Top videos
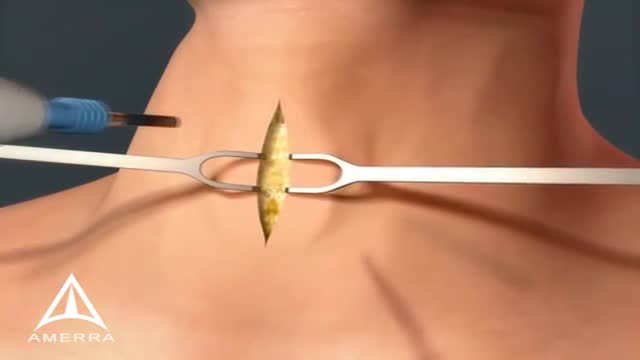
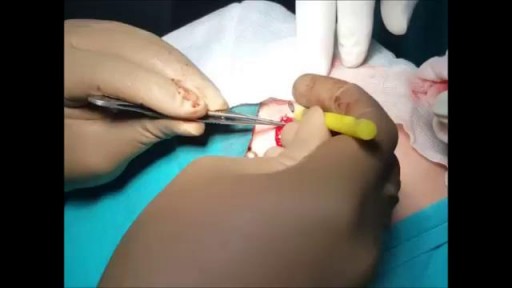
A tracheotomy or a tracheostomy is an opening surgically created through the neck into the trachea (windpipe) to allow direct access to the breathing tube and is commonly done in an operating room under general anesthesia. A tube is usually placed through this opening to provide an airway and to remove secretions from the lungs. Breathing is done through the tracheostomy tube rather than through the nose and mouth. The term “tracheotomy” refers to the incision into the trachea (windpipe) that forms a temporary or permanent opening, which is called a “tracheostomy,” however; the terms are sometimes used interchangeably.
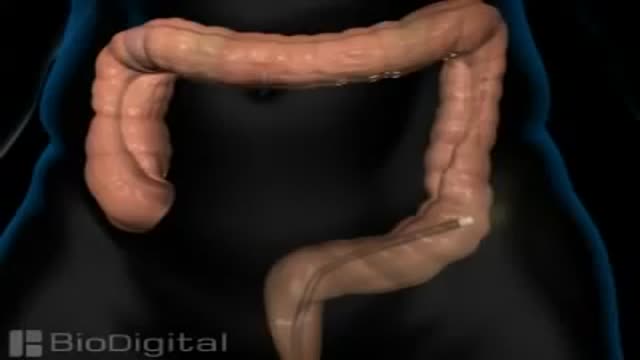
Colonoscopy is a test that allows your doctor to look at the inner lining of your large intestine (rectum and colon). He or she uses a thin, flexible tube called a colonoscope to look at the colon. A colonoscopy helps find ulcers, colon polyps, tumors, and areas of inflammation or bleeding.

t’s the brain, after all, that devises experiments and interprets their results. How the brain perceives, how it makes decisions and judgments, and how those judgments can go awry are at least as important to science as knowing the intricacies of nonbiotic experimental machinery. And as any brain scientist will tell you, there’s still a long way to go before understanding the brain will get crossed off science’s to-do list. But there has been progress. A recent special issue of the journal Neuron offers a convenient set of “perspective” papers exploring the current state of understanding of the brain’s inner workings. Those papers show that a lot is known. But at the same time they emphasize that there’s a lot we don’t know.

