Top videos

Today I'm using the best 3D animation to explain WHAT IS DIASTASIS RECTI and what you need to know about diastasis recti after pregnancy! Grab the Complete Diastasis Recti Healing Guide: https://landing.mailerlite.com..../webforms/landing/n0
If you are't sure what video to start with and you just want step-by-step daily instructions you can start my 30-day core healing program. You get a new 10-min core healing video daily for 30 days. https://pregnancyandpostpartum....tv.thinkific.com/cou
How I healed my 4-finger diastasis recti gap:
Jessica Pumple is a registered dietitian, and pre & postnatal fitness instructor and certified pregnancy and postpartum core exercise specialist (CPES). She helps pregnant women stay fit, have healthy babies, and easier labors. She helps new moms with postpartum recovery, to heal and strengthen their core and feel energized after pregnancy!
If you enjoy our content subscribe to our channel, hit the bell button, leave a comment and share with your friends so I can make you more of the videos you enjoy!
Disclaimer: This is general postnatal fitness only. Please check with your doctor or health care provider to see if this video is safe for you. Wait until you get clearance (usually 4-6 weeks or 6-8 weeks after a c-section).You are responsible for your own safety. Don’t do anything that feels unsafe for you or baby. Stop if you have any pain or discomfort, bleeding, chest pain or shortness of breath, dizziness or if you feel unwell. P&P Health Inc., Pregnancy and Postpartum TV and Jessica Pumple are not liable in any way for any injury, loss, damages, costs or expenses suffered by you in relation to this video or its content.
Copyright 2023 P&P Health Inc. All rights reserved
#diastasisrecti #whatisdiastasisrecti #3danimation
Music: Epidemic Sound

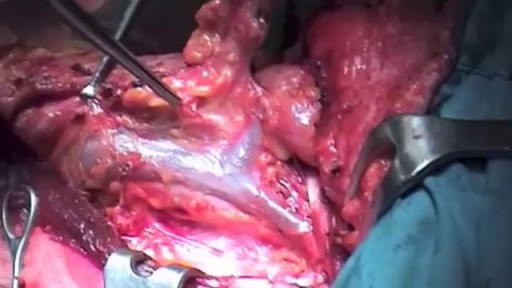
A Lecture Presented by Dr. Mostafa Yakoot to Vascular Surgery Congress. TITLE: SAFETY & EFFICACY OF A NEW HONEY OINTMENT (PEDYPHAR) FOR DIABETIC FOOT ULCERS. Based on the original article in JWC by: Yakoot M, Abdelatif M, Etman M.

© 2023 Elsevier. All rights reserved. Histologically the cervix is different from the rest of the uterus and also has a mucosa that doesn’t shed during menstruation.
Find our full video library only on Osmosis Prime: http://osms.it/more.
Join over 3 million current & future clinicians who learn by Osmosis, and over 130 universities around the world who partner with us to make medical and health education more engaging and efficient. We have unparalleled tools and materials to prepare you to succeed in school, on board exams, and as a future clinician. Sign up for a free trial at http://osms.it/more. If you're interested in exploring an institutional partnership, visit osmosis.org/educators to request a personalized demo.
Follow us on social:
Facebook: http://osms.it/facebook
Twitter: http://osms.it/twitter
Instagram for med: http://osms.it/instagram
Instagram for nursing: https://osms.it/ignursing
Linkedin: https://osms.it/linkedin
Our Vision: Everyone who cares for someone will learn by Osmosis.
Our Mission: To empower the world’s clinicians and caregivers with the best learning experience possible. Learn more here: http://osms.it/mission
Medical disclaimer: Knowledge Diffusion Inc (DBA Osmosis) does not provide medical advice. Osmosis and the content available on Osmosis's properties (Osmosis.org, YouTube, and other channels) do not provide a diagnosis or other recommendation for treatment and are not a substitute for the professional judgment of a healthcare professional in diagnosis and treatment of any person or animal. The determination of the need for medical services and the types of healthcare to be provided to a patient are decisions that should be made only by a physician or other licensed health care provider. Always seek the advice of a physician or other qualified healthcare provider with any questions you have regarding a medical condition. © 2023 Elsevier. All rights reserved.

