Top videos

Furosemide is a prescription drug. It’s available in two forms that you take by mouth: a tablet and a solution. It’s also available as an injectable solution, which is given by a healthcare provider. The furosemide tablet is available as the brand-name drug Lasix. It’s also available as a generic drug. Generic drugs usually cost less. In some cases, they may not be available in every strength or form as the brand-name version.
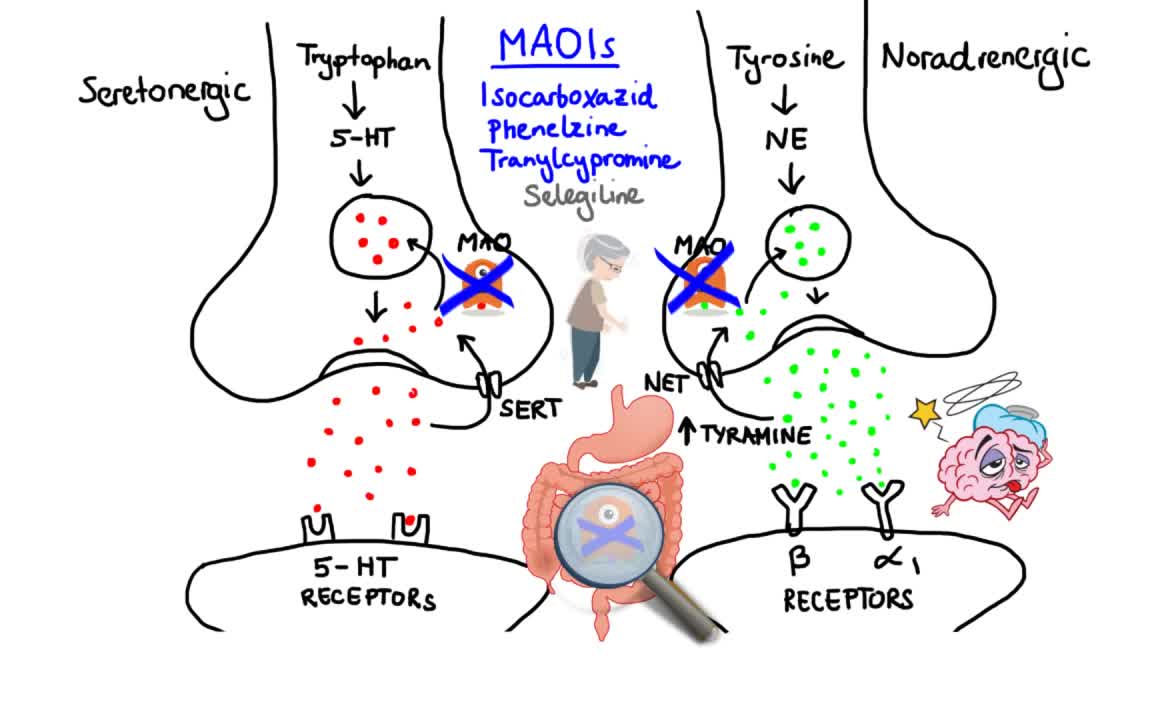
Do you suffer with depression? Maybe you’ve recently been diagnosed or are a caregiver to someone with depression. Learn more about this common mood disorder, including depression causes, risk factors, and prevention. We’ll help you take control of your depression and live an active, healthy life.
