Top videos

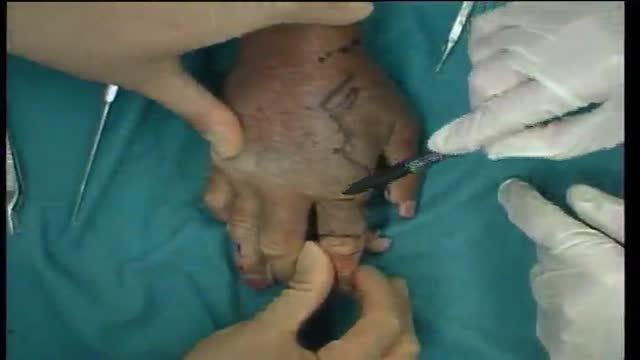
A spermatocelectomy is surgery to remove a spermatocele. A spermatocele is a cyst (sac of fluid) that contains sperm. It forms inside your scrotum on the outside of your testicle. The cyst is most often attached to your epididymis. The epididymis is a tube that stores sperm.

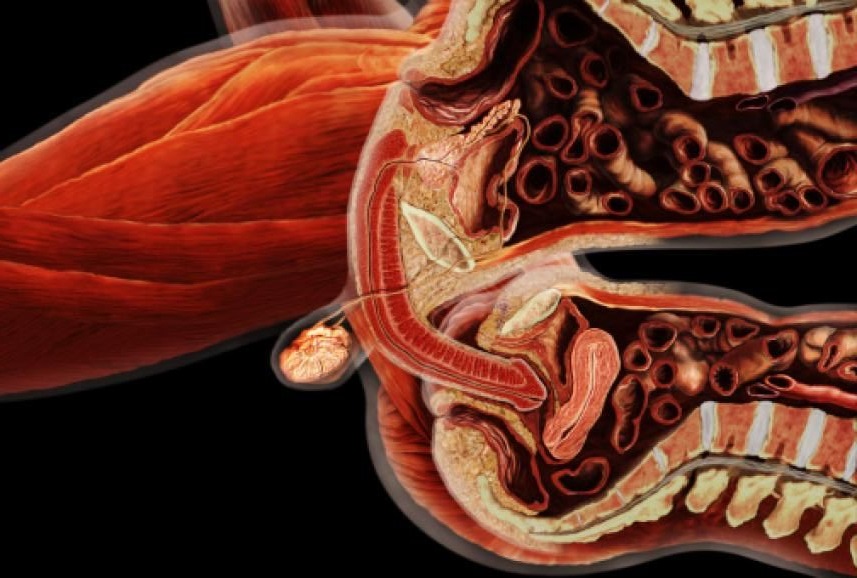
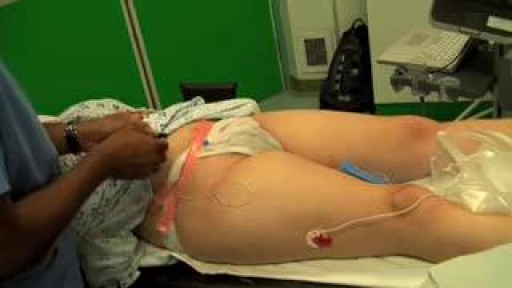
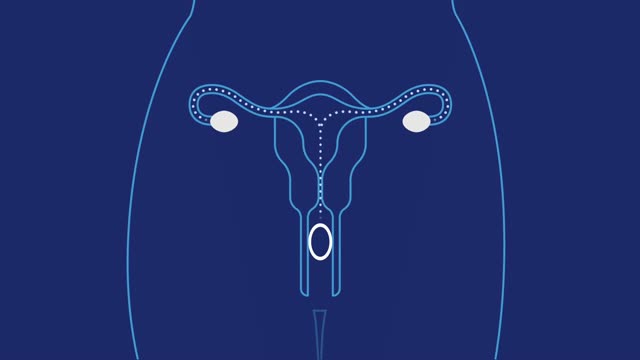
Intrauterine insemination (IUI) is a fertility treatment that involves placing sperm inside a woman's uterus to facilitate fertilization. The goal of IUI is to increase the number of sperm that reach the fallopian tubes and subsequently increase the chance of fertilization

