Top videos

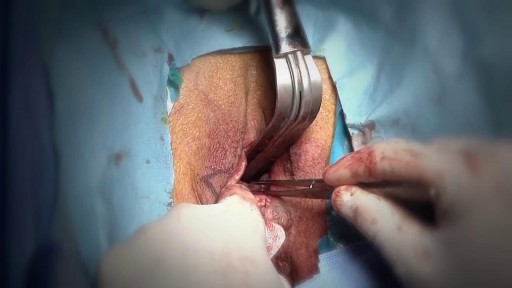
There are several reasons that your doctor may recommend that you have your spleen removed. These include having: a spleen that’s damaged from injury an enlarged spleen or ruptured spleen, which can occur from trauma certain rare blood disorders cancer or large cysts of the spleen infection
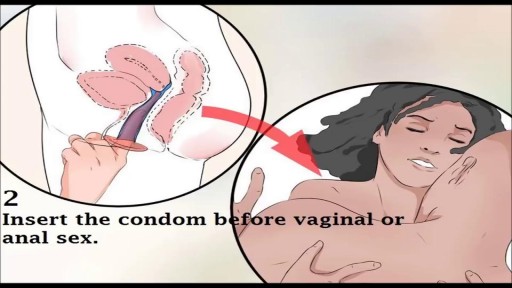
When you’re trying to conceive a baby it is worth giving anything a go which you think will boost your chances. This includes considering that there may be better positions for getting pregnant. But it pays to bear in mind that the human race has been around for over 200,000 years and most of us were probably conceived without our ancestors investing too much thought into the mechanics. Science has proven that successful conception isn’t so much about sexual position as the frequency of sex between a fertile couple. Basically, if you want to fall pregnant, don’t use contraception and have frequent, active and enjoyable sex. Importantly, don’t stress too much about whether you’re doing it the right way. Women can, and do, conceive in any position. Nature has a way of making sure of that.
The average time from symptom onset to diagnosis has been reported to be approximately 2 years. Despite recent attempts at increasing the awareness of pulmonary arterial hypertension (PAH), especially associated PAH (APAH), this delay in diagnosis has not changed appreciably in recent years. Early symptoms are nonspecific. Often, neither the patient nor the physician recognizes the presence of the disease, which leads to delays in diagnosis. Complicating matters, idiopathic PAH (IPAH) requires an extensive workup in an attempt to elucidate an identifiable cause of the elevated pulmonary artery pressure. The most common symptoms and their frequency, reported in a national prospective study, are as follows: Dyspnea (60% of patients) Weakness (19%) Recurrent syncope (13%) Additional symptoms include fatigue, lethargy, anorexia, chest pain, and right upper quadrant pain. Cough, hemoptysis, and hoarseness are less common symptoms. Women are more likely to be symptomatic than men.
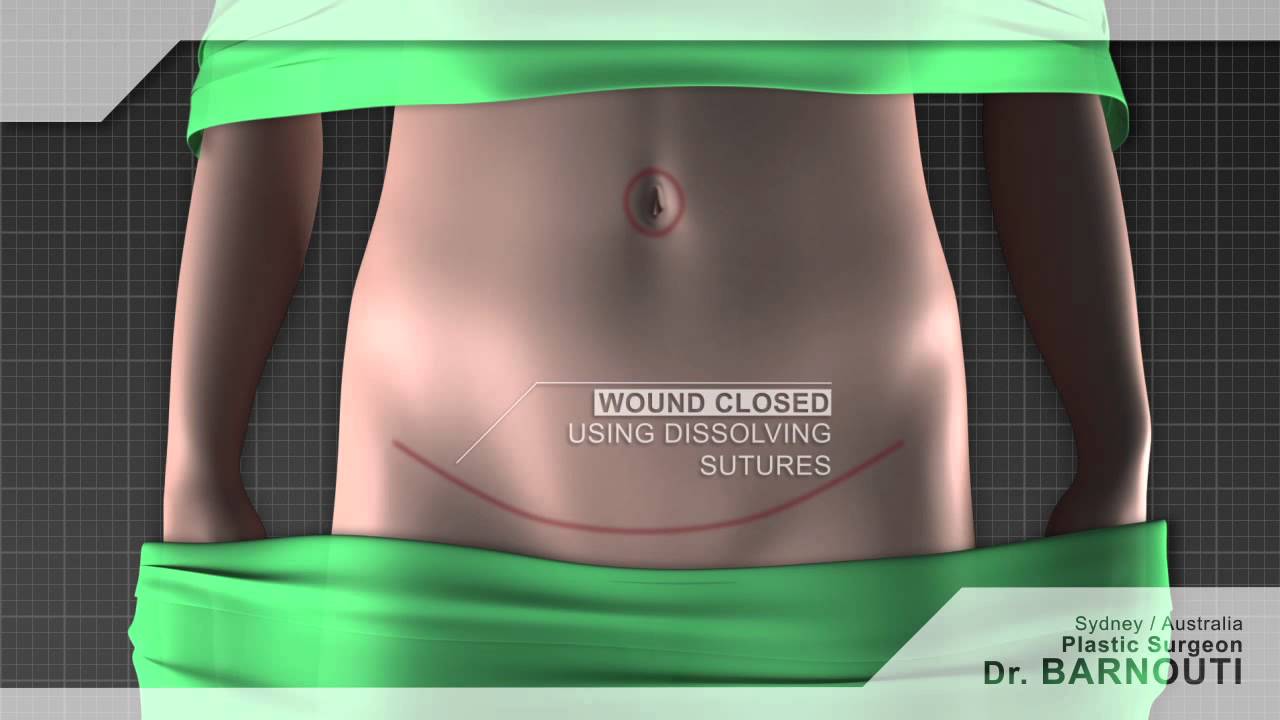
Tummy tuck Sydney Dr Barnouti. Call us on 02-9561 0222 or 1300 002 006
Broadway, Chatswood, Burwood NSW Australia
email:drbarnouti@australiaplasticsurgery.com.au
https://www.plasticsurgery-syd....ney.com.au/abdominop
What is a tummy tuck?
A tummy tuck operation is also known as abdominoplasty. It involves removing excess skin and fat from the stomach area, mainly the lower part of the tummy through surgical procedure. A tummy tuck operation is intended to leave the patient with a flatter tummy and to remove any signs of an 'apron' stomach or an overhang which is sometimes visible above underwear. The skin on this area tends to be stretched and of poor quality. A tummy tuck operation will usually focus on the lower part of the stomach, below the belly button and may require the belly button to be repositioned in some cases. The procedure is often carried out on women or men who have suffered from stretched skin in the stomach area after pregnancy, giving birth, excess fat deposition or weight loss.