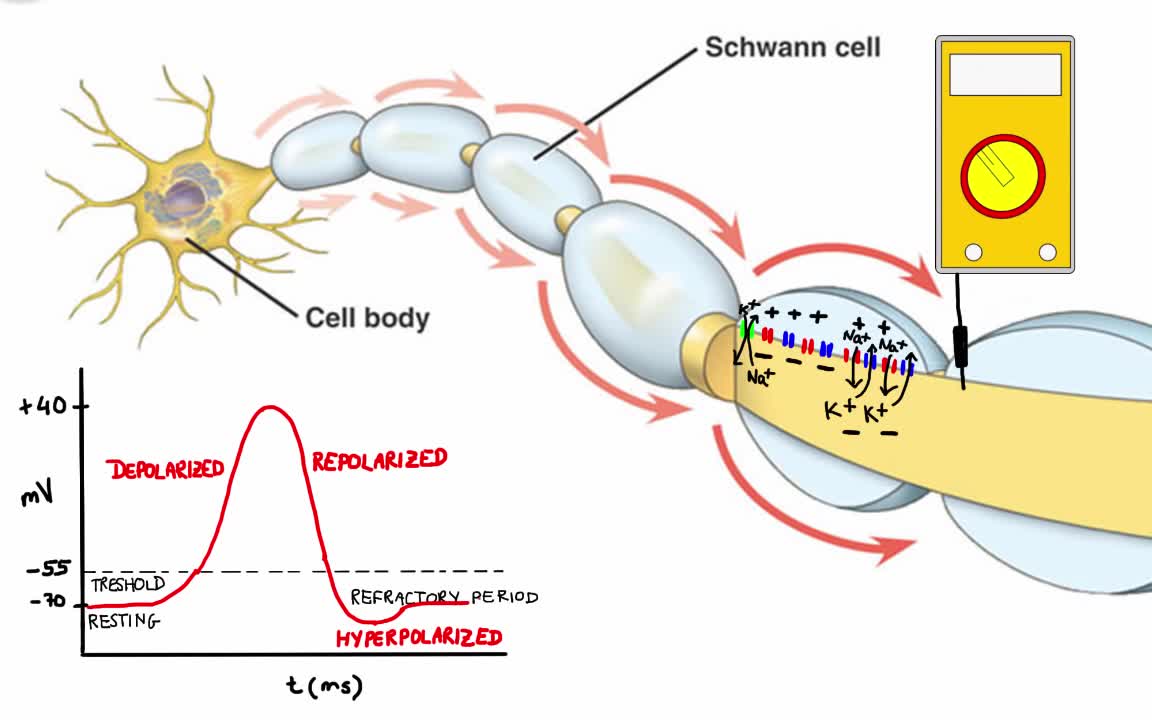
Your body has nerves that connect your brain to the rest of your organs and muscles, just like telephone wires connect homes all around the world. When you want your hand to move, your brain sends signals through your nerves to your hand telling the muscles to contract. But your nerves don’t just say “hand, move.” Instead your nerves send lots of electrical impulses (called action potentials) to different muscles in your hand, allowing you to move your hand with extreme precision.
Some of these advancements include the use of robots to perform the surgery and the use of computer mapping scanners and software and even 3D printers to make the artificial knee implant. We are also seeing a lot of different advances being made by the medical device manufacturers.Some of these changes are designed to make the devices more durable than the 10 to 20 years they are currently rated to last. This is important when younger patients who are years away from being considered elderly have a total knee replacement, they will typically need another artificial knee implanted at a later date since they are likely to outlive the implant, which doesn’t always happen with elderly patients.

Epstein-Barr is the virus that causes mononucleosis. You might know this disease better by its nickname, "mono." It's also called the "kissing disease" because of one way you can spread it to someone else. Even though Epstein-Barr virus (EBV) isn't a household name, you've probably been infected without knowing it. Lots of people carry the virus but don't get sick

Bovine respiratory disease (BRD) has a multifactorial etiology and develops as a result of complex interactions between environmental factors, host factors, and pathogens. Environmental factors (eg, weaning, transport, commingling, crowding, inclement weather, dust, and inadequate ventilation) serve as stressors that adversely affect the immune and nonimmune defense mechanisms of the host. In addition, certain environmental factors (eg, crowding and inadequate ventilation) can enhance the transmission of infectious agents among animals. Many infectious agents have been associated with BRD. An initial pathogen (eg, a virus) may alter the animal’s defense mechanisms, allowing colonization of the lower respiratory tract by bacteria.
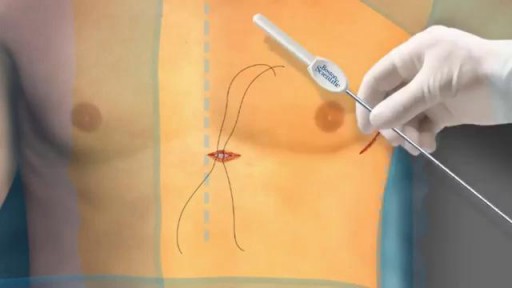
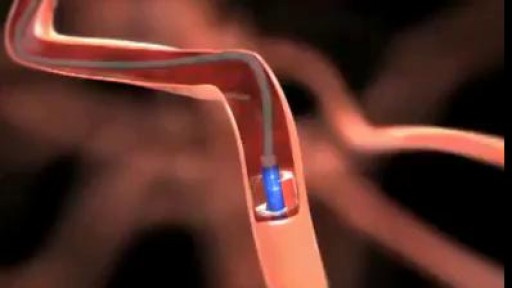
S-ICD leaves the heart and vasculature untouched. It may be implanted using only anatomical landmarks, thereby eliminating the need for fluoroscopy during implant and therefore reducing radiation exposure for both patients and physicians and eliminating the need for lead apron during implant.
