Top videos
Bone marrow is the soft, sponge-like material found inside bones. It contains immature cells known as hematopoietic or blood-forming stem cells. (Hematopoietic stem cells are different from embryonic stem cells. Embryonic stem cells can develop into every type of cell in the body.) Hematopoietic stem cells divide to form more blood-forming stem cells, or they mature into one of three types of blood cells: white blood cells, which fight infection; red blood cells, which carry oxygen; and platelets, which help the blood to clot. Most hematopoietic stem cells are found in the bone marrow, but some cells, called peripheral blood stem cells (PBSCs), are found in the bloodstream. Blood in the umbilical cord also contains hematopoietic stem cells. Cells from any of these sources can be used in transplants.
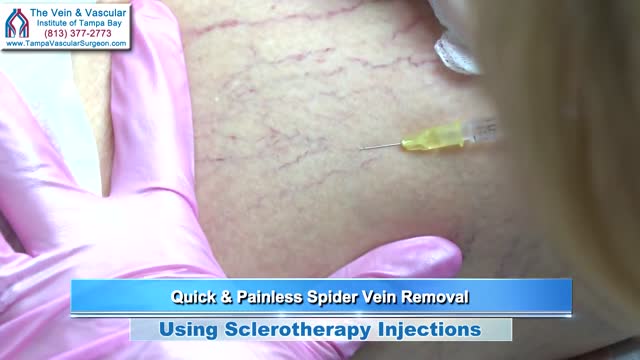
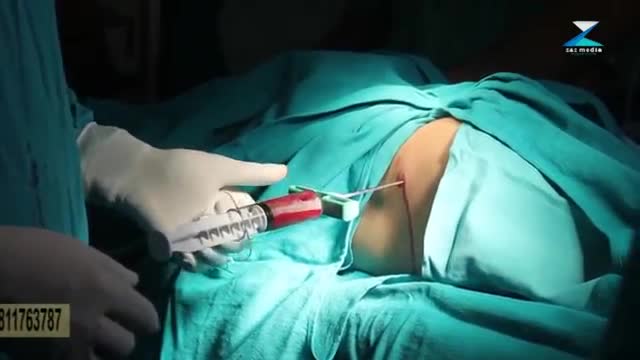
Sclerotherapy is a medical procedure used to eliminate varicose veins and spider veins. Sclerotherapy involves an injection of a solution (generally a salt solution) directly into the vein. The solution irritates the lining of the blood vessel, causing it to collapse and stick together and the blood to clot.

http://dissolve-kidney-stones-fast.good-info.co/ How To Dissolve Kidney Stone Naturally In Home, Herbs For Kidney Stones, Dissolve Kidney Stones. For thousands of years Amazonian Rainforest tribes have been using the Chanca Piedra plants liquid extract herbs to dissolve kidney stones and gallstones. I found out about this incredible plant, phyllanthus niruri, because I use to suffer from kidney stones. Just like you, I have been in the ER for kidney stones suffering incredible kidney pain. I eventually had to have surgery for relief & removal of the stone. It was a horrendous experience and at that point I knew I had to figure out a way to avoid having another kidney stone in my life! I started doing research and found out the Amazon Rainforest had the remedy! The next time I got kidney stone symptoms I quickly started taking Chanca Piedra tincture drops and it dissolved the stone and I passed it easily. My new mission was to help others suffering from stones. Mine were calcium oxalate, perhaps yours are the same type or uric acid, struvite or cystine. You want the most powerful kidney stone treatment available today and our Kidney Stone Crusher is that product. Make no mistake, if you suffer from stones you need this stone breaker and dissolver passing product! It shrinks and dissolves your stones naturally. No more ER visits, no more painful surgeries, expensive medicine, and no more stents! The added benefit of using our Kidney Stone Crusher is that you will cleanse your liver and kidneys at the same time giving you better digestion, regulate your hormones and purify your blood. Increases urination which is a must for passing stones & cleansing. Our product is all organic, natural and sustainably wildcrafted from the Rainforest in Peru. Works on animals as well, dogs, cats, even alpacas! Click the Buy Button now and get started dissolving your stones. http://dissolve-kidney-stones-fast.good-info.co/

