Top videos

Overactive bladder syndrome is common. Symptoms include an urgent feeling to go to the toilet, going to the toilet frequently and sometimes leaking urine before you can get to the toilet (urge incontinence). Treatment with bladder training often cures the problem. Sometimes medication may be advised in addition to bladder training to relax the bladder.
Myasthenia gravis is a chronic autoimmune neuromuscular disease characterized by varying degrees of weakness of the skeletal (voluntary) muscles of the body. The name myasthenia gravis, which is Latin and Greek in origin, literally means "grave muscle weakness."
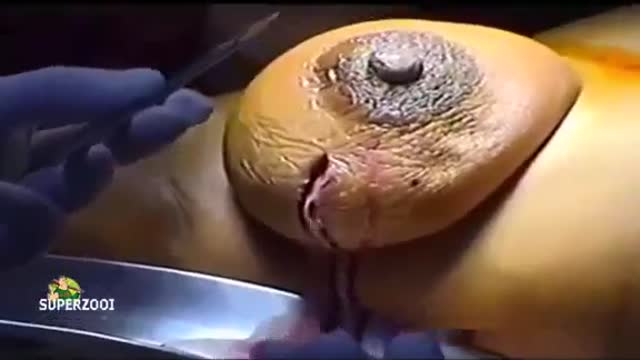
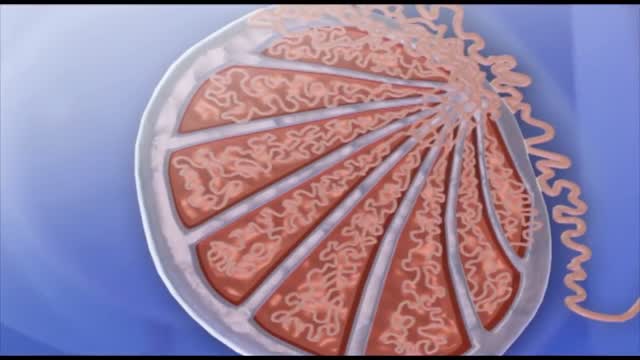
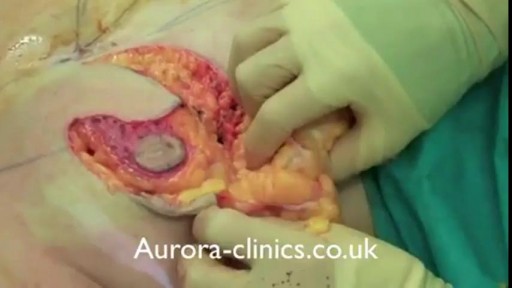
Breast abscesses are often linked to mastitis – a condition that causes breast pain and swelling (inflammation), and usually affects women who are breastfeeding. Infections can occur during breastfeeding if bacteria enter your breast tissue, or if the milk ducts (tiny tubes) become blocked. This can cause mastitis which, if not treated, can result in an abscess forming. Women who aren't breastfeeding can also develop mastitis if bacteria enter the milk ducts through a sore or cracked nipple, or a nipple piercing. White blood cells are sent to attack the infection, which causes tissue at the site of the infection to die. This creates a small, hollow area that fills with pus (an abscess).
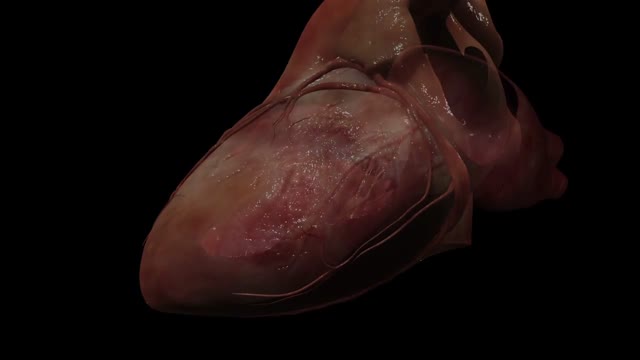
The heart is the body's engine room, responsible for pumping life-sustaining blood via a 60,000-mile-long (97,000-kilometer-long) network of vessels. The organ works ceaselessly, beating 100,000 times a day, 40 million times a year—in total clocking up three billion heartbeats over an average lifetime. It keeps the body freshly supplied with oxygen and nutrients, while clearing away harmful waste matter.
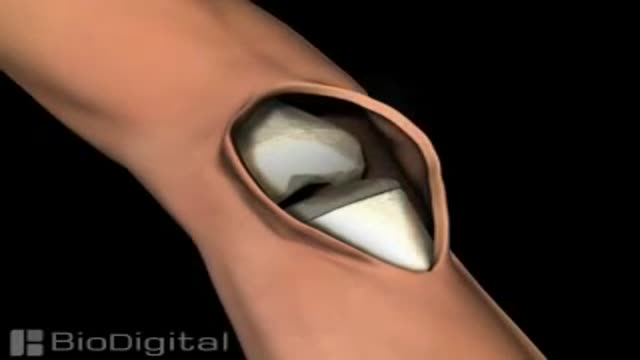
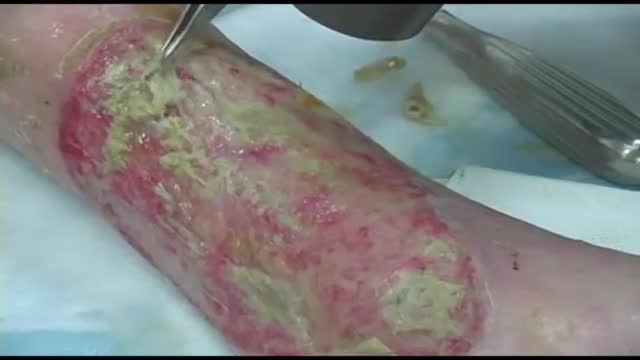
Knee replacement, also called arthroplasty, is a surgical procedure to resurface a knee damaged by arthritis. Metal and plastic parts are used to cap the ends of the bones that form the knee joint, along with the kneecap. This surgery may be considered for someone who has severe arthritis or a severe knee injury.
The external jugular vein receives the greater part of the blood from the exterior of the cranium and the deep parts of the face, being formed by the junction of the posterior division of the retromandibular vein with the posterior auricular vein.