http://www.highimpact.com - This brain surgery animation was used to demonstrate a young girl's craniotomy, cranioplasty, and reconstructive skull surgery after her vehicle was struck by a tractor-trailer. The procedures included the evacuation of a large epidural hematoma, the draining of the epidural space, and the reassembly of bone fragments to repair the skull.
More Brain Surgery Animations: https://tinyurl.com/y6m4lkdf
WHAT HAPPENED
A teenage girl was riding home with her parents and boyfriend from a Wednesday night church service when a tractor-trailer struck the back driver’s side of their car as they were traveling through an intersection. The impact sent the car spinning into oncoming traffic where it struck another vehicle. When paramedics arrived, the 17-year-old was unresponsive with bleeding from her left ear and a laceration from behind her left ear.
She was rushed to the hospital where she underwent a series of CT scans that showed a severely comminuted open skull fracture with an underlying 1.1 cm subdural hematoma. She was taken to the operating room where an emergency craniotomy was performed to evacuate the hematoma and reassemble the skull fragments. The patient gradually began to wake up and was discharged six days later, after she showed she could maneuver up and down the hallway.
The biggest challenge in a traumatic brain injury case like this - where most of the damages are deeply underlying and undetectable on the surface - is that the only visual evidence is in the form of 2D black-and-white radiographic films. This can look ambiguous to the typical juror because it’s often difficult to discern where these snapshots are located inside the person’s skull. Tony Seaton, Esq., and Robert Bates, Esq., needed to reinforce this 2D radiographic evidence with maximum 3D context.
We equipped them with a custom Diagnostic Slice Chooser: an interactive presentation that presents radiographic slides within a three-dimensional model of the patient’s head. We also designed the model accurately to the patient’s likeness and colorized the films to highlight key areas of damage. The attorneys could show the complete depth and magnitude of his client’s injuries at every level both before and after the surgery. After establishing the full extent of damages, we also created an animation to walk viewers through the surgical experience the patient would undergo as a result of her injuries.
The visual presentation helped jurors understand the destructive impact this collision had on this young teenager’s life, and Mr. Seaton and Mr. Bates, Esq., were able to acquire a $4.5M settlement for his client.
Read the Full Case Study: https://tinyurl.com/yy4v2dyh

