Top videos

Claudication, which is defined as reproducible ischemic muscle pain, is one of the most common manifestations of peripheral arterial occlusive disease (PAOD) caused by atherosclerosis. Claudication occurs during physical activity and is relieved after a short rest. Pain develops because of inadequate blood flow. Examination of a patient with claudication should include a complete lower-extremity evaluation and pulse examination, including measuring segmental pressures. Attempt to palpate pulses from the abdominal aorta to the foot, with auscultation for bruits in the abdominal and pelvic regions. When palpable pulses are not present, a handheld Doppler device may be used to assess circulation.
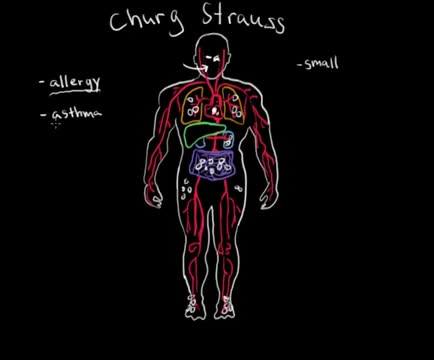
Eosinophilic granulomatosis with polyangiitis (EGPA)—or, as it was traditionally termed, Churg-Strauss syndrome—is a rare systemic necrotizing vasculitis that affects small-to-medium-sized vessels and is associated with severe asthma and blood and tissue eosinophilia. [1] Like granulomatosis with polyangiitis (Wegener granulomatosis), and the microscopic form of periarteritis (ie, microscopic polyangiitis), EGPA is an antineutrophil cytoplasmic antibody (ANCA)–associated vasculitide. [2, 3, 4, 5] In 1951, Churg and Strauss first described the syndrome in 13 patients who had asthma, eosinophilia, granulomatous inflammation, necrotizing systemic vasculitis, and necrotizing glomerulonephritis. [3] In 1990, the American College of Rheumatology (ACR) proposed the following six criteria for the diagnosis of Churg-Strauss syndrome [6] : Asthma (wheezing, expiratory rhonchi) Eosinophilia of more than 10% in peripheral blood Paranasal sinusitis Pulmonary infiltrates (may be transient) Histological proof of vasculitis with extravascular eosinophils Mononeuritis multiplex or polyneuropathy

As a pediatric surgeon at NewYork-Presbyterian/Weill Cornell Medical Center, Dr. Nitsana Spigland treats newborns, children, teens, and young adults requiring surgical interventions. She specializes in antenatal counseling and newborn congenital malformations.
Learn more about Dr. Spigland at: https://www.nyp.org/physician/nspigland.

Today, the most common approach for open-heart surgery is a sternotomy, which requires a 12-14-inch incision through the breastbone. But in the hands of experienced minimally invasive surgeons, many cardiac procedures can be performed through smaller 2- to 3-inch incisions between the ribs without the need to cut through the breastbone. Learn more in this medical animation from Sarasota Memorial's Minimally Invasive Cardiac Surgery Team and medical director Jonathan Hoffberger, DO. For information or referrals, visit smhheart.com.
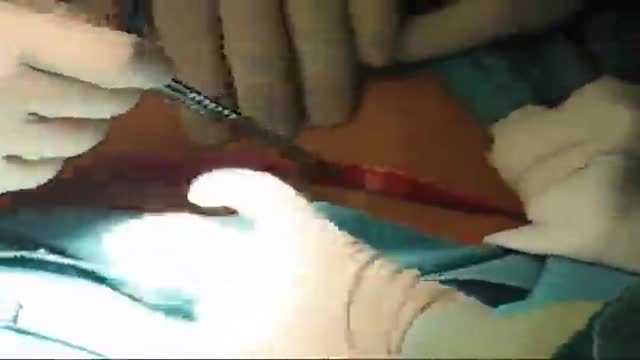
Join Rhinoplasty Specialist Dr. Paul Nassif, a world-renowned expert in revision rhinoplasty, in the operating room as he performs a Columella Strut Placement. His practice, Spalding Drive Cosmetic Surgery & Dermatology, is located in Beverly Hills, CA.
Video Produced by SPORE Medical
"I’m essentially taking care of the baby right now to give them 60 or 70 or 80 years of life so I have to perform my best every time. Every single time. That is a commitment that I have to the parents."
The highest standard. That’s what cardiothoracic surgeon Sergio Carrillo demands of himself every time he steps into the OR. Dr. Carrillo and his Heart Center team at Nationwide Children’s Hospital treat patients with congenital heart disease with the simplest to the most complex procedures.
Connect with a specialist: http://bit.ly/2LU2kJn
The Heart Center at Nationwide Children's: http://bit.ly/2LTQmPR
Advancing cardiac care through research: http://bit.ly/2LXFqAD
Tissue Engineering Research & Innovation: http://bit.ly/2LUD0Ts
Heart & Chest Surgery, What to Expect: http://bit.ly/2LVQr5J
Meet our Heart Center Team: http://bit.ly/2LUvdF9

