Top videos
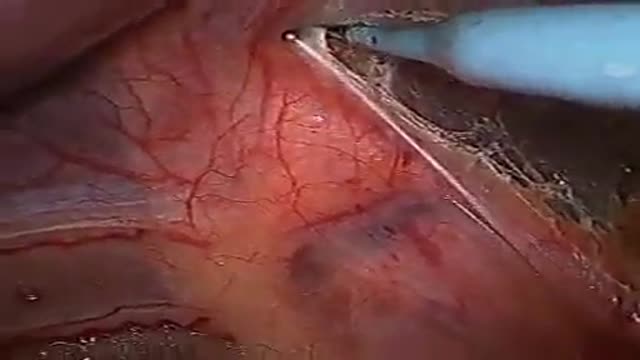
Austin arm lift surgery (also commonly referred to as Brachioplasty) reduces excess skin and tissue from the under arm region, leaving the patient with smoother, more contoured arms. Visit http://www.austinplasticsurgery.com/body-contouring.php for more info.

Valvular stenosis occurs when one or more heart valves are narrowed, stiffened, thickened or blocked. A variety of treatment options are available for this disorder. Learn more about the treatments on: bit.ly/2g6Mh8f
There are currently 2 types of pneumococcal vaccines: pneumococcal conjugate vaccine (PCV13 or Prevnar 13®) and pneumococcal polysaccharide vaccine (PPSV23 or Pneumovax®). PCV13 is recommended for all children younger than 5 years old, all adults 65 years or older, and people 6 years or older with certain risk factors.

During in vitro fertilization (IVF), eggs and sperm are brought together in a laboratory glass dish to allow the sperm to fertilize an egg. With IVF, you can use any combination of your own eggs and sperm and donor eggs and sperm. After IVF, one or more fertilized eggs are placed in the uterus .

High blood pressure and high cholesterol are the most common causes of these spasms. Approximately 2 percent of people with angina, or chest pain and pressure, experience coronary artery spasms. Coronary artery spasms can also occur in people who have atherosclerosis.

A pheochromocytoma (fee-o-kroe-moe-sy-TOE-muh) is a rare, usually noncancerous (benign) tumor that develops in cells in the center of an adrenal gland. You have two adrenal glands, one above each kidney. Your adrenal glands produce hormones that give instructions to virtually every organ and tissue in your body. If you have a pheochromocytoma, an adrenal gland releases hormones that cause persistent or episodic high blood pressure. If left untreated, a pheochromocytoma can result in severe or life-threatening damage to other body systems, especially the cardiovascular system. Most people with a pheochromocytoma are between the ages of 20 and 50, but the tumor can develop at any age. Surgical treatment to remove a pheochromocytoma usually returns blood pressure to normal.

Paget's disease of the breast or Paget disease of the breast (/ˈpædʒᵻt/, rhymes with "gadget") (also known as Paget's disease of the nipple) is a malignant condition that outwardly may have the appearance of eczema, with skin changes involving the nipple of the breast.
What is heparin injection? Heparin is an anticoagulant (blood thinner) that prevents the formation of blood clots. Heparin is used to treat and prevent blood clots in the veins, arteries, or lung. It is also used before surgery to reduce the risk of blood clots. Heparin works by inactivating thrombin in the clotting process. This stops the formation of fibrin and so stops blood clots forming. Heparin is used to treat blood clots that have formed abnormally inside the blood vessels. It can also be used to prevent these types of dangerous blood clots.

