Top videos
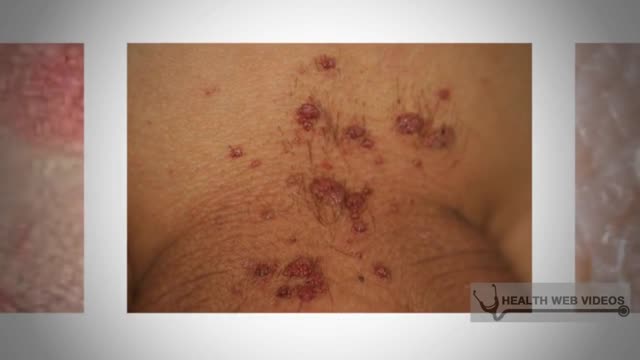
HPV is a different virus than HIV and HSV (herpes). HPV is so common that nearly all sexually active men and women get it at some point in their lives. There are many different types of HPV. Some types can cause health problems including genital warts and cancers.
This minimally invasive surgical procedure repairs the valve without removing the old, damaged valve. Instead, it wedges a replacement valve into the aortic valve’s place. The surgery may be called a transcatheter aortic valve replacement (TAVR) or transcatheter aortic valve implantation (TAVI).
The kidneys are a pair of organs located in the back of the abdomen. Each kidney is about 4 or 5 inches long -- about the size of a fist. The kidneys' function are to filter the blood. All the blood in our bodies passes through the kidneys several times a day. The kidneys remove wastes, control the body's fluid balance, and regulate the balance of electrolytes. As the kidneys filter blood, they create urine, which collects in the kidneys' pelvis -- funnel-shaped structures that drain down tubes called ureters to the bladder. Each kidney contains around a million units called nephrons, each of which is a microscopic filter for blood. It's possible to lose as much as 90% of kidney function without experiencing any symptoms or problems.
Shoulder impingement syndrome, also called subacromial impingement, painful arc syndrome, supraspinatus syndrome, swimmer's shoulder, and thrower's shoulder, is a clinical syndrome which occurs when the tendons of the rotator cuff muscles become irritated and inflamed as they pass through the subacromial space ...
Cirrhosis is a late stage of scarring (fibrosis) of the liver caused by many forms of liver diseases and conditions, such as hepatitis and chronic alcoholism. The liver carries out several necessary functions, including detoxifying harmful substances in your body, cleaning your blood and making vital nutrients. Cirrhosis occurs in response to damage to your liver. Each time your liver is injured, it tries to repair itself. In the process, scar tissue forms. As cirrhosis progresses, more and more scar tissue forms, making it difficult for the liver to function. Decompensated cirrhosis is the term used to describe the development of specific complications resulting from the changes brought on by cirrhosis. Decompensated cirrhosis is life-threatening. The liver damage done by cirrhosis generally can't be undone. But if liver cirrhosis is diagnosed early and the cause is treated, further damage can be limited and, rarely, reversed.
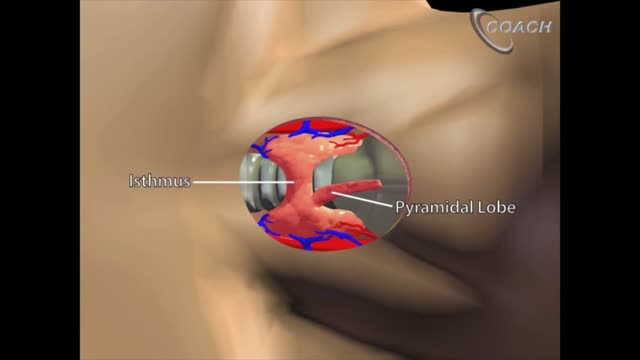
Minimally invasive open thyroidectomy (MIT) is similar to conventional thyroidectomy in its surgical approach. The major difference is the length of the neck incision. A smaller incision improves cosmesis and reduces discomfort. Typically, a skin incision less than 6 cm is considered minimally invasive. The remainder of the procedure is exactly the same as is used in conventional thyroidectomy. Adaptations to this technique include transection rather than lateral retraction of the strap muscles (the Sofferman technique). [1]

The two biggest considerations when choosing a suture are the location and tension of the wound. Other important considerations are tensile strength, knot strength, handling, and tissue reactivity. Sutures are divided into two major groups: Absorbable – lose the majority of their tensile strength in less than 60 days. They are generally used for buried sutures and do not require removal. Non-absorbable – maintain the majority of their tensile strength for more than 60 days. They are generally used for skin surface sutures and do require removal postoperatively. Suture needles also come in a variety of shapes and sizes. Curved needles are almost exclusively used in dermatological surgery. Cutting needles move through the tissue more easily and may have their primary cutting edge on the inside of the curve (conventional cutting) or outside of the curve (reverse cutting). The benefit of reverse cutting is that the tapered puncture left by the suture is directed away from the wound edge and therefore tissue tearing is less common. Non-cutting round needles cause even less tissue tearing and may be especially useful in delicate areas and fascia.
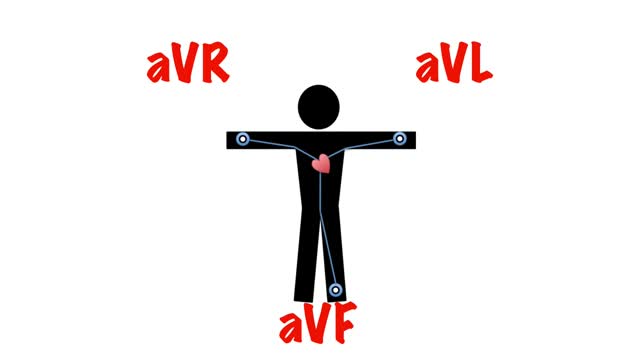
It then spreads down the bundle of his and then purkinje fibres to cause ventricular contraction. So when viewing the heart from the front, the direction of depolarisation is 11 o'clock to 5 o'clock. The general direction of depolarisation is known as the cardiac axis.
The annual incidence of primary intraspinal neoplasm is approximately five per million for females and three per million for males.[9] Spinal intradural extramedullary tumors account for two thirds of all intraspinal neoplasms and include neuromas and meningiomas.[1] Overall, meningiomas account for 25 to 46% of primary spinal neoplasms and are the second most common intradural spine tumor after neuromas.[9] Spinal meningiomas occur less frequently than intracranial ones and account for approximately 7.5 to 12.7% of all meningiomas.[25]

