Top videos

Rheum is made up of mucus, skin cells, oils and dust. The rheum that comes from the eyes and forms eye boogers is called gound, which you may know as eye sand, eye gunk, sleep dust, sleep sand, sleep in your eyes, or eye shnooters. When you're awake, gound doesn't cause any problems.
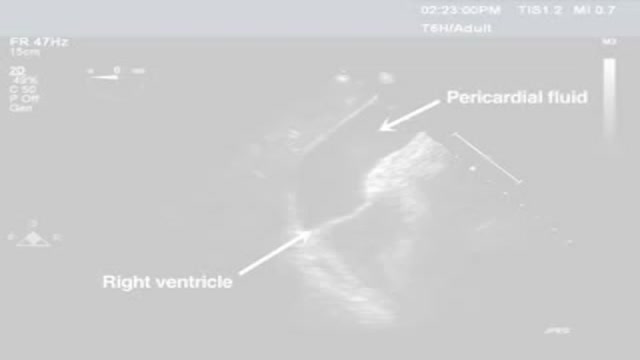
Pericardiocentesis is the aspiration of fluid from the pericardial space that surrounds the heart. This procedure can be life saving in patients with cardiac tamponade, even when it complicates acute type A aortic dissection and when cardiothoracic surgery is not available. [1] Cardiac tamponade is a time sensitive, life-threatening condition that requires prompt diagnosis and management. Historically, the diagnosis of cardiac tamponade has been based on clinical findings. Claude Beck, a cardiovascular surgeon, described 2 triads of clinical findings that he found associated with acute and chronic cardiac tamponade. The first of these triads consisted of hypotension, an increased venous pressure, and a quiet heart. It has come to be recognized as Beck's triad, a collection of findings most commonly produced by acute intrapericardial hemorrhage. Subsequent studies have shown that these classic findings are observed in only a minority of patients with cardiac tamponade. [2] The detection of pericardial fluid has been facilitated by the development and continued improvement of echocardiography. [3] Cardiac ultrasound is now accepted as the criterion standard imaging modality for the assessment of pericardial effusions and the dynamic findings consistent with cardiac tamponade. With echocardiography, the location of the effusion can be identified, the size can be estimated (small, medium, or large), and the hemodynamic effects can be examined by assessing for abnormal septal motion, right atrial or right ventricular inversion, and decreased respiratory variation of the diameter of the inferior vena cava.
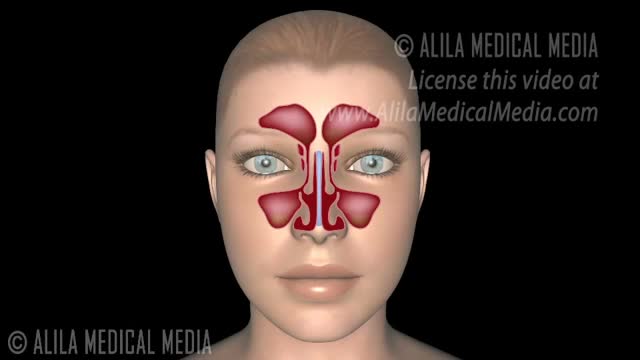
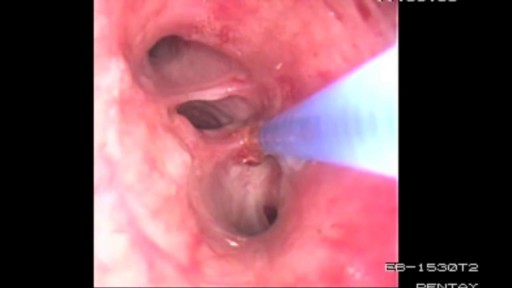
Sinusitis means your sinuses are inflamed. The cause can be an infection or another problem. Your sinuses are hollow air spaces within the bones surrounding the nose. They produce mucus, which drains into the nose. If your nose is swollen, this can block the sinuses and cause pain. There are several types of sinusitis, including Acute, which lasts up to 4 weeks Subacute, which lasts 4 to 12 weeks Chronic, which lasts more than 12 weeks and can continue for months or even years Recurrent, with several attacks within a year Acute sinusitis often starts as a cold, which then turns into a bacterial infection. Allergies, nasal problems, and certain diseases can also cause acute and chronic sinusitis. Symptoms of sinusitis can include fever, weakness, fatigue, cough, and congestion. There may also be mucus drainage in the back of the throat, called postnasal drip. Your health care professional diagnoses sinusitis based on your symptoms and an examination of your nose and face. You may also need imaging tests. Treatments include antibiotics, decongestants, and pain relievers. Using heat pads on the inflamed area, saline nasal sprays, and vaporizers can also help.
