Top videos
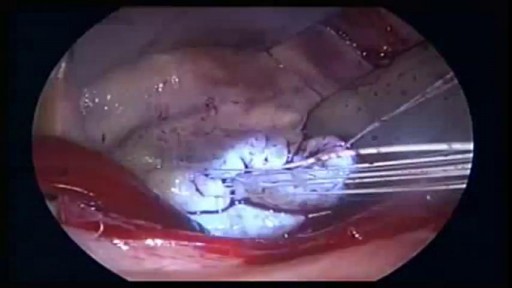
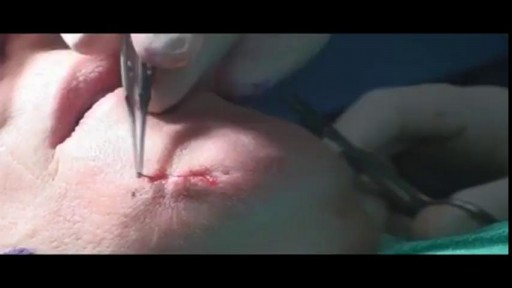
There are several ways to do minimally invasive aortic valve surgery. Techniques include min-thoracotomy, min-sternotomy, robot-assisted surgery, and percutaneous surgery. To perform the different procedures: Your surgeon may make a 2-inch to 3-inch (5 to 7.5 centimeters) cut in the right part of your chest near the sternum (breastbone). The muscles in the area will be divided. This lets the surgeon reach the heart and aortic valve. Your surgeon may split only the upper portion of your breast bone allowing exposure to the aortic valve. For robotically-assisted valve surgery, the surgeon makes 2 to 4 tiny cuts in your chest. The surgeon uses a special computer to control robotic arms during the surgery. A 3D view of the heart and aortic valve are displayed on a computer in the operating room.

Runners Knee Overview:
Welcome to our Patello-Femoral Rehab video. The goal of this video is to minimize pain around the kneecap and maximize recovery. This video should not be used as a substitute for regular physical therapy visits and guidance from your physician
Visit http://www.matthewboesmd.com/p....atello-femoral-rehab for more information

Blackheads are small bumps that appear on your skin due to clogged hair follicles. These bumps are called “blackheads” because the surface looks dark or black. Blackheads are a mild type of acne that usually form on the face, but they can also appear on the back, chest, neck, arms, and shoulders
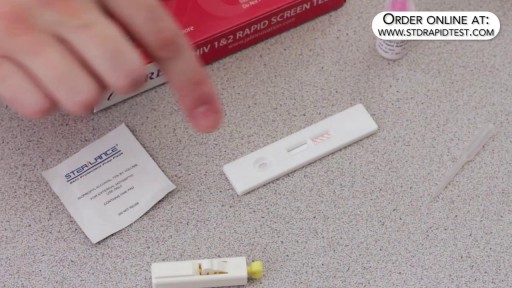
How to use a HIV rapid test kit for self-diagnosis of HIV (fingerstick blood). Convenient, Easy to Use, and over 99% Accurate. USAID approved. Test yourself at home with Complete Privacy. Buy online today at: http://www.stdrapidtest.com

A detailed description of Adrenal insufficiency (Addison's disease) including basic physiology of the HPA axis, causes of primary and secondary insufficiency, clinical features of acute and chronic adrenal insufficiency. Lab testing for Addison's disease is also dealt with in detail. The management, both short term and long term are discussed in detail.

Duke Sports Medicine Specialists Jocelyn Wittstein, MD, Janna Fonseca, ATC, and Michael Messer ,PT, present on Soccer Injury Prevention including Concussion Management and the 11+ program that significantly reduces ACL tear rates in soccer.

Hidradenitis Suppurativa Surgery, Hidradenitis Suppurativa Photos, Hidradenitis Suppurativa Nz. http://hidradenitis-suppurativa-cure.good-info.co --- symptoms of hidradenitis suppurativa: First let us look at the symptoms of the disease Black heads: When they appear in a double barreled pattern Red bumps: When tender lesions, or bumps, which often contain pus and/or itching. Hard, painful lumps: When pea sized lumps cause pain and get inflamed These recur very often Don’t heal or improve for weeks Returns after treatment Appears in several different locations The lumps are accompanied by pain I am going to reveal to you step by step how to understand and deal with the problems of hidradenitis suppurativa. click here http://hidradenitis-suppurativa-cure.good-info.co