Detailed examination of the joints is usually not included in the routine medical examination. However, joint related complaints are rather common, and understanding anatomy and physiology of both normal function and pathologic conditions is critically important when evaluating the symptomatic patient. By gaining an appreciation for the basic structures and functioning of the joint, you'll be able to "logic" your way thru the exam, even if you can't remember the eponym attached to each specific test!
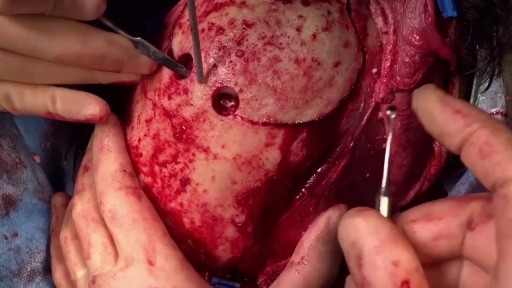
Surgery to replace an aortic valve is done for aortic valve stenosis and aortic valve regurgitation. During this surgery, the damaged valve is removed and replaced with an artificial valve. The valve replacement is typically an open-heart surgery.

Strep throat is a bacterial infection that can make your throat feel sore and scratchy. Strep throat accounts for only a small portion of sore throats. If untreated, strep throat can cause complications, such as kidney inflammation or rheumatic fever. Rheumatic fever can lead to painful and inflamed joints, a specific type of rash or heart valve damage. Strep throat is most common in children, but it affects people of all ages. If you or your child has signs or symptoms of strep throat, see your doctor for prompt testing and treatment.

NTIS refers to a syndrome found in seriously ill or starving patients with low fT3, usually elevated RT3, normal or low TSH, and if prolonged, low fT4. It is found in a high proportion of patients in the ICU setting, and correlates with a poor prognosis if TT4 is <4ug/dl. The patho-physiology includes suppression of TRH release, reducedT3 and T4 turnover, reduction in liver generation of T3, increased formation of RT3, and tissue specific down-regulation of deiodinases, transporters, and TH receptors. Although long debated, tissue TH levels are definitely reduced, and tissue hypothyroidism is presumably present. This is often not clinically evident because of the brief duration, and reduced but not absent tissue levels of TH. Although recognized for nearly 4 decades, interpretation of the syndrome is contested, because of lack of data. Some observes, totally without data, argue that it is a protective response and should not be treated. Other observers (as in this review) present available data suggesting, but not proving, that thyroid hormone replacement is appropriate, not harmful, and may be beneficial. The best form of treatment (TRH,TSH,or T3+T4) and possible accompanying treatments (GHRH, Cortisol, nutrition, insulin) lack consensus. In this review current data are laid out for reader’s review and judgment.

