Top videos
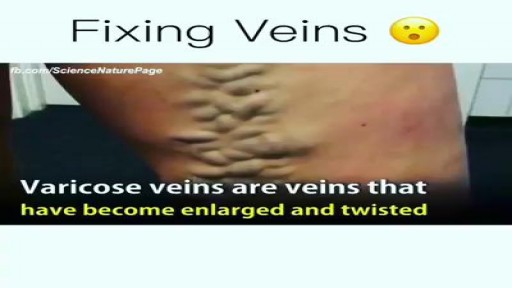
As a curious child, you might remember staring at an older relative's thick stockings at the blue, gnarled veins lying under the skin like bumpy snakes. Known as varicose veins, these blood vessels, which return blood from the legs to the heart, are actually a more superficial system. The real, working venous system for the legs lies deeper, says to Robert A. Weiss, MD, assistant professor of dermatology at the Johns Hopkins School of Medicine in Baltimore. This is good news, because it means that if the surface veins begin to clump up and bulge, they can be removed or destroyed without ruining circulation to the leg. The National Institutes of Health estimates that 60% of all men and women suffer from some form of vein disorder. A quarter of varicose vein sufferers are men, although Weiss notes that it is almost always women who seek help for spider veins.

Transcript: Body Restoration (http://stalbertphysiotherapy.com/) has treated over 12,400 patients since it opened its doors in 1992. While embracing new technology and techniques they have not left behind the basic tenets of hands-on healing. If you are injured or have chronic pain, the mission is to help you live pain-free. Relief is a click or a phone call away. Come in for your no obligation exam and find out what will work for you.

Dieta Alcalina, Lista Alimentos Alcalinos, Agua Alcalina Beneficios, Consejos Para Adelgazar---- http://dieta-alcalina-alimentos.good-info.co --- Entendiendo Como Funciona Una Dieta. Alcalina Las dietas Alcalinas son una forma popular para las personas que quieren logran una salud óptima. Sin embargo, muchas personas en verdad no entienden como esta dieta funciona. El concepto es realmente muy simple – la dieta se centra en volver a ganar el equilibrio que se perdió cuando el hombre empezó a tener una alimentación más "domesticada" en la revolución industrial y grandes almacenamientos de alimentos. Cuando comenzó a primar el beneficios económico a la salud de las personas. En vez de centrarse en la comida alta en azúcar, grasa y colesterol, una dieta alcalina consiste principalmente en frutas y vegetales frescos, cereales integrales, fuentes de proteínas saludables, como soya, frijoles, legumbres y aceites saludables como la canola, oliva y la semilla de lino. Estos alimentos pueden ser alcalinos o ácidos en su estado natural, pero todos ellos producen lo que se denomina “cenizas alcalinas” una vez que son digeridos y metabolizados por el cuerpo. Cuando el pH del cuerpo se mantiene a un nivel bajo de alcalinidad, todo el sistema puede trabajar más eficientemente. Descubre como la dieta alcalina funciona & por qué los alimentos alcalinos son altamente recomendados para tu salud. Haz clic aquí http://dieta-alcalina-alimentos.good-info.co

Dieta Alcalina Recetas, Listado De Alimentos Alcalinos, Que Es El Agua Alcalina, Menu Para Adelgazar-- http://dieta-alcalina-alimentos.good-info.co -- Entendiendo los Efectos del nivel de pH en el cuerpo El nivel de pH en el cuerpo tiene la habilidad de afectar cada célula del cuerpo. Cuando la sangre tiene un pH alcalino en vez de un pH ácido, ocurre un efecto positivo en cada función corporal del sistema. El cerebro, el sistema circulatorio, los nervios, los músculos, el sistema respiratorio, el sistema digestivo y reproductivo se pueden beneficiar de un nivel adecuado de pH. Por otro lado, cuando el pH del cuerpo es muy ácido, es susceptible a muchas enfermedades y problemas. Ganancia de peso, enfermedades del corazón, envejecimiento prematuro, fatiga, problemas nerviosos, alergias, enfermedades musculares y cáncer son las más probables a ocurrir cuando el pH del cuerpo no está al nivel óptimo. Ya que todos estos problemas son más probables a ocurrir cuando el pH del cuerpo está muy ácido, tiene sentido consumir una dieta rica en alimentos alcalinos. El objetivo principal es usualmente comer aproximadamente entre 75-80% de alimentos alcalinos junto con solamente entre 20-25% de alimentos ácidos. Si se mantiene este nivel en la dieta, el resultado final es un nivel de pH bajo en el cuerpo, el que se requiere para una salud óptima. Descubre como la dieta alcalina funciona & por qué los alimentos alcalinos son altamente recomendados para tu salud. Haz clic aquí http://dieta-alcalina-alimentos.good-info.co

