Top videos

Orthognathic surgery presented in this video in order of appearance. 1. Advancement Genioplasty 2. Maxillary Advancement 3. Maxillary impaction 4. BSSO Mandibular Advancement 5. BSSO Mandibular Set-back 6. Maxillary Posterior Impaction

An antisperm antibody test looks for special proteins (antibodies) that fight against a man's sperm in blood, vaginal fluids, or semen. The test uses a sample of sperm and adds a substance that binds only to affected sperm. Semen can cause an immune system response in either the man's or woman's body. The antibodies can damage or kill sperm. If a high number of sperm antibodies come into contact with a man's sperm, it may be hard for the sperm to fertilize an egg. The couple has a hard time becoming pregnant. This is called immunologic infertility.

15th August Special Offer - Get 50% discount on Chemical Peel & Medical Facial ! offer valid till 31st August 2018 ! Call now 09958221983 to book appointment! Send your Query: info@drkashyap.com #MedicalFacial #ChemicalPeels #Facial #SkinCare #NonSurgical #Treatments #Clinic #Delhi #India #15thAugust #IndependenceDay
Shaken baby syndrome usually occurs when a parent or caregiver severely shakes a child in frustration or anger, often because the child won't stop crying. Permanent brain damage or death may result. Symptoms include irritability, difficulty staying awake, seizures, abnormal breathing, poor eating, bruises, and vomiting. Treatment will vary depending on complications related to shaken baby syndrome. In rare instances, breathing support or surgery may be needed to stop bleeding in the brain.
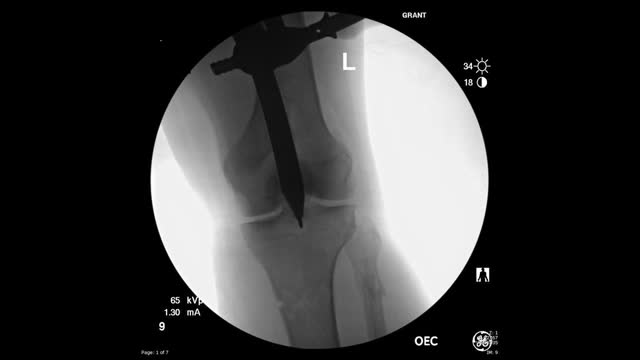
This video shows the technique of suprapatellar tibial nailing as used for a segmental tibia fracture. The broken leg was treated with the nail to allow immediate mobility and range of motion; no cast was needed for this injury.

Usually a sebaceous cyst grows very slowly and doesn't cause pain. However, they can become inflamed or infected, with the overlying skin becoming red, tender, and sore. Sometimes, they occur on a site that is constantly irritated, such as a cyst on your neck that rubs against your collar.

In Reye's syndrome, a child's blood sugar level typically drops while the levels of ammonia and acidity in his or her blood rise. At the same time, the liver may swell and develop fatty deposits. Swelling may also occur in the brain, which can cause seizures, convulsions or loss of consciousness. The signs and symptoms of Reye's syndrome typically appear about three to five days after the onset of a viral infection, such as the flu (influenza) or chickenpox, or an upper respiratory infection, such as a cold

This medication is used to treat certain types of serious (possibly fatal) irregular heartbeat (such as persistent ventricular fibrillation/tachycardia). It is used to restore normal heart rhythm and maintain a regular, steady heartbeat. Amiodarone is known as an anti-arrhythmic drug. It works by blocking certain electrical signals in the heart that can cause an irregular heartbeat.
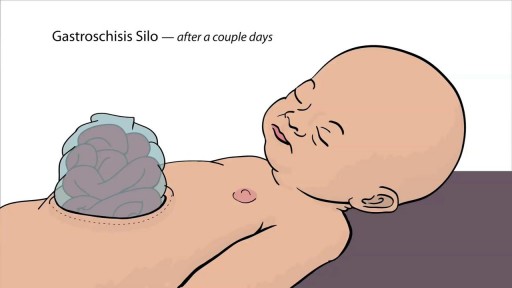
Gastroschisis is a birth defect of the abdominal (belly) wall. The baby’s intestines stick outside of the baby’s body, through a hole beside the belly button. The hole can be small or large and sometimes other organs, such as the stomach and liver, can also stick outside of the baby’s body. Gastroschisis occurs early during pregnancy when the muscles that make up the baby’s abdominal wall do not form correctly. A hole occurs which allows the intestines and other organs to extend outside of the body, usually to the right side of belly button. Because the intestines are not covered in a protective sac and are exposed to the amniotic fluid, the bowel can become irritated, causing it to shorten, twist, or swell.