Top videos
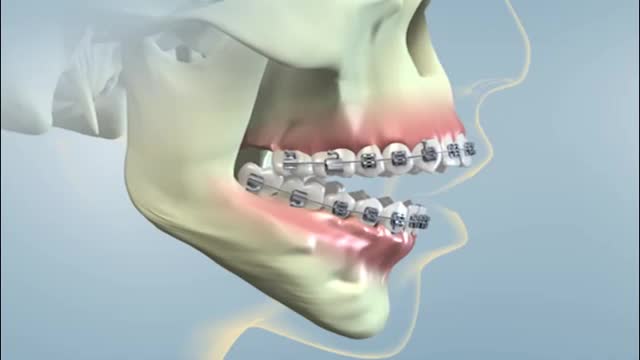
Jaw surgery, also known as orthognathic (or-thog-NATH-ik) surgery, corrects irregularities of the jaw bones and realigns the jaws and teeth to improve the way they work. Making these corrections may also improve your facial appearance. Jaw surgery may be a corrective option if you have jaw problems that can't be resolved with orthodontics alone. In most cases, you also have braces on your teeth before surgery and during recovery after surgery until healing and alignment are complete. Your orthodontist can work with your oral and jaw and face (maxillofacial) surgeon to determine your treatment plan.
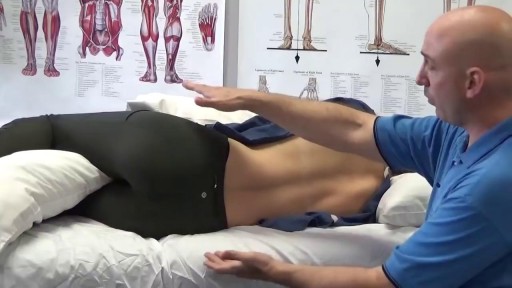
Your sleeping pose can have a major impact on your slumber—as well as your overall health. Poor p.m. posture could potentially cause back and neck pain, fatigue, sleep apnea, muscle cramping, impaired circulation, headaches, heartburn, tummy troubles, and even premature wrinkles
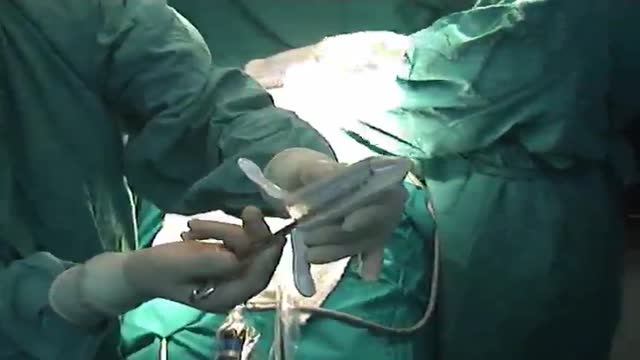
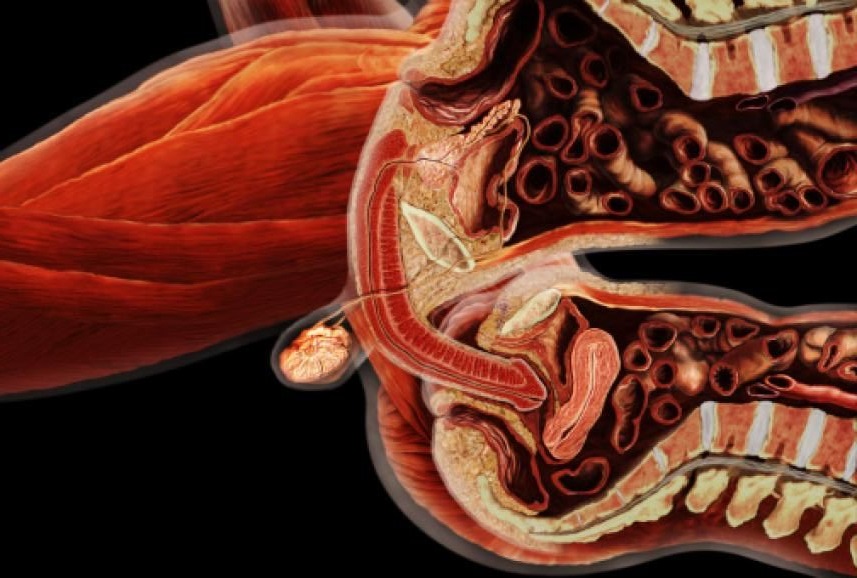
Internal hemorrhoids and loose rectal mucosa may block the exposure during the purse string suturing in stapled hemorrhooidopexy, and this may cause some complications. To retract the prolapsing rectal mucosa we modified the purse string anoscope of the PPH01 kit (Ethicon-Endosurgery, Cincinnati, O...H, USA) and produced a special anoscope. The open part of the purse string suture anoscope is covered by transparent acrylic (Orthoacryl�, Dentaurum, Pforzheim, Germany). The covering material had complete cylindrical outer and inner surfaces and was thin enough to let the anoscope easily rotate in the anal dilator and to let the 26 mm curved, round bodied needle of the 2/0 polypropilene suture move in the anoscope. A window, 3 cm long and 3-4 mm wide, was opened at the angled part of the anoscope 2 cm to the tip of the anoscope. This special anoscope was used for the purse string suture during stapled hemorrhoidopexy procedure in five patients. No postoperative complications, early or late, were encountered, and we propose that stapled hemorrhoidopexy procedure can be applied more easily by using this special anoscope.
