Top videos
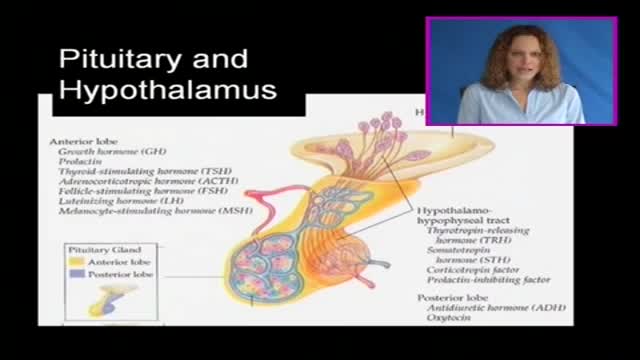
The pituitary gland is often portrayed as the "master gland" of the body. Such praise is justified in the sense that the anterior and posterior pituitary secrete a battery of hormones that collectively influence all cells and affect virtually all physiologic processes. The pituitary gland may be king, but the power behind the throne is clearly the hypothalamus. As alluded to in the last section, some of the neurons within the hypothalamus - neurosecretory neurons - secrete hormones that strictly control secretion of hormones from the anterior pituitary. The hypothalamic hormones are referred to as releasing hormones and inhibiting hormones, reflecting their influence on anterior pituitary hormones.
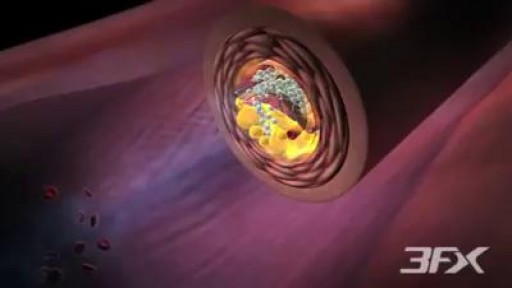
Experts once believed that atherosclerosis, or hardening of the arteries, developed when too much cholesterol clogged arteries with fatty deposits called plaques. ... Researchers have discovered how diabetes, by driving inflammation and slowing blood flow, dramatically accelerates atherosclerosis.Mar 17, 2008 Past studies had shown diabetes to worsen atherosclerosis, but its exact link to related inflammation had remained unclear. The current results provides the first mechanistic description of how diabetes takes away the ability of fast blood flow force to protect blood vessels, arguing that it does so by interfering with ERK5 and its signaling partners.
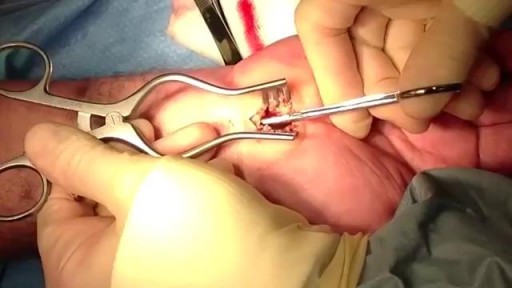
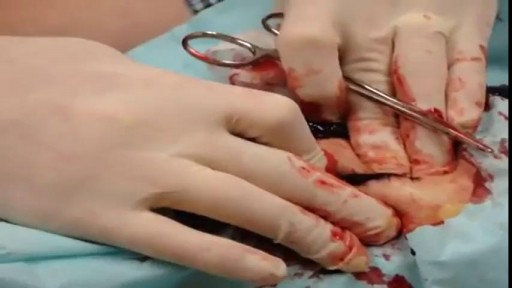
Carpal tunnel release is a surgery used to treat and potentially heal the painful condition known as carpal tunnel syndrome. Doctors used to think that carpal tunnel syndrome was caused by an overuse injury or a repetitive motion performed by the wrist or hand, often at work. They now know that it’s most likely a congenital predisposition (something that runs in families) – some people simply have smaller carpal tunnels than others. Carpal tunnel syndrome can also be caused by injury, such as a sprain or fracture, or repetitive use of a vibrating tool. It's also been linked to pregnancy, diabetes, thyroid disease, and rheumatoid arthritis.
Anemia is a condition in which the body does not have enough healthy red blood cells. Red blood cells provide oxygen to body tissues. There are many types of anemia. Pernicious anemia is a decrease in red blood cells that occurs when the intestines cannot properly absorb vitamin B12.

