Top videos

http://sciatica-rimedi.good-info.co Nervo Sciatico, Accavallamento Nervi, Lombosciatalgia Sintomi E Cure, Dolore Coscia, Sciatica. Come curare la sciatica a casa Se hai avuto abbastanza sciatalgia a dirigere la tua vita, non disperare! ti mostrerò tre dei più comuni trattamenti casalinghi per la sciatica, e come usarli per ridurre il dolore in modo rapido. La parte migliore di questi trattamenti è che possono curare la sciatica, e non solo coprire il dolore. Quindi, cominciamo... 1. Programma di esercizi a casa I programmi di esercizio sono una componente importante di qualsiasi piano di trattamento della sciatica. Con l'allungamento e il rafforzamento di parti del corpo che possono causare l'irritazione del nervo sciatico, è possibile ridurre il dolore e accelerare il recupero. Gli esercizi più efficaci dipendono dalla ragione di fondo per cui soffri di sciatica. La sciatica causata da un'ernia del disco, per esempio, non viene trattata con gli stessi esercizi della sciatica causata da stenosi spinale. È anche importante mantenere il corpo rilassato, per consentirgli di guarire. Un modo grandioso per farlo, senza aggravare la tua condizione, è camminare a ritmo sostenuto. Altre attività leggere possono avere un effetto simile, ma se qualcosa fa male è necessario fermarsi immediatamente. Suggerimento gratuito: è essenziale che non ci si riduca a letto a causa del dolore. Stare sdraiati a letto per più di due giorni ha dimostrato peggiorare la sciatica, perché i muscoli si irrigidiscono e si indeboliscono. 2. Bilancia la tua dieta Curare la sciatica in modo permanente, spesso significa trattare più che la semplice causa fisica. Per impedire che il dolore si ripresenti, dovrai anche migliorare la tua dieta. Uno dei modi più semplici per ridurre il dolore associato con sciatica è quello di bere più acqua. Quando si è disidratati, parti della colonna vertebrale si sgonfiano. Questo può causare ulteriore pressione sul nervo sciatico. Se possibile, si dovrebbe anche cercare di evitare alimenti infiammatori. Gli alimenti infiammatori sono troppi, per elencarli in questo articolo, ma qualsiasi alimento dotato di elevato contenuto di zucchero può, potenzialmente, portare a infiammazione e ad aumento del dolore. 3. Rimedi casalinghi I rimedi casalinghi possono fare una grande differenza per tua sciatalgia, spesso in tempi relativamente brevi. La cosa grandiosa dei rimedi casalinghi è che non richiedono prescrizione o ingredienti costosi. Uno dei più semplici rimedi casalinghi sono le noccioline. Questo perché le arachidi contengono un sacco di magnesio, che è cruciale per consentire muscoli di rilassarsi.
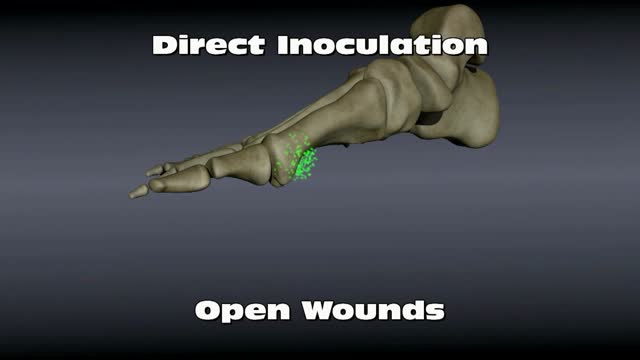
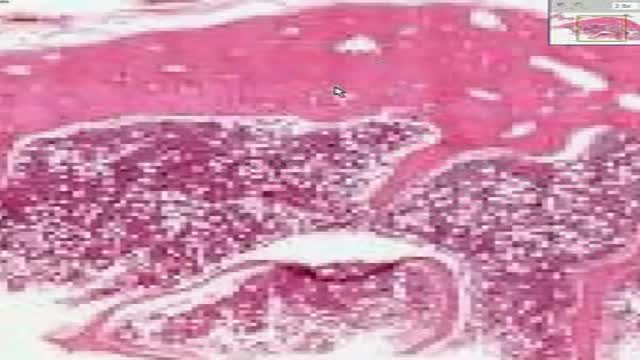
Osteomyelitis is an infection in a bone. Infections can reach a bone by traveling through the bloodstream or spreading from nearby tissue. Infections can also begin in the bone itself if an injury exposes the bone to germs. In children, osteomyelitis most commonly affects the long bones of the legs and upper arms. Adults are more likely to develop osteomyelitis in the bones that make up the spine (vertebrae). People who have diabetes may develop osteomyelitis in their feet if they have foot ulcers. Once considered an incurable condition, osteomyelitis can be successfully treated today. Most people require surgery to remove parts of the bone that have died — followed by strong antibiotics, often delivered intravenously, typically for at least four to six weeks.