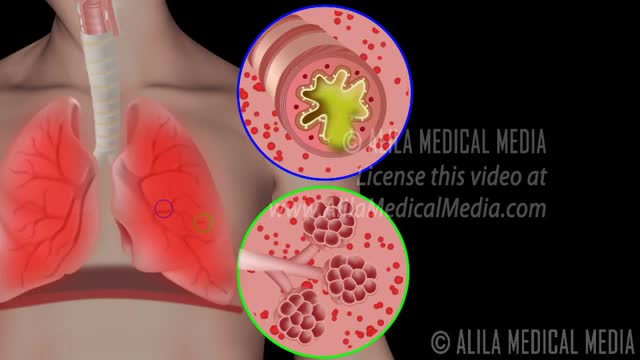
Chronic obstructive pulmonary disease Email this page to a friend Print Facebook Twitter Google+ Chronic obstructive pulmonary disease (COPD) is a common lung disease. Having COPD makes it hard to breathe. There are two main forms of COPD: Chronic bronchitis, which involves a long-term cough with mucus Emphysema, which involves damage to the lungs over time Most people with COPD have a combination of both conditions. Causes Smoking is the main cause of COPD. The more a person smokes, the more likely that person will develop COPD. But some people smoke for years and never get COPD. In rare cases, nonsmokers who lack a protein called alpha-1 antitrypsin can develop emphysema. Emphysema Other risk factors for COPD are: Exposure to certain gases or fumes in the workplace Exposure to heavy amounts of secondhand smoke and pollution Frequent use of a cooking fire without proper ventilation Symptoms Symptoms may include any of the following: Cough, with or without mucous Fatigue Many respiratory infections Shortness of breath (dyspnea) that gets worse with mild activity Trouble catching one's breath Wheezing Because the symptoms develop slowly, some people may not know that they have COPD.
Surgery to replace an aortic valve is done for aortic valve stenosis and aortic valve regurgitation. During this surgery, the damaged valve is removed and replaced with an artificial valve. The valve replacement is typically an open-heart surgery.
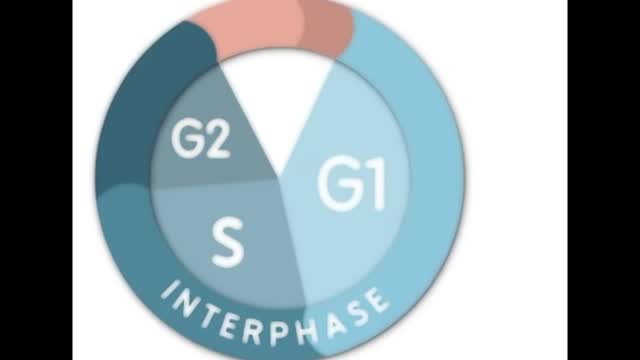
Mitosis is the process in which a eukaryotic cell nucleus splits in two, followed by division of the parent cell into two daughter cells. The word "mitosis" means "threads," and it refers to the threadlike appearance of chromosomes as the cell prepares to divide.

Antiphospholipid (AN-te-fos-fo-LIP-id) syndrome occurs when your immune system attacks some of the normal proteins in your blood. It can cause blood clots in your arteries or veins. And it can cause pregnancy complications, such as miscarriage and stillbirth. Blood clots in your leg veins cause a condition known as deep vein thrombosis (DVT). Damage from blood clots in your organs, such as your kidneys, lungs or brain, depends on the extent and location of the clot. For instance, a clot in your brain can cause a stroke. There's no cure for antiphospholipid syndrome, but medications can reduce your risk of blood clots.