To learn more about coronary artery bypass grafting (CABG), please visit https://cle.clinic/3b7dqpE
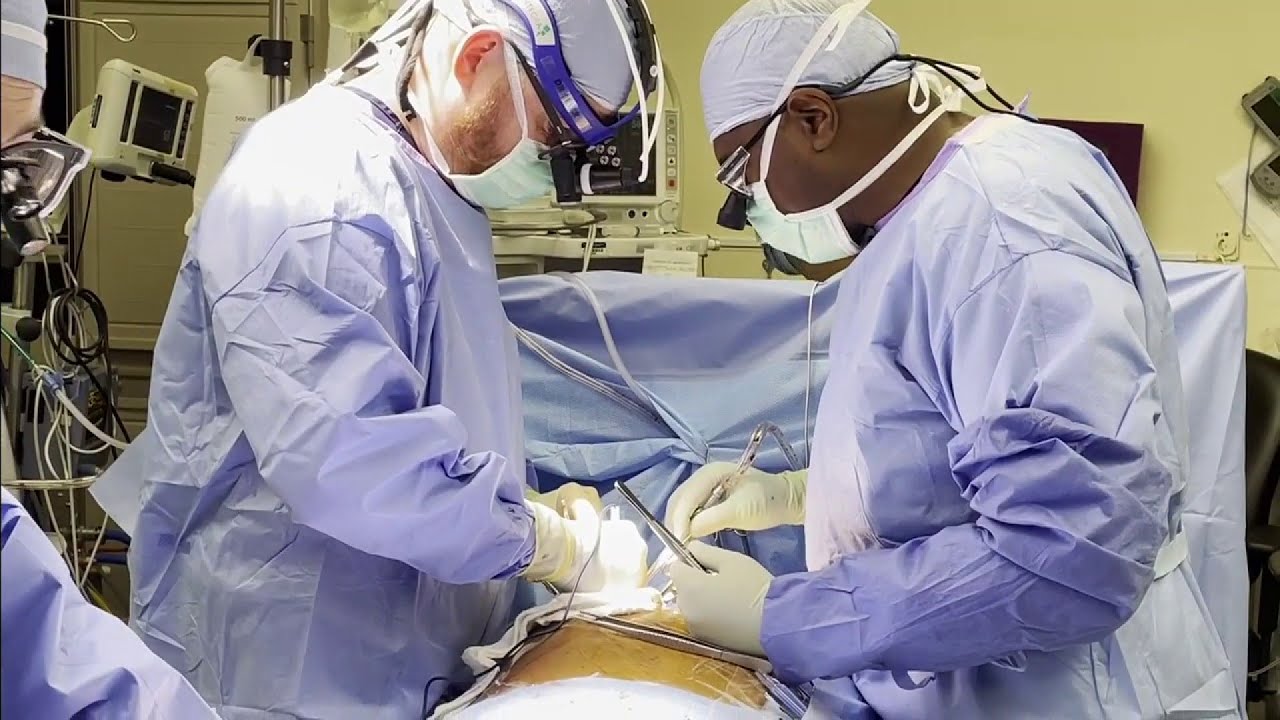
Cardiac surgeons Faisal Baaeen, MD and Edward Soltesz, MD talk about coronary artery bypass graft (CABG) surgery in this informative video.
They describe:
• how blockages are bypassed
• how vessels are used for the bypass graft
• reoperation experiences
• the importance of complete revascularization
• and options such as off pump bypass surgery and minimally invasive surgery
Dr. Bakaeen is the Director of the Coronary Artery Bypass Center at Cleveland Clinic. To learn more about him, please visit https://cle.clinic/2INN9AV
Dr. Soltesz is a cardiovascular and heart transplant surgeon. To learn more about him, please visit https://cle.clinic/3o86RMt
▶Share this video with others: https://youtu.be/Cp59BCMVHHc
▶Subscribe to learn more about @clevelandclinic
#clevelandclinic #coronaryartery #bypasssurgery #heartsurgery #heartcare #cardiacsurgery
Epidural hematoma (EDH) is a traumatic accumulation of blood between the inner table of the skull and the stripped-off dural membrane. EDH results from traumatic head injury, usually with an associated skull fracture and arterial laceration.The inciting event often is a focused blow to the head, such as that produced by a hammer or baseball bat. In 85-95% of patients, this type of trauma results in an overlying fracture of the skull. Blood vessels in close proximity to the fracture are the sources of the hemorrhage in the formation of an epidural hematoma. Because the underlying brain has usually been minimally injured, prognosis is excellent if treated aggressively. Outcome from surgical decompression and repair is related directly to patient's preoperative neurologic condition. [1]
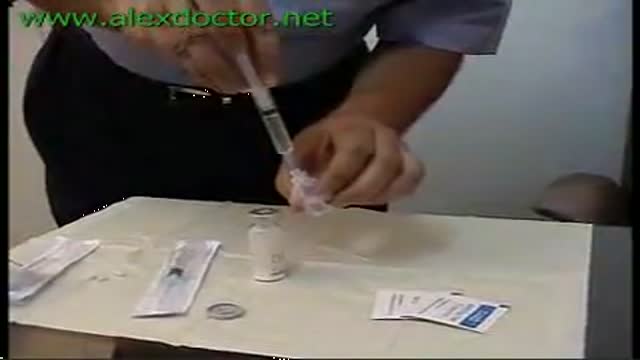
This is a breast life surgery. Over the years, factors such as pregnancy, nursing and the force of gravity take their toll on a woman's breasts. As the skin loses its elasticity, the breasts often lose their shape and firmness and begin to sag. Breast lift is a surgical procedure to raise and reshape the breasts (at least for a time). If your breasts are small or have lost volume (for example from pregnancy) breast implants inserted in conjunction with mastopexy can increase both their firmness and their size.

