Top videos
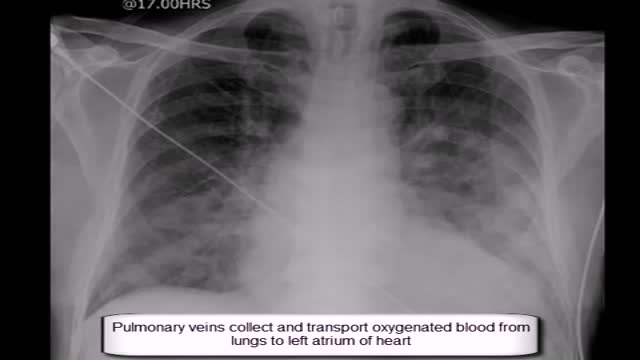
Expand Section. Pulmonary edema is often caused by congestive heart failure. When the heart is not able to pump efficiently, blood can back up into the veins that take blood through the lungs. As the pressure in these blood vessels increases, fluid is pushed into the air spaces (alveoli) in the lungs.
At one time, women who had delivered by cesarean section in the past would usually have another cesarean section for any future pregnancies. The rationale was that if allowed to labor, many of these women with a scar in their uterus would rupture the uterus along the weakness of the old scar. Over time, a number of observations have become apparent: Most women with a previous cesarean section can labor and deliver vaginally without rupturing their uterus. Some women who try this will, in fact, rupture their uterus. When the uterus ruptures, the rupture may have consequences ranging from near trivial to disastrous. It can be very difficult to diagnose a uterine rupture prior to observing fetal effects (eg, bradycardia). Once fetal effects are demonstrated, even a very fast reaction and nearly immediate delivery may not lead to a good outcome. The more cesarean sections the patient has, the greater the risk of subsequent rupture during labor. The greatest risk occurs following a “classical” cesarean section (in which the uterine incision extends up into the fundus.) The least risk of rupture is among women who had a low cervical transverse incision. Low vertical incisions probably increase the risk of rupture some, but usually not as much as a classical incision. Many studies have found the use of oxytocin to be associated with an increased risk of rupture, either because of the oxytocin itself, or perhaps because of the clinical circumstances under which it would be contemplated. Pain medication, including epidural anesthetic, has not resulted greater adverse outcome because of the theoretical risk of decreasing the attendant’s ability to detect rupture early. The greatest risk of rupture occurs during labor, but some of the ruptures occur prior to the onset of labor. This is particularly true of the classical incisions. Overall successful vaginal delivery rates following previous cesarean section are in the neighborhood of 70 This means that about 30of women undergoing a vaginal trial of labor will end up requiring a cesarean section. Those who undergo cesarean section (failed VBAC) after a lengthy labor will frequently have a longer recovery and greater risk of infection than had they undergone a scheduled cesarean section without labor. Women whose first cesarean was for failure to progress in labor are only somewhat less likely to be succesful in their quest for a VBAC than those with presumably non-recurring reasons for cesarean section. For these reasons, women with a prior cesarean section are counseled about their options for delivery with a subsequent pregnancy: Repeat Cesarean Section, or Vaginal Trial of Labor. They are usually advised of the approximate 70successful VBAC rate (modified for individual risk factors). They are counseled about the risk of uterine rupture (approximately 1in most series), and that while the majority of those ruptures do not lead to bad outcome, some of them do, including fetal brain damage and death, and maternal loss of future childbearing. They are advised of the usual surgical risks of infection, bleeding, anesthesia complications and surgical injury to adjacent structures. After counseling, many obstetricians leave the decision for a repeat cesarean or VBAC to the patient. Both approaches have risks and benefits, but they are different risks and different benefits. Fortunately, most repeat cesarean sections and most vaginal trials of labor go well, without any serious complications. For those choosing a trial of labor, close monitoring of mother and baby, with early detection of labor abnormalities and preparation for

The infection is generally transmitted by direct contact with the mucus or sores of someone else with strep. Common symptoms include sore throat, fever, and swollen lymph nodes in the neck. Rarely, complications can involve the heart or kidneys. Treatment is important to reduce complications. Oral antibiotics like penicillin, amoxicillin, cephalexin, or azithromycin are commonly used. Other medicines such as acetaminophen or ibuprofen can help with pain and fever.
