Top videos
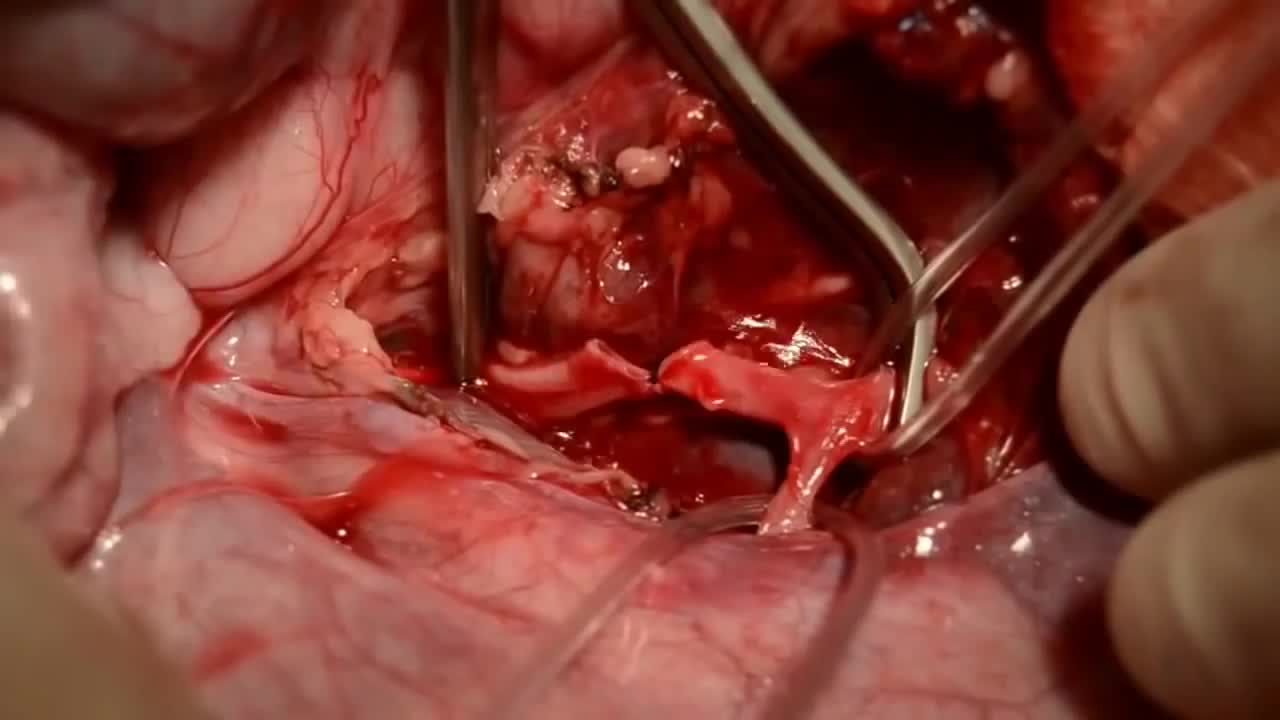
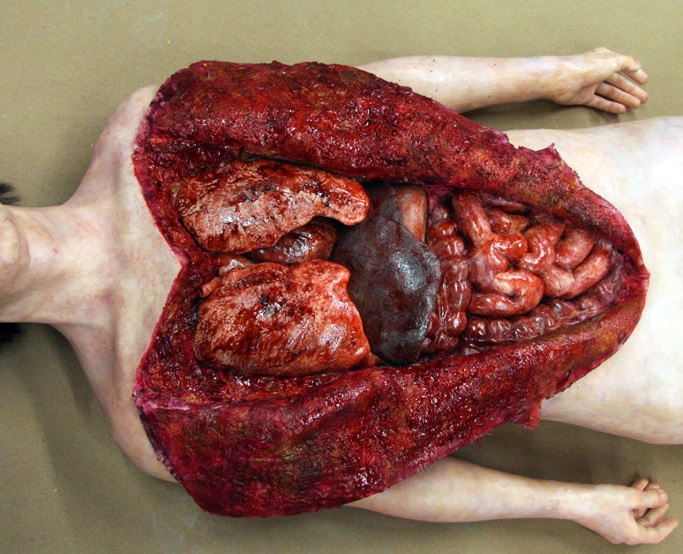
Throughout the body, there are several points at which blood vessels unite. The junctions are termed anastomoses. In the simplest sense, an anastomosis is any connection (made surgically or occurring naturally) between tube-like structures. Naturally occurring arterial anastomoses provide an alternative blood supply to target areas in cases where the primary arterial pathway is obstructed. They are most abundant in regions of the body where the blood supply may can be easily damaged or blocked (such as the joints or intestines). This article focuses on the arterial anastomotic networks of the upper limb.

