Top videos
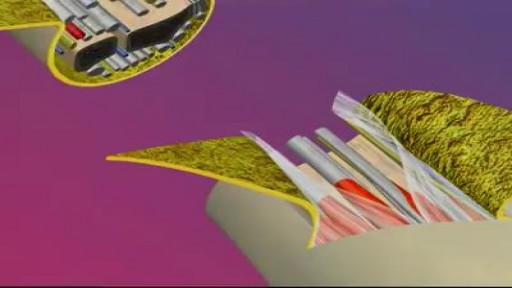
A reconstructive transplant, also called a composite tissue transplant or composite tissue allograft, is an operation that involves transplantation of bone, tissue, muscle and blood vessels. A reconstructive hand transplant is an operation tailored to each patient’s individual needs, type of injury and anatomy. This transplants an upper extremity, usually at the level of the forearm and wrist, but sometimes above the elbow, to help restore function after the loss of a hand or arm.

http://plantar-fasciitis-solution.info-pro.co Pain In Arch Of Foot, Severe Heel Pain, Best Running Shoes For Plantar Fasciitis, Foot Pain Heel Know the Symptoms of Plantar Fasciitis An injury to the plantar fascia can manifest in different ways. Initially, it may be a gradual pain that can progressively become worse, especially if the injured foot remains in active use. Sometimes, the pain from plantar fasciitis can be quite severe and seem like the stab of a knife of a sharp and sudden cut. The pain of plantar fasciitis may also occur more frequently after injured feet have been at rest for a while. For instance, after a person wakes up and tries to use his or her feet, pain may be experienced. It can be dangerous to ignore pain that is associated with the feet or any pain felt in the body. Sometimes, symptoms of plantar fasciitis include more subtle pain that may appear as a throbbing sensation which may be radial in nature or isolated to a particular part of the foot. If the pain from plantar fasciitis starts off mildly and is ignored, continued use of the affected foot or feet will cause further damage. The pain from plantar fasciitis is debilitating and it is essential that treatment is sought immediately. get instant plantar fasciitis pain relief in just 5 minutes! click here. http://plantar-fasciitis-solution.info-pro.co

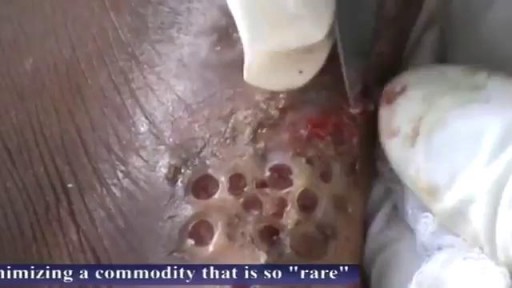
Suppurativa Hidradenitis, Hidradenitis Suppurativa Support, Hidradenitis Suppurativa Cures.--- http://hidradenitis-suppurativa-cure.good-info.co --- Causes of hidradenitis suppurativa Now that we know the symptoms, we must look deeper into the causes so as to get to the root of the problem Caused when hair follicles are blocked or inflamed When hair follicles are blocked due to smoking When hair follicles are blocked due to excess weight Hormonal fluctuations May be caused due to hyper active immune system Causes are sometimes also genetic Severe effects of hidradenitis suppurativa Smells, scars, itches and pains Fear of isolation due to stigmatization Overtime leading to depression Debility and strike on self esteem More information in. http://hidradenitis-suppurativa-cure.good-info.co

Come Rimanere Incinta Velocemente, Per Restare Incinta, Rimanere Incinta A 45 Anni, In Gravidanza--- http://come-rimanere-incinta.info-pro.co -- Farti rimanere incinta rapidamente e allo stesso tempo invertire l'infertilità. E' un dato di fatto. Il 92% delle donne che usano trattamenti convenzionali per aumentare le loro probabilità di concepire non riescono a rimanere incinta e, a volte, la loro situazione peggiora anzichè migliorare. Ora tu puoi decidere di far parte del 8% delle donne che sono guarite dall'infertilità per sempre, imparando a lavorare sinergicamente con il tuo corpo. Contrariamente agli approcci convenzionali, lavorando con il tuo corpo, eliminando la causa principale e specifica della tua infertilità (come: cisti ovariche, fibromi uterini, endometriosi, livelli di follitropina alti, sindrome dell'ovaio policistico, ecc), migliorando contemporaneamente la tua mentalità, il tuo stato emotivo e biologico-riproduttivo, rimarrai velocemente incinta e darai alla luce un bimbo sano e forte, indipendentemente dalla tua età, dal numero di tentativi andati male o dalla gravità della tua situazione. Farti rimanere incinta olisticamente. E' un dato di fatto, non potrai mai rimanere incinta naturalmente e curare la tua infertilità affrontando solo uno dei tanti fattori responsabili dell'infertilità. Ad esempio, se hai già provato trattamenti come le pillole ormonali, posizioni sessuali o diete differenti, e non hai ottenuto nessun risultato probabilmente è perchè ti sei concentrata solo su un aspetto della tua condizione. Il mio sistema non ti insegnerà solo l'unico modo per rimanere incinta naturalmente, ma imparerai anche l'unico modo per invertire la tua infertilità per sempre, in modo olistico. Questo Rivoluzionario Sistema E' Talmente Unico ed Efficace che Ha il Potere di... Clicca sul link http://come-rimanere-incinta.info-pro.co
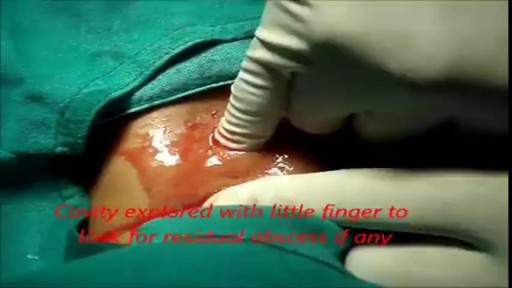
She is a twenty years young female presented with large cystic swelling in anterior aspect of neck. The swelling was of size 6cmx 6cm x5 cm ,tense tender, cystic just above sternal nutch.This was diagnosed as large neck abscess ./nRepeated aspiration done but the swelling reappeared. So Incision & Drainage planned under local anaesthesia./nPatient in supine position. Surgery part painted and draped. Local anaesthesia 2% xylocaine with adrenaline used for field block.After giving local anaesthesia, I used a no 11 blade for stab incision at the most prominent part of the swelling, where skin was thin and fluctuation present./nPus drained form that opening. Little dilatation of opening to be done with artery forceps or sinus forceps. Complete pus drainage to be ensured.Little finger can be introduced inside the pus cavity to ensure proper drainage of pus. The cavity I use to clean with a gauge piece. If necessary curette biopsy can be taken from the wall of the cavity.These wounds usually need daily proper dressing for faster healing.

