Top videos

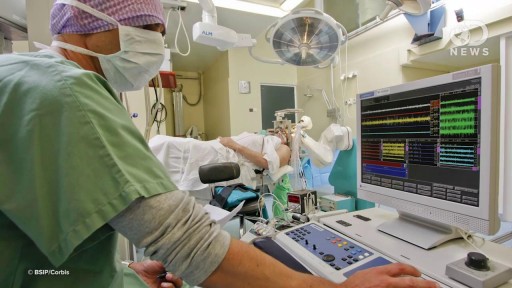
The pelvic floor or pelvic diaphragm is composed of muscle fibers of the levator ani, the coccygeus, and associated connective tissue which span the area underneath the pelvis. The pelvic diaphragm is a muscular partition formed by the levatores ani and coccygei, with which may be included the parietal pelvic fascia on their upper and lower aspects. The pelvic floor separates the pelvic cavity above from the perineal region (including perineum) below.
The right and left levator ani lie almost horizontally in the floor of the pelvis, separated by a narrow gap that transmits the urethra, vagina, and anal canal. The levator ani is usually considered in three parts: pubococcygeus, puborectalis, and iliococcygeus. The pubococcygeus, the main part of the levator, runs backward from the body of the pubis toward the coccyx and may be damaged during parturition. Some fibers are inserted into the prostate, urethra, and vagina. The right and left puborectalis unite behind the anorectal junction to form a muscular sling . Some regard them as a part of the sphincter ani externus. The iliococcygeus, the most posterior part of the levator ani, is often poorly developed.
The coccygeus, situated behind the levator ani and frequently tendinous as much as muscular, extends from the ischial spine to the lateral margin of the sacrum and coccyx.
The pelvic cavity of the true pelvis has the pelvic floor as its inferior border (and the pelvic brim as its superior border.) The perineum has the pelvic floor as its superior border.
Some sources do not consider “pelvic floor” and “pelvic diaphragm” to be identical, with the “diaphragm” consisting of only the levator ani and coccygeus, while the “floor” also includes the perineal membrane and deep perineal pouch. However, other sources include the fascia as part of the diaphragm. In practice, the two terms are often used interchangeably.
Inferiorly, the pelvic floor extends into the anal triangle.

A tummy tuck is a surgical process that removes excess fat and skin. Learn more about the procedure by watching this video!
Looking to book a consultation? Call Zuri Plastic Surgery now at 786-804-1603 or DM us today to schedule a complimentary consultation with Dr. Z.
Un tummy tuck es un procedimiento quirúrgico que elimina el exceso de grasa y piel. ¡Aprenda más sobre este procedimiento viendo este video!
¿Quiere agendar una consulta? Llame a Zuri Plastic Surgery ahora al 786-804-1603 o envíenos un DM hoy para programar una consulta gratuita con el Dr. Z.
This video has been updated to include an alternate name for the internal thoracic arteries. View the updated video here: https://youtu.be/kxc22Fjd1NQ
For Employees of Hospitals, Schools, Universities and Libraries: Download 8 FREE medical animations from Nucleus by signing up for a free trial: http://nmal.nucleusmedicalmedi....a.com/free-trial-mem
Biology students: Subscribe to the Nucleus Biology channel to see new animations on biology and other science topics, plus short quizzes to ace your next exam: https://bit.ly/3lH1CzV
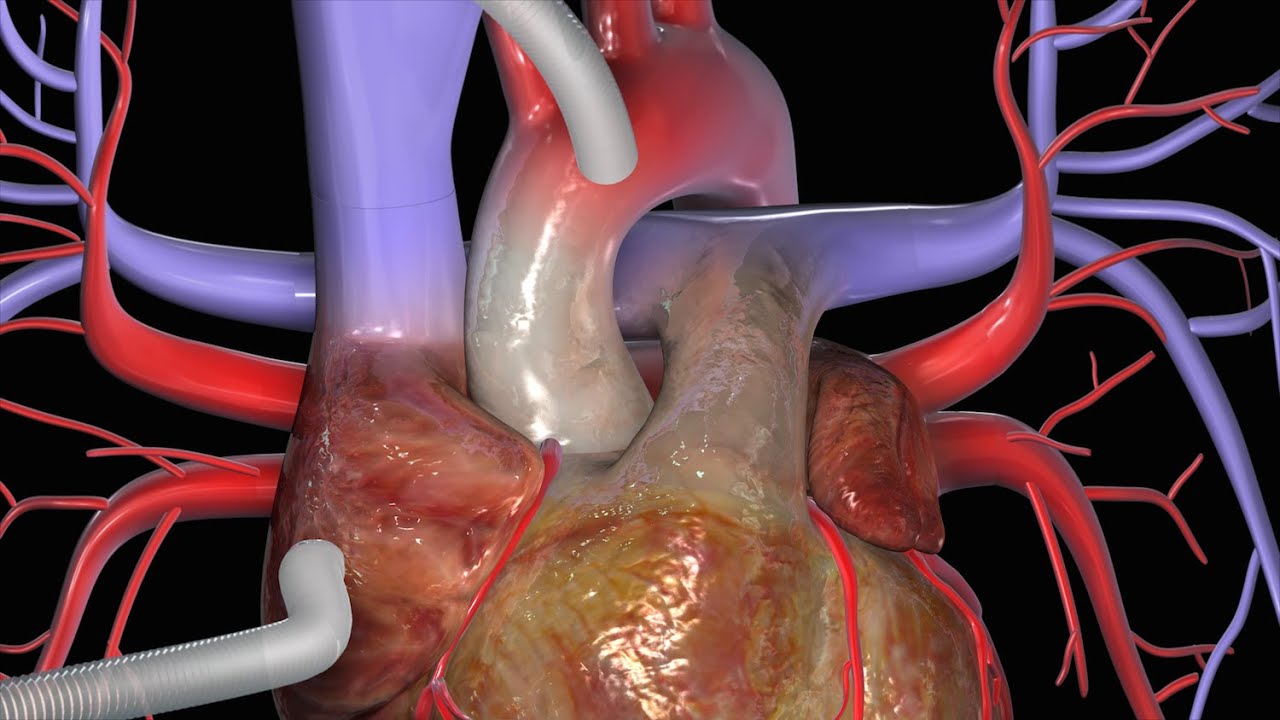
This video, created by Nucleus Medical Media, shows a coronary artery bypass graft (CABG) procedure used to combat coronary artery disease. Beginning with a midline sternal incision, the heart is connected to a perfusion machine which will take over the duties of the heart while the surgery takes place. Two different grafts are used to bypass the blocked coronary arteries: the internal thoracic artery from inside the chest wall, and the saphenous vein from the leg. After the procedure, the heart is shocked to restart its beating. A drainage tube is left at the incision site to drain away excess fluid. The animation continues to show two other types of approaches to a coronary artery bypass graft, off-pump bypass surgery and minimally invasive bypass surgery.
This is similar to the procedure performed on former president Bill Clinton and former California governor Arnold Schwarzenegger.
#HeartBypassSurgery #CABG #heart
ANCE00199

