Top videos
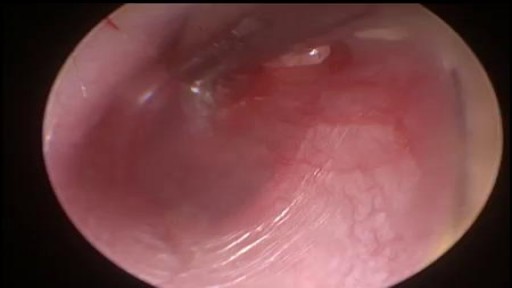
A myringotomy is a procedure in which your doctor creates a small hole in the eardrum so fluids such as water, blood, or pus can drain out. In many cases, your doctor will put in a tube so it won't get backed up again. The tube, which will usually fall out on its own in about six to 18 months, lets air flow through and keeps the middle ear dry. Tubes also: Reduce pain Improve hearing Cut down on the number of infections your child may have
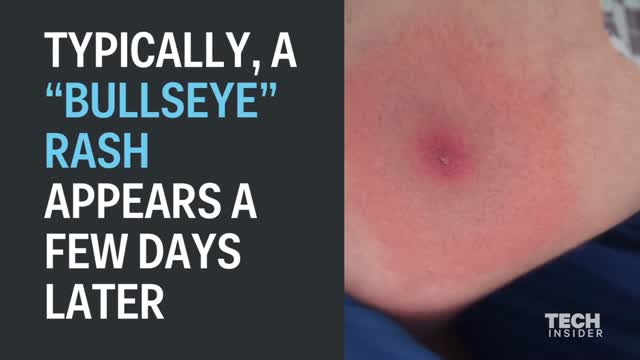
Lyme disease is a bacterial infection primarily transmitted by Ixodes ticks, also known as deer ticks, and on the West Coast, black-legged ticks. These tiny arachnids are typically found in wooded and grassy areas. Although people may think of Lyme as an East Coast disease, it is found throughout the United States, as well as in more than sixty other countries. The Centers for Disease Control and Prevention estimate that 300,000 people are diagnosed with Lyme disease in the US every year. That’s 1.5 times the number of women diagnosed with breast cancer, and six times the number of people diagnosed with HIV/AIDS each year in the US. However, because diagnosing Lyme can be difficult, many people who actually have Lyme may be misdiagnosed with other conditions. Many experts believe the true number of cases is much higher. Lyme disease affects people of all ages. The CDC notes that it is most common in children, older adults, and others such as firefighters and park rangers who spend time in outdoor activities and have higher exposure to ticks. LymeDisease.org has developed a Lyme disease symptom checklist to help you document your exposure to Lyme disease and common symptoms for your healthcare provider. You will receive a report that you can print out and take with you to your next doctor’s appointment.

