Top videos
It used to be when a woman needed a hysterectomy she could expect full abdominal surgery with a long recovery time. Dr. Melissa Lee uses less invasive methods that can cut the patients downtime in half.
"We were trained in more laparoscopic and minimally invasive cases so of course that's what I'm more comfortable with doing right now."
She sees a new generation of patients opting for laparoscopic surgery.
"Laparoscopy is the use of small cameras with small incisions and instruments that are guided by the hand, and you're able to see directly into the abdomen without actually fully opening the abdomen," says Dr. Lee, an obstetrician-gynecologist with Lee Memorial Health System.
Nowadays, even a large mass or uterus can be removed using the slender tools.
"There are multiple different laparoscopic instruments that you can use. Whether they're blunt dissections or just dissectors that hold and retract back or actual scissors or cutting instruments, there are multiple different options," says Dr. Lee.
While a standard abdominal hysterectomy requires a four to eight inch incision, the laparoscope needs only a quarter to half inch. It's enough to make a big difference in terms of recovery.
"They're able to get up and move around faster. They're able to recover faster, their pain level and their need for pain medicine is much lower," says Dr. Lee.
The laparoscopic procedure also cuts down on scarring and more importantly, shortens the hospital stay. The trend now is home within 24 hours.
"Where the patient is done early in the morning, they're doing well they're tolerating oral intake they're able to getup and move around. And those patients a lot of times will feel comfortable to go home that same nigh after a major surgery," says Dr. Lee.
New studies show women who've had a laparoscopic hysterectomy viewed their quality of life as better than those who had an open abdominal procedure, making this a good option for the right patient.
View More Health Matters video segments at leememorial.org/healthmatters/
Lee Memorial Health System in Fort Myers, FL is the largest network of medical care facilities in Southwest Florida and is highly respected for its expertise, innovation and quality of care. For nearly a century, we've been providing our community with everything from primary care treatment to highly specialized care services and robotic assisted surgeries.
Visit leememorial.org
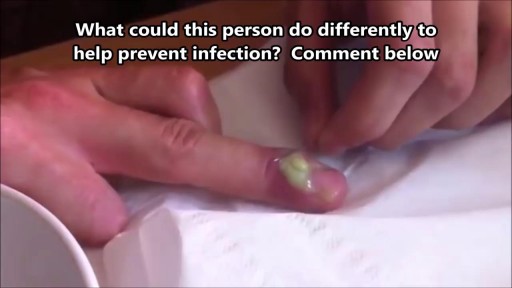
What Is a Paronychia (Nail Infection)? An infection that develops along the edge of the fingernail or toenail is called a paronychia (pear-ah-NIK-ee-ah). It is the most common hand infection and, if left untreated, can progress to a more severe infection of the entire finger or toe. Paronychia is distinguished from other infections such as onychomycosis and herpetic whitlow by its location and appearance.
Sclerotherapy is a medical procedure used to eliminate varicose veins and veins. Sclerotherapy involves an injection of a solution (generally a salt solution) directly into the vein. The solution irritates the lining of the blood vessel, causing it to collapse and stick together and the blood to clot.

In this video, we have explained the procedure of total #knee #replacement #surgery in patient in 3D animation.
Learn more: https://ecgkid.com
_____________________________________________________________________
Knee replacement, commonly known as complete knee replacement or knee arthroplasty, is a surgical treatment that resurfaces a knee that has been destroyed by arthritis. The extremities of the bones that make up the knee joint, as well as the kneecap, are capped with metal and plastic pieces. Someone with severe arthritis or a major knee injury may benefit from this procedure.
The knee joint can be affected by a variety of arthritis forms. The degradation of joint cartilage and neighboring bone in the knees can be caused by osteoarthritis, a degenerative joint disease that primarily affects middle-aged and older persons. Rheumatoid arthritis produces pain and stiffness by inflaming the synovial membrane and resulting in an excess of synovial fluid. Traumatic arthritis, or arthritis caused by an injury, can harm the joints.