More than 1 million Americans suffer a heart attack every year. Traditional symptoms—chest pain or pressure, cold sweat, extreme weakness—are well known. But there are more subtle signs you’re having or are about to have a heart attack that can be easy to miss. If you experience any of the following symptoms, see a doctor. Noticing heart attack signs early and getting prompt treatment can save your life.
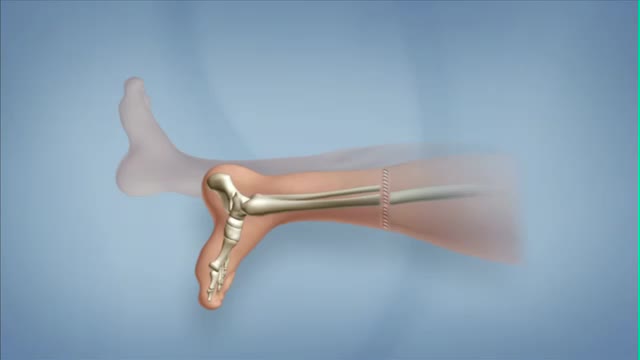
Rotationplasty is a type of autograft wherein a portion of a limb is removed, while the remaining limb below the involved portion is rotated and reattached. This procedure is used when a portion of an extremity is injured or involved with a disease, such as cancer. Typically, the ankle joint becomes the knee joint.
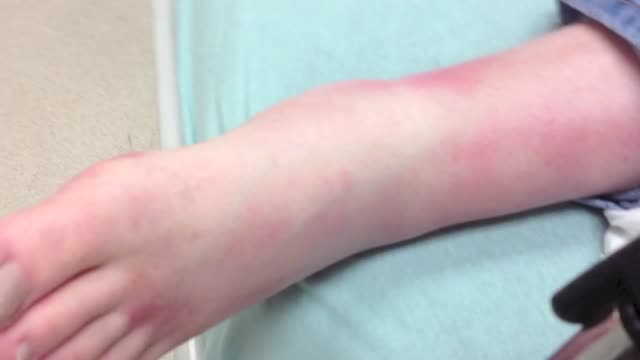
Cellulitis (sel-u-LIE-tis) is a common, potentially serious bacterial skin infection. Cellulitis appears as a swollen, red area of skin that feels hot and tender. It can spread rapidly to other parts of the body. Cellulitis isn't usually spread from person to person. Skin on lower legs is most commonly affected, though cellulitis can occur anywhere on your body or face. Cellulitis might affect only your skin's surface. Or it might also affect tissues underlying your skin and can spread to your lymph nodes and bloodstream. Left untreated, the spreading infection can rapidly turn life-threatening. It's important to seek immediate medical attention if cellulitis symptoms occur.

To identify an UTI, keep an eye out for the following symptoms: A burning feeling when you urinate. A frequent or intense urge to urinate, even though little comes out when you do. Pain or pressure in your back or lower abdomen. Cloudy, dark, bloody, or strange-smelling urine. Feeling tired or shaky.
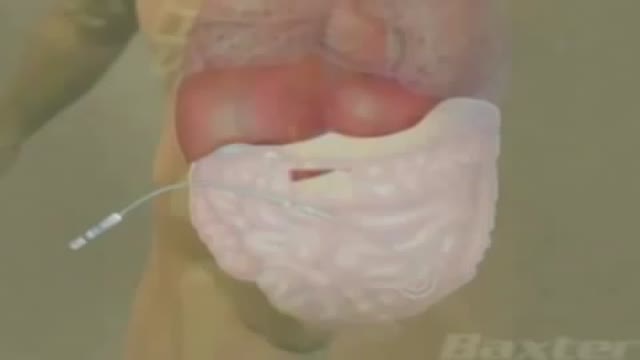
Peritoneal dialysis is a treatment for kidney failure that uses the lining of your abdomen, or belly, to filter your blood inside your body. ... The process of first draining the used dialysis solution and then replacing it with fresh solution is called an exchange.
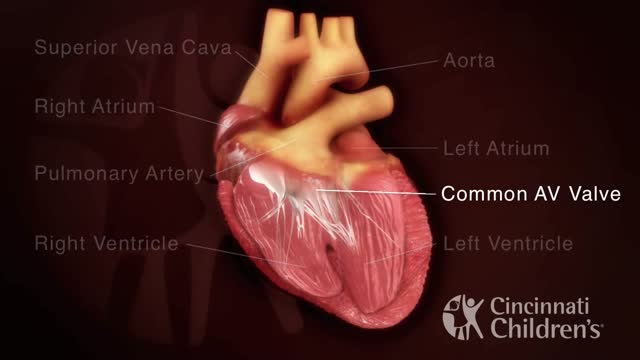
An atrioventricular septal defect (AVSD) is a heart defect in which there are holes between the chambers of the right and left sides of the heart, and the valves that control the flow of blood between these chambers may not be formed correctly