http://vencer-la-diabetes-rapido.info-pro.co/ Como Controlar La Diabetes Tipo 2 Naturalmente Sin Medicamentos, Pre Diabetes Y Diabetes Tipo 1. https://youtu.be/BOSkQ5MnjT0 Que es la Insulina? Una definición practica sin adentrarnos en terminos estrictamente medicos es que la insulina es una hormona formada por 51 aminoácidos. Dentro del páncreas, las células beta producen la hormona llamada insulina. Con cada comida, las células beta liberan insulina para ayudar al cuerpo a utilizar o almacenar en la sangre la glucosa que se obtiene de los alimentos. Su déficit provoca la diabetes mellitus y su exceso provoca hiperinsulinismo con hipoglucemia. En las personas con diabetes tipo 1, el páncreas no produce insulina. Las células beta han sido destruidas y se necesitan inyecciones de insulina para utilizar la glucosa de las comidas. Las personas con diabetes tipo 2 producen insulina, pero sus cuerpos no responden bien a la misma. Algunas personas con diabetes tipo 2 necesitan medicamentos para la diabetes o inyecciones de insulina para ayudar a su cuerpo a utilizar la glucosa para obtener energía. * La insulina no se puede tomar como una píldora, ya que se descompone durante la digestión al igual que la proteína en los alimentos. Se debe inyectar en la grasa debajo de la piel para que llegue a la sangre. Existen diferentes tipos de insulina en función de la rapidez con que trabajan, y en funcion de su duración. La insulina viene en diferentes concentraciones, la más común es U-100. Tipos de insulina: * De Acción Rápida: Comienza a trabajar unos 15 minutos después de la inyección, con picos en aproximadamente 1 hora, y continúa trabajando por un tiempo de 2 a 4 horas. Tipos: Insulina glulisina (Apidra), la insulina lispro (Humalog) y la insulina aspart (NovoLog). * Regular o de Acción Corta: Generalmente llega al torrente sanguíneo a los 30 minutos después de la inyección, picos de entre 2 a 3 horas después de la inyección, y es efectiva durante aproximadamente 3 a 6 horas. Tipos: Humulin R, Novolin R * De Acción Intermedia: Generalmente llega al torrente sanguíneo de aproximadamente 2 a 4 horas después de la inyección, picos de 4 a 12 horas y eseficaz durante aproximadamente 12 a 18 horas. Tipos: NPH (Humulin N, Novolin N) * De Acción Prolongada: Alcanza el torrente sanguíneo varias horas después de la inyección y tiende a disminuir los niveles de glucosa de manera bastante uniforme durante un período de 24 horas. Tipos: La insulina detemir (Levemir) y la insulina glargina (Lantus) Nota: Esta información debes consultarla siempre con tu medico especialista. La insulina Tiene 3 Características: El inicio: Es el tiempo antes de que la insulina alcance el torrente sanguíneo y se inicie la reducción de la glucosa en sangre. Pico: Es el tiempo durante el cual la insulina está surtiendo el máximo efecto en términos de reducción de la glucosa en sangre. La duración: Es cuánto tiempo la insulina continúa reduciendo la glucosa sanguínea.

Home Remedies For Acid Reflux, Ginger For Acid Reflux, Heartburn After Gallbladder Removal --- http://heartburn-acid-reflux.info-pro.co --- Stop using Pepto Bismol until you read the following… There is BREAKING scientific news reporting that many of America’s most popular antacids – both the ones you buy at the drug store and the ones you need prescriptions for… Are linked to more than a dozen forms of potentially DEADLY cancers. Click this link now to get the full story and see if you’re at risk. You’ll find out about a “just discovered” alternative to antacids…. Something that can permanently cure even the worst cases of acid reflux in as little few days, and that doesn’t require any pills or medications. Click Here: http://heartburn-acid-reflux.info-pro.co
Heart failure can occur if the heart cannot pump (systolic) or fill (diastolic) adequately. Symptoms include shortness of bronicreath, fatigue, swollen legs, and rapid heartbeat. Treatments can include eating less salt, limiting fluid intake, and taking prescription medications. In some cases a defibrillator or pacemaker may be implanted.