The purpose of knee replacement surgery is to resurface damaged areas of the knee joint and cure knee discomfort that has not responded to prior therapies.
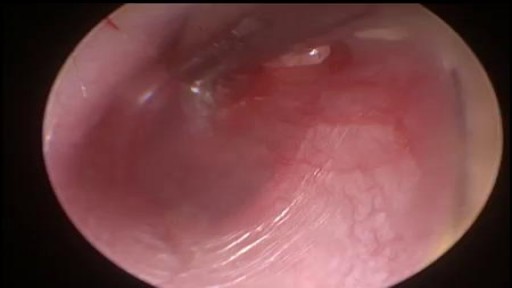
A myringotomy is a procedure in which your doctor creates a small hole in the eardrum so fluids such as water, blood, or pus can drain out. In many cases, your doctor will put in a tube so it won't get backed up again. The tube, which will usually fall out on its own in about six to 18 months, lets air flow through and keeps the middle ear dry. Tubes also: Reduce pain Improve hearing Cut down on the number of infections your child may have
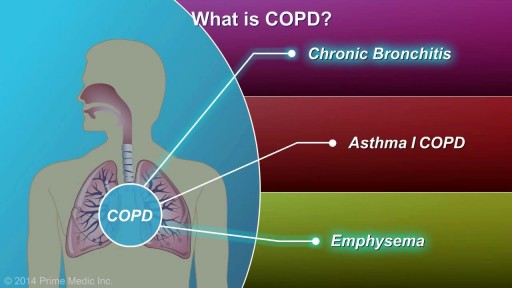
COPD, or chronic obstructive pulmonary disease, is a progressive disease that makes it hard to breathe. Progressive means the disease gets worse over time. COPD can cause coughing that produces large amounts of a slimy substance called mucus, wheezing, shortness of breath, chest tightness, and other symptoms. Cigarette smoking is the leading cause of COPD. Most people who have COPD smoke or used to smoke. However, up to 25 percent of people with COPD never smoked. Long-term exposure to other lung irritants—such as air pollution, chemical fumes, or dusts—also may contribute to COPD. A rare genetic condition called alpha-1 antitrypsin (AAT) deficiency can also cause the disease.

Colorectal surgeon Conor Delaney, MD, explains laparoscopic surgery for colon cancer, including how it works and what patients can typically expect before, during, and after the procedure.
Learn more about colon cancer at http://cancer.org/coloncancer
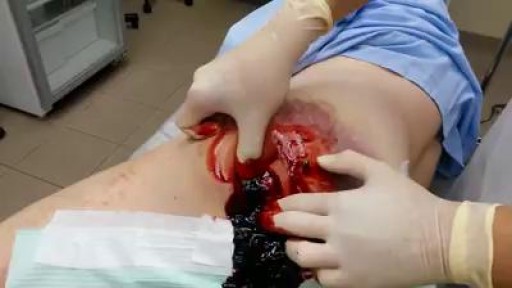
A hematoma is a collection of blood outside of a blood vessel Some causes of hematomas are as pelvic bone fractures, fingernail injuries (subungual), bumps, passing blood clots, blood clot in the leg (DVT), blood cancers, and excessive alcohol use.