On September 28, 1940 at Columbia Hospital in Columbia, South Carolina, Dr. Austin T. Moore (1899–1963), an American surgeon, reported and performed the first metallic hip replacement surgery. In a total hip replacement (also called total hip arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components. The damaged femoral head is removed and replaced with a metal stem that is placed into the hollow center of the femur.
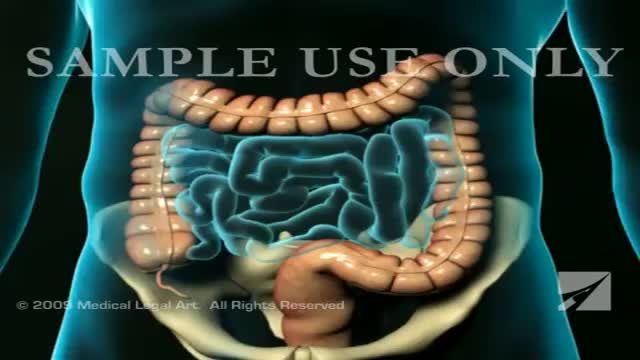
Appendicitis is an inflammation of the appendix, a 3 1/2-inch-long tube of tissue that extends from the large intestine. No one is absolutely certain what the function of the appendix is. One thing we do know: We can live without it, without apparent consequences.
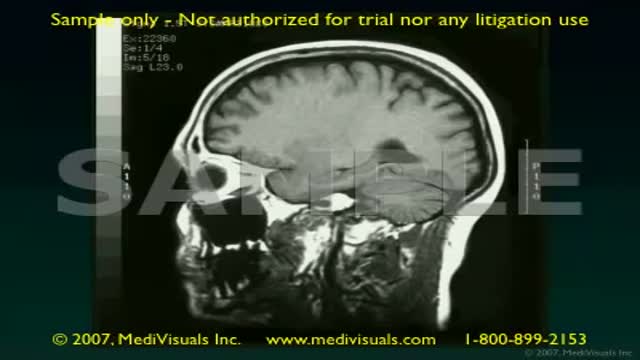
Traumatic brain injury (TBI) is a nondegenerative, noncongenital insult to the brain from an external mechanical force, possibly leading to permanent or temporary impairment of cognitive, physical, and psychosocial functions, with an associated diminished or altered state of consciousness.
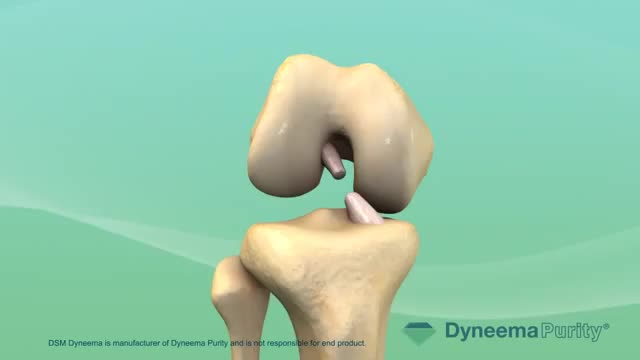
Most people have general anesthesia right before surgery. This means you will be asleep and pain-free. Other kinds of anesthesia, like regional anesthesia or a block, may also be used for this surgery. The tissue to replace your damaged ACL will come from your own body or from a donor. A donor is a person who has died and chose to give all or part of his or her body to help others. Tissue taken from your own body is called an autograft. The two most common places to take tissue from are the knee cap tendon or the hamstring tendon. Your hamstring is the muscle behind your knee. Tissue taken from a donor is called an allograft. The procedure is usually performed with the help of knee arthroscopy. With arthroscopy, a tiny camera is inserted into the knee through a small surgical cut. The camera is connected to a video monitor in the operating room. Your surgeon will use the camera to check the ligaments and other tissues of your knee. Your surgeon will make other small cuts around your knee and insert other medical instruments. Your surgeon will fix any other damage found, and then will replace your ACL by following these steps: The torn ligament will be removed with a shaver or other instruments. If your own tissue is being used to make your new ACL, your surgeon will make a larger cut. Then, the autograft will be removed through this cut. Your surgeon will make tunnels in your bone to bring the new tissue through. This new tissue will be in the same place as your old ACL. Your surgeon will attach the new ligament to the bone with screws or other devices to hold it in place. As it heals, the bone tunnels fill in. This holds the new ligament in place. At the end of the surgery, your surgeon will close your cuts with sutures (stitches) and cover the area with a dressing. You may be able to view pictures after the procedure of what the doctor saw and what was done during the surgery.