Chicken Skin, Chicken Skin On Legs, Keratosis Pilaris Treatment Over The Counter, Kp Vitamin A--- http://banishmybumps.plus101.com/ --- What Causes KP? The particular cause of Keratosis Pilaris is unidentified. Usually, it happens when there is a difficulty on the production of the keratin that is called hyper keratinizatinization. Keratosis Pilaris is believed to be inherited partially in origin. About fifty percent up to seventy percent of patients with this type of skin condition have identified genetic predisposition and has a higher rate of affected members of the family. Most people have a solid family history of follicular pilaris. The primary cause may be related partly to hypersensitivity reactions as well as the overall skin dryness. This skin condition is closely related also to dry skin, allergies, asthma, eczema, atopic dermatitis and rhinitis. The red bumps in Keratosis Pilaris seem to rise from the unnecessary build-up of keratin dry skin particles and very small at the hair follicles opening. The skin as observed under the hand held microscope demonstrates mild condensing, plugging and hyperkeratosis of your hair follicle. Your upper skin layers may have a number of dilation of the minor superficial blood vessels. In this manner, it gives the skin a flushed or reddish appearance. Keratosis Pilaris is not infectious, therefore people surrounding you are safe from this irritating skin condition. The condition is worse during winter. Summer season is normally a reprieve as it brings moisture and usually allows the skin condition to smooth up more than normal. The aggravating is associated directly with lower moisture, tight clothes and skin dryness that cause to rub the red bumps all the times. Many people stated that this skin condition worsened during the period of pregnancy before and after child birth. Medical doctors and patients as well, believed that keratosis pilaris is also related to food intake. So, large intakes of spicy foods increase the form of red bumps that make them more visible. In some way, patients that eliminated or reduced milk as well as the derivatives from their balance diet stated the improvement of their condition. Keratosis Pilaris can be difficult to treat, but it is possible to seek permanent relief. New research shows that all-natural treatment systems, such as BanishMyBumps, are successful. You can learn more at http://banishmybumps.plus101.com/

Protopic Vitiligo, Weiße Flecken Am Rücken, Pigmentflecken Im Gesicht Entfernen, Flecken Haut--- http://vitiligo-heilung.info-pro.co --- Weiße Flecken auf der Haut: Vitiligo, Die Entwicklung weißer Flecken auf der Haut ist ist ein Symptom einer Hautstörung, die Vitiligo genannt, im deutschen Sprachgebrauch aber auch häufig als "Weißfleckenkrankheit" bezeichnet wird. Man bringt den Zustand mit der Zerstörung oder Fuktionsstörung der Hautzellen in Verbindung, die für die Herstelleung des Hautpigmentes (Melanin) zuständig sind, welches dem Menschen seine Hautfarbe verleiht. Meistens entwickeln sich die Flecken dabei an Stellen, die oft der Sonne ausgesetzt sind, also z.B. die Hände, Arme, Füße, Beine und das Gesicht. Bisweilen treten die Flecken aber auch in den Achselhöhlen, im Genitalbereich und um den Bauchnabel herum auf. Von Vitiligo betroffene erleben häufig auch ein vorzeitiges Ergrauen der Haare. Es wird geschätzt, dass mindestens 1 % der Bevölkerung der Vereinigten Staaten an Vitiligo leidet; in Europe sind die Zahlen ähnlich. Weltweit leiden gegenwärtig mehr als 100 Millionen Menschen an der Hauterkrankung. Die Ursache von Vitiligo Die genaue Ursache der Erkrankung ist noch immer unbekannt. Eine der populärsten Theorien ist jedoch, dass es sich bei Vitiligo um eine Autoimmunstörung handelt. Sie veranlasst das Immunsystem, die Melanozyten (die Hautpigmente produzierenden Hautzellen) anzugreifen. In der Tat haben Menschen, die an einer anderen Autoimmunstörung, wie adrenocorticaler Unterfunktion or Schilddrüsenüberfunktion leiden, ein weitaus höheres Risiko, auch an Vitiligo zu erkranken. Manche Mediziner sind auch der Auffassung, dass Sonnenbrände, emotionaler Stress und bestimte Medikamente die weißen hautflecken hervorrufen könnten. Es wird außerdem geglaubt, dass Vitiligo is also believed eine genetisch vererbte Erkrankung darstellt. Behandlungsoptionen für Vitiligo Für Vitiligo gibt es unterschiedliche Behandlungsmöglichkeiten. Allerdings sind sie allesamt praktisch wirkungslos und beinhalten dazu noch das Risiko, ernsthafte Nebenwirkungen hervorzurufen. Krankenversicherer übernehmen zudem die vollen Behandlungskosten. Das allein macht eine Vitiligo-Behandlung bereits zu teuer für die meisten Patienten, denn es sind üblichwerweise zwei bis drei Besuche wöchentlich in ener Spezialklinik nötig. Ein Paradebeispiel für eine solche Behandlung ist die sogenannte PUVA-Therapie, die ausgesprochen häufig eingesetzt wird. "Gratis-Präsentation enthüllt einen ziemlich ungewöhnlichen Tipp zur Beseitigung von Vitiligo für alle Zeiten und in nur 45-60 Tagen - Garantiert!" http://vitiligo-heilung.info-pro.co Erfahren Sie mehr darüber, indem Sie diese Webseite besuchen: http://vitiligo-heilung.info-pro.co