Natural painkiller found in human spit. Compound in saliva could be more powerful than morphine. A new painkilling substance has been discovered that is up to six times more potent than morphine when tested in rats — and it's produced naturally by the human body.
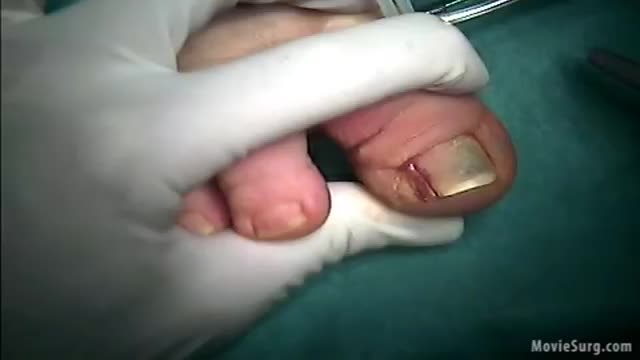
irregular, curved toenails. footwear that places a lot of pressure on the big toes, such as socks and stockings that are too tight or shoes that are too tight, narrow, or flat for your feet. toenail injury, including stubbing your toe, dropping something heavy on your foot, or kicking a ball repeatedly. poor posture.

Adult-onset Still's disease (AOSD) is a rare systemic inflammatory disease characterized by the classic triad of persistent high spiking fevers, joint pain, and a distinctive salmon-colored bumpy rash. The disease is considered a diagnosis of exclusion.

The condition is caused by a blockage in the lymphatic system, part of the immune and circulatory systems. Lymphedema is most commonly caused by lymph node removal or damage due to cancer treatment. The main symptom is swelling in an arm or leg that may be accompanied by pain or discomfort. Exercise, wrapping, massage, and compression can help.

Initially, lead poisoning can be hard to detect — even people who seem healthy can have high blood levels of lead. Signs and symptoms usually don't appear until dangerous amounts have accumulated. Lead poisoning symptoms in children Signs and symptoms of lead poisoning in children include: Developmental delay Learning difficulties Irritability Loss of appetite Weight loss Sluggishness and fatigue Abdominal pain Vomiting Constipation Hearing loss Seizures Eating things, such as paint chips, that aren't food (pica) Lead poisoning symptoms in newborns Babies exposed to lead before birth might: Be born prematurely Have lower birth weight Have slowed growth Lead poisoning symptoms in adults Although children are primarily at risk, lead poisoning is also dangerous for adults. Signs and symptoms in adults might include: High blood pressure Joint and muscle pain Difficulties with memory or concentration Headache Abdominal pain Mood disorders Reduced sperm count and abnormal sperm Miscarriage, stillbirth or premature birth in pregnant women Causes Lead is a metal that occurs naturally in the earth's crust, but human activity — mining, burning fossil fuels and manufacturing — has caused it to become more widespread. Lead was also once used in paint and gasoline and is still used in batteries, solder, pipes, pottery, roofing materials and some cosmetics. Lead in paint Lead-based paints for homes, children's toys and household furniture have been banned in the United States since 1978. But lead-based paint is still on walls and woodwork in many older homes and apartments. Most lead poisoning in children results from eating chips of deteriorating lead-based paint. Water pipes and imported canned goods Lead pipes, brass plumbing fixtures and copper pipes soldered with lead can release lead particles into tap water. Lead solder in food cans, banned in the United States, is still used in some countries. Other sources of lead exposure Lead sometimes can also be found in: Soil. Lead particles from leaded gasoline or paint settle on soil and can last years. Lead-contaminated soil is still a major problem around highways and in some urban settings. Some soil close to walls of older houses contains lead. Household dust. Household dust can contain lead from lead paint chips or from contaminated soil brought in from outside. Pottery. Glazes found on some ceramics, china and porcelain can contain lead that can leach into food served or stored in the pottery. Toys. Lead is sometimes found in toys and other products produced abroad. Cosmetics. Tiro, an eye cosmetic from Nigeria, has been linked to lead poisoning. Herbal or folk remedies. Lead poisoning has been linked to greta and azarcon, traditional Hispanic medicines, as well as some from India, China and other countries. Mexican candy. Tamarind, an ingredient used in some candies made in Mexico, might contain lead. Lead bullets. Time spent at firing ranges can lead to exposure. Occupations. People are exposed to lead and can bring it home on their clothes when they work in auto repair, mining, pipe fitting, battery manufacturing, painting, construction and certain other fields

