Top videos
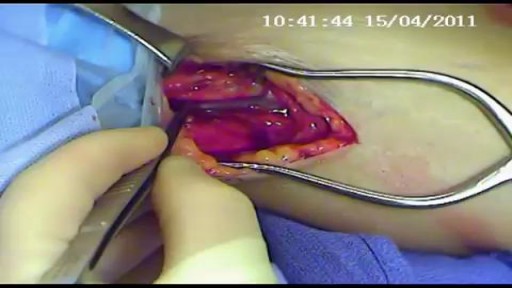
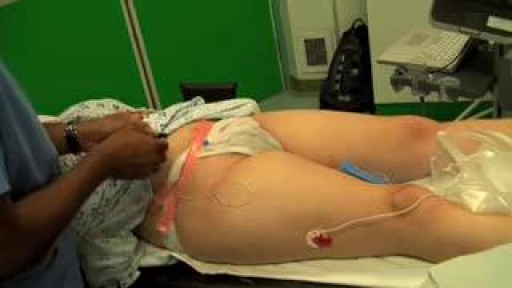
An AV fistula is a connection, made by a vascular surgeon, of an artery to a vein.Vascular surgeons specialize in blood vessel surgery. The surgeon usually places an AV fistula in the forearm or upper arm. An AV fistula causes extra pressure and extra blood to flow into the vein, making it grow large and strong.
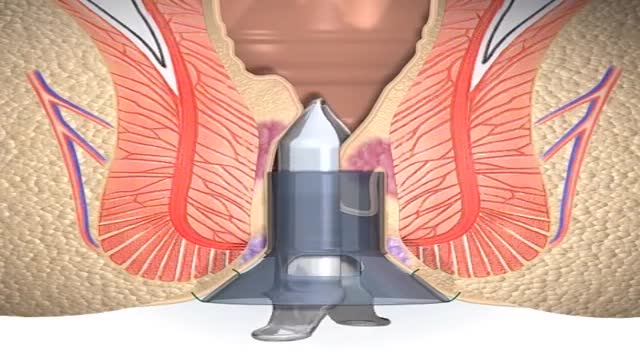
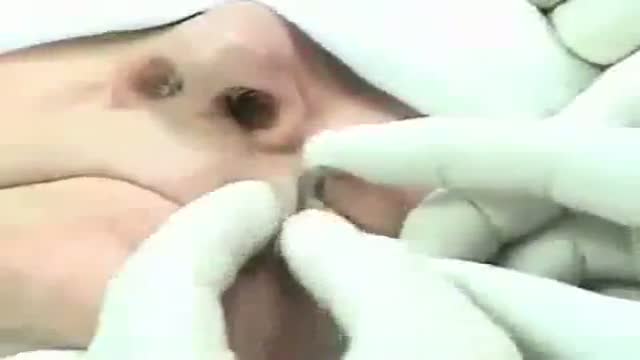
A stapled haemorrhoidopexy is an operation to return the haemorrhoids to a normal. position inside the rectum (back passage). A circular shaped stapling device is gently. inserted in the back passage. The surgeon is then able to use the device to remove.

http://www.utexas.edu
Nursing students practice their skills on mannequins and each other in the Nursing Skills Lab.

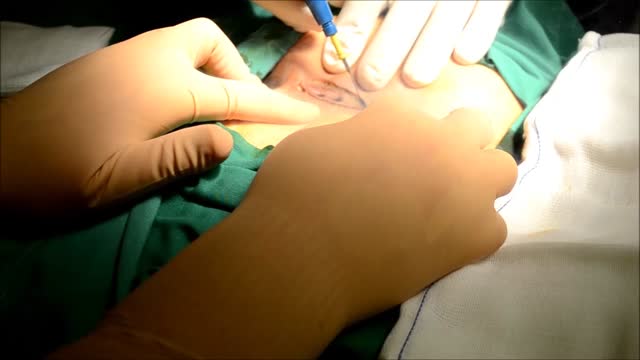
A Lecture Presented by Dr. Mostafa Yakoot to Vascular Surgery Congress. TITLE: SAFETY & EFFICACY OF A NEW HONEY OINTMENT (PEDYPHAR) FOR DIABETIC FOOT ULCERS. Based on the original article in JWC by: Yakoot M, Abdelatif M, Etman M.

the motor milestones expected in typically developing babies, from head control to walking and what pediatricians look for during a well-baby visit. She also explains the specific types of motor control a baby must master before the next milestone can be achieved