Top videos
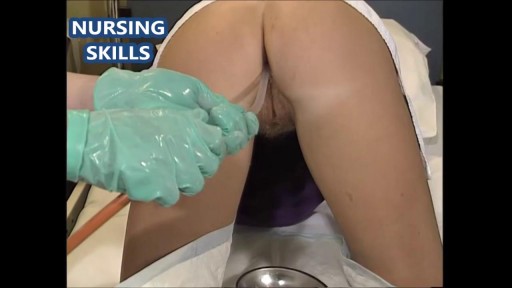
A renal biopsy is a procedure used to extract kidney tissue for laboratory analysis. The word “renal” describes the kidneys. A renal biopsy is also called a kidney biopsy. The test helps your doctor identify the type of kidney disease you have, how severe it is, and the best treatment for it.

http://smoking-videos.plus101.com
Quit Smoking Forever Formula Videos - How To Quit Smoking In As Fast As 1 Week Without Agitation, Cravings Or Withdrawal Symptoms.You're about to uncover the 3 elements that will rapidly boost your chances of success to quit smoking and not only that, you'll learn ways to escape cravings and how to avoid a relapse that can happen in the future even to people with the most willpower.

Nosebleeds are common due to the location of the nose on the face, and the large amount of blood vessels in the nose. The most common causes of nosebleeds are drying of the nasal membranes and nose picking (digital trauma), which can be prevented with proper lubrication of the nasal passages and not picking the nose.

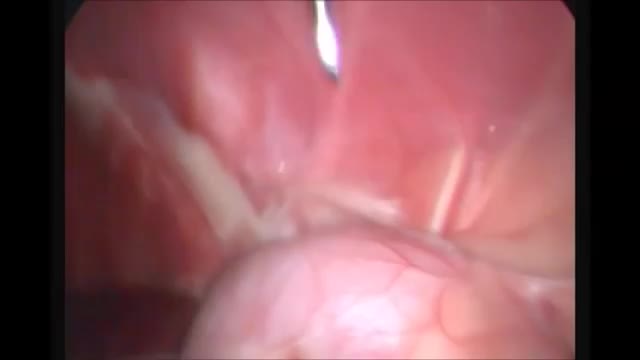
Dr. James Wall performs a bilateral inguinial hernia repair surgical procedure.
Featured:
James Wall, MD
Assistant Professor of Surgery, Pediatric Surgery
Assistant Professor of Bioengineering (By Courtesy)
Lucile Salter Packard Children's Hospital
Micaela Esquivel, MD
Chief Resident of General Surgery
Shingles is a painful skin rash camera.gif. It is caused by the varicella zoster virus. Shingles usually appears in a band, a strip, or a small area on one side of the face or body. It is also called herpes zoster. Shingles is most common in older adults and people who have weak immune systems because of stress, injury, certain medicines, or other reasons. Most people who get shingles will get better and will not get it again. But it is possible to get shingles more than once.