Rehydration Tips: Kids & Teens (Ages 1+) Give clear liquids (avoid milk and milk products) in small amounts every 15 minutes. ... If your child vomits, start over with a smaller amount of fluid (2 teaspoons, or about 10 milliliters) and continue as above. ... After no vomiting for about 8 hours, introduce solid foods slowly.
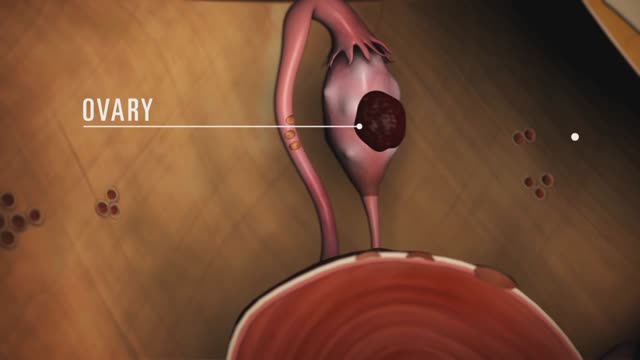
Endometriosis (en-doe-me-tree-O-sis) is an often painful disorder in which tissue that normally lines the inside of your uterus — the endometrium — grows outside your uterus. Endometriosis most commonly involves your ovaries, fallopian tubes and the tissue lining your pelvis. Rarely, endometrial tissue may spread beyond pelvic organs.
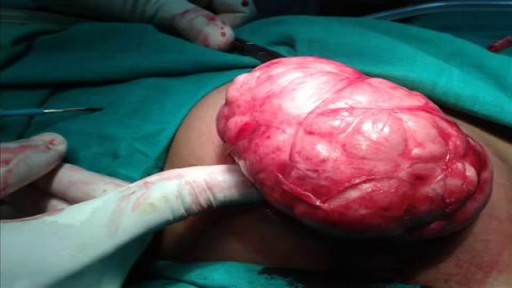
Bone tumors develop when cells in the bone divide without control, forming a mass of tissue. Most bone tumors are benign, which means they are not cancer and cannot spread. However, they may still weaken bone and lead to fractures or cause other problems. Bone cancer destroys normal bone tissue and may spread to other parts of the body (called metastasis). Benign Bone Tumors Benign tumors are more common than malignant tumors of the bones. These are a few common types of benign bone tumors: Osteochondroma is the most common benign bone tumor. It is more common in people under age 20. Giant cell tumor is a benign tumor, typically affecting the leg (malignant types of this tumor are uncommon). Osteoid osteoma is a bone tumor, often occurring in long bones, that occurs commonly in the early 20s. Osteoblastoma is a single tumor that occurs in the spine and long bones, mostly in young adults. Enchondroma usually appears in bones of the hand and feet. It often has no symptoms. It is the most common type of hand tumor.

Myelodysplastic syndromes are a group of cancers in which immature blood cells in the bone marrow do not mature or become healthy blood cells. In a healthy person, the bone marrow makes blood stem cells (immature cells) that become mature blood cells over time.Aug 12, 2015
If you look at someone’s back, you’ll see that the spine runs straight down the middle. When a person has scoliosis, their backbone curves to the side. The angle of the curve may be small, large or somewhere in between. But anything that measures more than 10 degrees is considered scoliosis. Doctors may use the letters “C” and “S” to describe the curve of the backbone. You probably don’t look directly at too many spines, but what you might notice about someone with scoliosis is the way they stand. They may lean a little or have shoulders or hips that look uneven. What Causes Scoliosis? In as many as 80% of cases, doctors don’t find the exact reason for a curved spine. Scoliosis without a known cause is what doctors call “idiopathic.” Some kinds of scoliosis do have clear causes. Doctors divide those curves into two types -- structural and nonstructural. In nonstructural scoliosis, the spine works normally, but looks curved. Why does this happen? There are a number of reasons, such as one leg’s being longer than the other, muscle spasms, and inflammations like appendicitis. When these problems are treated, this type of scoliosis often goes away.