Water is an essential nutrient for the body, as the body loses water through perspiration, breathing, bowel movements, and in urine. Water must be consumed regularly to maintain a sufficient level. Water has many vital functions in the body, including… Serving as a lubricant. Water is a main component of saliva, which helps moisten food making it easier to swallow. Water also helps lubricate joints, reducing friction and inflammation. Water is important in body temperature regulation. When body heat rises, such as during strenuous activities, the body starts to sweat to cool itself. And sweat is made up almost entirely of water.

An ICD is a battery-powered device placed under the skin that keeps track of your heart rate. Thin wires connect the ICD to your heart. If an abnormal heart rhythm is detected the device will deliver an electric shock to restore a normal heartbeat if your heart is beating chaotically and much too fast.
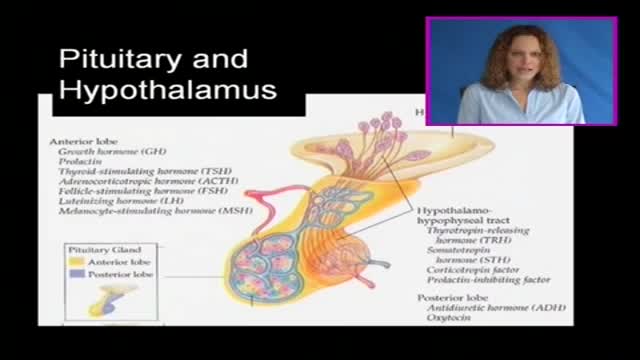
The pituitary gland is often portrayed as the "master gland" of the body. Such praise is justified in the sense that the anterior and posterior pituitary secrete a battery of hormones that collectively influence all cells and affect virtually all physiologic processes. The pituitary gland may be king, but the power behind the throne is clearly the hypothalamus. As alluded to in the last section, some of the neurons within the hypothalamus - neurosecretory neurons - secrete hormones that strictly control secretion of hormones from the anterior pituitary. The hypothalamic hormones are referred to as releasing hormones and inhibiting hormones, reflecting their influence on anterior pituitary hormones.
Keyhole surgery can be helpful for patients with brain, pituitary and skull base tumors. With cutting edge technology and a proven track record in keyhole and endonasal endoscopic approaches, we make surgery safer, less invasive and more effective.

A burn is tissue damage that results from scalding, overexposure to the sun or other radiation, contact with flames, chemicals or electricity, or smoke inhalation. Is it a major or minor burn? Call 911 or seek immediate care for major burns, which: Are deep Cause the skin to be dry and leathery May appear charred or have patches of white, brown or black Are larger than 3 inches (about 8 centimeters) in diameter or cover the hands, feet, face, groin, buttocks or a major joint A minor burn that doesn't require emergency care may involve: Superficial redness similar to a sunburn Pain Blisters An area no larger than 3 inches (about 8 centimeters) in diameter Treating major burns Until emergency help arrives: Protect the burned person from further harm. If you can do so safely, make sure the person you're helping is not in contact with the source of the burn. For electrical burns, make sure the power source is off before you approach the burned person. Make certain that the person burned is breathing. If needed, begin rescue breathing if you know how. Remove jewelry, belts and other restrictive items, especially from around burned areas and the neck. Burned areas swell rapidly. Cover the area of the burn. Use a cool, moist bandage or a clean cloth. Don't immerse large severe burns in water. Doing so could cause a serious loss of body heat (hypothermia). Elevate the burned area. Raise the wound above heart level, if possible. Watch for signs of shock. Signs and symptoms include fainting, pale complexion or breathing in a notably shallow fashion. Treating minor burns For minor burns: Cool the burn. Hold the burned area under cool (not cold) running water or apply a cool, wet compress until the pain eases. Remove rings or other tight items from the burned area. Try to do this quickly and gently, before the area swells. Don't break blisters. Fluid-filled blisters protect against infection. If a blister breaks, clean the area with water (mild soap is optional). Apply an antibiotic ointment. But if a rash appears, stop using the ointment. Apply lotion. Once a burn is completely cooled, apply a lotion, such as one that contains aloe vera or a moisturizer. This helps prevent drying and provides relief. Bandage the burn. Cover the burn with a sterile gauze bandage (not fluffy cotton). Wrap it loosely to avoid putting pressure on burned skin. Bandaging keeps air off the area, reduces pain and protects blistered skin. If needed, take an over-the-counter pain reliever, such as ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve) or acetaminophen (Tylenol, others).