URBN Dental is at your service to provide professional dental tips and quality service. Do you ever wonder how often you should be changing your toothbrush (or toothbrush head if you are using an electric one)? Switching your electric head or tossing your toothbrush is recommended every three months. If you are sick or have a cold sore or canker sore, it’s highly suggested to also switch your brushes. The toothbrush bristles can contain a lot of harmful bacteria and need to be replaced to decrease your risk of potential systemic illnesses. Also the bristles themselves can get worn and frayed and will decrease the efficiency of the toothbrush. Without replacing the toothbrush bristles, you suffer from a greater risk of encountering gum disease and cavities, so be sure you swap those bristles! Schedule a dental appointment now to learn more! Click on our website to book today: https://www.urbndental.com/

Pictures Of Shingles, Images Of Shingles, Cause Of Shingles, Can You Catch Shingles, Cause Shingles --- http://shingles-cure.good-info.co/ ---- Home Remedy For Shingles Treatment. There are surprisingly diverse amounts of treatments that can be used for viruses, especially one in particular known as Shingles. Shingles is the type of virus that is annoyingly unpredictable. Some people get it while others do not, and while it predominant after a certain age, most people can go their whole lives without ever seeing a hint of it. Yet, we all have it living inside of us. The first step to treating the virus correctly is to understand what can set it off. The first pre-requisite is to have had chicken-pox before. Most things manage to squeeze through an immune system if it is weak enough and the shingles virus is no different. In some cases that can kill someone with a weak enough system The shingles virus can also ‘wake up’ if sufficient levels of stress agitate a person’s immune system. As mentioned before, the virus is unpredictable, and even if you meet all the requirements you could go through your entire life without one outbreak. The second step to treating the virus is catching it in time. 72 hours after you first begin to notice symptoms of shingles is pushing your luck so within that time frame some type of treatment should be instigated. For the most part, for a disease like shingles, the main source of relief comes from skin creams and pain killers. Neither of which is a cure for the pain, but which do happen to fall under the heading of ‘home remedy’ Wet rags can be used to soothe the inflamed and tender skin, and a binding with a substance known as aluminum acetate can protect the infected area without causing further irritation. Calamine lotion is a fail safe for almost any sort of skin irritation so it would be smart to go through the aisles at your local grocery store to find products similar. Then of course there are the most obvious measures that need to be taken during your do it yourself treatment sessions. Stay out of the sun since the heat and UV rays can cause unbearable pain against already brutalized skin. Also, keep yourself from scratching at the area since, like the chicken-pox, you will only end up making it worse. If you do not believe me then consider the unlucky individuals who do not have the rash on a small area, but rather all over their bodies. Anti-itch cream would probably be more than appreciated at that point. Should the time come where the virus is making repeated appearances, then it may be time to throw in the towel and head for the hospital. The reason is that after the first outbreak, it isn’t unusual that the virus that was originally stored in the roots of your nerves ‘burned’ itself out. However, continual outbreaks are indications of something deeper that can only grow worse as the attacks continue. Some victims of the virus have described the sensation as having your flesh eaten from the inside out. Once the pain reaches that level, stubbornness should be put on the backburner. If you are forced to go to your local doctor, you may be provided with some of the medicines that have recently been created to help fight off shingles. They are by no means brand names, but neither are they over the counter drugs either. After a few more years to study their effectiveness, there is no reason why this new medication cannot ease the pain caused by shingles, and even, eventually cure it. In this presentation, shows you some unique and rare methods to get rid of shingles naturally in as little as 14 days! This is based on proven techniques used by shingles sufferers without the use of pills and other medication. Get Rid of Shingles will also boost your energy and health dramatically and improve the quality of your life. IMPORTANT NOTE: I can't leave this video up for long, so be sure to watch it from beginning to end while it's still here. REMEMBER: Watch the whole video, as the ending will pleasantly surprise you. click here: http://shingles-cure.good-info.co/

