Top videos

The eyes A close up of a young person's eyes. The eyes are responsible for four-fifths of all the information our brain receives. Here you can find out a bit more about how they work, common problems that affect vision and the work Sightsavers does to treat and prevent avoidable blindness. You can also find out more about the people whose lives have been changed thanks to donations from people like you. How do eyes work? (click image to see enlarged version or click here for text alternative) Graphic of an eye with information about its different parts The images we see are made up of light reflected from the objects we look at. This light enters the eye through the cornea. Because this part of the eye is curved, it bends the light, creating an upside down image on the retina (this is eventually put the right way up by the brain). The retina is a complex part of the eye, but only the very back of it is light sensitive. This part of the retina has roughly the area of a 10p coin, and is packed with photosensitive cells called rods and cones. Cones are the cells responsible for daylight vision. There are three kinds – each responding to a different wavelength of light: red, green and blue. The cones allow us to see images in colour and detail. Rods are responsible for night vision. They are sensitive to light but not to colour. In darkness, the cones do not function at all. How do we see an image? The lens focuses the image. It can do this because it is adjustable – using muscles to change shape and help us focus on objects at different distances. The automatic focusing of the lens is a reflex response and is not controlled by the brain. Once the image is clearly focused on the sensitive part of the retina, energy in the light that makes up that image creates an electrical signal. Nerve impulses can then carry information about that image to the brain through the optic nerve.

Researchers believe that the infectious agent that causes mad cow disease is an abnormal version of a protein normally found on cell surfaces, called a prion. For reasons still unknown, this protein becomes altered and destroys nervous system tissue -- the brain and spinal cord.
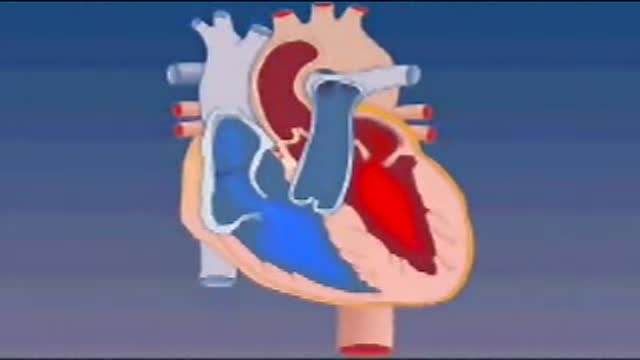
Blood enters the heart through two large veins, the inferior and superior vena cava, emptying oxygen-poor blood from the body into the right atrium. As the atrium contracts, blood flows from your right atrium into your right ventricle through the open tricuspid valve.
A chalazion is a swollen bump on the eyelid. It happens when the eyelid’s oil gland clogs up. It may start as an internal hordeolum (stye). At first, you might not know you have a chalazion as there is little or no pain. But as it grows, your eyelid may get red, swollen, and sometimes tender to touch. If the chalazion gets large, it can press on your eye and cause blurry vision. Rarely, the whole eyelid might swell.
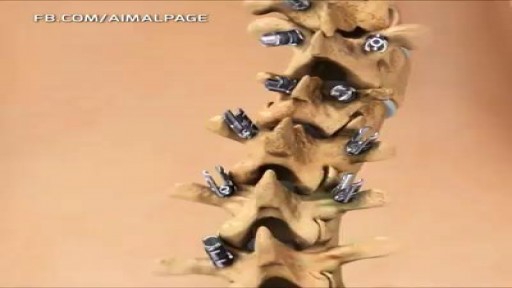
Scoliosis is a sideways curvature of the spine that occurs most often during the growth spurt just before puberty. While scoliosis can be caused by conditions such as cerebral palsy and muscular dystrophy, the cause of most scoliosis is unknown. Most cases of scoliosis are mild, but some children develop spine deformities that continue to get more severe as they grow. Severe scoliosis can be disabling. An especially severe spinal curve can reduce the amount of space within the chest, making it difficult for the lungs to function properly. Children who have mild scoliosis are monitored closely, usually with X-rays, to see if the curve is getting worse. In many cases, no treatment is necessary. Some children will need to wear a brace to stop the curve from worsening. Others may need surgery to keep the scoliosis from worsening and to straighten severe cases of scoliosis.