Obstetrical emergencies of pregnancy ECTOPIC PREGNANCY. ... PLACENTAL ABRUPTION. ... PLACENTA PREVIA. ... ECTOPIC PREGNANCY. ... PLACENTAL ABRUPTION. ... PLACENTA PREVIA. ... Amniotic fluid — The liquid in the placental sac that cushions the fetus and regulates temperature in the placental environment.

Trisomy 18, also called Edwards syndrome, is a chromosomal condition associated with abnormalities in many parts of the body. Individuals with trisomy 18 often have slow growth before birth (intrauterine growth retardation) and a low birth weight. Affected individuals may have heart defects and abnormalities of other organs that develop before birth. Other features of trisomy 18 include a small, abnormally shaped head; a small jaw and mouth; and clenched fists with overlapping fingers. Due to the presence of several life-threatening medical problems, many individuals with trisomy 18 die before birth or within their first month. Five to 10 percent of children with this condition live past their first year, and these children often have severe intellectual disability.

Cushing's disease is a serious condition of an excess of the steroid hormone cortisol in the blood level caused by a pituitary tumor secreting adrenocorticotropic hormone (ACTH). ACTH is a hormone produced by the normal pituitary gland. ACTH stimulates the adrenal glands (located on top of the kidneys) to produce cortisol, commonly referred to as the stress hormone.

You may have heard that some positions, such as your partner on top (missionary position), are better than others for getting pregnant. In fact, there's no evidence to back these theories up. Experts just haven't done the research yet. What experts have done, though, is use scanning to show what's going on inside when you're doing the deed. The research looked at two positions: the missionary position and doggy style. (Doggy style being when you're on all fours, and your partner enters you from behind). Common sense tells us that these positions allow for deep penetration. This means that they're more likely to place sperm right next to your cervix (the opening of your uterus). The scans confirm that the tip of the penis reaches the areas between the cervix and vaginal walls in both of these positions. The missionary position allows the penis to reach the area at the front of the cervix. The rear entry position reaches the area at back of the cervix. It's amazing what some experts spend their time doing, isn't it! Other positions, such as standing up, or woman on top, may be just as good for getting sperm right next to the cervix. We just don't know yet. http://www.babycentre.co.uk/sex-for-getting-pregnant#ixzz4XKnPLbxL

Gastroparesis -- literally “paralyzed stomach” -- is a serious condition manifested by delayed emptying of stomach contents into the small intestine after a meal. There is no cure for gastroparesis, but treatment can speed gastric emptying and relieve gastrointestinal symptoms such as nausea and vomiting.
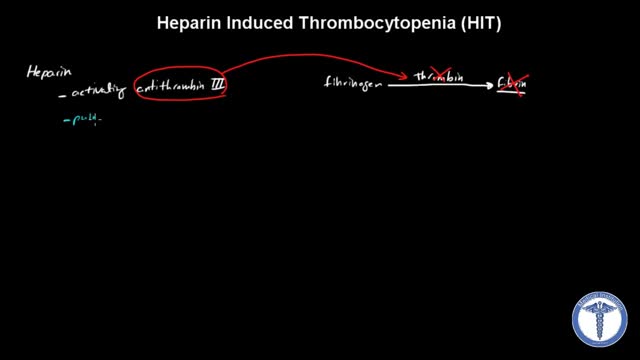
All forms of heparin (including low-molecular-weight heparin such as enoxaparin) must be stopped immediately in patients with suspected heparin-induced thrombocytopenia (HIT) while awaiting diagnostic confirmation. Patients with HIT remain at high risk of thrombosis even after discontinuation of heparin. Therefore, an alternate, rapidly acting, non-heparin anticoagulant such as direct thrombin inhibitor (eg, argatroban, bivalirudin) must be started immediately.