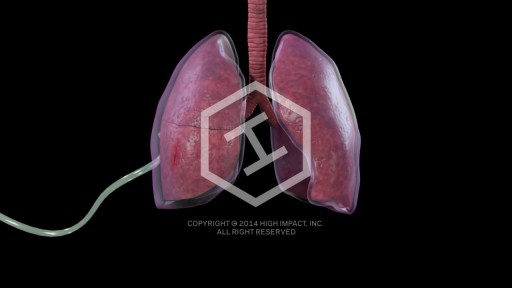
A small spontaneous pneumothorax may resolve without treatment; a pneumothorax arising as a result of lung disease or injury requires immediate treatment. Treatment may include insertion of a chest tube or aspiration of the free air in the chest cavity.
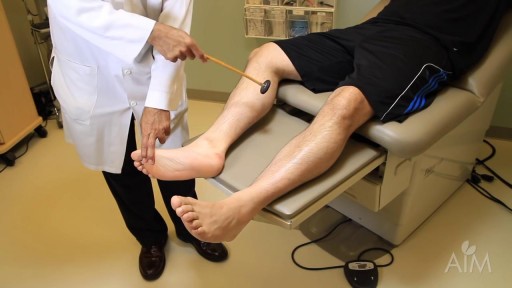
In a normal person, when a muscle tendon is tapped briskly, the muscle immediately contracts due to a two-neuron reflex arc involving the spinal or brainstem segment that innervates the muscle. The afferent neuron whose cell body lies in a dorsal root ganglion innervates the muscle or Golgi tendon organ associated with the muscles; the efferent neuron is an alpha motoneuron in the anterior horn of the cord. The cerebral cortex and a number of brainstem nuclei exert influence over the sensory input of the muscle spindles by means of the gamma motoneurons that are located in the anterior horn; these neurons supply a set of muscle fibers that control the length of the muscle spindle itself.
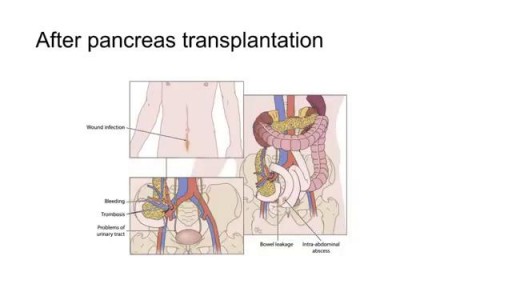
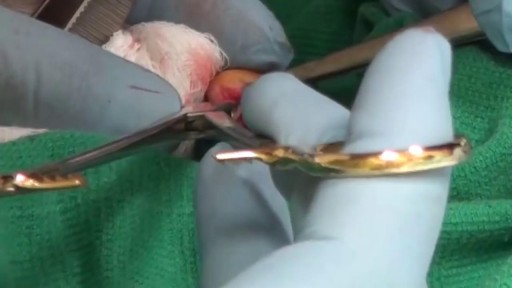
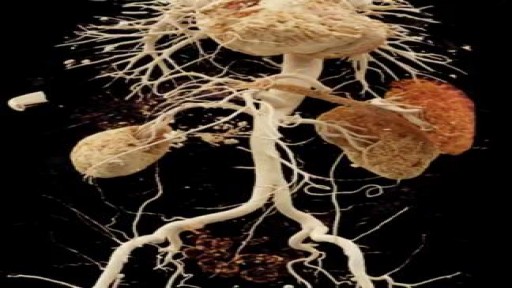
Kidney transplant surgery carries a risk of significant complications, including: Blood clots Bleeding Leaking from or blockage of the tube (ureter) that links the kidney to the bladder Infection Failure of the donated kidney Rejection of the donated kidney An infection or cancer that can be transmitted with the donated kidney Death, heart attack and stroke