Top videos
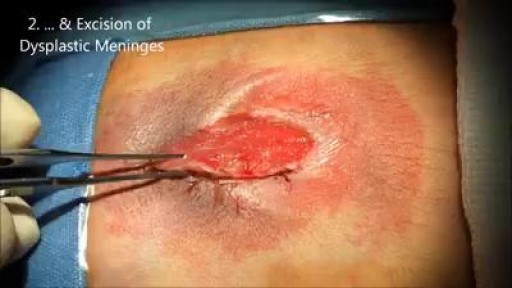
Myelomeningocele remains the most complex congenital malformation of the central nervous system that is compatible with life. This lesion results when the neural tube fails to fold normally during postovulatory Days 21 to 27.[6] The exact cause of disorders remains under some historical debate and is not within the scope of this paper. Myelomeningocele within the context of this discussion refers only to lesions that involve an open caudal neural tube defect on the surface of the skin
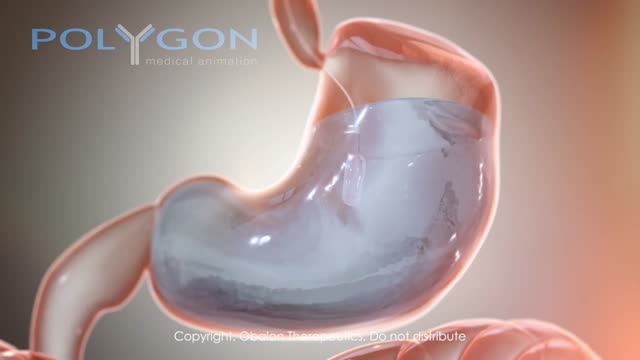
The gastric balloon procedure (endoscopic intragastric balloon) leaves an inflated silicon balloon in the stomach for 6 months, making less room for food. As a result, patients: Feel full sooner while eating and therefore eat less. Lose about 30% of their excess weight in 6 months.
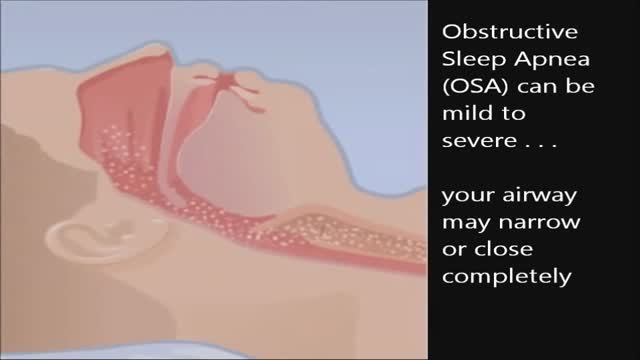
CPAP, or continuous positive airway pressure, is a treatment that uses mild air pressure to keep the airways open. CPAP typically is used by people who have breathing problems, such as sleep apnea. CPAP also may be used to treat preterm infants whose lungs have not fully developed.
Generic minoxidil is known to treat hair-fall issues in men and women, it is best for hair growth, hair re-development, etc. it is available in the strength of 5mg and easily available at online pharmacy store. For more information visit to http://www.medstorerx.com/generic-minoxidil.aspx
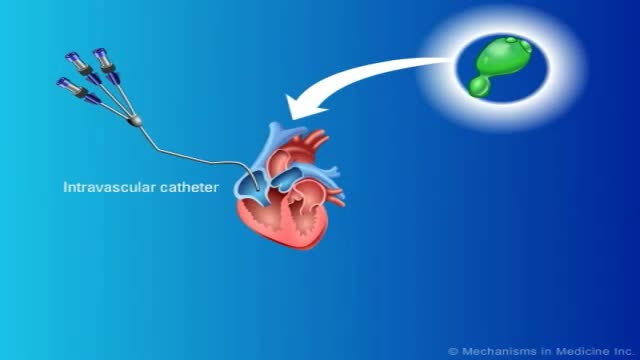
Fungal infections in bone marrow transplant patients. PURPOSE OF REVIEW: Invasive fungal infections have become the leading infectious cause of death in recipients of hematopoietic cell transplantation. Several factors have led to a renaissance in the study of invasive fungal infections.
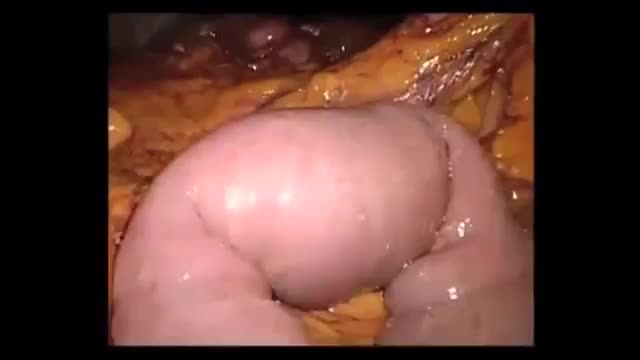
Gallstone ileus is an important, though infrequent, cause of mechanical bowel obstruction, affecting older adult patients who often have other significant medical conditions. It is caused by impaction of a gallstone in the ileum after being passed through a biliary-enteric fistula. The diagnosis is often delayed since symptoms may be intermittent and investigations fail to identify the cause of the obstruction. The mainstay of treatment is removal of the obstructing stone after resuscitating the patient. Gallstone ileus continues to be associated with relatively high rates of morbidity and mortality.