The ACL is one of the four main ligaments within the knee that connect the femur to the tibia. The knee is essentially a hinged joint that is held together by the medial collateral (MCL), lateral collateral (LCL), anterior cruciate (ACL) and posterior cruciate (PCL) ligaments.

Vitamin E is an antioxidant. It may help protect your cells from damage. This essential nutrient occurs naturally in many foods. It’s also available as a dietary supplement. Sometimes, it’s in processed foods. Vitamin E is fat-soluble. This means your body stores and uses it as needed. The term “vitamin E” describes eight different compounds. Alpha-tocopherol is the most active one in humans
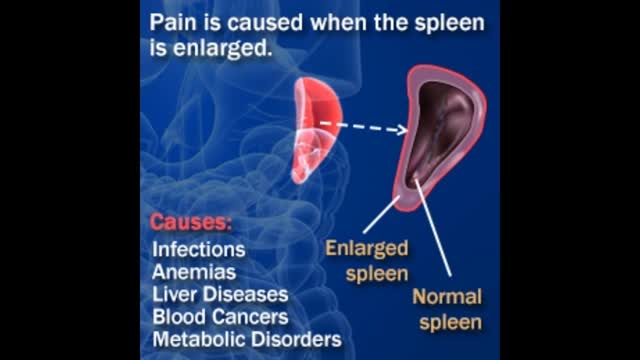
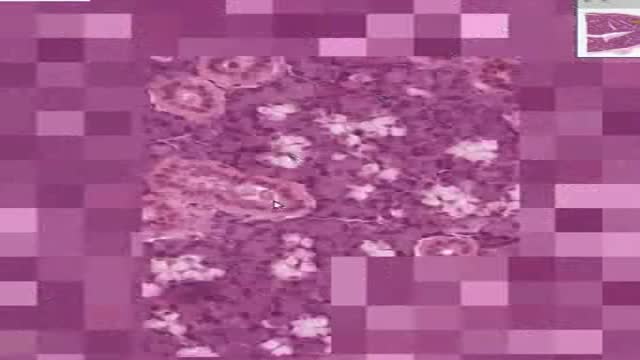
An enlarged spleen can be caused by infections, cirrhosis and other liver diseases, blood diseases characterized by abnormal blood cells, problems with the lymph system, or other conditions. Other causes of an enlarged spleen include: Inflammatory diseases such as sarcoidosis, lupus, and rheumatoid arthritis.

From the moment the baby weight starts to accumulate on our bodies, the scheming begins about how to drop the pounds once the little one arrives. After your baby is born and your days gradually begin to regain somewhat of a routine, it's time to put your ideas into action. If you're not sure exactly how to begin, here are seven proven steps for working your way back to your prepregnancy bod—or better!

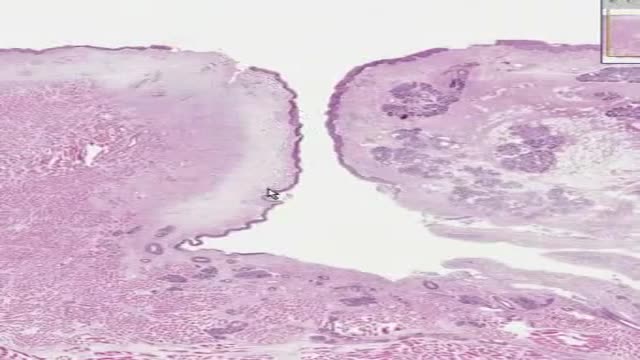
Pruritis is itchy skin that makes you want to scratch. It can be caused by many things. Normally, itchy skin isn't serious, but it can make you uncomfortable. Sometimes, itchy skin is caused by a serious medical condition. It can occur in association with a primary rash (e.g. dermatitis) or may occur because of hypersensitive nerves in the skin (neuropathic pruritus). ... Scratching a localised itch may lead to lichen simplex, prurigo or prurigo nodularis. Systemic causes of pruritus. Sytemic diseases may cause generalised pruritus.
A hormone is a chemical messenger that enables communication between cells. Hormones are secreted by the glands of the endocrine system and they serve to maintain homeostasis and to regulate numerous other systems and processes, including reproduction and development.
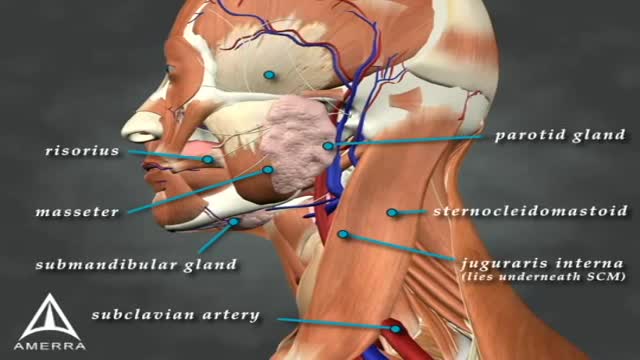
Sialorrhea or excessive drooling is a major issue in children with cerebral palsy and adults with neurodegenerative disorders. In this review, we describe the clinical features, anatomy and physiology of sialorrhea, as well as a review of the world literature on medical treatment using Yale University’s search engine; including but not limited to Medline and Erasmus. Level of drug efficacy is defined according to the guidelines of American Academy of Neurology. Current medical management is unsatisfactory. Topical agents (scopolamine and tropicamide) and oral agents (glyccopyrolate) combined render a level B evidence (probably effective); however, this treatment is associated with troublesome side effects. Double-blind and placebo-controlled studies of botulinum toxin (BoNT) provide a level A evidence for type B (two class I studies; effective and established) and both overall and individual B level of evidence for OnabotulinumtoxinA (A/Ona) and AbobotulinumtoxinA (A/Abo); these are probably effective. For IncobotulinumtoxinA (A/Inco), the level of evidence is U (insufficient) due to lack of blinded studies. Side effects are uncommon; transient and comparable between the two types of toxin. A clinical note at the end of this review comments on fine clinical points. Administration of BoNTs into salivary glands is currently the most effective way of treating sialorrhea.