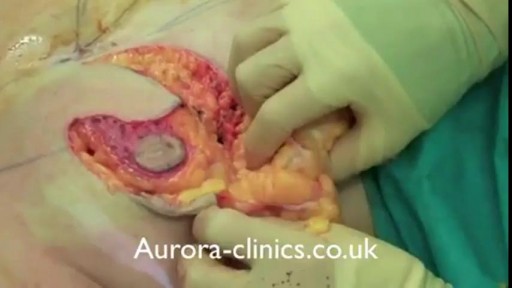
Knee replacement surgery advances are improving patients' experiences and outcomes. Knee surgery -- or even partial knee replacement -- is often the solution for advanced knee arthritis. Today you can regain significant mobility and flexibility after knee replacement thanks to advances in orthopedic surgery technology, materials and techniques. Knee replacement recovery times also have improved. This knee replacement surgery video covers what you can expect out of these knee joint replacement advances. Knee replacement surgery has been around for more than 30 years and is an incredibly successful operation. In the past the past, when a person had bad arthritis of the knee, they were pretty much out of luck other than taking aspirin. They'd be debilitated and limited in their activities. So, when a person has pain, stiffness, and their life is becoming restricted by that, that's when it's time to consider knee replacement. We always do non-surgical treatment first. When that doesn't work anymore, then it's time to consider knee replacement. About 500,000 a year are done, and most patients who have gone through this basically say that they wish they had done it sooner.
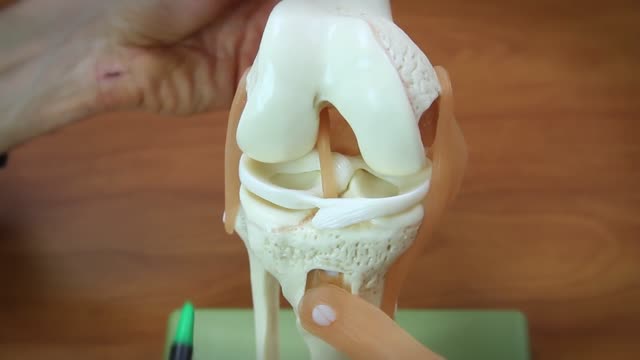
There are many factors that will determine how quickly, or completely you recover from your meniscal tear surgery. Key elements include your age, weight, and activity demands. The older you are, the heavier you are, the longer your recovery will be. The type of surgery you had will also impact upon your recovery. In some cases we only remove the torn piece — in general you will progress faster than someone who had sutures placed to repair the meniscus tear. Whether or not arthritis was found at the time of your meniscus surgery will also significantly influence your recovery from meniscus surgery. If you have arthritis then you are missing some or all of the cartilage on the ends of the bones. Knees with arthritis are prone to being more “cranky” during the recovery process. In those cases, a knee ice compression device can provide relief of pain/swelling. Many patients note they feel better wearing a compression sleeve during recovery. People with arthritis sometimes report improvement in their symptoms with supplements like Glucosamine, Curcumin, or Hyaluronic Acid which they believe (not proven) will smooth out the surface of the joint. Many try Tart Cherry juice because of its natural anti-inflammatory properties.. In the first few months following surgery, a knee compression sleeve does actually help many feel better. Some of the variables affecting your recovery from meniscus surgery are under your surgeon’s control. We can improve your immediate response after surgery with the use of various medications we inject within the knee before the surgery. We can also block a nerve on the side of your leg which will improve your pain for 18-24 hours after surgery. Many of you will purchase a ice compression sleeve to help minimize the pain after the surgery. In general, young, healthy active people with no evidence of osteoarthritis will experience a much more rapid recovery. Typically measured in days or a few weeks. Most people are off crutches in a day, and stop taking pain medicine within a day or two. In contrast, if you are a older, heavier and have arthritis as well as a meniscus tear, then you may take longer to recover — and may not experience a “full” recovery. This group can take weeks to months to improve. To ensure a good response to surgery, we also need to look at your health before surgery. Smoking leads to an increased infection rate and poorer healing. Diabetics with poor sugar control are at higher risk for infection and delays in healing as well. Obesity is a potential problem with anesthesia, the recovery from surgery and it may lead to more rapid progression of arthritis after surgery. The better shape you are in prior to surgery can influence your recovery.

Brown-Séquard syndrome is an incomplete spinal cord lesion characterized by a clinical picture reflecting hemisection injury of the spinal cord, often in the cervical cord region. (See Presentation.) Patients with Brown-Séquard syndrome suffer from ipsilateral upper motor neuron paralysis and loss of proprioception, as well as contralateral loss of pain and temperature sensation. A zone of partial preservation or segmental ipsilateral lower motor neuron weakness and analgesia may be noted. Loss of ipsilateral autonomic function can result in Horner syndrome. (See Etiology, Presentation, and Workup.) As an incomplete spinal cord syndrome, the clinical presentation of Brown-Séquard syndrome may range from mild to severe neurologic deficit. (See Presentation.) Brown-Séquard–plus syndrome The pure Brown-Séquard syndrome reflecting hemisection of the cord is not often observed. A clinical picture composed of fragments of the syndrome or of the hemisection syndrome plus additional symptoms and signs is more common. These less-pure forms of the disorder are often referred to as Brown-Séquard–plus syndrome.[1] Interruption of the lateral corticospinal tracts, the lateral spinal thalamic tract, and at times the posterior columns produces a picture of a spastic, weak leg with brisk reflexes and a strong leg with loss of pain and temperature sensation. Note that spasticity and hyperactive reflexes may not be present with an acute lesion.
The average time from symptom onset to diagnosis has been reported to be approximately 2 years. Despite recent attempts at increasing the awareness of pulmonary arterial hypertension (PAH), especially associated PAH (APAH), this delay in diagnosis has not changed appreciably in recent years. Early symptoms are nonspecific. Often, neither the patient nor the physician recognizes the presence of the disease, which leads to delays in diagnosis. Complicating matters, idiopathic PAH (IPAH) requires an extensive workup in an attempt to elucidate an identifiable cause of the elevated pulmonary artery pressure. The most common symptoms and their frequency, reported in a national prospective study, are as follows: Dyspnea (60% of patients) Weakness (19%) Recurrent syncope (13%) Additional symptoms include fatigue, lethargy, anorexia, chest pain, and right upper quadrant pain. Cough, hemoptysis, and hoarseness are less common symptoms. Women are more likely to be symptomatic than men.

