Top videos
![Histology of Exocrine Gland [Epithelium 7 of 7]](https://i.ytimg.com/vi/NkU7YJ7eYd0/maxresdefault.jpg)
Histological features and cellular biology of exocrine glands. This video is a part of our Histology Video Course (https://youtube.com/playlist?l....ist=PLnr1l7WuQdDynxT
Additional YouTube Content
Biochemistry videos: https://youtube.com/playlist?l....ist=PLnr1l7WuQdDzCUC
Anatomy Videos: https://youtube.com/playlist?l....ist=PLnr1l7WuQdDz2dK
DaVinci Cases Videos: https://youtube.com/playlist?l....ist=PLnr1l7WuQdDyJUl
The DaVinci Hour Podcast: https://youtube.com/playlist?l....ist=PLnr1l7WuQdDwSm9
DaVinci Academy Website: https://www.dviacademy.com/
Venous cutdown is an emergency procedure in which the vein is exposed surgically and then a cannula is inserted into the vein under direct vision. It is used to get vascular access in trauma and hypovolemic shock patients when peripheral cannulation is difficult or impossible
3D scans show still pictures of your baby in three dimensions. 4D scans show moving 3D images of your baby, with time being the fourth dimension. It's natural to be really excited by the prospect of your first scan. But some mums find the standard 2D scans disappointing when all they see is a grey, blurry outline.

WATCH MORE NURSING SKILLS HERE: https://nursing.com/course/nursing-skills/?utm_source=youtube&utm_medium=social
In our Nursing Skills course, we show you the most common and most important skills you will use as a nurse! We included everything from bed baths, to inserting a foley, to advanced skills like chest tube management.
Welcome to the NURSING Family, we call it the most supportive nursing cohort on the planet.
At NURSING.com, we want to help you remove the stress and overwhelm of nursing school so that you can focus on becoming an amazing nurse.
Check out our freebies and learn more at: (http://www.nursing.com)
Visit us at http://www.nursing.com/medical....-information-disclai for disclaimer information.
NCLEX®, NCLEX-RN® are registered trademarks of the National Council of State Boards of Nursing, INC. and hold no affiliation with NURSING.

The HEENT, or Head, Eye, Ear, Nose and Throat Exam is usually the initial part of a general physical exam, after the vital signs. Like other parts of the physical exam, it begins with inspection, and then proceeds to palpation. It requires the use of several special instruments in order to inspect the eyes and ears, and special techniques to assess their special sensory function. This module reviews some of the relevant surface anatomy and describes the basic HEENT exam. The module includes an introduction to use of the ophthalmoscope.

Sebaceous cysts are common noncancerous cysts of the skin. Cysts are abnormalities in the body that may contain liquid or semiliquid material. Sebaceous cysts are mostly found on the face, neck, or torso. They grow slowly and are not life-threatening, but they may become uncomfortable if they go unchecked. Doctors usually diagnose a cyst with only a physical examination and medical history. In some cases, a cyst will be examined more thoroughly for signs of cancer

Learn Basic Laparoscopic Surgery, the components of a laparoscopic surgical setup, optimal positioning and ergonomics in laparoscopic surgery, and much more. Check out the full course for free here: https://www.incision.care/free-trial
What is Laparoscopic Surgery:
Laparoscopic surgery describes procedures performed using one or multiple small incisions in the abdominal wall in contrast to the larger, normally singular incision of laparotomy. The technique is based around principles of minimally invasive surgery (or minimal access surgery): a large group of modern surgical procedures carried out by entering the body with the smallest possible damage to tissues. In abdominopelvic surgery, minimally invasive surgery is generally treated as synonymous with laparoscopic surgery as are procedures not technically within the peritoneal cavity, such as totally extraperitoneal hernia repair, or extending beyond the abdomen, such as thoraco-laparoscopic esophagectomy. The term laparoscopy is sometimes used interchangeably, although this is often reserved to describe a visual examination of the peritoneal cavity or the purely scopic component of a laparoscopic procedure. The colloquial keyhole surgery is common in non-medical usage.