OB_A_1013
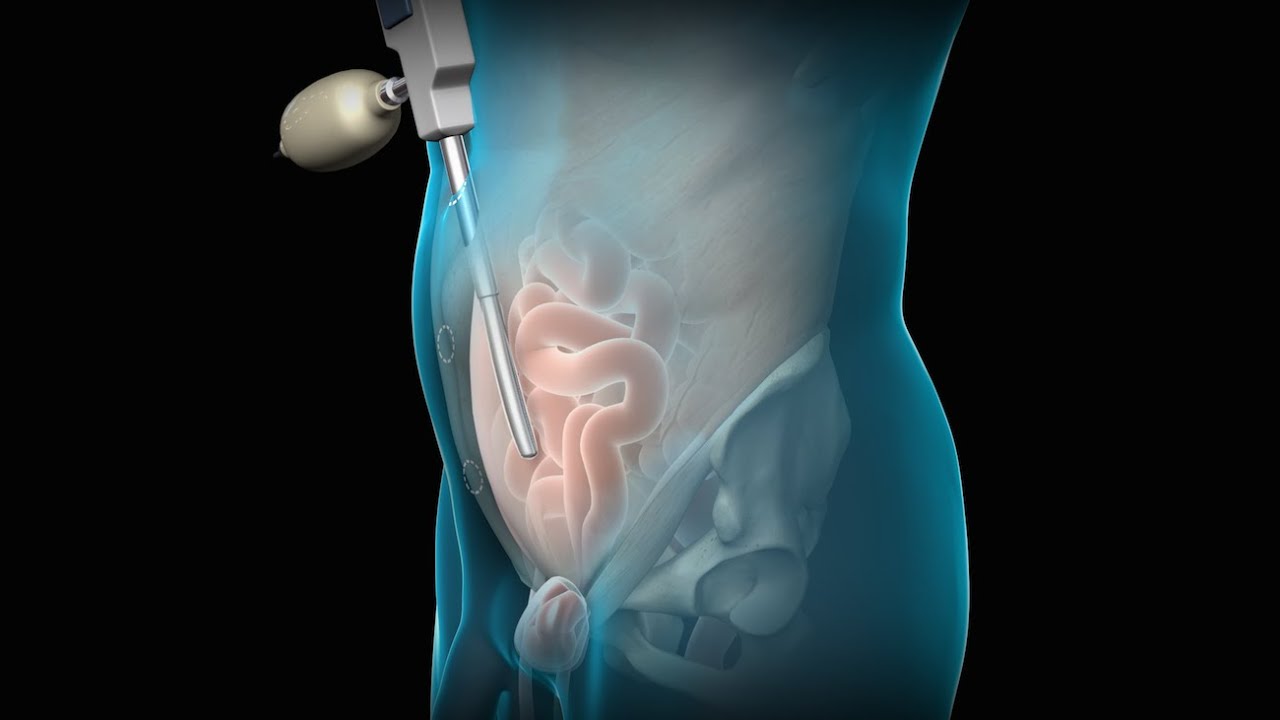
3D animation depicting the operating room and initial procedure preparing the patient for a laparoscopic hysterectomy. The patient is prepped and draped in the usual fashion and surrounded by the surgeon and surgical assistants. The skin is elevated, an infraumbilical incision is made, a trocar port is inserted through the incision and the abdomen is insufflated. Finally, a laparoscope is inserted into the port to allow for direct visualization of the uterus and the surgery can begin.
To view more animations and exhibits, visit our medical library: https://www.trialexhibitsinc.c....om/library/multimedi
Contact us on your next case for consulting, trial graphics, animations, medical illustrations or presentation services. 800-591-1123 [a]www.trialex.com[/a]
This video is for reference only. The video may not be otherwise used, reproduced nor modified. For more information to purchase a copy or permission to use this animation on your next case, project, website or TV, contact us at [a]www.trialex.com[/a] or 800-591-1123.
Copyright @ Trial Exhibits, Inc.
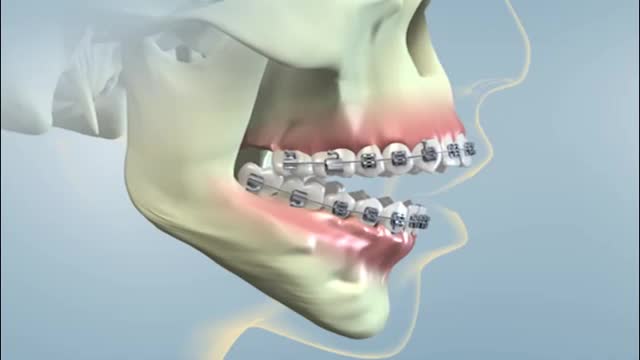
Jaw surgery, also known as orthognathic (or-thog-NATH-ik) surgery, corrects irregularities of the jaw bones and realigns the jaws and teeth to improve the way they work. Making these corrections may also improve your facial appearance. Jaw surgery may be a corrective option if you have jaw problems that can't be resolved with orthodontics alone. In most cases, you also have braces on your teeth before surgery and during recovery after surgery until healing and alignment are complete. Your orthodontist can work with your oral and jaw and face (maxillofacial) surgeon to determine your treatment plan.
To license this video for patient education or content marketing, visit: http://www.nucleushealth.com/?utm_source=youtube&utm_medium=video-description&utm_campaign=tephernia-030615
An inguinal hernia is a bulging of the intestine through a defect or weak spot in the wall of the lower abdomen. This video shows how inguinal hernias form and how they are treated.
#TotalExtraperitonealLaparoscopicInguinalHerniaRepair #TEP #laparoscopy
ANCE00200