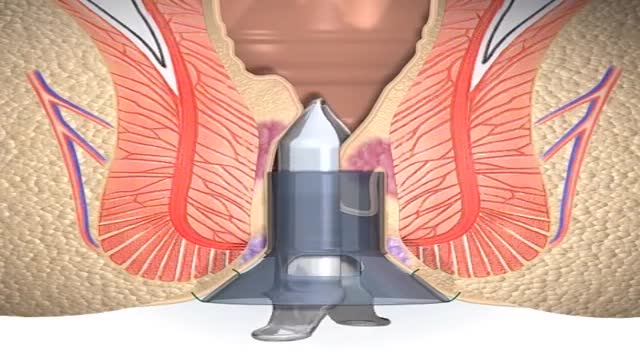
A stapled haemorrhoidopexy is an operation to return the haemorrhoids to a normal. position inside the rectum (back passage). A circular shaped stapling device is gently. inserted in the back passage. The surgeon is then able to use the device to remove.

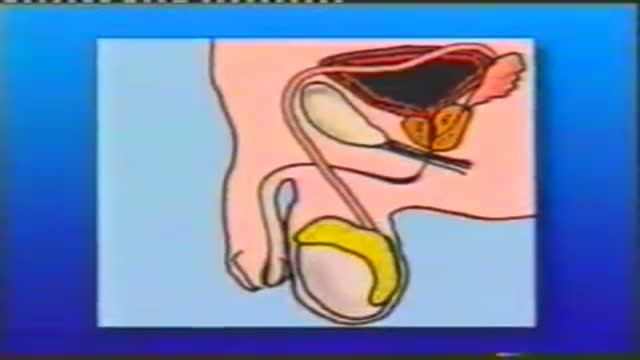
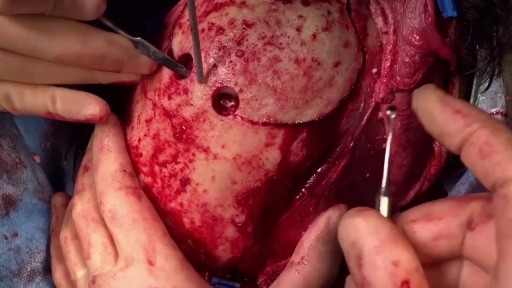
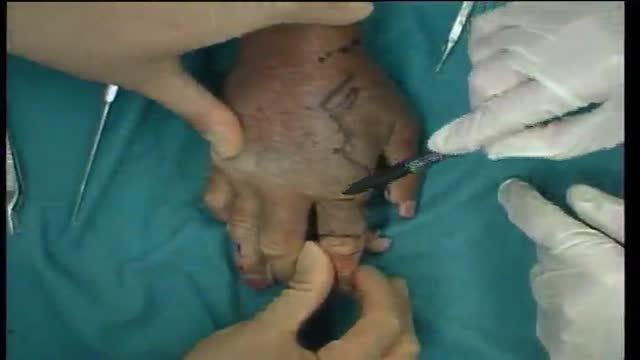
Urogenital neoplasms spreading to the inguinal lymph nodes are penile carcinoma (the most frequent), urethral and scrotum cancers, tumors of the testis with scrotal violation. Penile carcinoma is an uncommon malignant disease and accounts for as many 0.4-0.6% of male cancers. Most patients are elder...ly. It rarely occurs in men under age 60 and its incidence increases progressively until it reaches a peak in the eighth decade 1. The risk of a lymph node invasion is greater with high grade and high stage tumors 2. Some investigators have reported the inaccuracy of the sentinel node biopsy 3, 4, described by Cabanas 5. Patients with metastatic lymph node penis cancer have a very poor prognosis if penectomy only is performed. Ilioinguinal lymphadenectomy is basically carried out as a treatment modality and not only as a staging act. Patients with lymph node invasion have a 30-40% cure rate. Ilioinguinal lymphadenectomy should be also performed in patients with disseminated neoplasms for the local control of the disease. The 5 years survival rate of patients with clinically negative lymph nodes treated with a modified inguinal lymphadenectomy is 88% versus 38% in patients not initially treated with lymphadenectomy 6. This video-tape clearly shows a therapeutic algorithm, the anatomy of