Que Es Bueno Para La Impotencia Del Hombre, Problemas Para Mantener La Erección, Que Es Erección.--- http://erecciones-increibles.good-info.co --- 5 Errores comunes que empeoran tu disfunción eréctil, Cuando se trata de problemas de salud, a menudo somos nuestros peores enemigos. Esto se ve en muchos casos y con una variedad de enfermedades. Las personas que saben que tienen la presión arterial elevada y colesterol alto no cambian su dieta y siguen comiendo un montón de comida frita, por ejemplo. La disfunción eréctil no es diferente. Aquí hay cinco cosas que podrías estar haciendo en este momento, hoy, que están empeorando tu estado. Estás comiendo (y bebiendo) cosas malas Cafeína. Alcohol. Nicotina. Drogas. Exceso de grasa. Si disfrutas de cualquiera de estas cosas habitualmente, la triste verdad es que estás empeorando tu disfunción eréctil. Incluso si haces otras cosas para mejorar tu estado - incluso si tomas medicación para compensarlo, esas cosas serán menos eficaces de lo que podrían ser a menos que reduzcas dramáticamente o elimines los ítems mencionados anteriormente. No estás comiendo suficiente cosas buenas A continuación se presenta una corta lista de alimentos para aumentar tu salud vascular, lo que a su vez, mejorará la calidad de tus erecciones: granos enteros, verduras de hojas verdes, frutas (especialmente la sandía y arándanos), y ostras. Si te gusta todo lo de esa lista, estás de suerte. Come más de todo eso y vas a ver que los síntomas de la disfunción eréctil disminuyen considerablemente, y posiblemente incluso desaparezcan. Si actualmente no estás comiendo ninguno de los anteriormente, entonces definitivamente estás empeorando el problema. En sí misma, la dieta puede no ser completamente capaz de curar tu disfunción eréctil, pero puede hacer una gran diferencia y tener un tremendo impacto en la calidad de tus erecciones. Esta es la única cura comprobada para la disfunción eréctil que es 100% segura y natural, y combina un secreto ancestral de los amantes más viriles del mundo con ciencia moderna y revolucionaria… Ingresa ahora a: http://erecciones-increibles.good-info.co
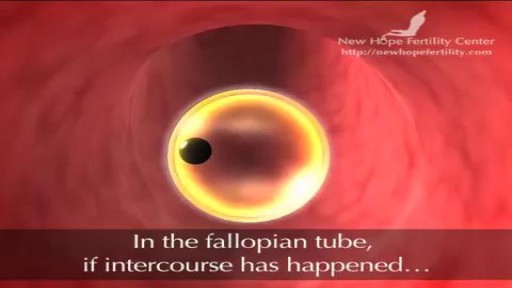
Before ovulation occurs, the average diameter of the dominant follicle is 22 to 24 mm (range 18-36 mm). It is the only marker that can predict ovulation with ease. * In stimulated cycle (hormonal treatment), generally, all or most of the antral follicles grow. The growth rate will be different for each of them.
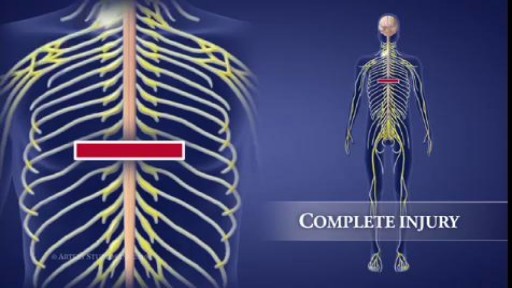
The spine is made flexible by discs located between each vertebra and ligaments made of tough elastic fibers which hold the vertebrae together. The spine gives the body stability and protects the spinal cord which is located in a narrow canal that runs through the center of each vertebra.