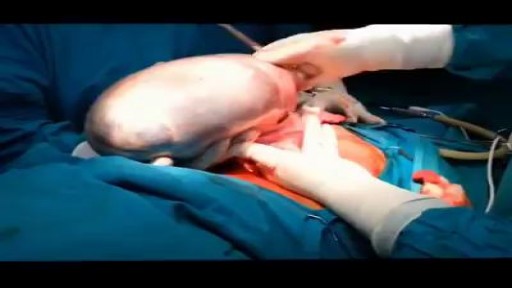
Pregnancy occurs when an egg is fertilized by a sperm, grows inside a woman's uterus (womb), and develops into a baby. In humans, this process takes about 264 days from the date of fertilization of the egg, but the obstetrician will date the pregnancy from the first day of the last menstrual period (280 days 40 weeks).
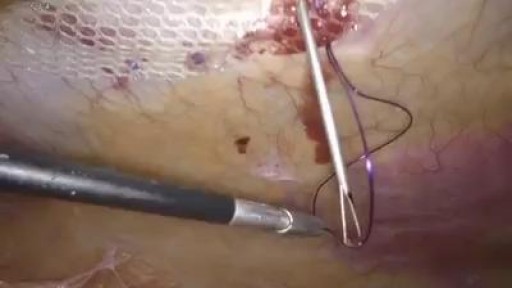
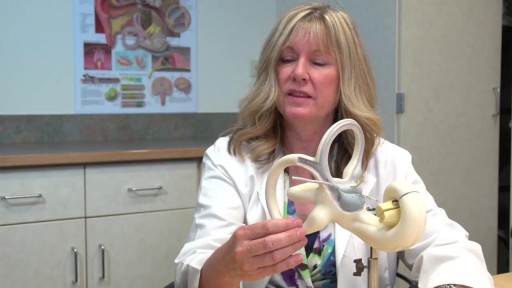
Keyhole surgery can be helpful for patients with brain, pituitary and skull base tumors. With cutting edge technology and a proven track record in keyhole and endonasal endoscopic approaches, we make surgery safer, less invasive and more effective.

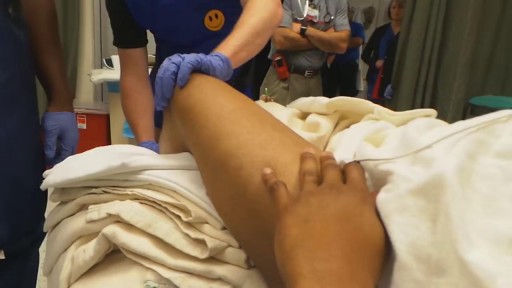
A burn is tissue damage that results from scalding, overexposure to the sun or other radiation, contact with flames, chemicals or electricity, or smoke inhalation. Is it a major or minor burn? Call 911 or seek immediate care for major burns, which: Are deep Cause the skin to be dry and leathery May appear charred or have patches of white, brown or black Are larger than 3 inches (about 8 centimeters) in diameter or cover the hands, feet, face, groin, buttocks or a major joint A minor burn that doesn't require emergency care may involve: Superficial redness similar to a sunburn Pain Blisters An area no larger than 3 inches (about 8 centimeters) in diameter Treating major burns Until emergency help arrives: Protect the burned person from further harm. If you can do so safely, make sure the person you're helping is not in contact with the source of the burn. For electrical burns, make sure the power source is off before you approach the burned person. Make certain that the person burned is breathing. If needed, begin rescue breathing if you know how. Remove jewelry, belts and other restrictive items, especially from around burned areas and the neck. Burned areas swell rapidly. Cover the area of the burn. Use a cool, moist bandage or a clean cloth. Don't immerse large severe burns in water. Doing so could cause a serious loss of body heat (hypothermia). Elevate the burned area. Raise the wound above heart level, if possible. Watch for signs of shock. Signs and symptoms include fainting, pale complexion or breathing in a notably shallow fashion. Treating minor burns For minor burns: Cool the burn. Hold the burned area under cool (not cold) running water or apply a cool, wet compress until the pain eases. Remove rings or other tight items from the burned area. Try to do this quickly and gently, before the area swells. Don't break blisters. Fluid-filled blisters protect against infection. If a blister breaks, clean the area with water (mild soap is optional). Apply an antibiotic ointment. But if a rash appears, stop using the ointment. Apply lotion. Once a burn is completely cooled, apply a lotion, such as one that contains aloe vera or a moisturizer. This helps prevent drying and provides relief. Bandage the burn. Cover the burn with a sterile gauze bandage (not fluffy cotton). Wrap it loosely to avoid putting pressure on burned skin. Bandaging keeps air off the area, reduces pain and protects blistered skin. If needed, take an over-the-counter pain reliever, such as ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve) or acetaminophen (Tylenol, others).