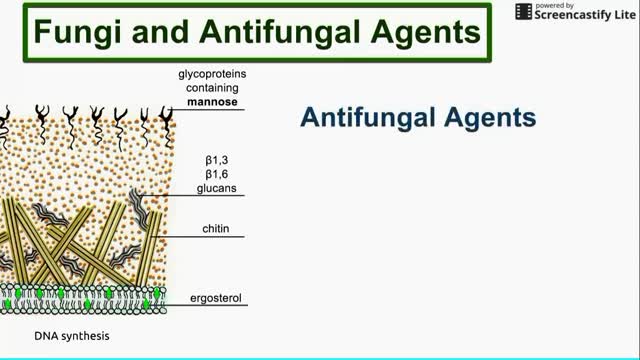
Top videos
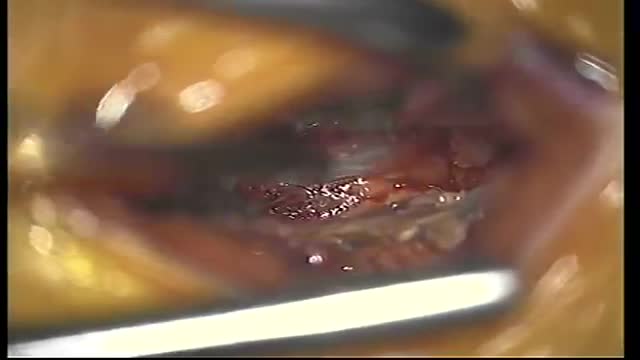
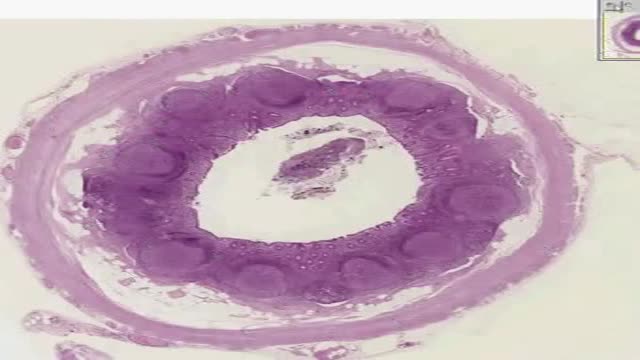
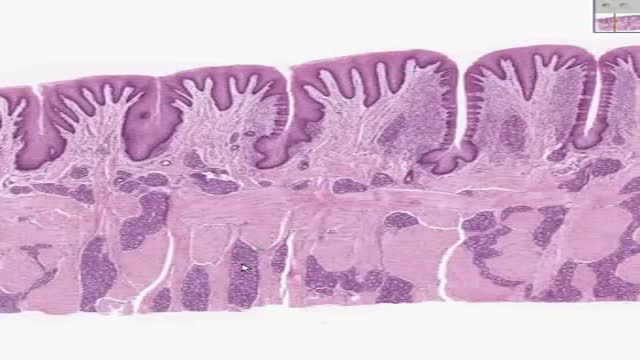
An epidural abscess is a collection of pus (infected material) between the outer covering of the brain and spinal cord and the bones of the skull or spine. The abscess causes swelling in the area. Spinal cord abscess (SCA) is a rare condition capable of causing permanent damage to the spinal cord. Abscesses are caused when injured tissue becomes infected. The body's immune system sends white blood cells to help fight off the infection. They begin to fill the damaged tissue, causing pus to build up.