What happens during a tummy tuck?
During a tummy tuck procedure the aim of the surgeon is to cut away fat and excess skin. To do this Dr Barnouti will make in incision on the lowest part of the stomach, where a fold will be visible above the pubic bone. He will take out as much excess fat as can be removed and will then cut the skin to fit back over the place where the fat has been removed from. It is important to have realistic expectations of a tummy tuck. Taking too much fat and skin away can result in folds at each end of the resulting scar which are sometimes referred to as "dog ears". Dr Barnouti will make sure you will not have this problem.
Who should have a tummy tuck?
Tummy tucks are recommended for either men or women who have an excess of fat and skin around their abdomen which cannot be removed by weight loss, exercise or liposuction. Tummy tuck operations in women are usually reserved for those who are not likely to have children as it is inadvisable to get pregnant again after having skin removed, this can cause the wound to stretch and scar.
The cost of a tummy tuck in Sydney Australia
The total cost is $7,900 if the patient's health fund cover the hospital's fees. In case the health fund does not cover the hospital's fee, the total cost will be around $12,000 inclusive of the Surgeon, assistant surgeon, Anaesthetist, hospital, operating theatre and follow ups visit.
Payment plans are alos available from Dr Barnouti's office in Chatswood, Burwood or Broadway.
A tummy tuck is a cosmetic procedure that removes excess skin and fatty tissue in order to give a flatter appearance to the stomach. Tummy tucks, also known as abdominoplasties, are ideal for patients who are not excessively overweight but suffer from an overhang of skin around the abdomen.
Performed under general anaesthetic, tummy tucks involve a horizontal incision being made just above the pubic area between the hip bones. Skin and fatty tissue is separated from the muscle and the area is tightened, with the excess skin and fatty tissues then being pulled downwards and removed.
Following your tummy tuck, there will be a scar present across the lower abdomen, but this will gradually fade. You may experience moderate tissue swelling for several months, but this will disappear with time. There may also be a sensation reduction just above the pubic area.
Once your tummy tuck recovery is complete however, you'll benefit from a more attractive figure and the ability to wear a wider selection of clothes.