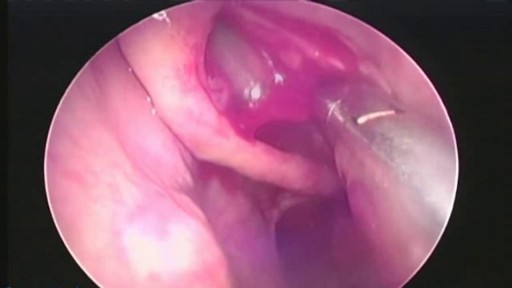
Nasal polyps are linked to allergic rhinitis, asthma, aspirin allergy, sinus infections, acute and chronic infections, something stuck in the nose, and cystic fibrosis. But many times the cause is unknown. Sometimes, people get them before they develop asthma or sinusitis
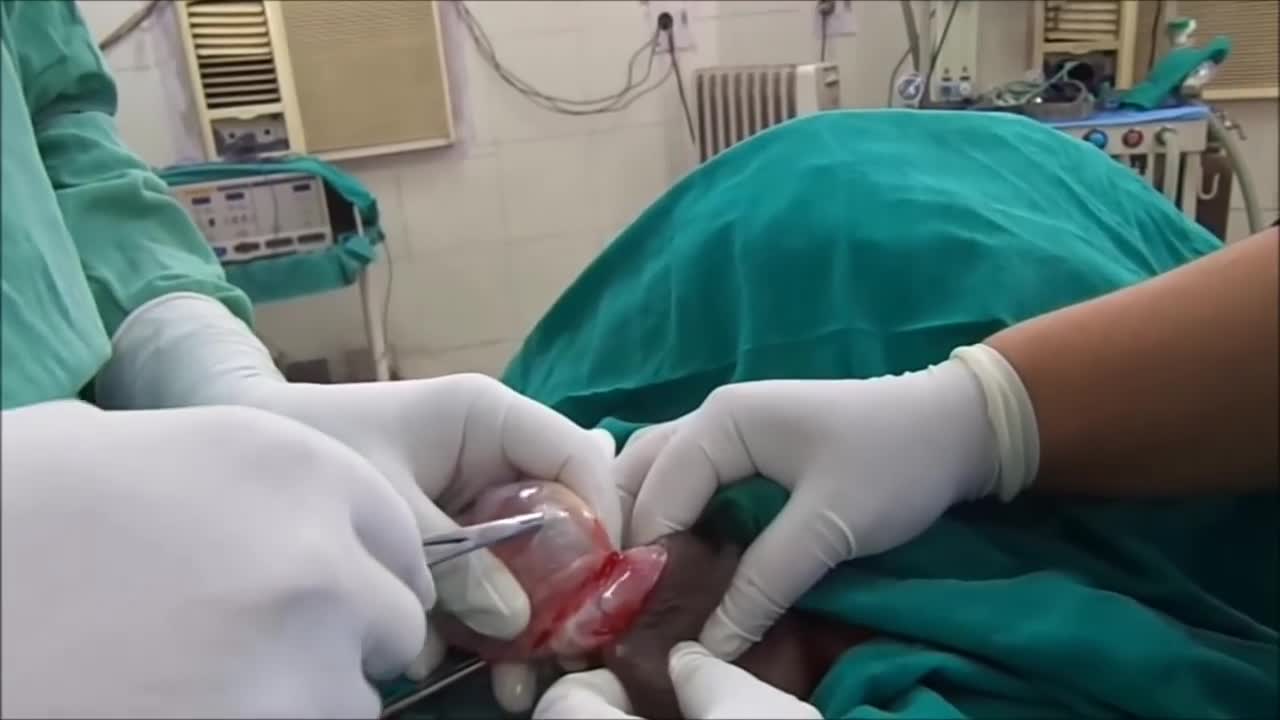
A spermatocele (SPUR-muh-toe-seel) is an abnormal sac (cyst) that develops in the epididymis — the small, coiled tube located on the upper testicle that collects and transports sperm. Noncancerous and generally painless, a spermatocele usually is filled with milky or clear fluid that might contain sperm. The exact cause of spermatoceles is unknown but might be due to a blockage in one of the tubes that transports sperm. Spermatoceles, sometimes called spermatic cysts, are common. They typically don't reduce fertility or require treatment. If a spermatocele grows large enough to cause discomfort, your doctor might suggest surgery.