A heart attack is a medical emergency. A heart attack usually occurs when a blood clot blocks blood flow to the heart. Without blood, tissue loses oxygen and dies. Symptoms include tightness or pain in the chest, neck, back, or arms, as well as fatigue, lightheadedness, abnormal heartbeat, and anxiety. Women are more likely to have atypical symptoms than men. Treatment ranges from lifestyle changes and cardiac rehabilitation to medications, stents, and bypass surgery.
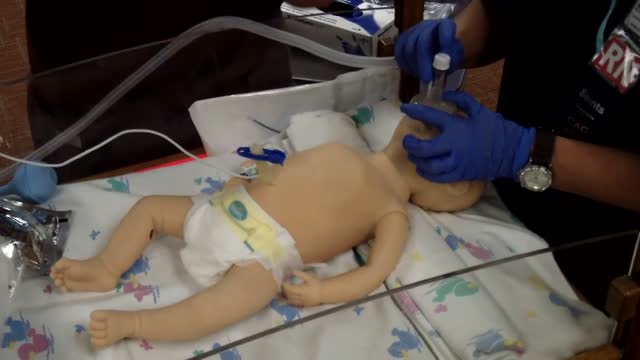
Neonatal resuscitation skills are essential for all health care providers who are involved in the delivery of newborns. The transition from fetus to newborn requires intervention by a skilled individual or team in approximately 10% of all deliveries. This figure is concerning because 81% of all babies in the United States are born in nonteaching, nonaffiliated level I or II hospitals. In such hospitals, the volume of delivery service may not be perceived as sufficient economic justification for the continuous in-hospital presence of personnel with high-risk delivery room experience, as recommended by the American Academy of Pediatrics (AAP) and the American College of Obstetricians and Gynecologists (ACOG). [1] Perinatal asphyxia and extreme prematurity are the 2 complications of pregnancy that most frequently necessitate complex resuscitation by skilled personnel. However, only 60% of asphyxiated newborns can be predicted ante partum. The remaining newborns are not identified until the time of birth. Additionally, approximately 80% of low-birth-weight infants require resuscitation and stabilization at delivery. Nearly one half of newborn deaths (many of which involve extremely premature infants) occur during the first 24 hours after birth. Many of these early deaths also have a component of asphyxia or respiratory depression as an etiology. For the surviving infants, effective management of asphyxia in the first few minutes of life may influence long-term outcome. Even though prenatal care can identify many potential fetal difficulties ante partum, allowing maternal transfer to the referral center for care, many women who experience preterm labor are not identified prospectively and therefore are not appropriately transferred to a tertiary perinatal center. Consequently, many deliveries of extremely premature infants occur in smaller hospitals. For this reason, all personnel involved in delivery room care of the newborn should be trained adequately in all aspects of neonatal resuscitation. Additionally, equipment that is appropriately sized to resuscitate infants of all gestational ages should be available in all delivering institutions, even if the institution does not care for preterm or intensive care infants. Along with the necessary skills, the practitioner should approach any resuscitation with a good comprehension of transitional physiology and adaptation, as well as an understanding of the infant's response to resuscitation. Resuscitation involves much more than possessing an ordered list of technical skills and having a resuscitation team; it requires excellent assessment skills and a grounded understanding of physiology.

Weight loss is the most effective nonpharmacologic measure to decrease blood pressure in overweight individuals. Weight loss with other nonpharmacologic measures can prevent or delay the onset of hypertension and reduce the overall risk of cardiovascular events in such patients. In some patients with established hypertension, lifestyle changes alone may control their blood pressure.
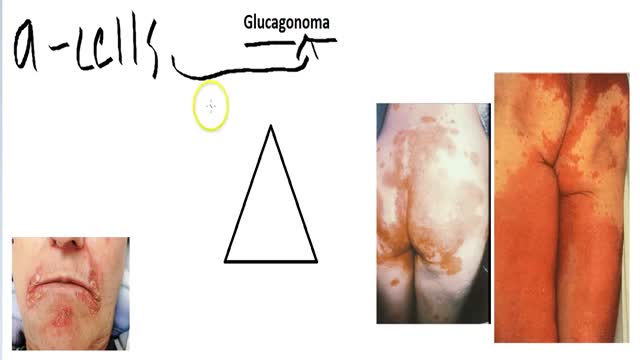
A glucagonoma is a rare tumor of the alpha cells of the pancreas that results in the overproduction of the hormone glucagon. Alpha cell tumors are commonly associated with glucagonoma syndrome, though similar symptoms are present in cases of pseudoglucagonoma syndrome in the absence of a glucagon-secreting tumor.

Alendronate Sodium is used for the following diseases and conditions: osteoporosis, and osteogenesis imperfecta. Alendronate Sodium improves the patient's condition by performing the following functions: slowing down the bone loss and helps to keep the bones strong and less likely to break. Side effects are possible with Alendronate Sodium, but do not always occur. Some of the side effects may be rare but serious. Consult your doctor if you observe any side effects, especially if they do not go away. Alendronate Sodium may cause the following side-effects: stomach pain, constipation, diarrhea, gas, nausea, and jaw pain

Warfarin is an anticoagulant medication - it is used to slow down the blood-clotting process. Anticoagulants are used to prevent blood clots which may cause vein blockages, heart attack and stroke. Warfarin is known under the brand names Warfant, Jantoven, Coumadin, Lawarin, Marevan, and Waran.