A new well designed randomized study has suggested that long term baby aspirin usage may aid in fight against cancer. The suggested mechanism is that cancers induce inflammatory responses so the anti-inflammatory mechanism of prostaglandins inhibitors may cease the progress of many cancers. There are some concerns about the study because despite the well-designed randomized study; the study didn't include a satisfying number of female participants. The study was also conducted on esophageal, colorectal and lung cancers.

MRCPCH Clinical Revision - more videos at http://mrcpch.paediatrics.co.uk
Revise for your MRCPCH Clinical exam, with videos and high quality content created by the London Paediatrics Trainees Committee.
Examiner: Jonathan Round
Candidate: Amitav Parida
Filming: Mary Chesshyre, Huey Miin Lee, Chris Kelly
Thank you to the Evelina Children's Hospital for allowing us to film during their MRCPCH Revision Course (https://www.guysandstthomaseve....nts.co.uk/mrcpch-cli

Dilation and curettage (D&C) is a procedure to remove tissue from inside your uterus. Doctors perform dilation and curettage to diagnose and treat certain uterine conditions — such as heavy bleeding — or to clear the uterine lining after a miscarriage or abortion. In a dilation and curettage — sometimes spelled "dilatation" and curettage — your doctor uses small instruments or a medication to open (dilate) your cervix — the lower, narrow part of your uterus. Your doctor then uses a surgical instrument called a curette to remove uterine tissue. Curettes used in a D&C can be sharp or use suction

plantar fasciitis and calcaneal spur can be treated by EPFR with calcanean drilling - endoscopic plantar fascia release علاج الشوكة العظمية للكعب بالمنظار د. أسامة الشاذلي مدرس جراحة العظام واستشاري جراحات و مناظير القدم والكاحل كلية الطب جامعة عين شمس
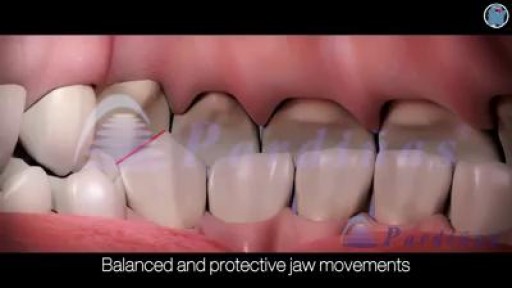
Your temporomandibular joint is a hinge that connects your jaw to the temporal bones of your skull, which are in front of each ear. It lets you move your jaw up and down and side to side, so you can talk, chew, and yawn. Problems with your jaw and the muscles in your face that control it are known as temporomandibular disorders (TMD). But you may hear it wrongly called TMJ, after the joint.
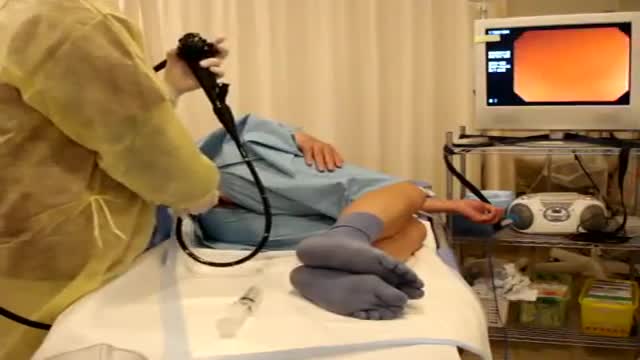
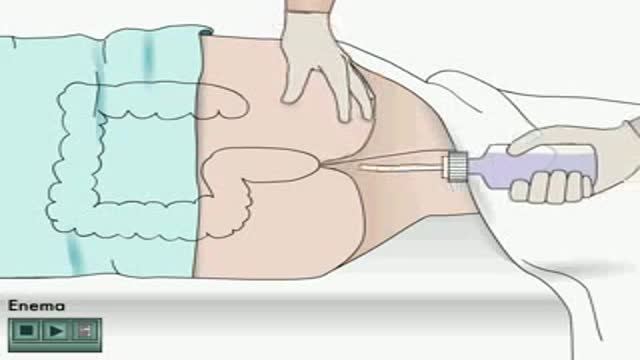
Colonoscopy is a test that allows your doctor to look at the inner lining of your large intestine (rectum and colon). He or she uses a thin, flexible tube called a colonoscope to look at the colon. A colonoscopy helps find ulcers, colon polyps, tumors, and areas of inflammation or bleeding.