Adult Still's disease is a rare type of inflammatory arthritis that features fevers, rash and joint pain. Some people have just one episode of adult Still's disease. In other people, the condition persists or recurs. This inflammation can destroy affected joints, particularly the wrists. Treatment involves medications, such as prednisone, that help control inflammation
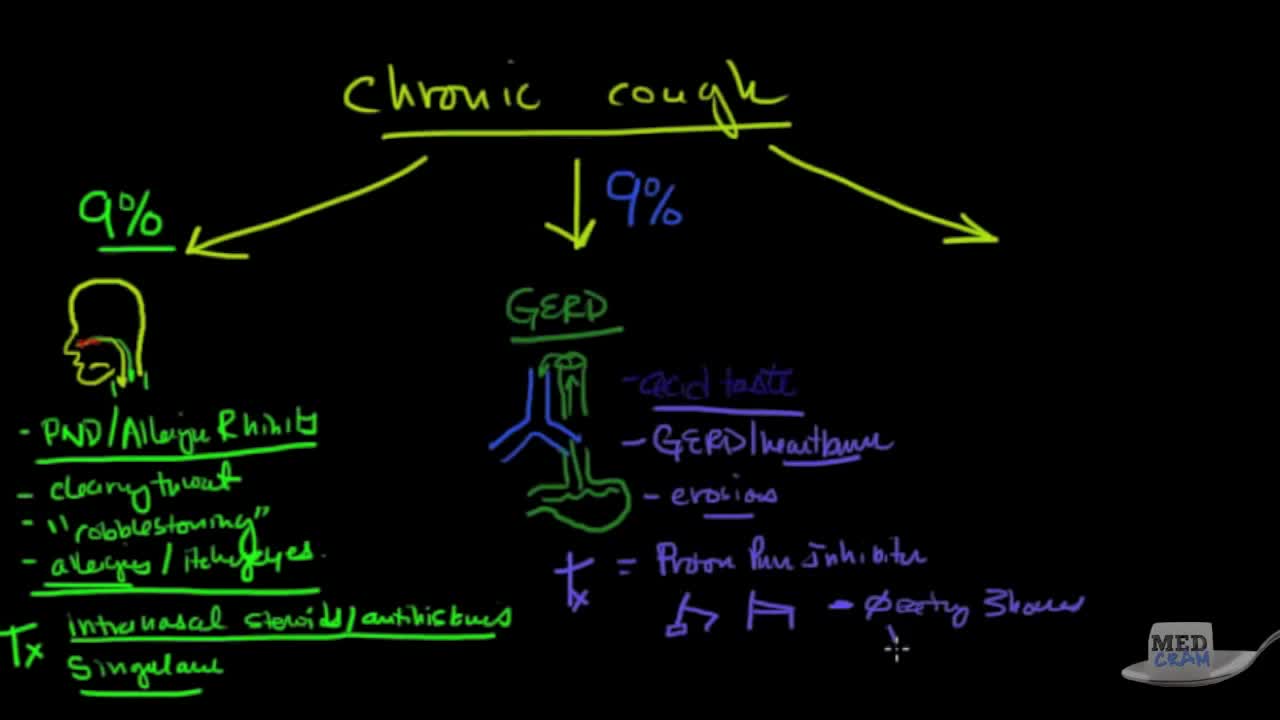
A chronic cough is a cough that lasts eight weeks or longer in adults, or four weeks in children. A chronic cough is more than just an annoyance. A chronic cough can interrupt your sleep and leave you feeling exhausted. Severe cases of chronic cough can cause vomiting, lightheadedness and even rib fractures. While it can sometimes be difficult to pinpoint the problem that's triggering a chronic cough, the most common causes are tobacco use, postnasal drip, asthma and acid reflux. Fortunately, chronic cough typically disappears once the underlying problem is treated.

