Top videos
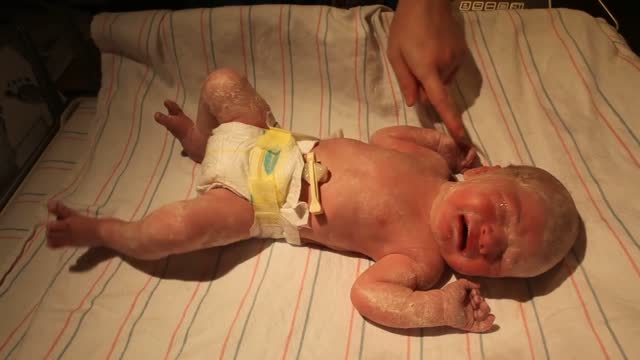
Although the Apgar score was developed in 1952 by an anesthesiologist named Virginia Apgar, you also might hear it referred to as an acronym for: Appearance, Pulse, Grimace, Activity, and Respiration. The Apgar test is usually given to a baby twice: once at 1 minute after birth, and again at 5 minutes after birth.

Major signs and symptoms include enlargement of the liver and spleen (hepatosplenomegaly), a low number of red blood cells (anemia), easy bruising caused by a decrease in blood platelets (thrombocytopenia), lung disease, and bone abnormalities such as bone pain, fractures, and arthritis.

Dialysis patients need to choose their heart medicine carefully, as Canadian researchers say that some beta blockers are easily removed from the blood during treatment. Also, people who eat a Mediterranean diet may decrease their risk of developing kidney problems. Eboni Williams reports on the day's top health news.

Diabetes insipidus (die-uh-BEE-teze in-SIP-uh-dus) is an uncommon disorder that causes an imbalance of water in the body. This imbalance leads to intense thirst even after drinking fluids (polydipsia), and excretion of large amounts of urine (polyuria). While the names diabetes insipidus and diabetes mellitus sound similar, they're not related. Diabetes mellitus — which can occur as type 1 or type 2 — is the more common form of diabetes. There's no cure for diabetes insipidus, but treatments are available to relieve your thirst and normalize your urine output.

When taking oral corticosteroids longer term, you may experience: Clouding of the lens in one or both eyes (cataracts) High blood sugar, which can trigger or worsen diabetes. Increased risk of infections. Thinning bones (osteoporosis) and fractures. Suppressed adrenal gland hormone production
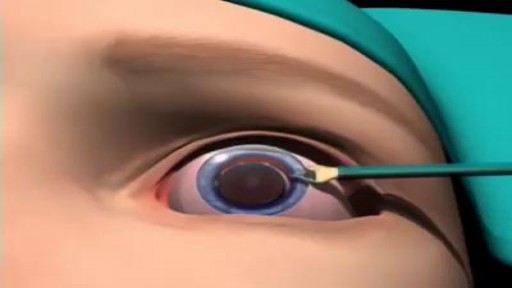
Most cataracts are associated with the aging process and are common among older Americans. In fact, according to the National Eye Institute (NEI), 68.3 percent of Americans 80 and older had cataracts in 2010. And the prevalence of cataracts in the U.S. is expected to grow significantly in the years ahead, due in part to the aging of the population. In 2010, roughly 24.4 million Americans had cataracts, and that number is projected to grow to 50.2 million by the year 2050, according to NEI.

Aspirin is used to reduce fever and relieve mild to moderate pain from conditions such as muscle aches, toothaches, common cold, and headaches. It may also be used to reduce pain and swelling in conditions such as arthritis. Aspirin is known as a salicylate and a nonsteroidal anti-inflammatory drug (NSAID).
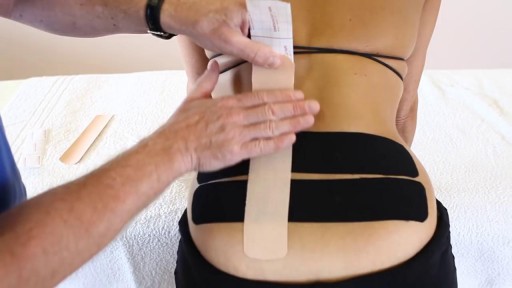
Dysfunction in the sacroiliac joint, also called the SI joint, can sometimes cause lower back and/or leg pain. Leg pain from sacroiliac joint dysfunction can be particularly difficult to differentiate from radiating leg pain caused by a lumbar disc herniation (sciatica) as they can feel quite similar.
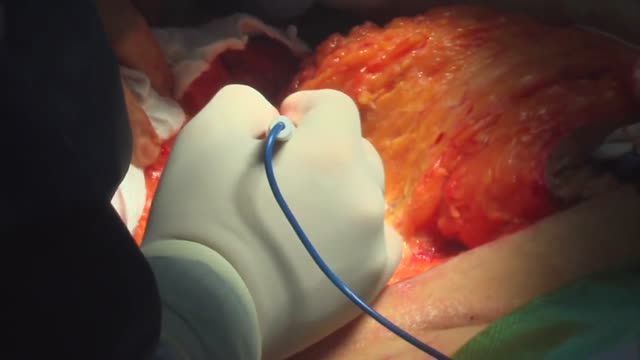
surgical procedure used to remove excess skin and fat from the abdomen and to tighten the muscles of the abdominal wall. Most tummy tuck patients are dealing with the effects of pregnancies and weight loss and find themselves with loose skin in spite of exercise and weight control. Each year, thousands of Americans undergo a tummy tuck to tone, firm and define the abdominal area.