Curious about physiotherapy or wanting to know how to properly perform an exercise? Check us out on Social Media! Facebook: https://www.facebook.com/striveptandperformance/ Instagram: https://www.instagram.com/striveptandperf/ Twitter: https://twitter.com/StrivePTandPerf Blog: http://www.strivept.ca/blog
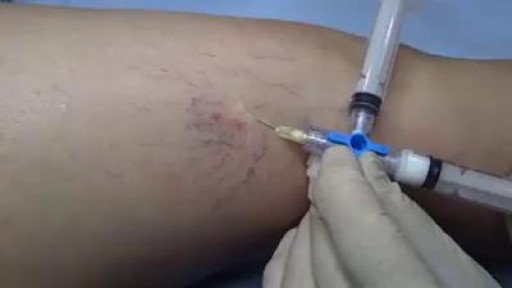
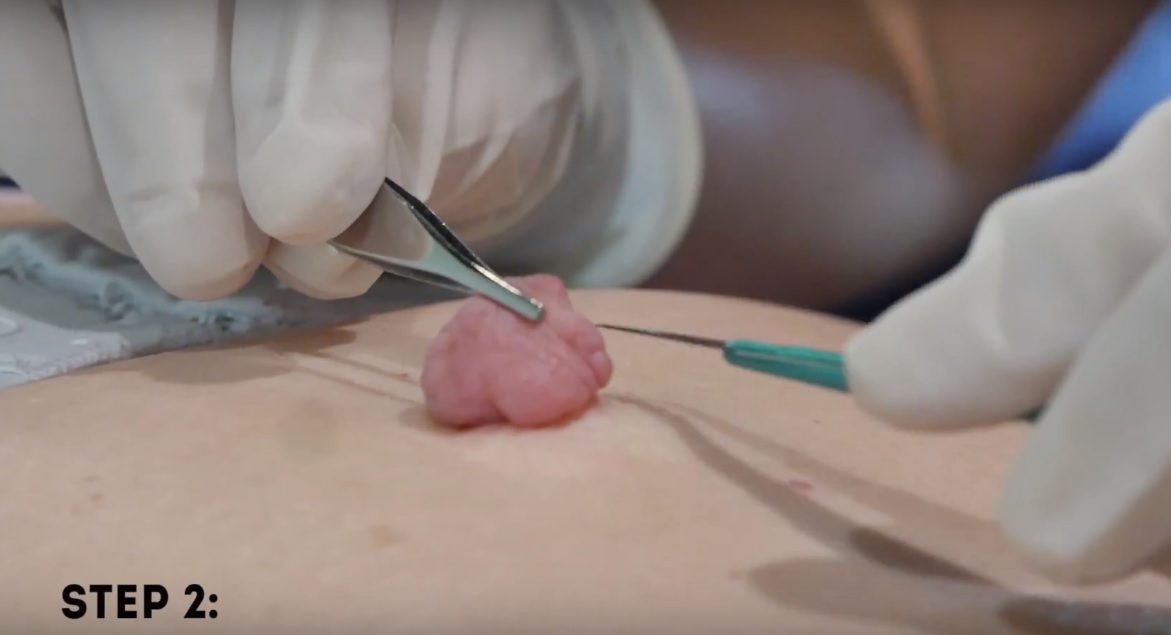
Several options are available to remove spider veins — thin red lines or weblike networks of blood vessels that appear on your legs and feet. Spider veins are usually harmless, though they can sometimes cause aching, burning or pain, especially when you've been standing for long periods. If you have symptoms or are concerned about the appearance of spider veins, treatment options include: Sclerotherapy. In this procedure, your doctor injects the veins with a solution that scars and closes those veins, causing the blood to reroute through healthier veins. In a few weeks, treated spider veins fade. Although the same vein may need to be injected more than once, sclerotherapy is usually effective if done correctly. Sclerotherapy doesn't require anesthesia and can be done in your doctor's office. Side effects include swelling, itching and skin color changes in the treated area. Laser surgery. Laser surgery works by sending strong bursts of light into the vein that make the vein slowly fade and disappear. No incisions or needles are used. The treatment is often less effective than sclerotherapy, particularly for larger veins. Side effects may include redness, bruising, itching, swelling and permanent skin tone changes. After treatment, blood vessels fade over several months, but they may not disappear completely. Also, new spider veins can develop in the same area.

Acute sinusitis can be triggered by a cold or allergies and may resolve on its own. Chronic sinusitis lasts up to eight weeks and may be caused by an infection or growths. Symptoms include headache, facial pain, runny nose, and nasal congestion. Acute sinusitis usually doesn't require any treatment beyond symptomatic relief with pain medications, nasal decongestants, and nasal saline rinses. Chronic sinusitis may require antibiotics.