Shoulder Clinical Examination - Medical School Clinical Skills - Dr Gill
Personally, I find the shoulder examination the most complex examination possibly as there are so many variations and special tests. Some of which overlap and some will relate specifically to a patients presentation.
Often in a medical school syllabus, only select special tests will be used. In this shoulder exam demonstration, we include the Hawkins-Kennedy Test looking for impingement. This is dovetailed with examination for bicipital tendonitis as this is another possible cause of impingement type symptoms.
This shoulder upper limb exam follows the standard "Look, Feel, Move" orthopaedic exam approach, and overall order as set out in MacLeods Clinical Examination
Watch further orthopaedic examinations for your OSCE revision:
The Spine Examination:
https://youtu.be/pJxMHa6SCgU
Knee Examination
https://youtu.be/oyKH4EYfJDM
Hip Joint Clinical Examination
https://youtu.be/JC9GKq5nSdQ
________
Please note that there is no ABSOLUTE way to perform a clinical examination. Different institutions and even clinicians will have differing degrees of variations - the aim is the effectively identify medically relevant signs.
However during OSCE assessments. Different medical schools, nursing colleges, and other health professional courses will have their own preferred approach to a clinical assessment - you should concentrate on THEIR marks schemes for your assessments.
The examination demonstrated here is derived from Macleods Clinical Examination - a recognized standard textbook for clinical skills.
#ShoulderExamination #ClinicalSkills #DrGill
Purpose: To evaluate the results of LASIK and IntraLASIK treatment in myopic patients with nystagmus. Methods: Eight patients with congenital nystagmus (16 eyes), from 23 to 49 years of age, underwent LASIK surgery. Corneal flaps were created using either the Hansatome microkeratome or the Intral...ase femtosecond laser. The ablations were performed with the Bausch & Lomb excimer laser with an active tracking system. In some patients, the eyes were fixated with forceps or a fixation ring during the laser ablation. Results: The refractive errors were corrected in all cases. There was no decentration or loss of best corrected visual acuity greater than 1 line. In 56% of the eyes, the post-operative uncorrected visual acuity was better than the best spectacle corrected-visual acuity (BSCVA). 62.5% of the eyes improved their BSCVA. The overall visual performance was improved in all the patients. One patient that did not not drive before become eligible to get a driver license after the surgery. Conclusions: Selected patients with myopia and congenital nystagmus may benefit from laser refractive surgery. Laser refractive surgery may be safely and accurately performed by using either the Hansatome microkeratome or the Intralase femtosecond laser and an active tracking system with or without mechanical fixation. Certain patients improve their BSCVA post-operatively.