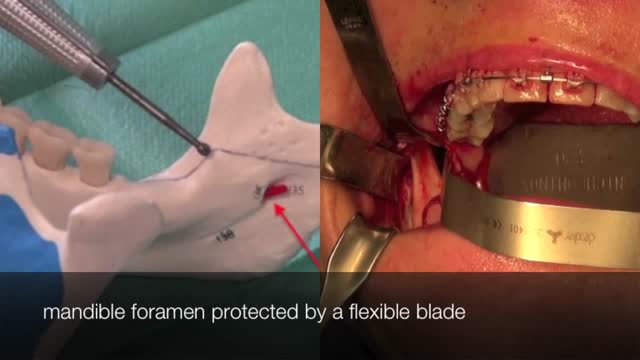
The bilateral sagittal split osteotomy is an indispensable tool in the correction of dentofacial abnormalities. The technique has been in practice since the late 1800s, but did not reach widespread acceptance and use until several modifications were described in the 1960s and 1970s. Those modifications came from a desire to make the procedure safer, more reliable, and more predictable with less relapse. Those goals continue to stimulate innovation in the field today and have helped the procedure evolve to be a very dependable, consistent method of correction of many types of malocclusion. The operative surgeon should be well versed in the history, anatomy, technical aspects, and complications of the bilateral sagittal split osteotomy to fully understand the procedure and to counsel the patient.

Live TV is so exciting because anything can happen, and sometimes that means injuries. Today I'm reacting to injuries and medical emergencies that happened on live tv. We're talking America's Got Talent, American Idol, newscasters having strokes, dehydration, Wendy Williams overheating, swallowing swords, being hit with a motorcycle, vasovagal syncope, drowning, Dan Harris, and magical tricks like David Blaine's needle in going wrong. Which clips did I miss? Let me know down below.
I LOVE reading your comments and take your suggestions seriously. If there’s a subject you want me to discuss or something you’d like for me to react to, leave a comment down below. Many of my videos have been born out of suggestions directly from you, so don’t hold back!
-Doctor Mike Varshavski
Help us continue the fight against medical misinformation and change the world through charity by becoming a Doctor Mike Resident on Patreon where every month I donate 100% of the proceeds to the charity, organization, or cause of your choice! Residents get access to bonus content, an exclusive discord community, and many other perks for just $10 a month. Become a Resident today:
https://www.patreon.com/doctormike
Please SUBSCRIBE for new videos every Wednesday afternoon and Sunday morning! https://goo.gl/87kYq6
Let’s connect:
IG https://goo.gl/41ZS7w - Doctor Mike
Reddit https://www.reddit.com/r/DoctorMike/
Twitter https://goo.gl/kzmGs5 - Real Doctor Mike
Facebook https://goo.gl/QH4nJS - Real Doctor Mike
Contact Email: DoctorMikeMedia@Gmail.com
* Select photos/videos provided by Getty Images *