Como Aumentar La Libido, Aumentar Niveles De Testosterona, Como Aumentar El Deseo Masculino ---- http://aumentar-testosterona.good-info.co/ --- ¿Se puede tener una erección con bajos niveles de testosterona? Mi libido está quedando atrás y estoy teniendo dificultades para conseguir una erección, así que estoy tratando de averiguar qué está pasando aquí. La disfunción eréctil rara vez es causada sólo por la deficiencia de testosterona. Por lo general es un grupo de cosas que funcionan en concierto juntos, que se alimentan entre sí, que conducen a la incapacidad del hombre para lograr una erección. La aterosclerosis (estrechamiento y endurecimiento de las arterias) es uno de los mayores impulsores de la disfunción eréctil, pero estas arterias dañadas no aparecen de la nada. Otras cosas tienen que estar sucediendo en el cuerpo para que ésta aterosclerosis pase, y como estamos a punto de ver, estas otras cosas contribuyen al problema también. Así que vamos a repasar esta lista… Nivel de azúcar alto – baja testosterona y disfunción eréctil La azúcar elevada en la sangre es un arma de doble filo, porque los hombres que sufren de esta condición son mucho más propensos a ser afectados por la disfunción eréctil y la testosterona baja. Una Investigación de John Hopkins encontró que las ratas diabéticas presentaron una respuesta eréctil 30% inferior, sus erecciones fueron como máximo 40% más pequeñas y las erecciones tomaron 70% más tiempo para lograrse en comparación con los controles que no eran diabéticos. Otros estudios han confirmado que los hombres con diabetes tipo 2 son dos veces más propensos a sufrir de disfunción eréctil, y la condición les golpeará una década antes, en comparación con los hombres sin tipo 2. Este vínculo es tan fuerte porque el azúcar en la sangre hace un daño directo a las arterias cuando se tiene demasiado de él, y las arterias en el pene suelen ser afectados en primer lugar, porque son muy pequeñas y estrechas. Por lo tanto, tiene todo el sentido que éstas pueden dañarse primero. El ejercicio que baja la testosterona haga click aqui http://aumentar-testosterona.good-info.co/

Discover how hemodialysis works and the different options available for this dialysis treatment.
Related articles on DaVita.com:
What Is Hemodialysis? (http://www.davita.com/treatmen....t-options/hemodialys
How Does a Dialysis Machine Work? (http://www.davita.com/treatmen....t-options/hemodialys

A doctor explains the purpose of dialysis and explains the difference between hemodialysis and peritoneal dialysis. Learn more at https://www.niddk.nih.gov/heal....th-information/kidne

Hair Transplant Results Before and After Photos who undergone Hair Transplant. View our patient's successful results with the FUE, Bio - FUE and B.E.S.T FUE hair transplant technique. Comparable before & after photos! For More Visit Here:- https://www.hairtransplantchennai.org/hair-transplant-results-chennai.php or call us:- +91-8939636222
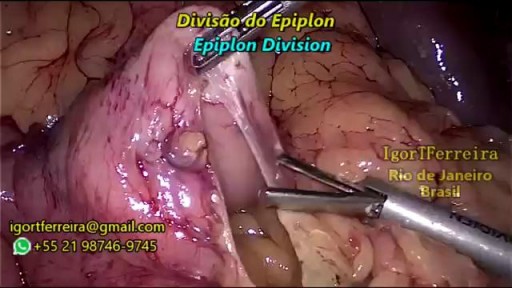
a sleeve gastrectomy with very few edditing. During the start 3 smal spleen perforations caused by Veres Needle were identified, caused by a giant spleen undentified on pre operatory ultrasound. They were controled with gauze compression and at the end of the surgery surgicel was placed and no complications were observed. Patient discharged 3 days after the surgery.

Acute sinusitis can be triggered by a cold or allergies and may resolve on its own. Chronic sinusitis lasts up to eight weeks and may be caused by an infection or growths. Symptoms include headache, facial pain, runny nose, and nasal congestion. Acute sinusitis usually doesn't require any treatment beyond symptomatic relief with pain medications, nasal decongestants, and nasal saline rinses. Chronic sinusitis may require antibiotics.
Antibiotic therapy is the mainstay of medical treatment for pediatric rhinosinusitis.] Because of increasing prevalence of beta-lactam–resistant bacteria in the community, administer antibiotics only for suspected infection as based on a careful history and physical examination. Direct the therapeutic regimen against the prevalent pathogens in the community and carefully consider suspicion for highly resistant bacteria. Typically, uncomplicated cases of acute sinusitis are responsive to amoxicillin. Most patients respond to this initial regimen. For children allergic to penicillin, a second- or third-generation cephalosporin can be used (only if the allergic reaction is not a type 1 hypersensitivity reaction). In cases of serious allergic reaction, a macrolide or clindamycin can be used.