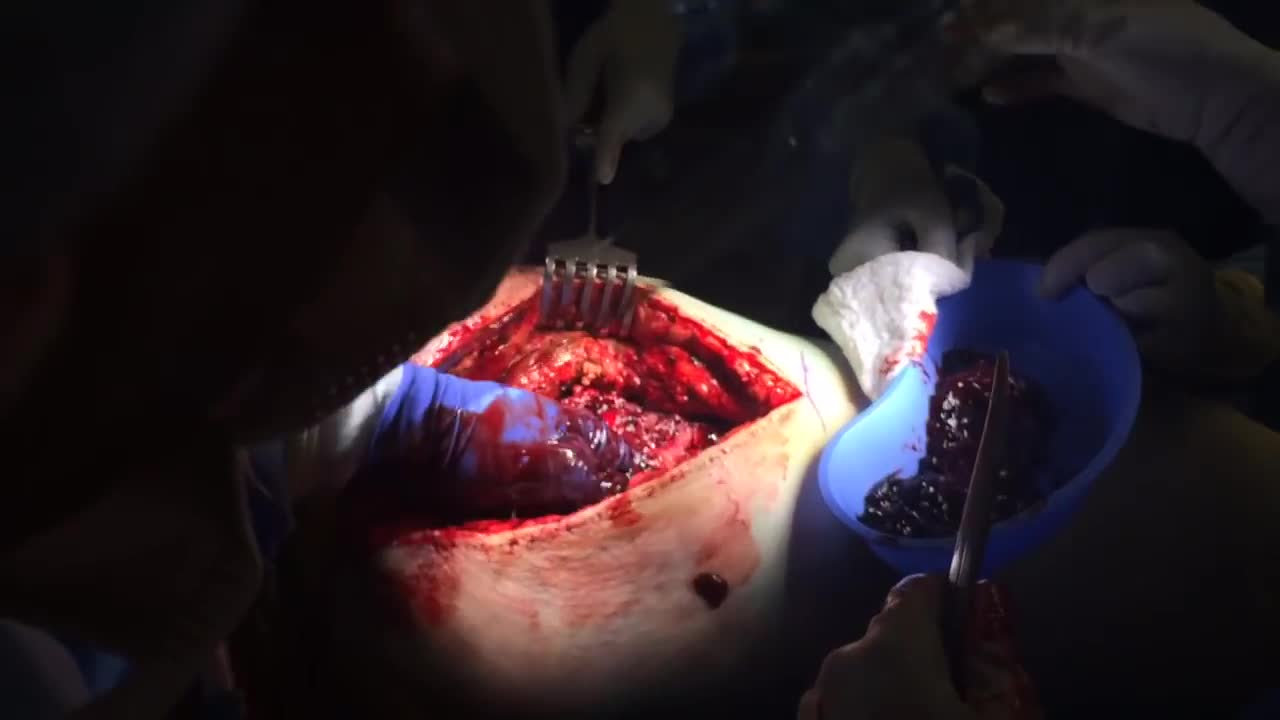
A hematoma is a common complication of surgical procedures. A large, expanding hematoma can result in necrosis of the overlying skin (1,2) or adjacent subcutaneous fat, increased incidence of infection, scarring, skin hyperpigmentation, tissue edema and a prolonged convalescence.
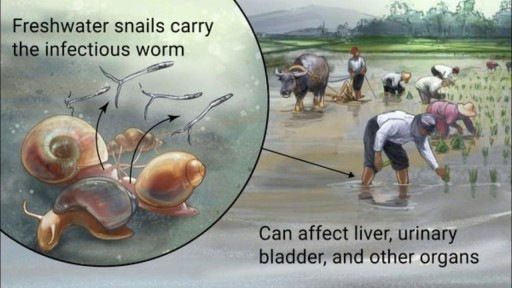
Schistosomiasis is a parasitic disease caused by flukes (trematodes) of the genus Schistosoma. After malaria and intestinal helminthiasis, schistosomiasis is the third most devastating tropical disease in the world, being a major source of morbidity and mortality for developing countries in Africa, South America, the Caribbean, the Middle East, and Asia. (See Epidemiology and Prognosis.) [1] More than 207 million people, 85% of who live in Africa, are infected with schistosomiasis, [1] and an estimated 700 million people are at risk of infection in 76 countries where the disease is considered endemic, as their agricultural work, domestic chores, and recreational activities expose them to infested water. [1, 2] Globally, 200,000 deaths are attributed to schistosomiasis annually. [3] Transmission is interrupted in some countries. [2] (See Etiology and Epidemiology.)
Ettore Vulcano, MD, Foot and Ankle Orthopedic Surgeon at Mount Sinai West, discusses a new minimally invasive bunion surgery that has patients walking immediately after surgery, and getting back to an active lifestyle much quicker than with the traditional surgery.