The majority of epileptic seizures are controlled by medication, particularly anticonvulsant drugs. The type of treatment prescribed will depend on several factors, including the frequency and severity of the seizures and the person's age, overall health, and medical history. An accurate diagnosis of the type of epilepsy is also critical to choosing the best treatment. Drug Therapy Many drugs are available to treat epilepsy. Although generic drugs are safely used for most medications, anticonvulsants are one category where doctors proceed with caution. Most doctors prefer to use brand-name anticonvulsants, but realize that many insurance companies will not cover the cost. As a result, it is acceptable to start taking a generic anticonvulsant medication, but if the desired control is not achieved, the patient should be switched to the brand-name drug.
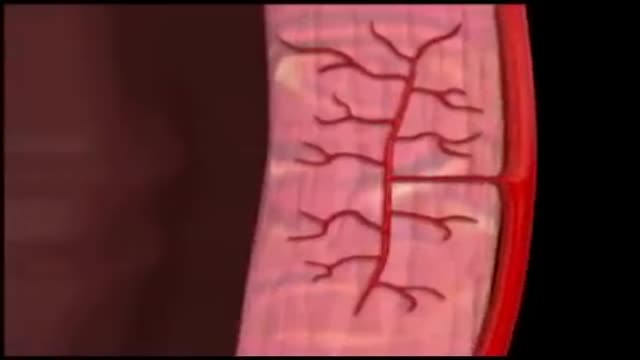
Coronary circulation is the circulation of blood in the blood vessels of the heart muscle (myocardium). The vessels that deliver oxygen-rich blood to the myocardium are known as coronary arteries. The vessels that remove the deoxygenated blood from the heart muscle are known as cardiac veins.

Triglycerides are a type of fat (lipid) found in your blood. When you eat, your body converts any calories it doesn't need to use right away into triglycerides. The triglycerides are stored in your fat cells. Later, hormones release triglycerides for energy between meals. If you regularly eat more calories than you burn, particularly "easy" calories like carbohydrates and fats, you may have high triglycerides (hypertriglyceridemia).

Gastroparesis is a disorder affecting people with both type 1 and type 2 diabetes in which the stomach takes too long to empty its contents (delayed gastric emptying). The vagus nerve controls the movement of food through the digestive tract. If the vagus nerve is damaged or stops working, the muscles of the stomach and intestines do not work normally, and the movement of food is slowed or stopped. Just as with other types of neuropathy, diabetes can damage the vagus nerve if blood glucose levels remain high over a long period of time. High blood glucose causes chemical changes in nerves and damages the blood vessels that carry oxygen and nutrients to the nerves. - See more at: http://www.diabetes.org/living-with-diabetes/complications/gastroparesis.html?referrer=https://www.google.com/#sthash.rTgZiOuM.dpuf

It's a symptom of heart disease but typically does not cause permanent damage to the heart. It is, though, a sign that you are a candidate for a heart attack at some point in the future. The chest pain may spread to your arm, shoulder, jaw, or back. It may feel like a pressure or squeezing sensation.
Surgery is the only way to treat parathyroid disease (hyperparathyroidism). There are no medications or pills that work to cure or treat parathyroid problems or high calcium. The parathyroid tumor must be removed by a surgeon. As soon as the parathyroid tumor has been removed, you are cured! It is very likely this will change your life. If you have hyperparathyroidism you need to have parathyroid surgery. If you have an expert surgeon this operation should be very easy.

The eyes A close up of a young person's eyes. The eyes are responsible for four-fifths of all the information our brain receives. Here you can find out a bit more about how they work, common problems that affect vision and the work Sightsavers does to treat and prevent avoidable blindness. You can also find out more about the people whose lives have been changed thanks to donations from people like you. How do eyes work? (click image to see enlarged version or click here for text alternative) Graphic of an eye with information about its different parts The images we see are made up of light reflected from the objects we look at. This light enters the eye through the cornea. Because this part of the eye is curved, it bends the light, creating an upside down image on the retina (this is eventually put the right way up by the brain). The retina is a complex part of the eye, but only the very back of it is light sensitive. This part of the retina has roughly the area of a 10p coin, and is packed with photosensitive cells called rods and cones. Cones are the cells responsible for daylight vision. There are three kinds – each responding to a different wavelength of light: red, green and blue. The cones allow us to see images in colour and detail. Rods are responsible for night vision. They are sensitive to light but not to colour. In darkness, the cones do not function at all. How do we see an image? The lens focuses the image. It can do this because it is adjustable – using muscles to change shape and help us focus on objects at different distances. The automatic focusing of the lens is a reflex response and is not controlled by the brain. Once the image is clearly focused on the sensitive part of the retina, energy in the light that makes up that image creates an electrical signal. Nerve impulses can then carry information about that image to the brain through the optic nerve.

Researchers believe that the infectious agent that causes mad cow disease is an abnormal version of a protein normally found on cell surfaces, called a prion. For reasons still unknown, this protein becomes altered and destroys nervous system tissue -- the brain and spinal cord.