When diving into a Breast Reduction procedure, there are many things to consider. Even as a patient, being aware of any concerns and how the procedure works is important. Therefore, when a plastic surgeon operates on a patient, the results are clear. Dr. Linder, a Breast surgeon specialist in Beverly Hills, helps explain what goes into a Breast Reduction Procedure.
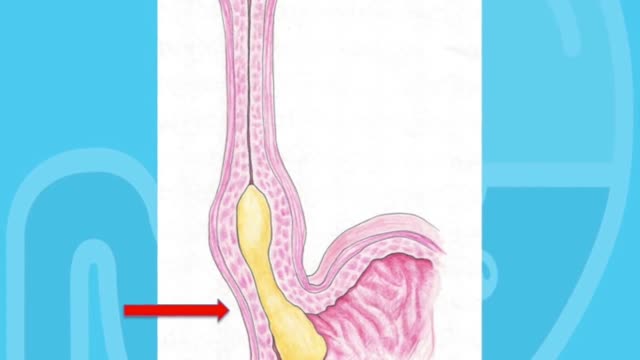
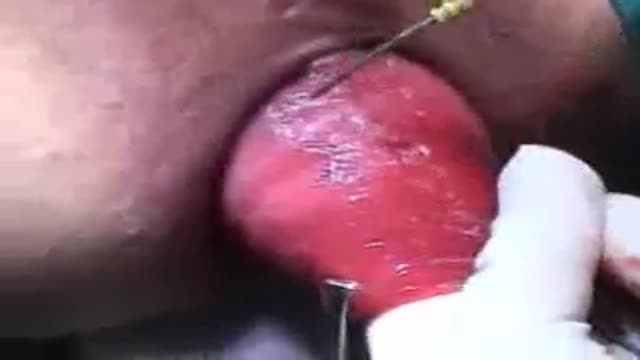
Achalasia is a neurogenic esophageal motility disorder characterized by impaired esophageal peristalsis and a lack of lower esophageal sphincter relaxation during swallowing. Symptoms are slowly progressive dysphagia, usually to both liquids and solids, and regurgitation of undigested food. Evaluation typically includes manometry, barium swallow, and endoscopy. Treatments include dilation, chemical denervation, surgical myotomy, and peroral endoscopic myotomy.

The Combitube is a twin lumen device designed for use in emergency situations and difficult airways. It can be inserted without the need for visualization into the oropharynx, and usually enters the esophagus. It has a low volume inflatable distal cuff and a much larger proximal cuff designed to occlude the oro- and nasopharynx.
If the tube has entered the trachea, ventilation is achieved through the distal lumen as with a standard ETT. More commonly the device enters the esophagus and ventilation is achieved through multiple proximal apertures situated above the distal cuff. In the latter case the proximal and distal cuffs have to be inflated to prevent air from escaping through the esophagus or back out of the oro- and nasopharynx.
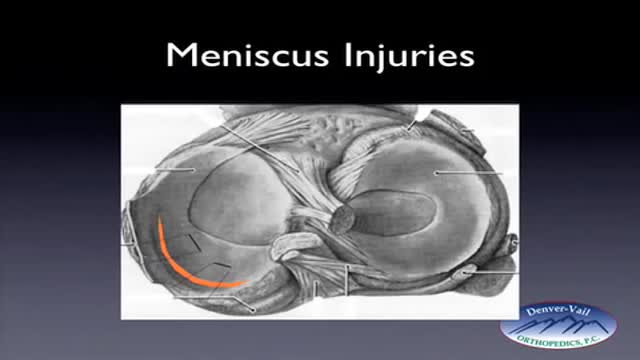
Rehabilitation time for a meniscus repair is about 3 months. A meniscectomy requires less time for healing — approximately 3 to 4 weeks. Meniscus tears are extremely common knee injuries. With proper diagnosis, treatment, and rehabilitation, patients often return to their pre-injury abilities.
A myringotomy is a procedure in which your doctor creates a small hole in the eardrum so fluids such as water, blood, or pus can drain out. In many cases, your doctor will put in a tube so it won't get backed up again. The tube, which will usually fall out on its own in about six to 18 months, lets air flow through and keeps the middle ear dry. Tubes also: Reduce pain Improve hearing Cut down on the number of infections your child may have
Over one million Americans have the sexually transmitted virus, HIV, which can lead to the deadly disease known as AIDS.
HIV can be transmitted in the sexual fluids, blood or breast milk of an infected person. HIV prevention therefore involves a wide range of activities including prevention of mother-to-child transmission, needle exchanges and harm reduction for injecting drug users, and precautions for health care workers.

Will you still love me if I have herpes? About 1 in 6 Americans between the ages of 14 and 49 is infected with herpes simplex virus type 2, according to a health survey released by the Centers for Disease Control and Prevention. If you’re living with herpes, HSV, HPV or other STDs, you're recommended to check out the largest STD support site STDdatings.