► Sign up here and try our FREE content: http://lectur.io/freecontentyt
► If you’re an medical educator or faculty member, visit: http://lectur.io/medytb2u
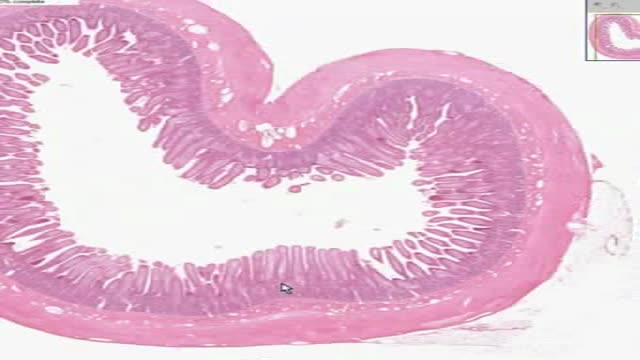
This video “Respiratory Histology” is part of the Lecturio course “Histology” ► WATCH the complete course on http://lectur.io/respiratoryhistology
► LEARN ABOUT:
- The cellular components of epithelium
- Structure and function of the conchae
- The cellular components of olfactory epithelium
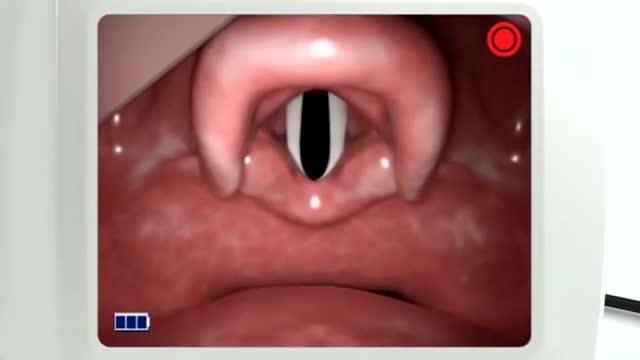
- Components of the true vocal cord
- Function of the epiglottis
- The difference between bronchus, bronchiole, respiratory bronchiole
- Alveolar duct and Alveolar sac
- Components that make up the interalveolar septum
- Type I and Type II of alveolar cells, macrophages and endothelium
- Two separate blood supplies to the lungs and their functions
- Summary of the functions and the system of the respiratory system
► THE PROF: Your lecturer is Professor Geoff Meyer. He is currently teaching at the School of Anatomy, Physiology and Human Biology at the University of Western Australia (UWA). As a leading anatomy and histology expert he is also coordinating the Federative International Program for Anatomical Terminologies (FIPAT) of the International Federation of Associations of Anatomists (IFAA). Besides medical research on the ovarian function, steroidogenesis, corpus luteum, angiogenesis, and microcirculation, Geoff Meyer’s research activities also focus on developing innovative, computer-aided learning and teaching tools. For his inventiveness, Geoff Meyer has received a number of awards, including the Australian University Teaching Award.
► LECTURIO is your single-point resource for medical school:
Study for your classes, USMLE Step 1, USMLE Step 2, MCAT or MBBS with video lectures by world-class professors, recall & USMLE-style questions and textbook articles. Create your free account now: http://lectur.io/respiratoryhistology
► INSTALL our free Lecturio app
iTunes Store: https://app.adjust.com/z21zrf
Play Store: https://app.adjust.com/b01fak
► READ TEXTBOOK ARTICLES related to this video:
Histology of the Airways
http://lectur.io/respiratoryhistoloyarticle
► SUBSCRIBE to our YouTube channel: http://lectur.io/subscribe
► WATCH MORE ON YOUTUBE: http://lectur.io/playlists
► LET’S CONNECT:
• Facebook: https://www.facebook.com/lectu....rio.medical.educatio
• Instagram: https://www.instagram.com/lecturio_medical_videos
• Twitter: https://twitter.com/LecturioMed
• Pinterest: https://www.pinterest.de/lecturiomedical
• LinkedIn: https://www.linkedin.com/company/lecturio-medical/
0:00 Introduction
2:00 Respiratory system Summary of structure and function
3:32 Conducting portion
7:49 The Nasal cavities
11:27 The nasal cavity
13:06 Respiratory mucosa
15:26 Olfactory mucosa
17:13 Olfactory receptor
21:16 The larynx (and the epiglottis)
25:44 The trachea
29:16 The bronchi
31:35 Bronchiole
38:50 Alveolus
40:45 Air blood barrier
43:36 Alveolar macrophages
45:35 Blood supply and lymphatic drainage of the pulmonary lobule