Surgical Objective of Laparoscopic Surgery:
The objective of a laparoscopic approach is to minimize surgical trauma when operating on abdominal or pelvic structures. When correctly indicated and performed, this can result in smaller scars, reduced postoperative morbidity, shorter inpatient durations, and a faster return to normal activity. For a number of abdominopelvic procedures, a laparoscopic approach is now generally considered to be the gold-standard treatment option.
Definitions
Developments of Laparoscopic Surgery:
Following a number of smaller-scale applications of minimally invasive techniques to abdominopelvic surgery, laparoscopic surgery became a major part of general surgical practice with the introduction of laparoscopic cholecystectomy in the 1980s and the subsequent pioneering of endoscopic camera technology. This led to the widespread adoption of the technique by the early- to mid-1990s. The portfolio of procedures that can be performed laparoscopically has rapidly expanded with improvements in instruments, imaging, techniques and training — forming a central component of modern surgical practice and cross-specialty curricula [2]. Techniques such as laparoscopically assisted surgery and hand-assisted laparoscopic surgery have allowed the application of laparoscopic techniques to a greater variety of pathology. Single-incision laparoscopic surgery, natural orifice transluminal endoscopic surgery, and minilaparoscopy-assisted natural orifice surgery continue to push forward the applications of minimally invasive abdominopelvic techniques; however, the widespread practice and specific indications for these remain to be fully established. More recently, robotic surgery has been able to build on laparoscopic principles through developments in visualization, ergonomics, and instrumentation.
This Basic Laparoscopic Surgery Course Will Teach You:
- Abdominal access techniques and the different ways of establishing a pneumoperitoneum
- Principles of port placement and organization of the operative field
- Key elements of laparoscopic suturing, basic knotting and clip application
Specific attention is paid to the following hazards you may encounter:
- Fire hazard and thermal injury
- Lens fogging
- Contamination of insufflation system
- Complications from trocar introduction
- Limitations of Veress needle technique
- Limitations of open introduction technique
- Complications of the pneumoperitoneum
- Gas embolism
- Mirroring and scaling of instrument movements
- Firing clip applier without a loaded clip
The following tips are designed to improve your understanding and performance:
- Anatomy of a laparoscope
- Checking for optic fiber damage
- "White balance" of camera
- Checking integrity of electrosurgical insulation
- Access at Palmer's point
- Lifting abdominal wall before introduction
- Confirming position of Veress needle
- Umbilical anatomy
- Identification of inferior epigastric vessels under direct vision
- Translumination of superficial epigastric vessels
- Selection of trocar size
- Aiming of trocar
- Working angles in laparoscopic surgery
- Choice of suture material
- Instruments for suturing
- Optimal ergonomics for suturing
- Extracorporeal needle positioning
- Optimal suture lengths
- "Backloading" needle
- Intracorporeal needle positioning
- Hand movements when suturing
- Optimal positioning of scissors
- Extracorporeal knot tying
- Visualization of clip applier around target structure
- Common clip configurations
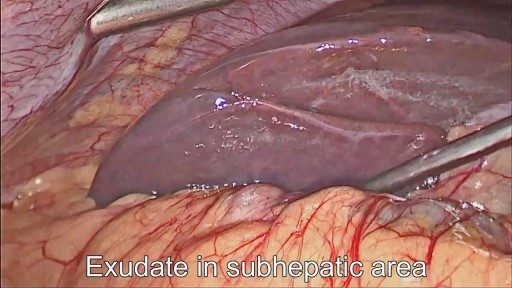
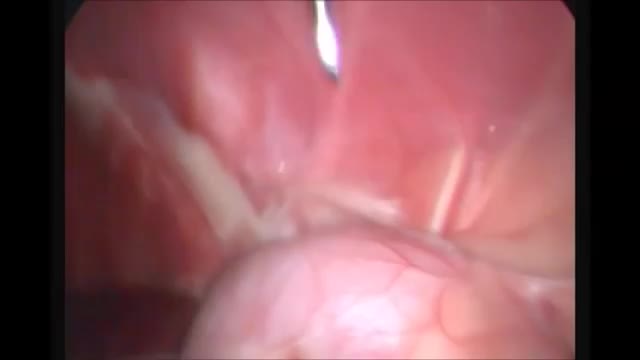
28 years old gentleman presented with huge liver abscess in the right lobe, with repeated attempts of percutaneous aspirations in the past. He was evaluated and subjected to Laparoscopic drainage. This video depicts feasibility of laparoscopy in deep seated liver abscesses. Video created by: Dr. Juneed M. Lanker Fellow Minimal Access Surgery Apollo Hospitals Chennai.