Women who have untreated chlamydia might develop pelvic inflammatory disease, which can cause ectopic pregnancies, chronic pelvic pain and infertility. ... The antibiotics used to treat chlamydia are safe in pregnancy and are used in pregnant women for many other types of infections.

Of the many factors that affect your compatibility with a man, one of the biggest (or smallest) is in his pants. As with humour, interests or habits, the wrong fit can leave you cold. Or traumatised. In a study of 1,661 penises, Dr Debby Herbenick, author of Sex Made Easy, found an almost nine-inch difference in erection size: from 1.6 inches to 10.2. And since absolutely nothing outside the package tells you what to expect with the package, you have to test compatibility the hard way. Sometimes you hit your jackpot, sometimes it's just fine, and sometimes he's the guy on either end of that erection spectrum. These writers have been there, so here's what they learned - and how you can deal (without the gasp reflex).
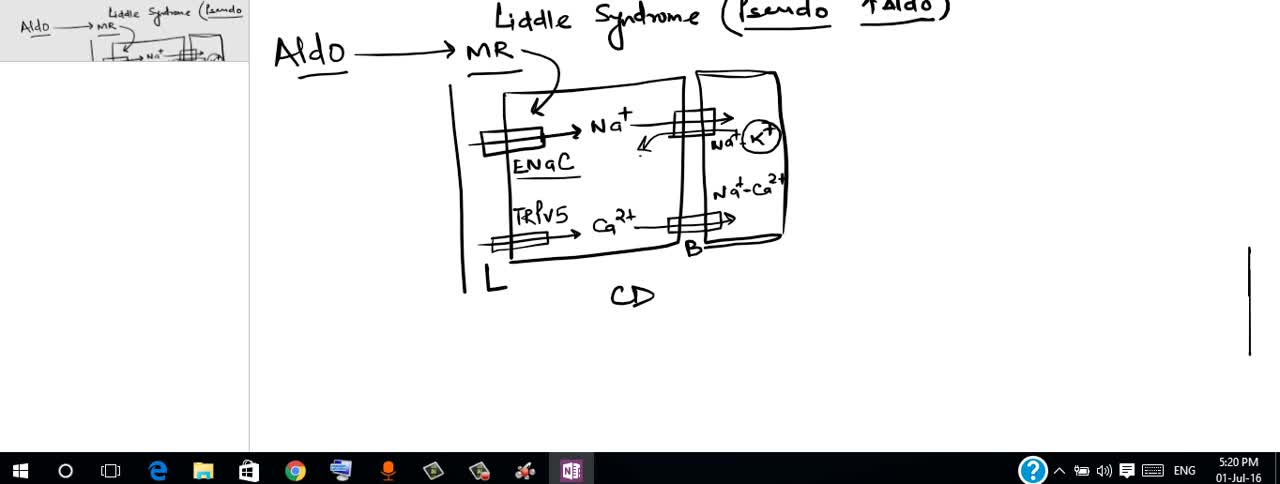
Liddle syndrome is an inherited form of high blood pressure (hypertension). This condition is characterized by severe hypertension that begins unusually early in life, often in childhood, although some affected individuals are not diagnosed until adulthood. Some people with Liddle syndrome have no additional signs or symptoms, especially in childhood. Over time, however, untreated hypertension can lead to heart disease or stroke, which may be fatal.
Primary biliary cholangitis (PBC), formerly known as primary biliary cirrhosis, is a chronic liver disease resulting from progressive destruction of the bile ducts in the liver – called the intrahepatic bile ducts. Bile produced in your liver travels via these ducts to your small intestine where it aids in the digestion of fat and fat-soluble vitamins (A, D, E and K). When the ducts are destroyed, bile builds up in the liver contributing to inflammation and scarring (fibrosis). Eventually this can lead to cirrhosis and its associated complications, as scar tissue replaces healthy liver tissue and liver function becomes increasingly impaired.
Reduction techniques can vary in terms of required force, time, equipment, and staff. [7] No single reduction method is successful in every instance; therefore, the clinician should be familiar with several reduction techniques. Techniques commonly used to reduce anterior shoulder dislocations include the following [35, 36, 37, 38, 39] : Stimson maneuver Scapular manipulation External rotation Milch technique Spaso technique Traction-countertraction
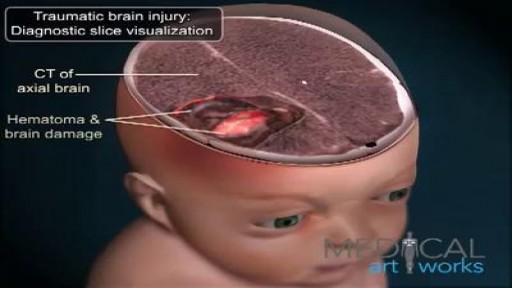
Traumatic Brain Injury (TBI) TBI is defined as an alteration in brain function, or other evidence of brain pathology, caused by an external force. Adopted by the Brain Injury Association Board of Directors in 2011. This definition is not intended as an exclusive statement of the population served by the Brain Injury Association of America. Acquired Brain Injury An acquired brain injury is an injury to the brain, which is not hereditary, congenital, degenerative, or induced by birth trauma. An acquired brain injury is an injury to the brain that has occurred after birth. There is sometimes confusion about what is considered an acquired brain injury. By definition, any traumatic brain injury (e.g. from a motor vehicle accident or assault) could be considered an acquired brain injury. In the field of brain injury, acquired brain injuries are typically considered any injury that is non traumatic. Examples of acquired brain injury include stroke, near drowning, hypoxic or anoxic brain injury, tumor, neurotoxins, electric shock or lightning strike.