Ellis demonstrates how to perform a central venous catheter (CVC) dressing change. Please note, you would want to perform hand hygiene after removing the clean gloves before donning the sterile gloves.
Our Critical Nursing Skills video tutorial series is taught by Ellis Parker MSN, RN-BC, CNE, CHS and intended to help RN and PN nursing students study for your nursing school exams, including the ATI, HESI and NCLEX.
#NCLEX #CVC #ClinicalSkills #HESI #Kaplan #ATI #NursingSchool #NursingStudent #Nurse #RN #PN #Education #LVN #LPN #nurseeducator
00:00 CVC Dressing Change
00:26 Preparing patient for CVC Change
00:54 Removing previous dressing
1:56 Removing gloves CVC Change
2:06 Opening CVC Change Kit
2:05 Sterile gloving CVC Change
3:22 Exploring CVC Change kit
3:36 Snap the scrubber CVC Change
3:49 Scrub site CVC Change
4:18 Applying antimicrobial patch CVC Change
4:41 Applying transparent dressing CVC Change
:rocket: Introducing FLASHABLES: Our signature flashcard content in an on-the-go DIGITAL format with guided, personalized learning & progress tracking. :books::syringe:
:mega: Limited-Time Offer Alert: :mega:
:fire: Bundle Up & SAVE! :fire: Purchase any of our amazing flashcard sets, SAVE BIG on FLASHABLES :heavy_dollar_sign::sparkles:& Level Up your study game!
:star2: There’s more…EITHER get 1 MONTH of Membership :free: with any flashcard purchase OR get a WHOLE YEAR of Membership :free: when you grab the Comprehensive Collection or the Ultimate Nursing School Survival Kit! :tada::gift:
Conquer nursing school like a pro with FLASHABLES! :thermometer::pill:
Don’t miss out on this incredible offer - click the link below and start making your nursing school journey your own! :star2::books::mortar_board: https://bit.ly/Flashables
🚪 Access our Cram Courses, Quizzes and Videos all in one ad free space with Level Up RN Membership https://bit.ly/LevelUpRNMembership
Want more ways to MASTER Clinical Skills? Check out our flashcards & videos!
👇👇👇👇👇👇👇👇👇👇
👉 https://bit.ly/clinicalnursingskills 👈
☝️👆☝️👆☝️👆☝️👆☝️👆
This is your one-stop-shop for materials to help you LEARN & REVIEW so you can PASS Nursing School.
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our resources are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of ⭐️⭐️⭐️⭐️⭐️ reviews from nurses who passed their exams and the NCLEX with Level Up RN.
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
L👀king for EVEN MORE resources to survive Nursing School? Make your Nursing School experience your own! Life’s difficult enough—learning shouldn’t be.
🪅 Games https://nursesquad.com
💻 Digital resources https://bit.ly/NursingStudyCourses
📅 Organizational tools https://bit.ly/OrganizingSchool
✨Want perks? Join our channel!
https://youtube.com/leveluprn/join
🏷 Head to https://leveluprn.com/specials for all our latest deals!🥳️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://leveluprn.com/signup ⬅️
⚕ 👩 LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.