A 29 years old man lost his left wrist in car turn over in 2014. this video is taken 1 year after replantation. You can see another videos in my site: https://drliaghatclinic.com, https://instagram.com/liaghatclinic, https://t.me/liaghatclinic
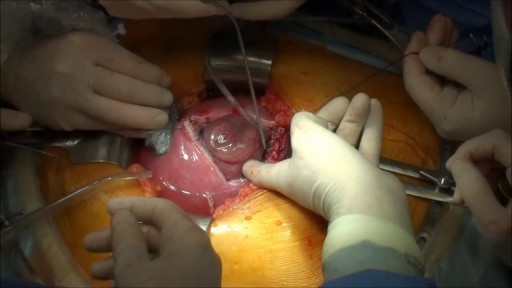
Prenatal repair of myelomeningocele (MMC), the most common and severe form of spina bifida, is a delicate surgical procedure where fetal surgeons open the uterus and close the opening in the baby's back while they are still in the womb.

Mini-Laparoscopic Cholecystectomy with Intraoperative Cholangiogram for Symptomatic Cholelithiasis (Gallstones) - Extended
Authors: Brunt LM1, Singh R1, Yee A2
Published: September 26, 2017
AUTHOR INFORMATION
1 Department of Surgery, Washington University, St. Louis, Missouri
2 Division of Plastic and Reconstructive Surgery, Washington University, St. Louis, Missouri
DISCLOSURE
No authors have a financial interest in any of the products, devices, or drugs mentioned in this production or publication.
ABSTRACT
Minimal invasive laparoscopic cholecystectomy is the typical surgical treatment for cholelithiasis (gallstones), where patients present with a history of upper abdominal pain and episodes of biliary colic. The classic technique for minimal invasive laparoscopic cholecystectomy involves four ports: one umbilicus port, two subcostal ports, and a single epigastric port. The Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) has instituted a six-step strategy to foster a universal culture of safety for cholecystectomy and minimize risk of bile duct injury. The technical steps are documented within the context of the surgical video for (1) achieving a critical view of safety for identification of the cystic duct and artery, (2) intraoperative time-out prior to management of the ductal structures, (3) recognizing the zone of significant risk of injury, and (4) routine intraoperative cholangiography for imaging of the biliary tree. In this case, the patient presented with symptomatic biliary colic due to a gallstone seen on the ultrasound in the gallbladder. The patient was managed a mini-laparoscopic cholecystectomy using 3mm ports for the epigastric and subcostal port sites with intraoperative fluoroscopic cholangiogram. Specifically, the senior author encountered a tight cystic duct preventing the insertion of the cholangiocatheter and the surgical video describes how the author managed the cystic duct for achieving a cholangiogram, in addition to the entire technical details of laparoscopic cholecystectomy.