Is Shingles Contagious, What Are Shingles, Herpes Zoster Pictures, Shingles Home Remedies --- http://shingles-cure.good-info.co/ --- If You Are A Newcomer To This Disease, I Hate To Be The Bringer Of Bad News But You Should Know That The List Of Potential Symptoms Is Depressingly Long. These Include The Following: A General Feeling Of Muscle Pain To Begin With, Almost Like Flu A Tingling, Burning Type Sensation In A Specific Area Of The Skin Fever And Headache And Sometimes A Swelling Of The Lymph Nodes A Band Of Spots And Then A Rash At A Specific Part Of Your Body – Very Often The Head Or The Side Of The Trunk Infection Over The Site Of The Rash – Leaving It Prone To Additional Tissue Damage From Bacteria Postherpetic neuralgia leading to chronic nerve pain Ulceration Of The Eye – In Those Cases Where The Shingles Rash Occurs In The Area Of The Eye – Known As Zoster Ophthalmicus. Stress And Depression – Particularly Where The Illness Lingers On For A Long Period Everyone Is Different And Not Everyone Will Experience All Of Those Symptoms. However Even The Most Mild Case Of Shingles Can Be Extremely Debilitating – Something Of Which I Am All Too Aware. Tired Of Fighting A Never Ending Battle Against Shingles? Sick Of Being Told That There´s Nothing You Can Do To Speed Up Recovery? Wherever You Are In Your Fight Against Shingles, I Can Help In this presentation, shows you some unique and rare methods to get rid of shingles naturally in as little as 14 days! This is based on proven techniques used by shingles sufferers without the use of pills and other medication. Get Rid of Shingles will also boost your energy and health dramatically and improve the quality of your life. IMPORTANT NOTE: I can't leave this video up for long, so be sure to watch it from beginning to end while it's still here. REMEMBER: Watch the whole video, as the ending will pleasantly surprise you. click here: http://shingles-cure.good-info.co/

Verrugas Genitales, Verrugas Del Papiloma Humano, Verrugas En El Cuerpo, Como Eliminar Lunares -- http://sinverrugasylunares.plus101.com --- El Nitrógeno Liquido Es Seguro Para Eliminas Tus Verrugas? Dentro de los tratamientos para las verrugas que la medicina convencional ofrece existe la crioterapia el cual se utiliza nitrógeno líquido. Este tratamiento es de los más comunes que se utilizan para remover las verrugas, este tratamiento debe ser administrado por un profesional especializado. Ya que si se hace sin la supervisión adecuada puede provocar severos daños en la piel. El tratamiento se aplica de la forma siguiente: Se aplica sobre la verruga un poco de nitrógeno líquido ya sea en aerosol o con un algodón, teniendo cuidado de no aplicar a áreas sanas de la piel, esto debido a que el nitrógeno líquido puede afectar severamente a la piel sana, es por eso que debe ser aplicado por un profesional. Para eliminar la verruga serán necesarias varias aplicaciones, al cabo de 2 a 3 semanas la verruga se caerá dejando una costra sobre la piel. Las molestias sobre este tratamiento depende mucho del especialista que lo aplique, existen casos en que a sido doloroso porque el médico a rociado nitrógeno líquido en las partes alrededor de la verruga, lo cual produce un severo daño a la piel, eso sin contar la costra que se forma en la parte donde estuvo la verruga después de que esta se cayera. Generalmente el dolor es mínimo pero también se tiene la opción de aplicar anestesia local sobre la parte afectada. Tu sistema inmunológico es un arma poderosa contra todas las infecciones que existen, pero lamentablemente no le damos el debido mantenimiento q ue necesita para poder luchar contra las infecciones virales. Te invito a conocer esta guía aquí: http://sinverrugasylunares.plus101.com