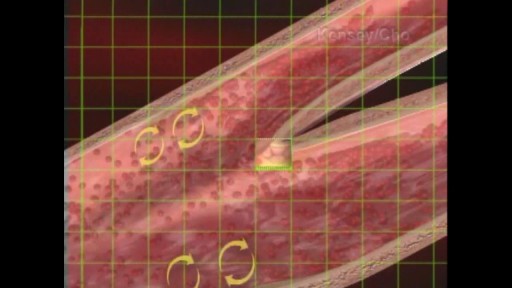
When the hematocrit rises to 60 or 70%, which it often does in polycythemia, the blood viscosity can become as great as 10 times that of water, and its flow through blood vessels is greatly retarded because of increased resistance to flow. This will lead to decreased oxygen delivery.
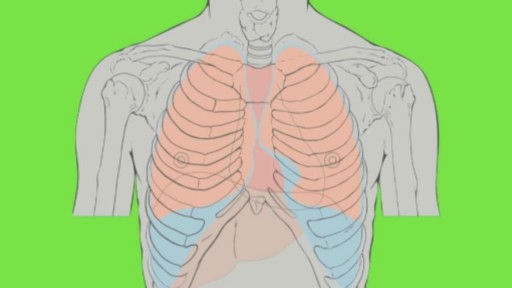
Pulmonary edema is usually caused by a heart condition. Other causes include pneumonia, exposure to certain toxins and drugs, and being at high elevations. Depending on the cause, pulmonary edema symptoms may appear suddenly or develop over time. Mild to extreme breathing difficulty can occur. Cough, chest pain, and fatigue are other symptoms. Treatment generally includes supplemental oxygen and medications.
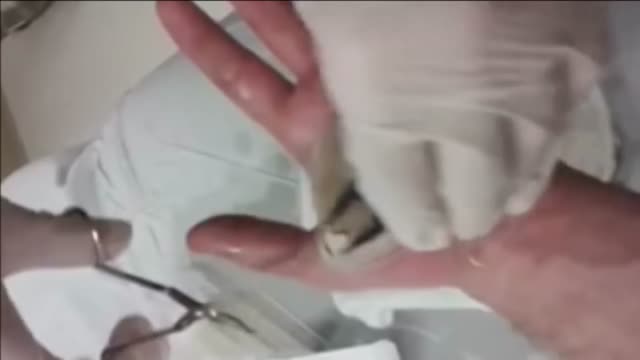
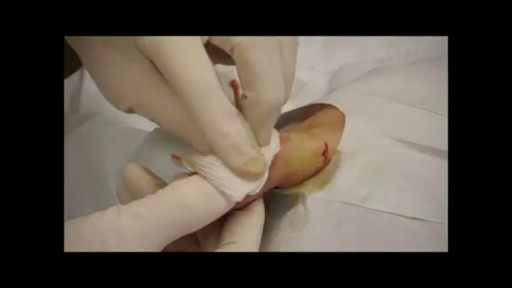
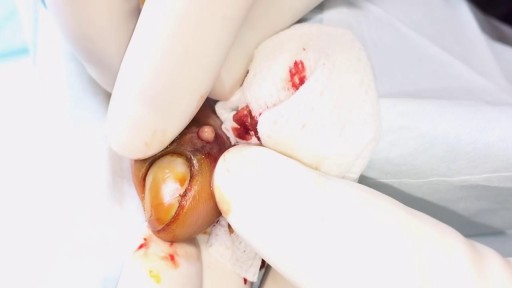
This video: Blisters caused by friction or minor burns do not require a doctor's care. New skin will form underneath the affected area and the fluid is simply absorbed. Do not puncture a blister unless it is large, painful, or likely to be further irritated. The fluid-filled blister keeps the underlying skin clean, which prevents infection and promotes healing.

The Epley maneuver is a series of movements, normally carried out on a person by a doctor, to relieve the symptoms of BPPV. Research has found it to be an easy, safe, and effective treatment for the condition in both the long- and short-term. The Epley maneuver is sometimes called the particle repositioning maneuver or the canalith repositioning maneuver. These names are used because the maneuver involves a series of movements that help to reposition crystals in a person's ear that may cause feelings of dizziness. Repositioning the crystals helps to relieve the person's dizziness and nausea.

Acromegaly is usually caused by a noncancerous tumor. Middle-aged adults are most commonly affected. Symptoms include enlargement of the face, hands, and feet. Prompt treatment is needed to avoid serious illness. Drugs can reduce the effects of growth hormone. If needed, surgery and radiation may be used to remove tumor cells.