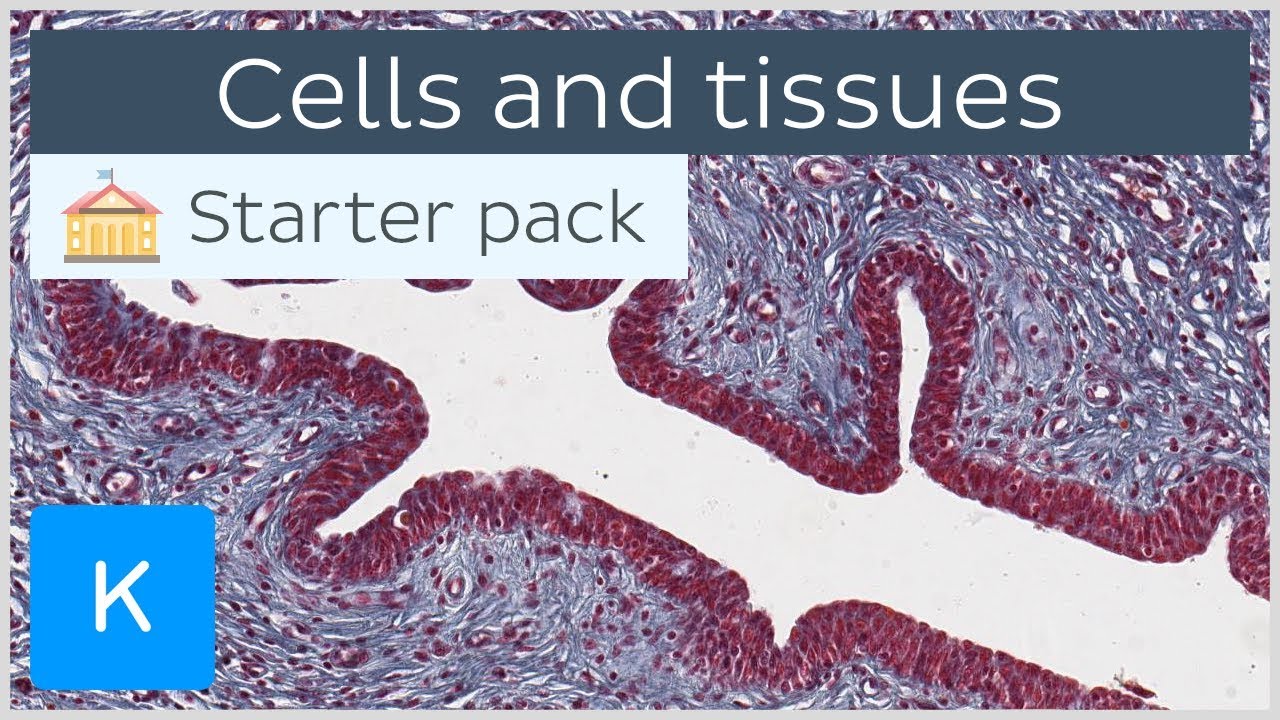
This tutorial is an introduction to the histology of the different tissues in the human body and the cells they are made of. Test yourself on our cells and tissue histology quiz at https://khub.me/jnhny
Oh, are you struggling with learning anatomy? We created the ★ Ultimate Anatomy Study Guide ★ to help you kick some gluteus maximus in any topic. Completely free. Download yours today: https://khub.me/1fcwd
A tissue is a group of cells that has a similar structure and acts together to perform one or more specific functions. In this tutorial, we will introduce you to the 4 main types of tissues in the human body: epithelial tissue, connective tissue, muscle tissue and nervous tissue. Epithelial tissue creates protective boundaries and is involved in the diffusion of ions and molecules, whereas connective tissue underlies and supports other tissue types.
Muscle tissue contracts to initiate movement in the body and nervous tissue transmits and integrates information through the central and peripheral nervous systems.
In this video tutorial we will take a closer look at the histology of the main cells and tissues under the microscope.
- 0:33 introduction to histology
- 1:22 epithelial tissue histology and types
- 5:45 function of the basement membrane
- 6:20 connective tissue histology and structure
- 10:53 muscle tissue and types of muscle cells
- 13:11 basics of the nervous system
Want to test your knowledge on the cells and tissues of the human body? Take this quiz: https://khub.me/jnhny
Why don't you jump into the introduction of the cell and its components with our free article next? Find it here: https://khub.me/apv1d
For more engaging video tutorials, interactive quizzes, articles and an atlas of Human anatomy and histology, go to https://khub.me/wcyx7
A renal biopsy is a procedure used to extract kidney tissue for laboratory analysis. The word “renal” describes the kidneys. A renal biopsy is also called a kidney biopsy. The test helps your doctor identify the type of kidney disease you have, how severe it is, and the best treatment for it.