When food is taken, it is broken down into smaller components. Sugars and carbohydrates are thus broken down into glucose for the body to utilize them as an energy source. The liver is also able to manufacture glucose. In normal persons the hormone insulin, which is made by the beta cells of the pancreas, regulates how much glucose is in the blood. When there is excess of glucose in blood, insulin stimulates cells to absorb enough glucose from the blood for the energy that they need. Insulin also stimulates the liver to absorb and store any excess glucose that is in the blood. Insulin release is triggered after a meal when there is a rise in blood glucose. When blood glucose levels fall, during exercise for example, insulin levels fall too. High insulin will promote glucose uptake, glycolysis (break down of glucose), and glycogenesis (formation of storage form of glucose called glycogen), as well as uptake and synthesis of amino acids, proteins, and fat. Low insulin will promote gluconeogenesis (breakdown of various substrates to release glucose), glycogenolysis (breakdown of glycogen to release gluose), lipolysis (breakdown of lipids to release glucose), and proteolysis (breakdown of proteins to release glucose). Insulin acts via insulin receptors.

On the day of your surgery, your health care team will take you to a preparation room. Your blood pressure and breathing will be monitored. You may receive an antibiotic medication through a vein in your arm. You will then be taken to an operating room and positioned on a table. You'll be given a general anesthesia medication to put you in a sleep-like state so that you won't be aware during your operation. The surgical team will then proceed with your colectomy. Colon surgery may be performed in two ways: Open colectomy. Open surgery involves making a longer incision in your abdomen to access your colon. Your surgeon uses surgical tools to free your colon from the surrounding tissue and cuts out either a portion of the colon or the entire colon. Laparoscopic colectomy. Laparoscopic colectomy, also called minimally invasive colectomy, involves several small incisions in your abdomen. Your surgeon passes a tiny video camera through one incision and special surgical tools through the other incisions. The surgeon watches a video screen in the operating room as the tools are used to free the colon from the surrounding tissue. The colon is then brought out through a small incision in your abdomen. This allows the surgeon to operate on the colon outside of your body. Once repairs are made to the colon, the surgeon reinserts the colon through the incision. The type of operation you undergo depends on your situation and your surgeon's expertise. Laparoscopic colectomy may reduce the pain and recovery time after surgery. But not everyone is a candidate for this procedure. Also, in some situations your operation may begin as a laparoscopic colectomy, but circumstances may force your surgical team to convert to an open colectomy. Once the colon has been repaired or removed, your surgeon will reconnect your digestive system to allow your body to expel waste. Options may include: Rejoining the remaining portions of your colon. The surgeon may stitch the remaining portions of your colon together, creating what is called an anastomosis. Stool then leaves your body as before. Connecting your intestine to an opening created in your abdomen. The surgeon may attach your colon (colostomy) or small intestine (ileostomy) to an opening created in your abdomen. This allows waste to leave your body through the opening (stoma). You may wear a bag on the outside of the stoma to collect stool. This can be permanent or temporary. Connecting your small intestine to your anus. After removing both the colon and the rectum (proctocolectomy), the surgeon may use a portion of your small intestine to create a pouch that is attached to your anus (ileoanal anastomosis). This allows you to expel waste normally, though you may have several watery bowel movements each day. As part of this procedure, you may undergo a temporary ileostomy.