Train with some of the region’s very best pediatric general surgeons — in a two-year, pediatric surgical fellowship training program at Nemours/Alfred I. duPont Hospital for Children. Our hospital’s Division of Pediatric Surgery is offering this program in affiliation with Sidney Kimmel Medical College at Thomas Jefferson University .
The goal of the fellowship is to give individuals who have completed an accredited general surgery residency advanced knowledge and training in the management and surgical treatment of newborns, infants and children.
Our Fellowship Program
This fellowship will help you prepare for certification by the American Board of Surgery, and is accredited by the Accreditation Council for Graduate Medical Education (ACGME).
The Pediatric Surgery Fellowship aims to:
train a well-rounded, empathetic, safe pediatric surgeon who is confident managing all aspects of the surgical care of children.
steward our fellow in quality improvement projects and methodology, and provide research opportunities.
provide a rigorous didactic curriculum for our fellow utilizing 360 degree feedback.
cultivate opportunities for our fellow to educate residents and students.
encourage our fellow to collaborate across specialties.
develop our fellow’s presentation skills during M&M conferences and multi-disciplinary educational meetings.
The program features the full participation of all nine of the pediatric surgical division’s full-time faculty members. Each of these physicians will contribute greatly to your education. Your training will include operating room and outpatient clinic experience, as well as bedside evaluation of children. You’ll also play a role in the organization of formal teaching conferences, held weekly. Formal rotations will be spent on Pediatric Urology, PICU and Neonatology during the first 12 months. The last year will be spent entirely on the Pediatric Surgical Service.
The majority of your inpatient consultative time will take place at Nemours/Alfred I. duPont Hospital for Children, a freestanding children’s hospital in Wilmington, Del. The hospital:
is nationally ranked by U.S. News & World Report in eight pediatric specialties
recently opened expansion with 260 beds
performs more than 2,800 inpatient and 9,300 outpatient surgical procedures each year in our operating rooms
has an on-site delivery center for newborns with complex congenital anomalies
receives more than 50,000 annual visits in our Emergency Department (ED)
is accredited by The American College of Surgeons as a Level One Pediatric Trauma Center
is accredited by the Commission on Accreditation of Rehabilitation Facilities (CARF)
Visit https://www.nemours.org/educat....ion/gme/fellowships/ to learn more.
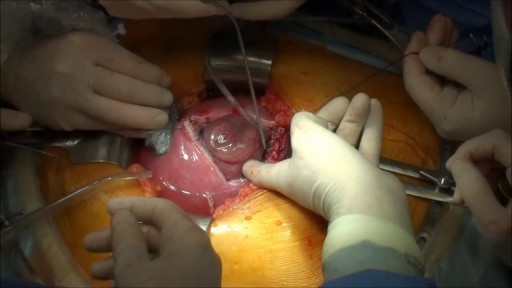
Prenatal repair of myelomeningocele (MMC), the most common and severe form of spina bifida, is a delicate surgical procedure where fetal surgeons open the uterus and close the opening in the baby's back while they are still in the womb.
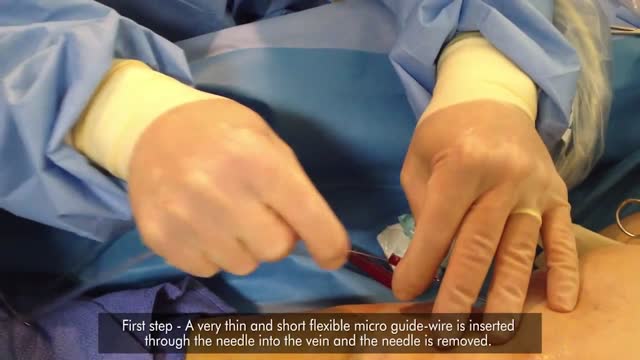
It can treat spider veins and tiny varicose veins just under the skin's surface. ... (If you have poor blood circulation feeding these tiny veins, the larger "feeder" vein must first be treated with surgery, endovenous laser or radiofrequency treatment, or sclerotherapy.) Endovenous laser treatment.