Top videos

Work out the length of your average menstrual cycle. Day one is the first day of the menstrual period and the last day is the day before the next period begins. Ovulation happens about two weeks before the next expected period. So if your average menstrual cycle is 28 days, you ovulate around day 14.
This could be caused by an infection, food poisoning, parasites, Crohn's disease, or reduced blood flow in the colon. Hemorrhoids are another common cause of GI or rectal bleeding. A hemorrhoid is an enlarged vein in your rectum or anus. These enlarged veins can rupture and bleed, causing rectal bleeding.
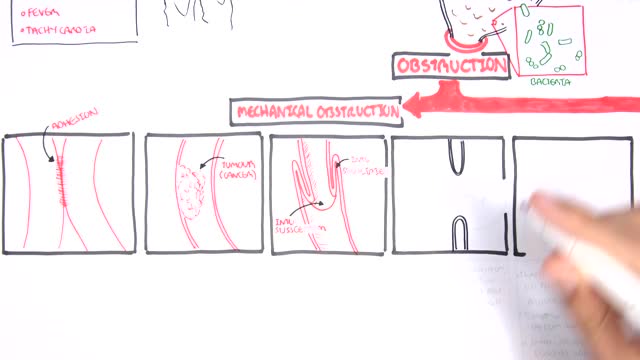
A bowel obstruction happens when either your small or large intestine is partly or completely blocked. The blockage prevents food, fluids, and gas from moving through the intestines in the normal way. The blockage may cause severe pain that comes and goes. This topic covers a blockage caused by tumors, scar tissue, or twisting or narrowing of the intestines. It does not cover ileus, which most commonly happens after surgery on the belly (abdominal surgery). What causes a bowel obstruction? Tumors, scar tissue (adhesions), or twisting or narrowing of the intestines can cause a bowel obstruction. These are called mechanical obstructions . In the small intestine, scar tissue is most often the cause. Other causes include hernias and Crohn's disease, which can twist or narrow the intestine, and tumors, which can block the intestine. A blockage also can happen if one part of the intestine folds like a telescope into another part, which is called intussusception.

Controlled studies on treatment of catscratch disease (CSD) are lacking. Thus, treatment recommendations are based on case reports, reviews, a single controlled trial, and anecdotal data. Practice guidelines for the diagnosis and management of skin and soft-tissue infections, including CSD, have been established.Oct 19, 2016
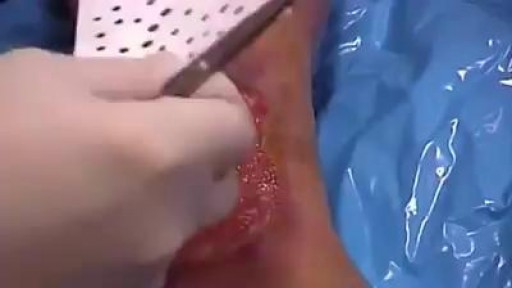
irregular, curved toenails. footwear that places a lot of pressure on the big toes, such as socks and stockings that are too tight or shoes that are too tight, narrow, or flat for your feet. toenail injury, including stubbing your toe, dropping something heavy on your foot, or kicking a ball repeatedly. poor posture. How can ingrowing toenails be prevented? Cut your nails straight across; do not cut them too short or too low at the sides. ... Keep your feet clean and dry. ... Avoid tight shoes and use cotton socks rather than synthetic. If you have diabetes, you should take extra care when cutting your nails:

Diabetes is a growing global health concern, as is obesity. Diabetes and obesity are intrinsically linked: obesity increases the risk of diabetes and also contributes to disease progression and cardiovascular disease. Although the benefits of weight loss in the prevention of diabetes and as a critical component of managing the condition are well established, weight reduction remains challenging for individuals with type 2 diabetes due to a host of metabolic and psychological factors. For many patients, lifestyle intervention is not enough to achieve weight loss, and alternative options, such as pharmacotherapy, need to be considered. However, many traditional glucose-lowering medications may lead to weight gain. This article focuses on the potential of currently available pharmacological strategies and on emerging approaches in development to support the glycemic and weight-loss goals of individuals with type 2 diabetes. Two pharmacotherapy types are considered: those developed primarily for blood glucose control that have a favorable effect on body weight and those developed primarily to induce weight loss that have a favorable effect on blood glucose control. Finally, the potential of combination therapies for the management of obese patients with type 2 diabetes is discussed.
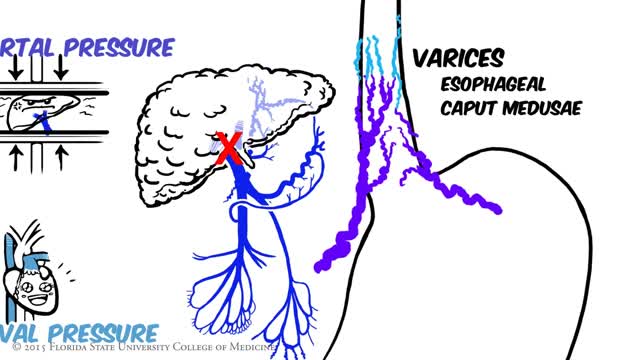
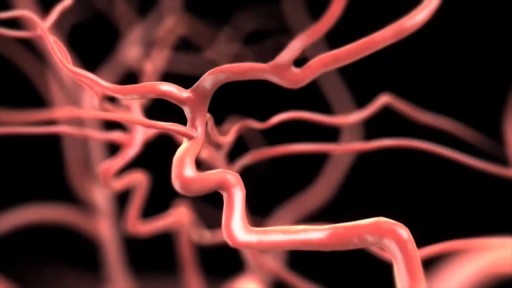
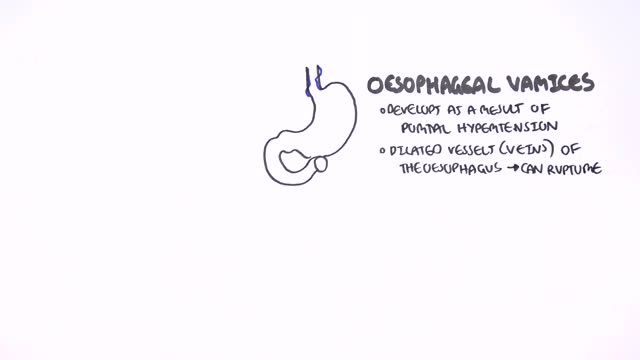
Portal hypertension is an increase in the blood pressure within a system of veins called the portal venous system. Veins coming from the stomach, intestine, spleen, and pancreas merge into the portal vein, which then branches into smaller vessels and travels through the liver.
an incision made on the back of the lower leg starting just above the heel bone. After the surgeon finds the two ends of the ruptured tendon, these ends are sewn together with sutures. The incision is then closed. Another repair method makes a small incision on the back of the lower leg at the site of the rupture.

Rheumatic heart disease (RHD) is the most common acquired heart disease in children in many countries of the world, especially in developing countries. The global burden of disease caused by rheumatic fever currently falls disproportionately on children living in the developing world, especially where poverty is widespread. RHD is a chronic heart condition caused by rheumatic fever that can be prevented and controlled. Rheumatic fever is caused by a preceding group A streptococcal (strep) infection. Treating strep throat with antibiotics can prevent rheumatic fever. Moreover, regular antibiotics (usually monthly injections) can prevent patients with rheumatic fever from contracting further strep infections and causing progression of valve damage. Consequences of rheumatic heart disease Acute rheumatic fever primarily affects the heart, joints and central nervous system. The major importance of acute rheumatic fever is its ability to cause fibrosis of heart valves, leading to crippling valvular heart disease, heart failure and death. The decline of rheumatic fever in developed countries is believed to be the result of improved living conditions and availability of antibiotics for treatment of group A streptococcal infection. Overcrowding, poor housing conditions, undernutrition and lack of access to healthcare play a role in the persistence of this disease in developing countries.

Diarrhea in Children: Common Causes and Treatments Diarrhea is the body's way of ridding itself of germs, and most episodes last a few days to a week. Diarrhea often occurs with fever, nausea, vomiting, cramps, and dehydration. Some of the most common reasons kids get diarrhea include: Infection from viruses like rotavirus, bacteria like salmonella and, rarely, parasites like giardia. Viruses are the most common cause of a child's diarrhea. Along with loose or watery stools, symptoms of a viral gastroenteritis infection often include vomiting, stomachache, headache, and fever. When treating viral gastroenteritis -- which can last 5-14 days -- it's important to prevent fluid loss. Offer additional breast milk or an oral rehydration solution (ORS) to infants and young children. Water alone doesn't have enough sodium, potassium, and other nutrients to safely rehydrate very young children. Be sure to talk to your doctor about the amount of fluids your child needs, how to make sure he or she gets them, when to give them, and how to watch for dehydration. Older children with diarrhea can drink anything they like to stay hydrated, including ORS and brand-name products (their names usually end in "lyte"). Popsicles can also be a good way to get fluids into a child who's been vomiting and needs to rehydrate slowly.
Although the Apgar score was developed in 1952 by an anesthesiologist named Virginia Apgar, you also might hear it referred to as an acronym for: Appearance, Pulse, Grimace, Activity, and Respiration. The Apgar test is usually given to a baby twice: once at 1 minute after birth, and again at 5 minutes after birth.

Major signs and symptoms include enlargement of the liver and spleen (hepatosplenomegaly), a low number of red blood cells (anemia), easy bruising caused by a decrease in blood platelets (thrombocytopenia), lung disease, and bone abnormalities such as bone pain, fractures, and arthritis.

Diabetes insipidus (die-uh-BEE-teze in-SIP-uh-dus) is an uncommon disorder that causes an imbalance of water in the body. This imbalance leads to intense thirst even after drinking fluids (polydipsia), and excretion of large amounts of urine (polyuria). While the names diabetes insipidus and diabetes mellitus sound similar, they're not related. Diabetes mellitus — which can occur as type 1 or type 2 — is the more common form of diabetes. There's no cure for diabetes insipidus, but treatments are available to relieve your thirst and normalize your urine output.