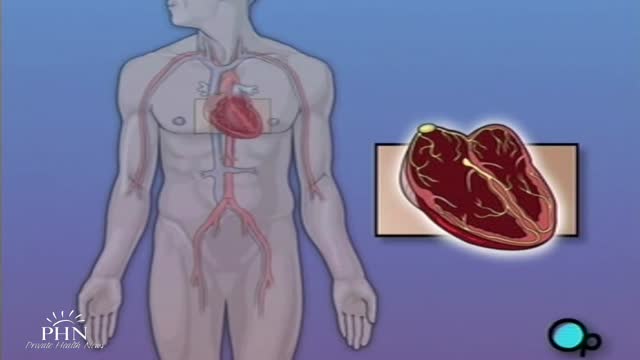
Permanent pacemaker insertion is considered a minimally invasive procedure. Transvenous access to the heart chambers under local anesthesia is the favored technique, most commonly via the subclavian vein, the cephalic vein, or (rarely) the internal jugular vein or the femoral vein.

An intra-aortic balloon pump (IABP) is a mechanical device that helps the heart pump blood. This device is inserted into the aorta, the body's largest artery. It is a long, thin tube called a catheter with a balloon on the end of it. If you are hospitalized, your doctor may insert an IABP.
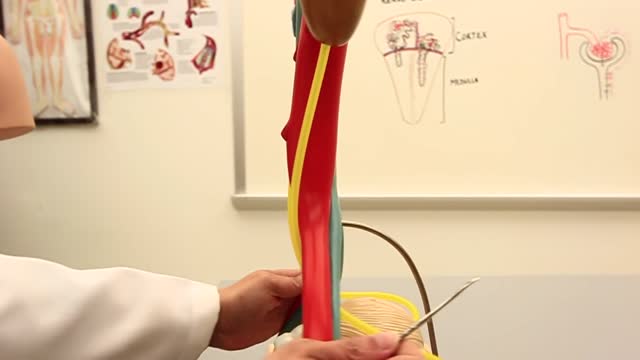
Pelvic ureter. The ureter enters the pelvis, where it crosses anteriorly to the iliac vessels, which usually occurs at the bifurcation of the common iliac artery into the internal and external iliac arteries. Here, the ureters are within 5 cm of one another before they diverge laterally.

Breast lumps facts Breast lumps can be caused by infections, injuries, non-cancerous growths, and cancer. Breast cancer usually causes no pain in the breast. The symptoms of breast cancer include painless breast lumps, nipple discharge, and inflammation of the skin of the breast. The chances that a particular breast lump could be cancerous depends on many factors, including past medical history, physical examination, as well as genetic and other risk factors. The only way to be certain that a lump is not cancerous is to have a tissue sampling (biopsy). There are several ways to do the biopsy. The treatment of a breast lump depends on its cause.

Come Si Può Rimanere Incinta, Rimanere Incinta A 42 Anni Naturalmente, Settimane Di Gravidanza--- http://come-rimanere-incinta.info-pro.co --- Come rimanere incinta in modo naturale La sterilità può essere generalmente definita come l'incapacità di avere una gravidanza dopo aver provato per almeno un anno senza l'uso di contraccettivi. Nei paesi occidentali la sterilità colpisce circa il 15% della popolazione. Mentre c'è chi cerca di concepire con metodi alternativi come la fecondazione in vitro, altri preferiscono ottimizzare le probabilità di rimanere incinta naturalmente. Cercare di rimanere incinta naturalmente può essere molto importante dal momento che molte coppie o individui con diagnosi di sterilità possono tornare ad essere fertili senza trattamenti (e quindi si dovrebbe parlare di "sub-fertilità" piuttosto che di "sterilità"). Quando si cerca di rimanere incinta naturalmente, il fattore più importante è capire il ciclo mestruale e la tempistica di ovulazione, che porta ad ottimizzare le possibilità di ottenere una gravidanza. Di solito l'ovulazione avviene intorno al quattordicesimo giorno e, di conseguenza, per ottenere una gravidanza naturale la coppia dovrebbe avere più rapporti sessuali possibili tra il dodicesimo e il quindicesimo giorno. Ogni donna ha un ciclo leggermente diverso. Per cui, per migliorare le probabilità di rimanere incinta, è indispensabile studiare i propri cicli e calcolare con esattezza quando si ovula. L'antico Sistema Olistico Cinese In 5-passi Per Rimanere Incita Naturalmente E Avere Bimbi Sani Clicca sul link http://come-rimanere-incinta.info-pro.co

