Top videos

Thyroiditis is a general term that refers to “inflammation of the thyroid gland”. Thyroiditis includes a group of individual disorders causing thyroidal inflammation but presenting in different ways. For example, Hashimoto’s thyroiditis is the most common cause of hypothyroidism in the United States. Postpartum thyroiditis, which causes temporary thyrotoxicosis (high thyroid hormone levels in the blood) followed by temporary hypothyroidism, is a common cause of thyroid problems after the delivery of a baby. Subacute thyroiditis is the major cause of pain in the thyroid. Thyroiditis can also be seen in patients taking the drugs interferon and amiodarone.
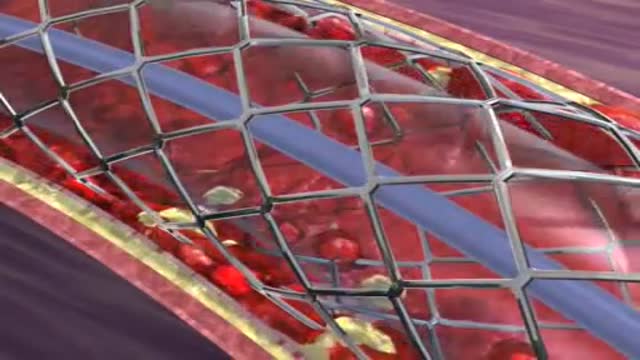
Blood clots form in an already-narrowed artery and block the flow of oxygen-rich blood to the heart muscle. When taken during a heart attack, aspirin slows clotting and decreases the size of the blood clot that is forming. After a heart attack. Aspirin can help prevent a second heart attack.

Adult stem cells are cells from your own body that can renew themselves and turn into other cells (differentiate). They live inside all of us in various tissues, poised to leap into action to repair damage as it occurs. As we age or have big injuries, we may not be able to recruit enough of these cells to the site to fully repair the area. Regenexx Stem Cell Procedures help overcome this problem by extracting stem cells from an area of high volume, then concentrating the cells and reinjecting them into the damaged area to help the body heal naturally.
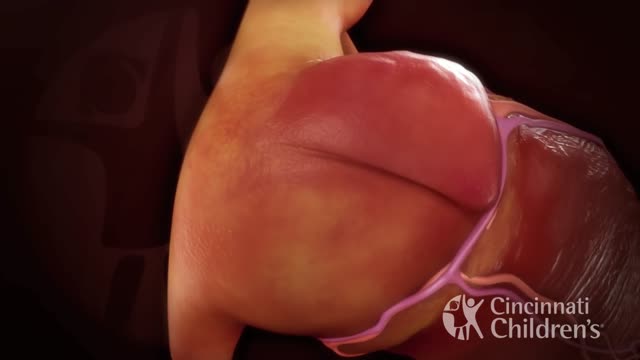
The term hypoplastic left heart syndrome (HLHS), initially proposed by Noonan and Nadas, [1] describes a spectrum of cardiac abnormalities characterized by marked hypoplasia of the left ventricle and ascending aorta. This is the same disorder characterized as hypoplasia of the aortic tract complex by Lev. [2] The aortic and mitral valves are atretic, hypoplastic, or stenotic. A patent foramen ovale or an atrial septal defect is usually present. The ventricular septum is usually intact. A large patent ductus arteriosus supplies blood to the systemic circulation. Systemic arterial desaturation may be present because of complete mixing of pulmonary and systemic venous blood in the right atrium. Coarctation of the aorta is also commonly present. See the images below.
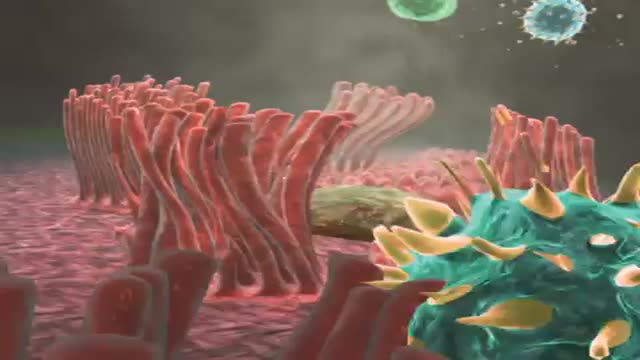
Cells may have slender extensions of the cell membrane to form cilia or the smaller extensions called microvilli. The microscopic microvilli effectively increase the surface area of the cell and are useful for absorption and secretion functions. A dramatic example is the human small intestine. The tissue has small fingerlike extensions called villi which are collections of cells, and those cells have many microvilli to even further increase the available surface area for the digestion process. According to Audesirk & Audesirk, this can give an effective surface area of about 250 square meters for absorption.
Endoscopic retrograde cholangiopancreatography, or ERCP, is a specialized technique used to study the bile ducts, pancreatic duct and gallbladder. Ducts are drainage routes; the drainage channels from the liver are called bile or biliary ducts. The pancreatic duct is the drainage channel from the pancreas.