Train with some of the region’s very best pediatric general surgeons — in a two-year, pediatric surgical fellowship training program at Nemours/Alfred I. duPont Hospital for Children. Our hospital’s Division of Pediatric Surgery is offering this program in affiliation with Sidney Kimmel Medical College at Thomas Jefferson University .
The goal of the fellowship is to give individuals who have completed an accredited general surgery residency advanced knowledge and training in the management and surgical treatment of newborns, infants and children.
Our Fellowship Program
This fellowship will help you prepare for certification by the American Board of Surgery, and is accredited by the Accreditation Council for Graduate Medical Education (ACGME).
The Pediatric Surgery Fellowship aims to:
train a well-rounded, empathetic, safe pediatric surgeon who is confident managing all aspects of the surgical care of children.
steward our fellow in quality improvement projects and methodology, and provide research opportunities.
provide a rigorous didactic curriculum for our fellow utilizing 360 degree feedback.
cultivate opportunities for our fellow to educate residents and students.
encourage our fellow to collaborate across specialties.
develop our fellow’s presentation skills during M&M conferences and multi-disciplinary educational meetings.
The program features the full participation of all nine of the pediatric surgical division’s full-time faculty members. Each of these physicians will contribute greatly to your education. Your training will include operating room and outpatient clinic experience, as well as bedside evaluation of children. You’ll also play a role in the organization of formal teaching conferences, held weekly. Formal rotations will be spent on Pediatric Urology, PICU and Neonatology during the first 12 months. The last year will be spent entirely on the Pediatric Surgical Service.
The majority of your inpatient consultative time will take place at Nemours/Alfred I. duPont Hospital for Children, a freestanding children’s hospital in Wilmington, Del. The hospital:
is nationally ranked by U.S. News & World Report in eight pediatric specialties
recently opened expansion with 260 beds
performs more than 2,800 inpatient and 9,300 outpatient surgical procedures each year in our operating rooms
has an on-site delivery center for newborns with complex congenital anomalies
receives more than 50,000 annual visits in our Emergency Department (ED)
is accredited by The American College of Surgeons as a Level One Pediatric Trauma Center
is accredited by the Commission on Accreditation of Rehabilitation Facilities (CARF)
Visit https://www.nemours.org/educat....ion/gme/fellowships/ to learn more.
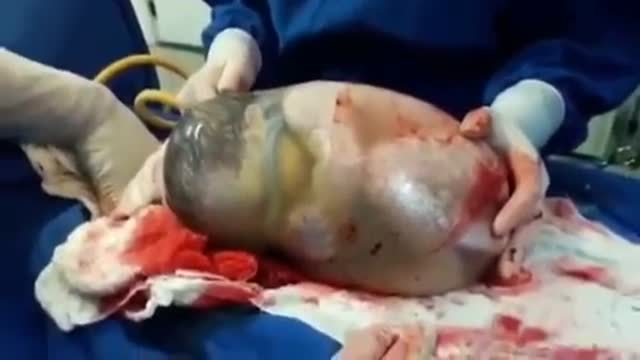
This is the incredible moment a new-born baby arrived still inside its amniotic sac, completely intact. The tiny infant can be seen moving and stretching still inside the sac, as medics prepare to snip the new born free. The amniotic sac is a thin but durable membrane filled with fluid which helps keep a baby warm and safe from bumps during pregnancy. When it breaks, this is typically referred to as a woman's 'waters breaking' shortly before she gives birth. But in rare cases, less than 1-in-80,000 births, the baby is delivered with the membranes still intact and this is known as a 'caul birth'. Some babies are born with part of the membrane still attached to them, but to be born completely encased in the intact membrane is incredibly rare. Many people still believe the phenomenon to be a good omen for the child's infancy and it is has even been suggested, but not proven, that caul babies will always have a natural affinity for water. The video was taken in Spain on Saturday and captures the rare moment the baby was born with the membrane covering its entire body, just minutes after its twin was delivered normally.