The cat's stomach is a sac-like structure designed to store large volumes of food and continue the digestive process. The esophagus carries food to the stomach, where it enters via a valve-like structure called the cardiac sphincter. On the interior surface of the stomach is a series of folds called gastric folds. These folds function to help grind and digest food. The inner stomach lining secretes acids and enzymes to break down food. Once the initial stomach digestive process is complete, the partially digested food exits the stomach through the pyloric sphincter area and then enters the duodenum (first segment of the small intestine). Once eaten, most food leaves the stomach within twelve hours after entering.
There is nothing that compares to the fresh-faced feeling you have when you leave the aesthetician after a facial. There is just something so freeing about knowing that nasty little buggers like blackheads, whiteheads and all other kinds of heads have been given the heave-ho. That could be why this Facebook video of a blackhead being removed has gone viral. With more than 24 million views, the popular video is weirdly difficult to stop watching.
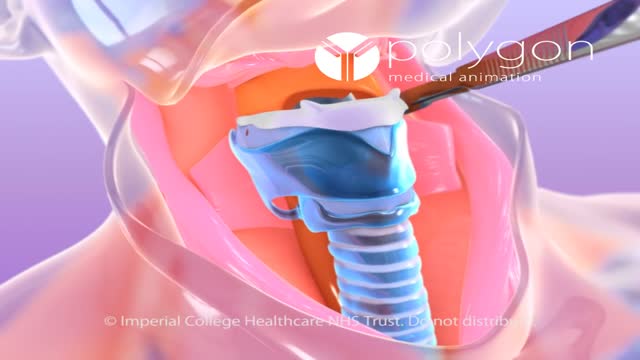
Laryngectomy is the removal of the larynx and separation of the airway from the mouth, nose and esophagus. In a total laryngectomy the entire larynx is removed and in a partial laryngectomy only a portion is taken out. The laryngectomee breathes through an opening in the neck known as a stoma.
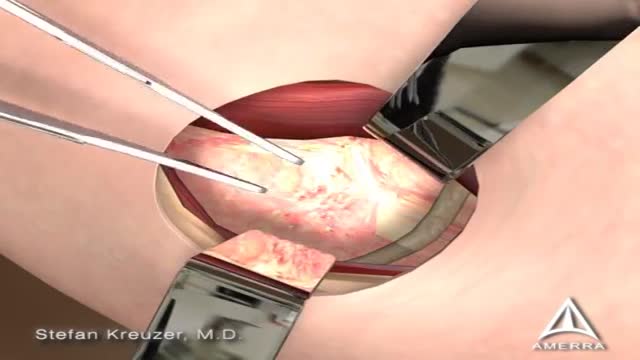
Femoroacetabular impingement (FAI) is a condition in which extra bone grows along one or both of the bones that form the hip joint — giving the bones an irregular shape. Because they do not fit together perfectly, the bones rub against each other during movement. Over time this friction can damage the joint, causing pain and limiting activity.

Blood clotting, or coagulation, is an important process that prevents excessive bleeding when a blood vessel is injured. Platelets (a type of blood cell) and proteins in your plasma (the liquid part of blood) work together to stop the bleeding by forming a clot over the injury.

You may have a lot of questions about epilepsy. We will help you understand the basics, answer the most common questions, and help you find resources and other information you may need. However, information alone won’t help you manage your epilepsy and find a way to cope with the effects on your daily life. You’ll need to learn how to use the information and make it work for you.

