Top videos

MRCPCH Clinical Revision - more videos at http://mrcpch.paediatrics.co.uk
Revise for your MRCPCH Clinical exam, with videos and high quality content created by the London Paediatrics Trainees Committee.
Examiner: Jonathan Round
Candidate: Amitav Parida
Filming: Mary Chesshyre, Huey Miin Lee, Chris Kelly
Thank you to the Evelina Children's Hospital for allowing us to film during their MRCPCH Revision Course (https://www.guysandstthomaseve....nts.co.uk/mrcpch-cli
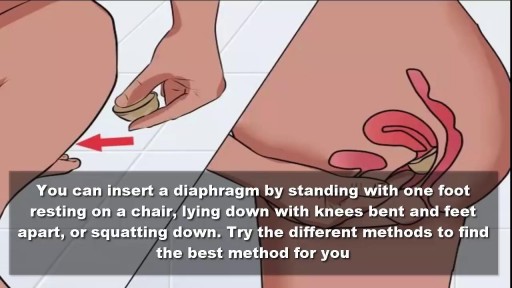
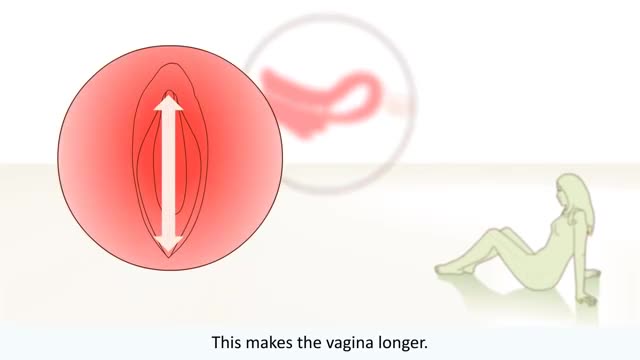
To use the diaphragm, first cover the inside of it with spermicide. Then insert it into your vagina so that it covers your cervix. You can insert the diaphragm up to 6 hours before sex. You should leave it in for at least 6 hours after the last time you have sex.
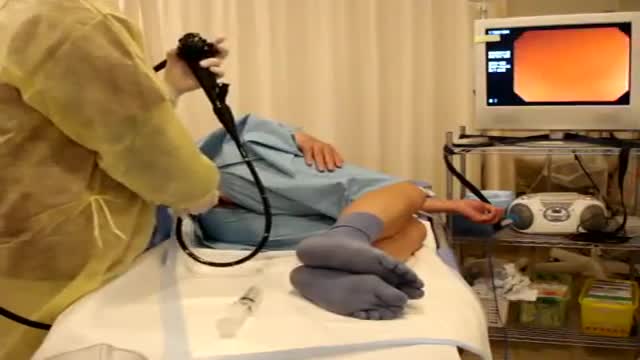
Colonoscopy is a test that allows your doctor to look at the inner lining of your large intestine (rectum and colon). He or she uses a thin, flexible tube called a colonoscope to look at the colon. A colonoscopy helps find ulcers, colon polyps, tumors, and areas of inflammation or bleeding.

Acclaimed sexologist Hanny Lightfoot-Klein, author of several highly illuminating books on genital mutilation, discusses compromises in orgasm after male circumcision. Also commenting is cultural anthropologist James De Meo.From the groundbreaking documentary film, "Whose Body, Whose Rights?"

Thyroid nodules increase with age and are present in almost 10% of the adult population. Autopsy studies reveal the presence of thyroid nodules in 50% of the population, so they are fairly common. 95% of solitary thyroid nodules are benign, and therefore, only 5% of thyroid nodules are malignant.

It is held in place with a balloon at the end, which is filled with sterile water to prevent the catheter from being removed from the bladder. The urine drains through the catheter tube into a bag, which is emptied when full. The procedure to insert a catheter is called catheterization.

The Epley Maneuver for Vertigo can be very effective at relieving vertigo symptoms, but it’s a procedure that should be performed by a physical therapist or other health care professional. This video is for demonstration purposes only. See Doctor Jo’s blog post about the Epley

-A finding of ASC on cytology requires further investigation to exclude precancerous lesions. Recommendations differ for women age 21 -24 and those age ;::25. For women age 21 -24 with ASCUS or low-grade squamous intraepitheliallesion (LSIL), current guidelines recommend repeating Pap smear in one year. In this younger patient population, HPV infection is transient and malignant transformation is rare. Therefore, colposcopy is not performed unless the patient demonstrates ASC-US or LSIL on 3

A Pap smear (Papanicolau smear; also known as the Pap test) is a screening test for cervical cancer. The test itself involves collection of a sample of cells from a woman's cervix (the end of the uterus that extends into the vagina) during a routine pelvic exam