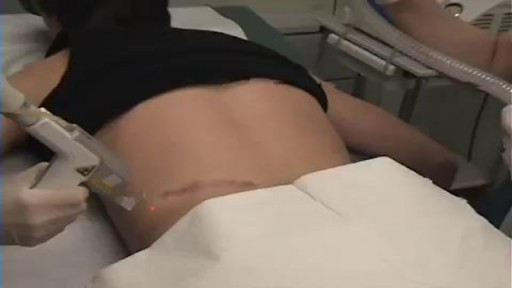
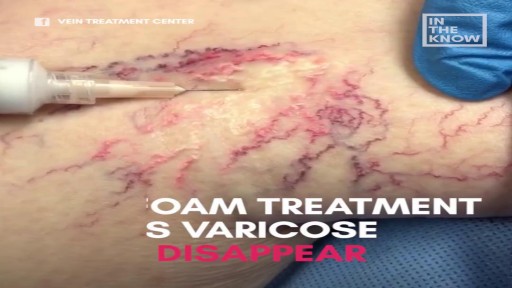
aser treatment for scars reduces the appearance of scars. It uses focused light therapy to either remove the outer layer of the skin’s surface or stimulate the production of new skin cells to cover damaged skin cells. Laser treatment for scars can reduce the appearance of warts, skin wrinkles, age spots, scars, and keloids. It doesn’t completely remove a scar.

In breech position, the baby's bottom is down. There are a few types of breech: Complete breech means the baby is bottom-first, with knees bent. Frank breech means the baby's legs are stretched up, with feet near the head. Footling breech means one leg is lowered over the mother's cervix. You are more likely to have a breech baby if you: Go into early labor Have an abnormally shaped uterus, fibroids, or too much amniotic fluid Have more than one baby in your womb Have placenta previa (when the placenta is on the lower part of the uterine wall, blocking the cervix)
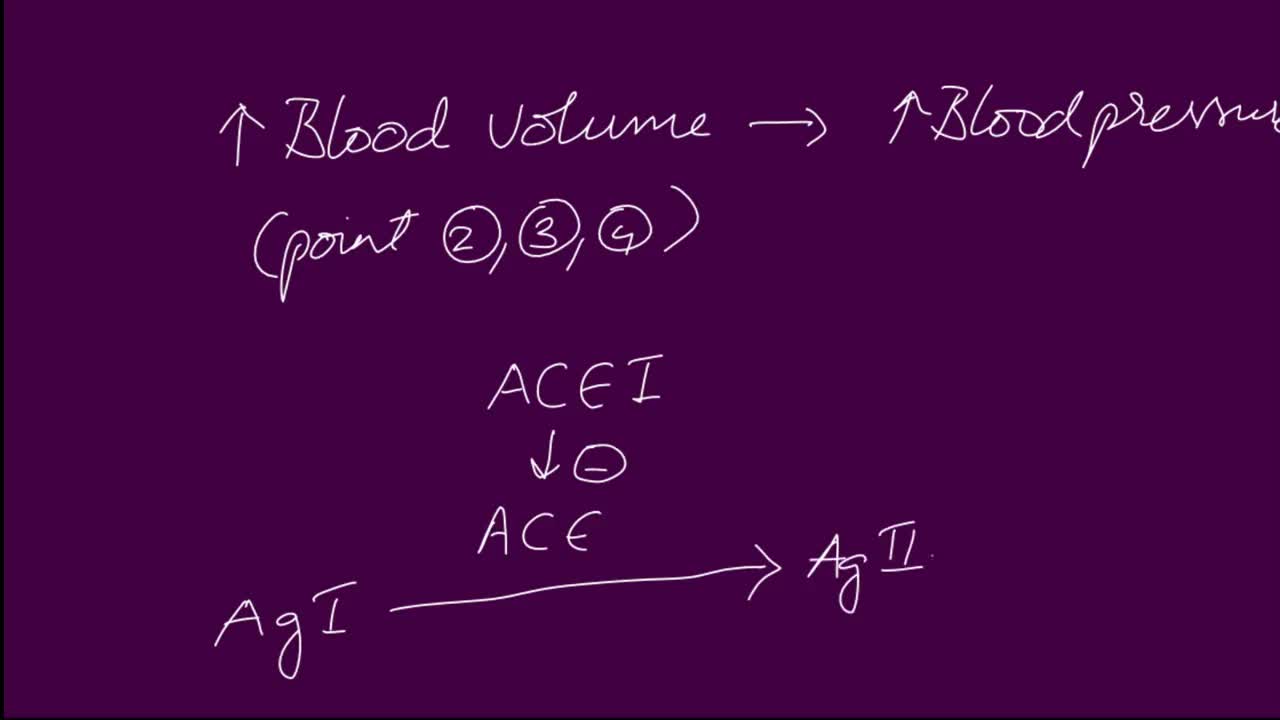
ACE Inhibitor Mechanisms. Angiotensin converting enzyme (ACE) inhibitors are agents used to relax blood vessels and lower blood pressure. They prevent an enzyme from producing angiotensin II, which narrows blood vessels and raises blood pressure, meaning the heart has to work harder to pump blood around the body.