Rheum is made up of mucus, skin cells, oils and dust. The rheum that comes from the eyes and forms eye boogers is called gound, which you may know as eye sand, eye gunk, sleep dust, sleep sand, sleep in your eyes, or eye shnooters. When you're awake, gound doesn't cause any problems.
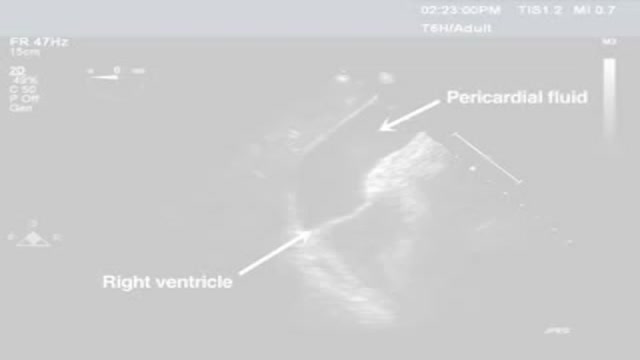
Pericardiocentesis is the aspiration of fluid from the pericardial space that surrounds the heart. This procedure can be life saving in patients with cardiac tamponade, even when it complicates acute type A aortic dissection and when cardiothoracic surgery is not available. [1] Cardiac tamponade is a time sensitive, life-threatening condition that requires prompt diagnosis and management. Historically, the diagnosis of cardiac tamponade has been based on clinical findings. Claude Beck, a cardiovascular surgeon, described 2 triads of clinical findings that he found associated with acute and chronic cardiac tamponade. The first of these triads consisted of hypotension, an increased venous pressure, and a quiet heart. It has come to be recognized as Beck's triad, a collection of findings most commonly produced by acute intrapericardial hemorrhage. Subsequent studies have shown that these classic findings are observed in only a minority of patients with cardiac tamponade. [2] The detection of pericardial fluid has been facilitated by the development and continued improvement of echocardiography. [3] Cardiac ultrasound is now accepted as the criterion standard imaging modality for the assessment of pericardial effusions and the dynamic findings consistent with cardiac tamponade. With echocardiography, the location of the effusion can be identified, the size can be estimated (small, medium, or large), and the hemodynamic effects can be examined by assessing for abnormal septal motion, right atrial or right ventricular inversion, and decreased respiratory variation of the diameter of the inferior vena cava.
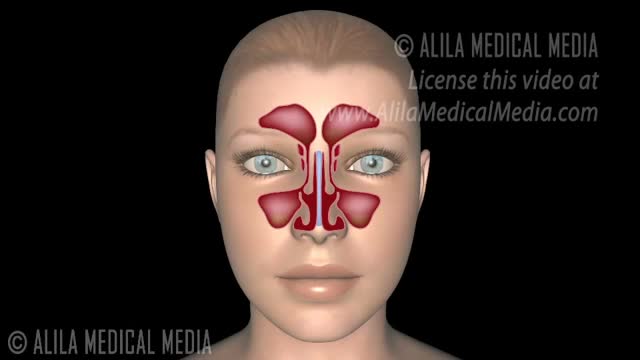
Sinusitis means your sinuses are inflamed. The cause can be an infection or another problem. Your sinuses are hollow air spaces within the bones surrounding the nose. They produce mucus, which drains into the nose. If your nose is swollen, this can block the sinuses and cause pain. There are several types of sinusitis, including Acute, which lasts up to 4 weeks Subacute, which lasts 4 to 12 weeks Chronic, which lasts more than 12 weeks and can continue for months or even years Recurrent, with several attacks within a year Acute sinusitis often starts as a cold, which then turns into a bacterial infection. Allergies, nasal problems, and certain diseases can also cause acute and chronic sinusitis. Symptoms of sinusitis can include fever, weakness, fatigue, cough, and congestion. There may also be mucus drainage in the back of the throat, called postnasal drip. Your health care professional diagnoses sinusitis based on your symptoms and an examination of your nose and face. You may also need imaging tests. Treatments include antibiotics, decongestants, and pain relievers. Using heat pads on the inflamed area, saline nasal sprays, and vaporizers can also help.
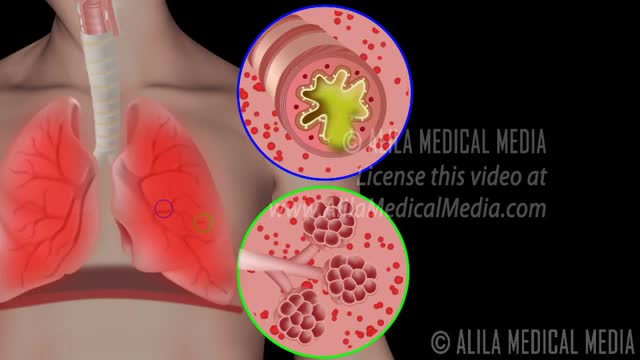
Chronic obstructive pulmonary disease Email this page to a friend Print Facebook Twitter Google+ Chronic obstructive pulmonary disease (COPD) is a common lung disease. Having COPD makes it hard to breathe. There are two main forms of COPD: Chronic bronchitis, which involves a long-term cough with mucus Emphysema, which involves damage to the lungs over time Most people with COPD have a combination of both conditions. Causes Smoking is the main cause of COPD. The more a person smokes, the more likely that person will develop COPD. But some people smoke for years and never get COPD. In rare cases, nonsmokers who lack a protein called alpha-1 antitrypsin can develop emphysema. Emphysema Other risk factors for COPD are: Exposure to certain gases or fumes in the workplace Exposure to heavy amounts of secondhand smoke and pollution Frequent use of a cooking fire without proper ventilation Symptoms Symptoms may include any of the following: Cough, with or without mucous Fatigue Many respiratory infections Shortness of breath (dyspnea) that gets worse with mild activity Trouble catching one's breath Wheezing Because the symptoms develop slowly, some people may not know that they have COPD.