A torn meniscus is one of the most common knee injuries. Any activity that causes you to forcefully twist or rotate your knee, especially when putting the pressure of your full weight on it, can lead to a torn meniscus. Each of your knees has two menisci — C-shaped pieces of cartilage that act like a cushion between your shinbone and your thighbone. A torn meniscus causes pain, swelling and stiffness. You also might have trouble extending your knee fully. Conservative treatment — such as rest, ice and medication — is sometimes enough to relieve the pain of a torn meniscus and give the injury time to heal on its own. In other cases, however, a torn meniscus requires surgical repair.
Although most women have had enough experience to know how to pleasure a man in the bedroom, but you can be sure that are several girls who would be virgins when you first take them to bed. Though most Indian men actually prefer to make love with a virgin. There are also numerous men who dislike the idea due to the pressure of making love to someone with no experience. So if you happen to be dating a virgin then there are a few important things that you should always keep in mind when you take her to bed. Though you have made love to different women before, you need to understand that this one being a virgin will know little or nothing about what is expected of her in bed. Because she will be anxious and nervous, you have to be all the more careful to ensure that she gets to enjoy her first time with you. Kiss her Whether you are doing it with a virgin or someone with a record that would put Pam Anderson to shame, you should take your time to make love to her just with your lips. Use your lips with passion, and kiss her parts that other guys tend to ignore. Kiss her lips, her hips, her shoulders, her hands, nuzzle her ears - parts which aren’t necessary sexual. Give your girl a hand Okay this one may look straight out of a B-grade south Indian movie, but starting off with a sensual full body massage is an excellent way of warming her up. So use some nice aromatic oils like lavender or Yang-Yang to massage her body. If you are more experienced, you would be aware the various erogenous zones of a woman’s body. Start with the nape of her neck and slowly work your way down to her back, gently knead her breasts and play with her nipples, gently flick at them and manipulate them to erection. Get her to lie on her stomach and massage her inner thighs. Lovingly caress her buttocks and move your hands close to her valley of pleasure. She might be too shy to tell you, but her ultimate pleasure point would be dying for your attention. Gently, stroke her outer lips or the labia. Whatever, apprehensions or fears she may have had about sex will all disappear once your finger start creating magic in her nether regions. Never criticise her Remember, she has never felt a man’s body before, which essentially means that when she tries to explore your body you may not necessarily enjoy it. So let her hold your penis and fondle it, let her lick and nibble you and tickle you body. You may not find her amateurish attentions very arousing but don’t make her feel like an amateur in bed. If she does something right let her know how much you are enjoying it. Guide her fingers to your pleasure points and tell her what you would like a girl to do in bed. Being the more experienced partner you should be like her loving mentor, and teach her the intricacies of pleasuring a man. Make her touch herself While she may or may not have masturbated before, by getting her to touch herself you would be able to make her feel the unknown. Tell her how badly you want to see her masturbate. The idea is open her to own sexuality. Its time to penetrate When you think that she is finally ready to be penetrated, enter her as gently as possible. Also make sure that she is producing enough lubrication to facilitate the act. Keep your strokes slow and shallow and avoid pushing too deep during your first few strokes. If you are able to make her feel comfortable and safe, any pain that she may experience in the beginning will soon disappear, and be replaced by moans of ecstasy. The first time can be nerve racking for most men. Just remember how nervous you were when you had sex for the first time. So when your take your virginal girlfriend to bed for first time makes the experience as pleasurable for her as possible.
Identify the anatomy and explain the physiology of the breast on diagrams and sonograms.
Describe and demonstrate the protocol for sonographic scanning of the breast, including the clock and quadrant methods, and targeted examinations based on mammographic findings.
Describe the various diagnostic pathways that may lead to a sonographic breast examination, and explain how the ultrasound findings are correlated with other imaging modalities.
Identify and describe sonographic images of benign and malignant features and common breast pathologies.
Explain biopsy techniques for breast tumors.
Define and use related medical terminology.
Explain the Patient Privacy Rule (HIPAA) and Patient Safety Act (see reference