Breast lump removal is surgery to remove a lump that may be breast cancer. Tissue around the lump is also removed. This surgery is called a lumpectomy. When a noncancerous tumor such as a fibroadenoma of the breast is removed, it is often called an excisional breast biopsy, instead of a lumpectomy
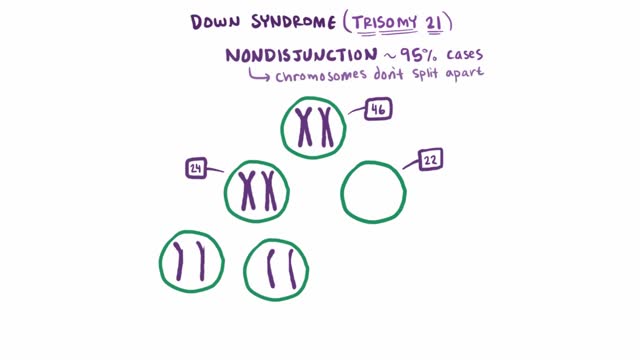
The term trisomy is used to describe the presence of three chromosomes, rather than the usual matched pair of chromosomes. For example, if a baby is born with three #21 chromosomes, rather than the usual pair, then the baby would be said to have "trisomy 21." Trisomy 21 is also known as Down syndrome. Other examples of trisomy include syndromes like trisomy 18 and trisomy 13. Again, trisomy 18 or trisomy 13 simply means the child has three copies of the #18 chromosome (or of the #13 chromosome) present in each cell of the body, rather than the usual pair.

Sex easily falls to the wayside during pregnancy. Research shows that good sex has a significant impact upon not just the relationship, but also a woman’s ability to have an easeful and even joyful birth. Unfortunately, sex during pregnancy can be quite complicated for a variety of physical and emotional reasons. This week’s video will outline how to overcome these hurdles and make sure you continue to enjoy the wonders of sex as you embark on the first steps of parenthood.
Iatrogenic injury to the ureter is a potentially devastating complication of modern surgery. The ureters are most often injured in gynecologic, colorectal, and vascular pelvic surgery. There is also potential for considerable ureteral injury during endoscopic procedures for ureteric pathology such as tumor or lithiasis. While maneuvers such as perioperative stenting have been touted as a means to avoid ureteral injury, these techniques have not been adopted universally, and the available literature does not make a case for their routine use. Distal ureteral injuries are best managed with ureteroneocystostomy with or without a vesico-psoas hitch. Mid-ureteral and proximal ureteral injuries can potentially be managed with ureteroureterostomy. If the distal segment is unsuitable for anastomosis then a number of techniques are available for repair including a Boari tubularized bladder flap, transureteroureterostomy, or renal autotransplantation. In rare cases renal autotransplantation or ureteral substitution with gastrointestinal segments may be warranted to re-establish urinary tract continuity. Laparoscopic and minimally invasive techniques have been employed to remedy iatrogenic ureteral injuries.
Possible complications include: Cardiovascular disease. ... Nerve damage (neuropathy). ... Kidney damage (nephropathy). ... Eye damage (retinopathy). ... Foot damage. ... Skin conditions. ... Hearing impairment. ... Alzheimer's disease.

Cardiovascular disease (CVD) is a general term that describes a disease of the heart or blood vessels. Blood flow to the heart, brain or body can be reduced as the result of a blood clot (thrombosis), or by a build-up of fatty deposits inside an artery that cause the artery to harden and narrow (atherosclerosis).
Sperm Meets Egg: Weeks 1 to 3 of Pregnancy. Something magical is about to happen! Watch as the ovulation process occurs, and then millions of sperm swim upstream on a quest to fertilize an egg. Your due date is calculated from the first day of your last menstrual period

A new study from Mayo Clinic finds the use of the drug therapy etanercept ineffective in treating alcoholic hepatitis, an acute inflammation of the liver caused by excessive consumption of alcohol. Alcoholic hepatitis is a major cause of morbidity and mortality worldwide. Severe alcohol-related liver disease carries a poor prognosis. Several research studies have worked to find a successful treatment for alcoholic hepatitis, but no consensus has been reached on the most effective treatment regimen.
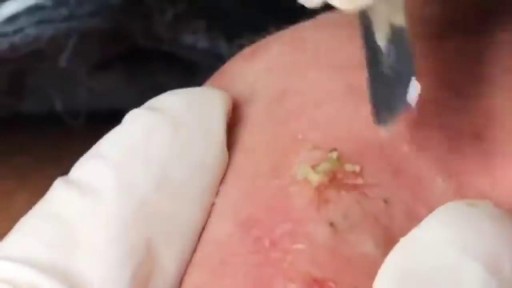
Follow these steps for a successful home extraction: Clean your hands. Wash your hands with soap and warm water. ... Clean your face. Wash and gently exfoliate your face. ... Sterilize your tools. ... Sterilize the pimple. ... Pierce the pimple. ... Create a small tear. ... Release the pus. ... Apply drying lotion


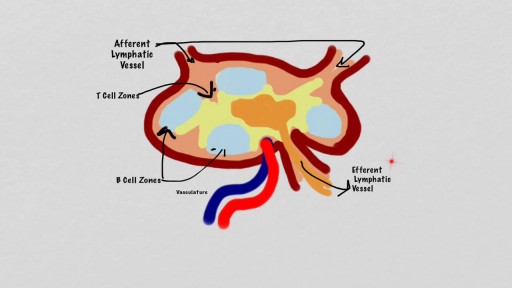
![Kneecap [patella] button loosens after total #kneereplacement #kneeinjury #fracture](https://i.ytimg.com/vi/1pgqwZDgIPs/maxresdefault.jpg)
