Top videos
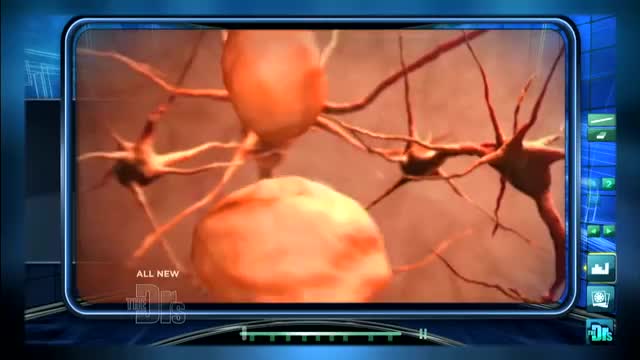
Memory Loss & the Brain. It's not just a movement disorder. Besides causing tremors and other motion-related symptoms, Parkinson's disease affects memory, learning, and behavior. Parkinson's disease is notorious for so-called motor symptoms like muscle rigidity, tremor, slowed movement, and unsteady posture and gait.
Shoulder dystocia is a rare emergency that can happen during the end of the second stage of labour. It's all to do with how your baby moves down through your vagina and out into the world. Shoulder dystocia happens when your baby's head has been born, but one of her shoulders becomes stuck.
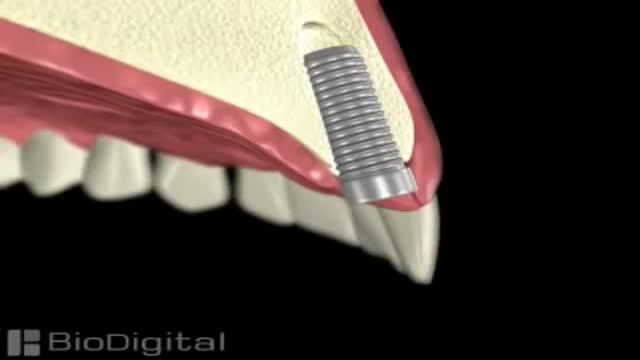
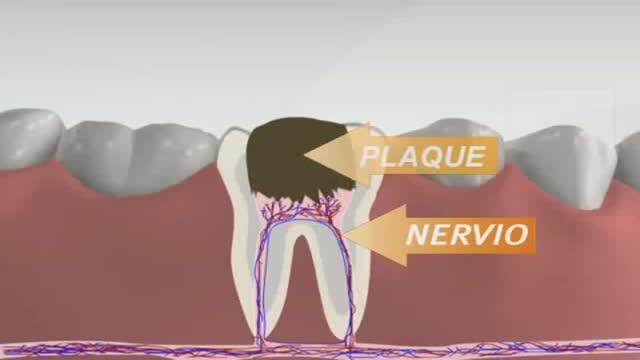
If you are self-conscious because you have missing teeth, wear dentures that are uncomfortable or don't want to have good tooth structure removed to make a bridge, talk to your dentist to see if dental implants are an option for you. Dental implants are a popular and effective way to replace missing teeth and are designed to blend in with your other teeth. They are an excellent long-term option for restoring your smile. In fact, the development and use of implants is one of the biggest advances in dentistry in the past 40 years. Dental implants are made up of titanium and other materials that are compatible with the human body. They are posts that are surgically placed in the upper or lower jaw, where they function as a sturdy anchor for replacement teeth.