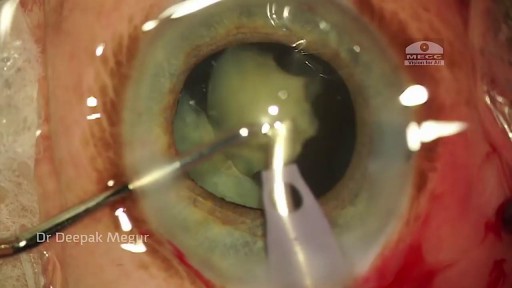
Phacolytic glaucoma usually is associated with a mature or hypermature cataract and typically occurs in elderly patients. Today, phacolytic glaucoma is rare in the United States, found primarily in areas where access to care is poor. Will the increase in the number of under- and uninsured patients lead to an increase in this condition? Evaluation and Diagnosis Signs and symptoms. Patients typically report acute-onset pain, decreased vision, tearing and photophobia. Examination will reveal injection, corneal edema, elevated IOP, anterior chamber reaction with or without pseudohypopyon, particles on the lens capsule and anterior capsule wrinkling. Patient history. The duration of symptoms should be elicited; a delayed presentation of more than five days since onset can result in glaucomatous disc damage and poorer prognosis.¹ The ocular history may reveal that the patient decided against removal of an advanced cataract. Prior intraocular surgery or trauma may have left residual lens material that could cause phacoanaphylactic glaucoma or exacerbate infectious endophthalmitis. Visual acuity and visual potential should be assessed. Exam essentials. A complete ophthalmologic examination should be done. The eye should be inflamed, and the cornea may be edematous due to the high IOP. The anterior chamber will demonstrate massive inflammation and/ or pseudohypopyon. Gonioscopy is essential; it will help rule out angle closure due to phacomorphic glaucoma or neovascularization of the angle. Assess ment of the posterior pole should be performed to rule out vitreous hemorrhage (which can result in ghost-cell glaucoma) or vitritis (which may be associated with infectious endophthalmitis or panuveitis). If the view to the fundus is obstructed, B-scan ultrasonography also should be performed. Differential diagnosis. The differential diagnosis includes infectious endophthalmitis, phacoanaphylactic glaucoma, inflammatory glaucoma, glaucoma secondary to intraocular tumor, phacomorphic glaucoma, acute-angle closure glaucoma and neovascular glaucoma. Management Medication. Medical management is used to temporarily control the glaucoma and inflammation. Initial treatment consists of hyperosmotic agents, aqueous suppressants, anti-inflammatory drugs and cycloplegics. Surgery. Definitive treatment is removal of the lens via extracapsular cataract extraction with or without an IOL. Some ophthalmologists defer placement of an IOL until after the inflammation subsides; however, there is no significant difference in final visual acuity between those patients who did receive an IOL and those who did not.¹ If the phacolytic glaucoma is of long duration (more than seven days), a combined trabeculectomy may be needed to prevent postoperative IOP spikes.² In eyes with hypermature Morgagnian cataracts, one must be especially careful, as the capsule is fragile, the zonules are weak and the view is difficult due to the white, milky cortex. Vision limited to light perception on presentation is not a contraindication to performing cataract extraction. Surgical Tips For a planned extracapsular cataract extraction with a posterior chamber IOL, fashion a superior fornix-based conjunctival flap.³ Make a partial-thickness incision along the sclerolimbal junction superiorly for 120 degrees with a No. 69 blade. Forty-five degrees away, a paracentesis should be done to decompress the eye. The anterior chamber fluid can be withdrawn for analysis, to look for macrophages and high molecular-weight proteins. Inject balanced salt solution in a cannula to wash out any residual particulate matter, then inject Healon or viscoelastic into the anterior chamber. Make an incision entering the anterior chamber at the 12 o’clock position with a keratome. A 26-gauge cystotome mounted on a syringe is then introduced through the 12 o’clock incision and used to puncture the capsular bag. The milky cortex should be aspirated as much as possible, until the nucleus is visible. Withdraw the needle through the keratome incision, then inject Healon through the 12 o’clock incision into the capsular bag. Next, enlarge the corneoscleral keratome incision with curved Westcott scissors to 120 degrees. Perform a partial V-shaped capsulotomy; this can be done either with the cystotome or with an angled Vannas scissors. Place viscoelastic under the nucleus to float the nucleus and sever any adhesions between the nucleus and the capsule. The nuclear portion of the lens can then be removed with an irrigating vectis (lens loop) with or without gentle pressure at the inferior limbus (6 o’clock). Irrigate and aspirate the residual cortex with the Simcoe cannula. Inspect the capsular bag; if it is intact, place a posterior chamber IOL into the bag. Close the incision with several interrupted 10-0 monofilament nylon sutures and reattach the conjunctival flap. Potential Sequelae and Prognosis Postoperatively, the patient should be managed with topical steroids and/or aqueous suppressants and hyperosmotics if necessary. Vitreous opacification behind the posterior capsule occurs in a small percentage of eyes. These vitreous opacities are typically absorbed by one to two weeks postoperatively. IOP usually is controlled without antiglaucoma medications after the cataract removal. A detailed glaucoma evaluation (including repeat gonioscopy to assess for peripheral anterior synechiae, visual field and optic nerve status) should be done to assess the extent of glaucomatous damage. The prognosis is dependent on the duration of elevated IOP, PAS and optic nerve damage. In one study, patients who were older than 60 and whose glaucoma was present for more than five days did significantly worse than a comparison group of younger individuals with shorter disease duration.