Bloating And Gas, Flatulence Remedy Ginger, Get Rid Of Gas And Bloating, Involuntary Flatulence--- http://flatulence-cure.plus101.com --- 7 tips on Flatulence Treatment and help you get rid of flatulence forever. 1. Flatulence is such a broad term, with so many connected and side issues, that it is rather short sighted to refer to it simply as "farting" - which so many people do. Certainly, the breaking of wind is the key identifier for flatulence. However, to merely concentrate on the noise and the smell of flatulence is to miss out on the important facts that govern its causes, its symptoms and its remedies. Picking the right flatulence treatment means needing to concentrate on the type of flatulence you have, the health issues surrounding it and the general health situation of the sufferer. 2. Be Realistic in Your Flatulence Treatment If the definition of flatulence was simply that you had wind a few times a day and occasionally broke wind in embarrassing situations, then flatulence treatment really would not be that much of a priority. However, the truth of the matter is that excessive flatulence will affect more than just social situations. It is thankfully uncommon enough to suffer from painful stomach flatulence, but that is not to say that it is something you should ever ignore. Your digestive system is vitally important for your health, and if problems arise then they need to be addressed with the right flatulence treatment. 3. When you are suffering from flatulence problems, you need to identify why it is a problem and what the problem can be traced back to. We all have flatulence every so often, most of us having wind at least once a day and usually more often. Getting rid of the gases that our system generates when digesting food is essential, as is finding a kind flatulence treatment - otherwise we would soon become quite unwell. It is how often you release those gases and how they are released that matters more than anything. The last thing you want is to have occasional, sporadic flatulence that hurts, smells foul or is particularly audible. 4. Gas is a by-product of digestion, and if you are not breaking wind at all then there is probably a problem. Excessive flatulence means that you are producing too much gas when digesting food, and means that your digestive system is not functioning as it should be. 5. Painful flatulence occurs when you are digesting the food badly, because the stomach is failing to break it down as smoothly as it should. It is not that uncommon to feel, perhaps, a little bit of burning flatulence - this can happen after too much spicy food - but if it is becoming the norm then it is something that needs to be addressed with the right flatulence treatments. 6. Keep A Note For Best Flatulence Treatment Results 7. By identifying which foods are connected with which problems, you can begin the right flatulence treatment. It is better to do this, and deal with the problem before it grows rather than trying to cure a bigger problem. Would you like to cure your gas problems and bloating today! Then you need to see this website below: http://flatulence-cure.plus101.com
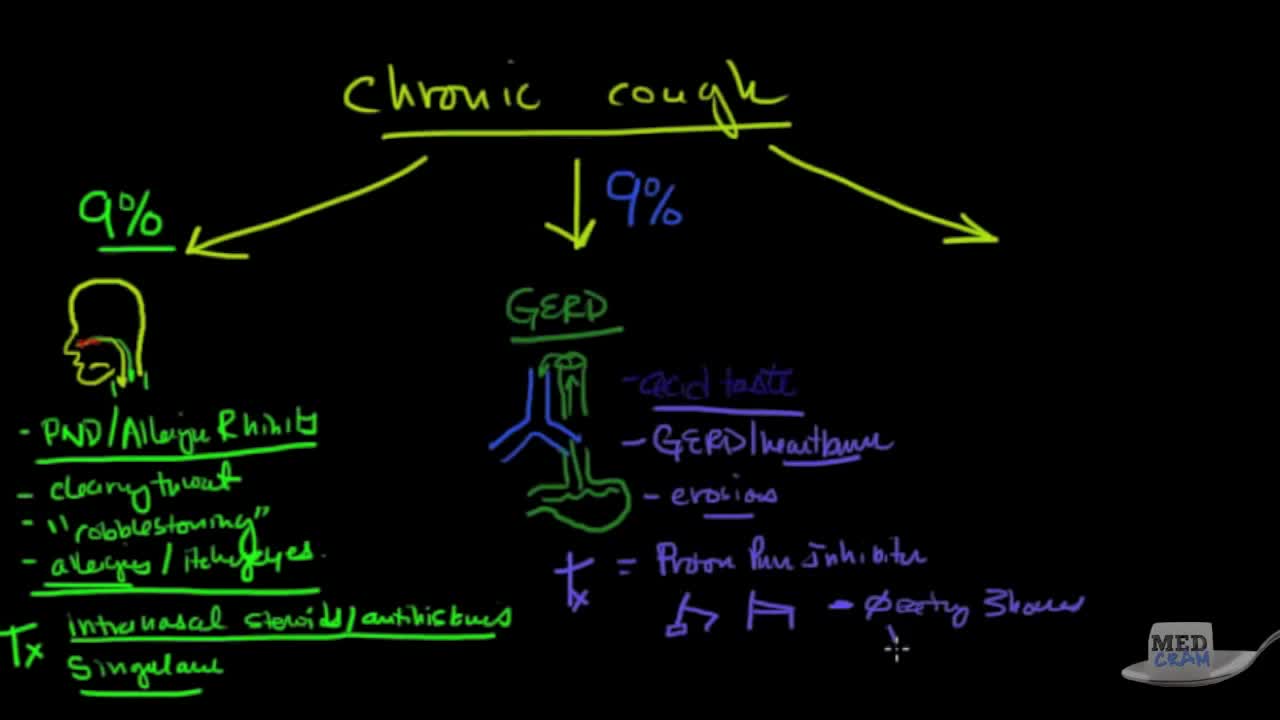
A chronic cough is a cough that lasts eight weeks or longer in adults, or four weeks in children. A chronic cough is more than just an annoyance. A chronic cough can interrupt your sleep and leave you feeling exhausted. Severe cases of chronic cough can cause vomiting, lightheadedness and even rib fractures. While it can sometimes be difficult to pinpoint the problem that's triggering a chronic cough, the most common causes are tobacco use, postnasal drip, asthma and acid reflux. Fortunately, chronic cough typically disappears once the underlying problem is treated.

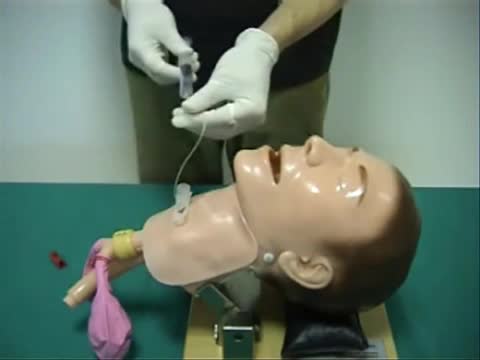
Pinch air out of the tip of the condom. Unroll condom all the way down the penis. After sex but before pulling out, hold the condom at the base. Then pull out, while holding the condom in place. Carefully remove the condom and throw it in the trash.

The goal of COPD management is to improve a patient’s functional status and quality of life by preserving optimal lung function, improving symptoms, and preventing the recurrence of exacerbations. Currently, no treatments aside from lung transplantation have been shown to significantly improve lung function or decrease mortality; however, oxygen therapy (when appropriate) and smoking cessation may reduce mortality. Once the diagnosis of COPD is established, it is important to educate the patient about the disease and to encourage his or her active participation in therapy.

Transgender Man Gives Birth to Healthy Baby, Talks Navigating Pregnancy as a Man Trystan Reese is a transgender man who just gave birth to a healthy baby boy. He told us about his pregnancy—and why his story isn't so out of the ordinary.