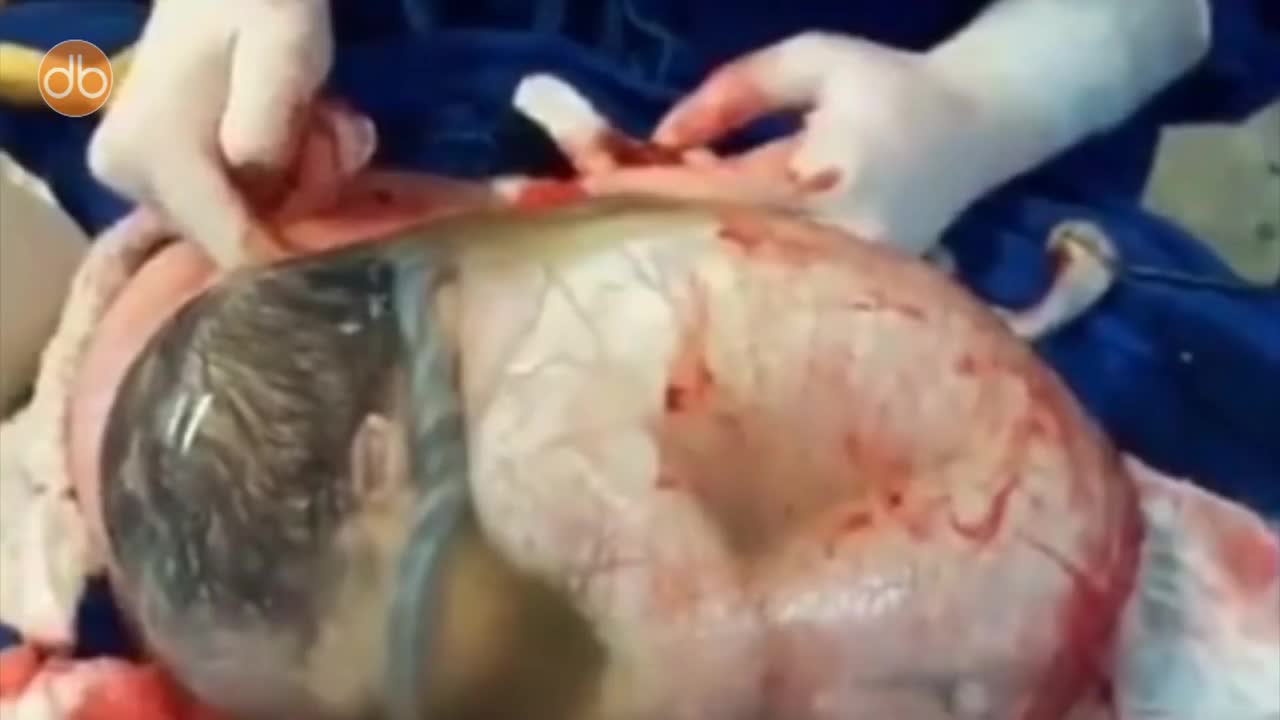
Are you a first time would be mom? If yes, then you must be very excited to feel the first movement and kick from your baby. It is undoubtedly the most exciting experience for many expecting moms. It is an indication that there is a little angel growing inside you. There are interesting facts about baby kicks during pregnancy that you need to know.

When a stroke affects an extensive portion of the front and back regions of the left hemisphere, the result may be global aphasia. Survivors with global aphasia: May have great difficulty in understanding words and sentences. May have great difficulty in forming words and sentences. May understand some words. Get out a few words at a time. Have severe difficulties that prevent them from effectively communicating.