** The information in this video is not intended nor implied to be a substitute for professional medical advice, diagnosis or treatment. All content, including text, graphics, images, and information, contained in this video is for general information purposes only and does not replace a consultation with your own doctor/health professional **

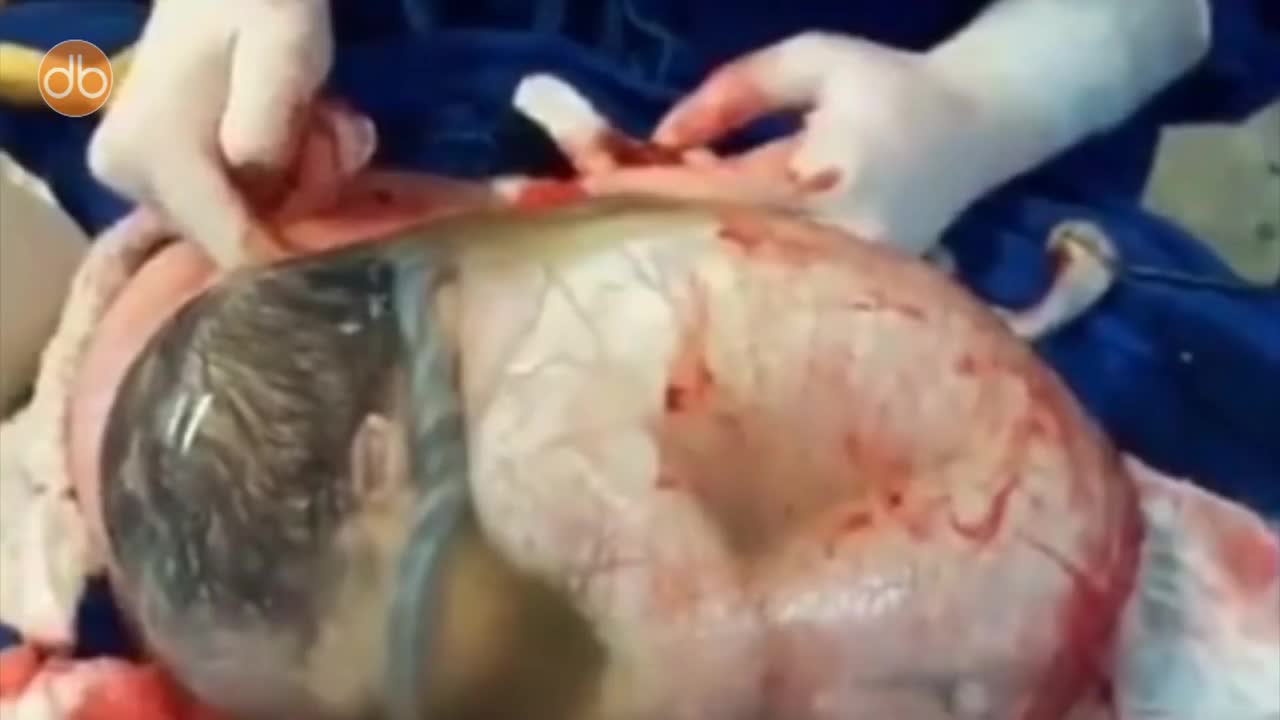
Are you a first time would be mom? If yes, then you must be very excited to feel the first movement and kick from your baby. It is undoubtedly the most exciting experience for many expecting moms. It is an indication that there is a little angel growing inside you. There are interesting facts about baby kicks during pregnancy that you need to know.

When a stroke affects an extensive portion of the front and back regions of the left hemisphere, the result may be global aphasia. Survivors with global aphasia: May have great difficulty in understanding words and sentences. May have great difficulty in forming words and sentences. May understand some words. Get out a few words at a time. Have severe difficulties that prevent them from effectively communicating.
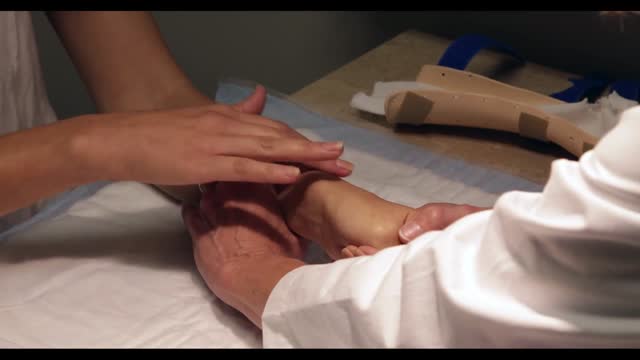
De Quervain's tenosynovitis (dih-kwer-VAINS ten-oh-sine-oh-VIE-tis) is a painful condition affecting the tendons on the thumb side of your wrist. If you have de Quervain's tenosynovitis, it will probably hurt when you turn your wrist, grasp anything or make a fist. Although the exact cause of de Quervain's tenosynovitis isn't known, any activity that relies on repetitive hand or wrist movement — such as working in the garden, playing golf or racket sports, or lifting your baby — can make it worse. Symptoms ShareTweet June 13, 2015 References Products and Services Mayo Clinic Sports Medicine Newsletter: Mayo Clinic Health Letter See also Prednisone risks, benefits Prednisone withdrawal: Why taper down slowly? Integrative approaches to treating pain Lifestyle strategies for pain management Nutrition and pain Pain rehabilitation Self-care approaches to treating pain Show more Advertisement Mayo Clinic does not endorse companies or products. Advertising revenue supports our not-for-profit mission. Advertising & Sponsorship PolicyOpportunitiesAd Choices Mayo Clinic Store Check out these best-sellers and special offers on books and newsletters from Mayo Clinic. NEW! – The Mayo Clinic Diet, Second Edition Healthy Heart for Life! Mayo Clinic on Better Hearing and Balance Treatment Strategies for Arthritis The Mayo Clinic Diet Online

Ellis Parker MSN, RN-BC, CNE, CHSE covers Incentive Spirometry. The Critical Nursing Skills - Shorts series is intended to help RN and PN nursing students study for nursing school exams, including the ATI, HESI and NCLEX.