Like a fine whiskey barrel and wine cellar, cannabis also comes at its best when aged in a dark, cool place. Though there is no steadfast expiration date for cannabis, the method you use for preserving the cannabis makes a big difference in maintaining the buds’ freshness and potency. The question is, how do you store cannabis in a way that could extend its longevity while maintaining the vigor and freshness? Experts have described different methods. However, here are some time-proven methods that are easy and inexpensive and require very less equipment. Use air-tight glass containers to store the weed Use clean air-tight glass containers or jars to store cannabis. You can buy glass containers from any ordinary supermarket or hardware store. The tricky part is to make sure you do leave some air in the container while the air stored with cannabis isn’t in detrimental extent. Always leave 1/4 space at the top of the canister or container. Do not fill the containers to the brim with the buds. If you leave no air, then the buds will dry out. If you have too much air, the buds will get damp and moldy. Freeze your cannabis in a convenient temperature The best way to store your buds is in air-tight glass jars, in a cool and dark place under an ideal temperature between 60 and 70 degrees Fahrenheit. If you need to store a high volume of cannabis, you can freeze them after keeping them completely dry for a period of 4 weeks. On this note, you should know that you must not handle frozen buds until it becomes normal in room temperature as trichomes become brittle and can easily break off in freezing temperature. Refrigerate your cannabis (Not Recommended) Even if you use airtight jars, cannabis can grow mold in the fridge. So, you should avoid storing cannabis in the fridge. If you can’t help but doing it, make sure the weed is completely dry and put them in the back where the humidity and temperature don’t fluctuate. Plastic Baggies (Worst method!) Albeit this is very common among people who aren’t expert in handling cannabis, this is the worst of all storage methods. Cannabis gets brittle and dries out in plastic bags. It also loses its natural smell, and the potency deteriorates sharply. So, it should be avoided entirely or can be used for a short-term if there is no better alternative. Here are some things you should know while storing cannabis - Make sure cannabis has been cured for at least 4 weeks before putting them into long-term storage. Without proper curing before storage, the buds can lose their strength and smoothness. - Sunlight can stop the medicinal qualities of cannabis. Your cannabis, if stored correctly, can maintain its medicinal qualities for a few years. Exposure to Sun will turn your cannabis brown, no matter how you have stored it away. - Air-tight, nonporous glass jar are the best way for storing the buds for long term. You can use metal or plastic box/bag, but that could reduce the smell and taste after a while. - Avoid heat and middling temperature in the place where you store your buds. The ideal temperature is 60-70°F (15-21°C) or under 32°F (0°C). Extra heat, cold or middling temperature cause the cannabis potency to decrease. - Keep your cannabis away from any electronic devices or appliances that will expose the cannabis to heat. Keeping cannabis on top of a microwave, or near a laptop or mobile charge is a bad idea. Now, as you know that how to store cannabis properly and make it last for years, enjoy the best form of your weeds even it comes from the previous year. Do write to us in the comments section if you have any questions. Also, don’t forget to hit the subscribe button below. Visit OnlineMedicalCard.com now to get an MMJ recommendation online in less than 10 minutes.