In most instances, STDs are passed from an infected person to another person during sexual activities, through contact with the mucous membranes of the penis, vagina, mouth and rectum. Such activity includes vaginal, oral and anal intercourse. Gonorrhea and chlamydia also can be transmitted by fingers to eyes. A sexually transmissible infection (STI) is any infection or disease that can be passed from one person to another during sexual activity. Sexually transmissible infections include chlamydia, herpes, gonorrhoea, syphilis, genital herpes, scabies, pubic lice (crabs), hepatitis and HIV (the virus that causes AIDS).
Alzheimer's worsens over time. Alzheimer's is a progressive disease, where dementia symptoms gradually worsen over a number of years. In its early stages, memory loss is mild, but with late-stage Alzheimer's, individuals lose the ability to carry on a conversation and respond to their environment. Alzheimer's is the sixth leading cause of death in the United States. Those with Alzheimer's live an average of eight years after their symptoms become noticeable to others, but survival can range from four to 20 years, depending on age and other health conditions. Alzheimer's has no current cure, but treatments for symptoms are available and research continues. Although current Alzheimer's treatments cannot stop Alzheimer's from progressing, they can temporarily slow the worsening of dementia symptoms and improve quality of life for those with Alzheimer's and their caregivers. Today, there is a worldwide effort under way to find better ways to treat the disease, delay its onset, and prevent it from developing. Alzheimer's has no current cure, but treatments for symptoms are available and research continues. Although current Alzheimer's treatments cannot stop Alzheimer's from progressing, they can temporarily slow the worsening of dementia symptoms and improve quality of life for those with Alzheimer's and their caregivers. Today, there is a worldwide effort under way to find better ways to treat the disease, delay its onset, and prevent it from developing.
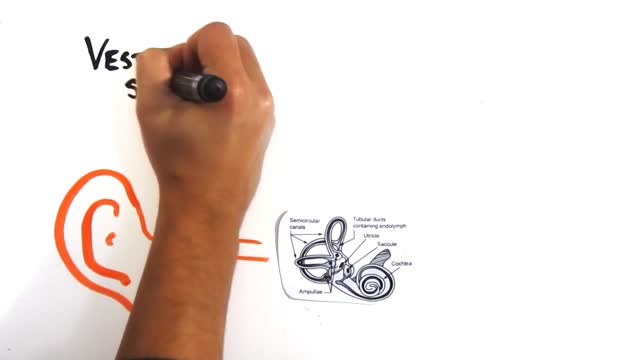
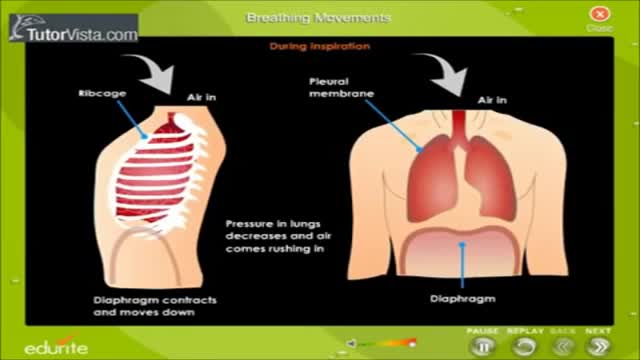
You get motion sickness when one part of your balance-sensing system (your inner ear , eyes, and sensory nerves) senses that your body is moving, but the other parts don't. For example, if you are in the cabin of a moving ship, your inner ear may sense the motion of waves, but your eyes don't see any movement.
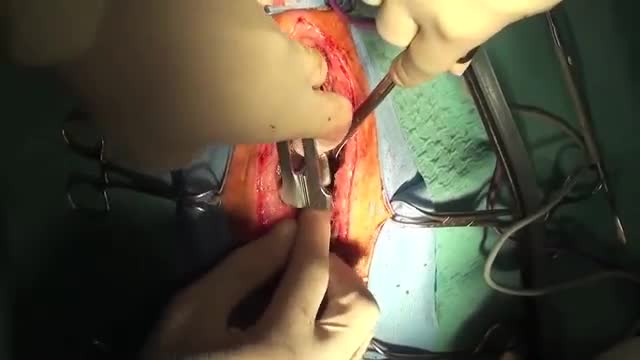
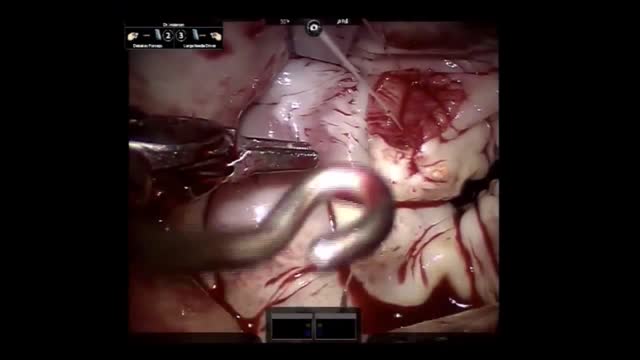
Thymoma is a tumor originating from the epithelial cells of the thymus. Thymoma is an uncommon tumor, best known for its association with the neuromuscular disorder myasthenia gravis; thymoma is found in 20% of patients with myasthenia gravis. Once diagnosed, thymomas may be removed surgically.

Waardenburg syndrome is a group of genetic conditions that can cause hearing loss and changes in coloring (pigmentation) of the hair, skin, and eyes. Although most people with Waardenburg syndrome have normal hearing, moderate to profound hearing loss can occur in one or both ears. The hearing loss is present from birth (congenital). People with this condition often have very pale blue eyes or different colored eyes, such as one blue eye and one brown eye. Sometimes one eye has segments of two different colors. Distinctive hair coloring (such as a patch of white hair or hair that prematurely turns gray) is another common sign of the condition. The features of Waardenburg syndrome vary among affected individuals, even among people in the same family.

An intelligence quotient (IQ) is a total score derived from one of several standardized tests designed to assess human intelligence. IQ is a number meant to measure people cognitive abilities (intelligence) in relation to their age group. An I.Q between 90 and 110 is considered average; over 120, superior. Roughly 68% of the population has an IQ between 85 and 115. The average range between 70 and 130, and represents about 95% of the population.

1500 mg of sodium amounts to 0.75 teaspoons or 3.75 grams of salt per day, while 2300 mg amounts to one teaspoon or 6 grams of salt per day. Most people today are eating much more than that. The average intake of sodium is about 3400 mg, most of it coming from processed foods.
Pompe disease is a rare multisystem genetic disorder that is characterized by absence or deficiency of the lysosomal enzyme alpha-glucosidase (GAA). This enzyme is required to breakdown (metabolize) the complex carbohydrate glycogen and convert it into the simple sugar glucose.