#NCLEX #HESI #Kaplan #ATI #NursingSchool #NursingStudent #Nurse #RN #PN #Education #LVN #LPN #clinicalskills #safety
Comments? Suggestions? Please share! Your feedback can help inform our future videos and study resources. 🙂
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our flashcards are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of 5-star reviews from nurses who passed their exams and the NCLEX with Level Up RN.
Our #Clinical Nursing Skills Flashcards are available at
➡️ https://bit.ly/clinicalnursingskills
👇SHOP ALL OUR FLASHCARDS👇
http://bit.ly/allstudycards
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://www.leveluprn.com/signup ⬅️
Want perks? Join our channel!
➡️ https://www.youtube.com/leveluprn/join ⬅️
👩⚕️ LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.
👋 STAY CONNECTED 👋
TikTok: https://tiktok.com/@leveluprn
Instagram: https://www.instagram.com/leveluprn/
Facebook: https://fb.me/LevelUpRN
Pinterest: https://www.pinterest.com/leveluprn/
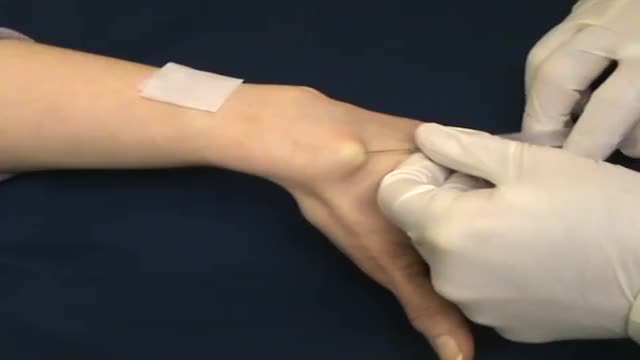
A nonsurgical method of treating a ganglion is to drain the fluid from (aspirate) the ganglion sac. Your doctor can do this in the office using the following procedure: The ganglion area is cleaned with an antiseptic solution. A local anesthetic is injected into the ganglion area to numb the area. When the area is numb, the ganglion sac is punctured with a sterile needle. The fluid is drawn out of the ganglion sac. The ganglion collapses. A bandage and, in some cases, a splint are used for a few days to limit movement and prevent the ganglion sac from filling again. Treating a ganglion by draining the fluid with a needle may not work because the ganglion sac remains intact and can fill again, causing the ganglion to return. For this reason, your doctor may puncture the sac with the needle 3 or 4 times so the sac will collapse completely. Even then, the ganglion is likely to come back.

How To Help Your Child Learn To Read, Help My Child Learn To Read, Best Way To Teach Reading---- http://children-learning-reading.good-info.co -- how to help your child learn to read - Help My Child Learn to Read The ability to read is vital for success. It helps your child succeed in school, helps them build self-confidence, and helps to motivate your child. Being able to read will help your child learn more about the world, understand directions on signs and posters, allow them to find reading as an entertainment, and help them gather information. Learning to read is very different from learning to speak, and it does not happen all at once. There is a steady progression in the development of reading ability over time. The best time for children to start learning to read is at a very young age - even before they enter pre-school. Once a child is able to speak, they can begin developing basic reading skills. Very young children have a natural curiosity to learn about everything, and they are naturally intrigued by the printed texts they see, and are eager to learn about the sounds made by those letters. You will likely notice that your young child likes to look at books and thoroughly enjoys being read to. They will even pretend to behave like a reader by holding books and pretend to read them. As parents, you're the most important first step in your children's journey into the wonderful world of reading. It is up to you to create the most supportive environment that turns your child on to reading - such as reading aloud to them often during the day and before bedtime, and placing age appropriate books for children around the house, so that the child will have access to plenty of books. Reading often to your child will help develop their interest in books and stories, and soon they will want to read stories on their own. >>Teach your child to read and enable your child to become a fast and fluent reader! Click here to help your child learn to read http://children-learning-reading.good-info.co