the inguinal lymph nodes, according to Rouviere 7 and Daseler 8, the radical ilioinguinal node dissection with transposition of the sartorius muscle and the modified inguinal lymphadenectomy proposed by Catalona 9. References: 1. Lynch D.F. and Schellhammer P: Tumors of the penis. In Campbell’s Urology Seventh Edition, edited by Walsh P.C., Retik A.B., Darracott Vaughan E. and Wein A.J. W.B. Saunders Company, Vol. 3, chapt. 79, p. 2458, 1998. 2. Pizzocaro G., Piva L., Bandieramonte G., Tana S. Up-to-date management of carcinoma of the penis. Eur. Urol. 32: 5-15, 1997 3. Perinetti E., Crane D.B. and Catalona W.J. Unreliability of sentinel lymph node biopsy for staging penile carcinoma. J. Urol. 124: 734, 1980 4. Fowler J.E. Jr. Sentinel lymph node biopsy for staging penile cancer. Urology 23: 352, 1984 5. Cabanas R.M. An approach for the treatment of penile carcinoma. Cancer 39: 456, 1977 6. Russo P. and Gaudin P. Management strategies for carcinoma of the penis. Contemporary Urology;5:48-66, 2000 7. Rouviere H. Anatomy of the human lymphatic system. Edwards Brothers, p. 218, 1938 8. Daseler E.H., Anson B.J., Reimann A.F. Radical excision of the inguinal and iliac lymph glands: a study based on 450 anatomical dissections and upon supportive clinical observations. Surg. Gynecol. Obstet. 87: 679, 1948 9. Catalona W.J. Modified inguinal lymphadenectomy for carcinoma of the penis with preservation of saphenous veins: technique and preliminary results. J. Urol. 140: 306-310, 1988

This shows a full Abdominoplasty surgery performed by Dr. Art Foley in Olympia Washington. Abdominoplasty is also commonly referred to as a "Tummy Tuck." Tummy tuck is a surgical procedure also known as abdominoplasty to remove excess skin and fat from the middle and lower abdomen and to tighten the muscles of the abdominal wall. The procedure can dramatically reduce the appearance of a protruding abdomen. But bear in mind, it does produce a permanent scar.