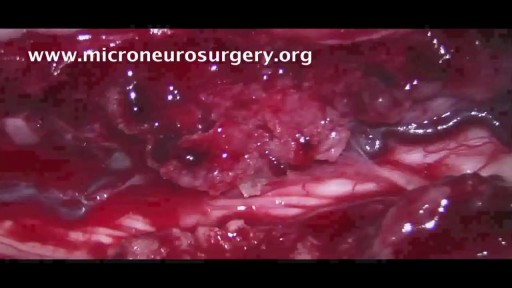
Retro-sigmoid craniotomy (often called "keyhole" craniotomy) is a minimally-invasive surgical procedure performed to remove brain tumors. This procedure allows for the removal of skull base tumors through a small incision behind the ear, providing access to the cerebellum and brainstem. Neurosurgeons may use this approach to reach certain tumors, such as meningiomas and acoustic neuromas (vestibular schwannomas).

Réduire La Cellulite, Meilleure Creme Anti Cellulite, Programme Anti Cellulite, Cuisse Cellulite http://perdre-sa-cellulite.plus101.com Une Bonne Alimentation Pour Lutter Contre la Cellulite. Certains aliments ont des composants naturels antioxydants et draineurs qui éliminent naturellement la cellulite. Parmi eux se trouvent le céleri branche. Il s’agit d’un légume un peu amère mais qui aide beaucoup à accélérer le métabolisme des graisses afin de débarrasser la cellulite. Coupé en bâtonnet, il peut être consommé en apéro ou en plat de crudités. Le poireau figure également dans la liste des meilleurs aliments anticellulite. Légume anti-rétention d’eau, il chasse les toxines tout en luttant contre la cellulite. Enfin, n’oubliez pas de consommer de l’ananas si vous voulez combattre votre cellulite. Il a pour principal mission de réduire la rétention d’eau. Selon des experts en physiologie, les femmes ont 90 muscles dans les membres inférieurs et en les stimulant doucement, ces muscles des fesses, jambes, hanches et cuisses, 76,3% des femmes peuvent inverser la cause de la peau d’orange et des capitons pour avoir une peau tonifiée et lisse. CLIQUEZ ICI: http://perdre-sa-cellulite.plus101.com

A new natural painkiller based on a body-own molecule, available as supplement. An educational video on its mechanism of action: palmitoylethanolamide (PEA) is a new compound ready 4 use in the clinic to calm glia and mast cells in all states of chronic pain. Thus it focusses on 2 new targets in the treatment of pain: these extra-neuronal targets in chronic pain can be modulated by PEA.
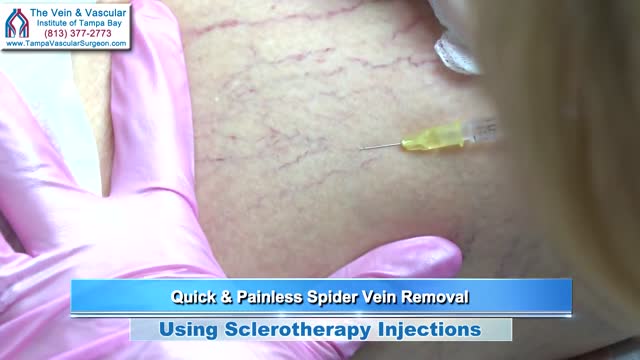
Sclerotherapy is a medical procedure used to eliminate varicose veins and spider veins. Sclerotherapy involves an injection of a solution (generally a salt solution) directly into the vein. The solution irritates the lining of the blood vessel, causing it to collapse and stick together and the blood to clot.

Bacterial abscess of the liver is relatively rare; however, it has been described since the time of Hippocrates (400 BCE), with the first published review by Bright appearing in 1936. In 1938, Ochsner's classic review heralded surgical drainage as the definitive therapy; however, despite the more aggressive approach to treatment, the mortality remained at 60-80%.[1] The development of new radiologic techniques, the improvement in microbiologic identification, and the advancement of drainage techniques, as well as improved supportive care, have reduced mortality to 5-30%; yet, the prevalence of liver abscess has remained relatively unchanged. Untreated, this infection remains uniformly fatal. The three major forms of liver abscess, classified by etiology, are as follows: Pyogenic abscess, which is most often polymicrobial, accounts for 80% of hepatic abscess cases in the United States Amebic abscess due to Entamoeba histolytica accounts for 10% of cases [2] Fungal abscess, most often due to Candida species, accounts for fewer than 10% of cases