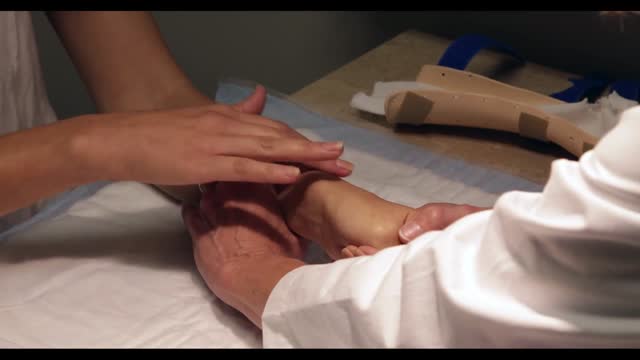
De Quervain's tenosynovitis (dih-kwer-VAINS ten-oh-sine-oh-VIE-tis) is a painful condition affecting the tendons on the thumb side of your wrist. If you have de Quervain's tenosynovitis, it will probably hurt when you turn your wrist, grasp anything or make a fist. Although the exact cause of de Quervain's tenosynovitis isn't known, any activity that relies on repetitive hand or wrist movement — such as working in the garden, playing golf or racket sports, or lifting your baby — can make it worse. Symptoms ShareTweet June 13, 2015 References Products and Services Mayo Clinic Sports Medicine Newsletter: Mayo Clinic Health Letter See also Prednisone risks, benefits Prednisone withdrawal: Why taper down slowly? Integrative approaches to treating pain Lifestyle strategies for pain management Nutrition and pain Pain rehabilitation Self-care approaches to treating pain Show more Advertisement Mayo Clinic does not endorse companies or products. Advertising revenue supports our not-for-profit mission. Advertising & Sponsorship PolicyOpportunitiesAd Choices Mayo Clinic Store Check out these best-sellers and special offers on books and newsletters from Mayo Clinic. NEW! – The Mayo Clinic Diet, Second Edition Healthy Heart for Life! Mayo Clinic on Better Hearing and Balance Treatment Strategies for Arthritis The Mayo Clinic Diet Online

Knee replacement involves replacing a knee joint that has been damaged or worn away, usually by arthritis or injury. Find out more here: http://bit.ly/MAdfmE
The content is intended for general information only and does not replace the need for personal advice from a qualified health professional.
Syringomyelia is a cystic cavitation of the spinal cord associated with Chiari I malformation (70%) or basilar invagination (10%) or tumor. It may be a post-traumatic condition. There are 2 main forms: communicating with the central canal or subarachnoid spaces (Chiari I malformation); non communicating (trauma, tumors).
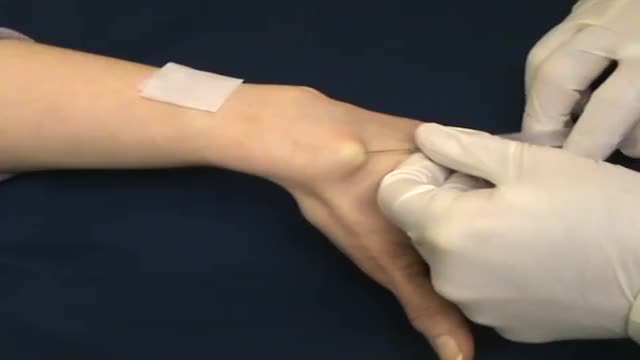
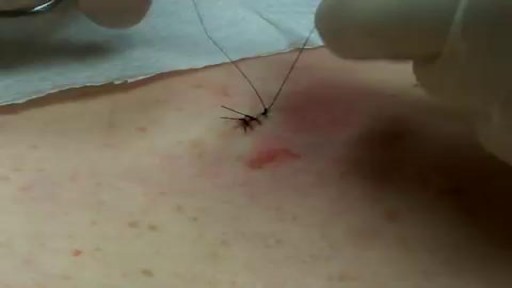
A nonsurgical method of treating a ganglion is to drain the fluid from (aspirate) the ganglion sac. Your doctor can do this in the office using the following procedure: The ganglion area is cleaned with an antiseptic solution. A local anesthetic is injected into the ganglion area to numb the area. When the area is numb, the ganglion sac is punctured with a sterile needle. The fluid is drawn out of the ganglion sac. The ganglion collapses. A bandage and, in some cases, a splint are used for a few days to limit movement and prevent the ganglion sac from filling again. Treating a ganglion by draining the fluid with a needle may not work because the ganglion sac remains intact and can fill again, causing the ganglion to return. For this reason, your doctor may puncture the sac with the needle 3 or 4 times so the sac will collapse completely. Even then, the ganglion is likely to come back.