Top videos
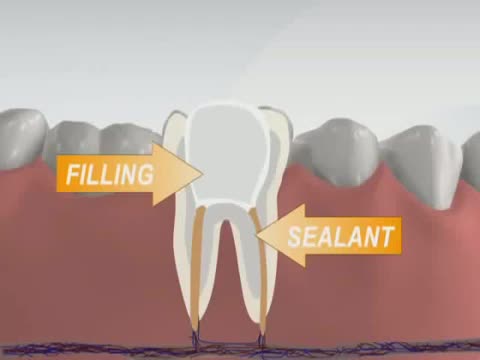
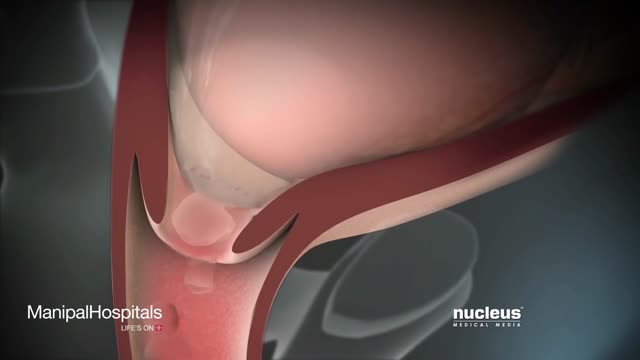
Has your dentist or endodontist told you that you need root canal treatment? If so, you're not alone. Millions of teeth are treated and saved each year with root canal, or endodontic, treatment. Remember, root canal treatment doesn't cause pain, it relieves it. Watch our videos below to learn more! Inside the tooth, under the white enamel and a hard layer called the dentin, is a soft tissue called the pulp. The pulp contains blood vessels, nerves and connective tissue, and helps to grow the root of your tooth during development. In a fully developed tooth, the tooth can survive without the pulp because the tooth continues to be nourished by the tissues surrounding it.

This video shows you how to examine the hand and wrist and how to identify common causes of pain.
This video clip is part of the FIFA Diploma in Football Medicine and the FIFA Medical Network. To enrol or to find our more click on the following link http://www.fifamedicalnetwork.com
The Diploma is a free online course designed to help clinicians learn how to diagnose and manage common football-related injuries and illnesses. There are a total of 42 modules created by football medicine experts. Visit a single page, complete individual modules or finish the entire course.
The network provides the opportunity for clinicians around the world to meet and share ideas relating to football medicine. Ask about an interesting case, debate current practice and discuss treatment strategies. Create a profile and log on to interact with other health professionals from around the globe.
This is not medical advice. The content is intended as educational content for health care professionals and students. If you are a patient, seek care of a health care professional.

Transgender Man Gives Birth to Healthy Baby, Talks Navigating Pregnancy as a Man Trystan Reese is a transgender man who just gave birth to a healthy baby boy. He told us about his pregnancy—and why his story isn't so out of the ordinary.

Examination of Peripheral Vascular System - Clinical Skills OSCE Revision - Dr Gill
In this video, we demonstrate the peripheral vascular examination - a less common examination, but still vitally important, particularly amongst the older population
Starting with the examination of the hands looking for clinical signs of vascular compromise, we then check the pulses of the major arteries of the upper body - the radial, brachial and carotid arteries, before moving down to assess for an abdominal aortic aneurysm.
At this point, I feel it's a practical step to check the femoral pulses before doing the overview of the legs.
After visually assessing we must examine the major vascular areas of leg.- namely the popliteal pulses, before wrapping up around the ankle with the posterior tibial and dorsalis pedis pulses
For completeness, the cardiovascular examination is demonstrated here
https://www.youtube.com/watch?v=ECs9O5zl6XQ&t=2s
#PeripheralVascular #ClinicalSkills #DrGill

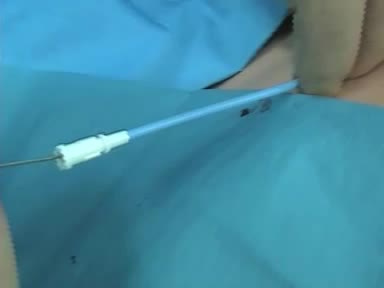
With help from Trisolt Video Productions. We created a video to help payer sources, caregivers, and Healthcare Profesionals relate to the concept of not recycling Intermttent Catheters. Take a look and let us know what you think. If you would like to learn more about our Service Plus Program. Please call 800-747-0246 or visit www.colonialmed.com
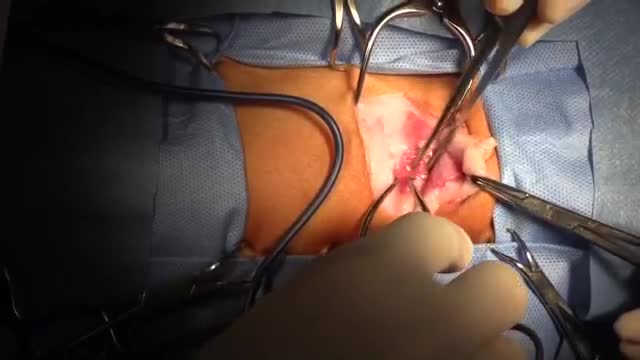
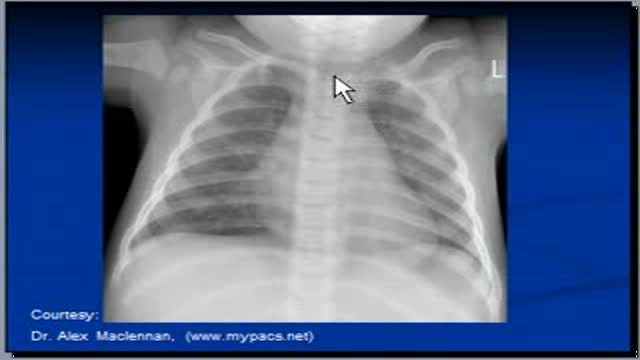
This video: Patent ductus arteriosus (PDA) is a persistent opening between two major blood vessels leading from the heart. The opening, called the ductus arteriosus, is a normal part of a baby's circulatory system before birth that usually closes shortly after birth. If it remains open, however, it's called a patent ductus arteriosus. A small patent ductus arteriosus often doesn't cause problems and might never need treatment. However, a large patent ductus arteriosus left untreated can allow poorly oxygenated blood to flow in the wrong direction, weakening the heart muscle and causing heart failure and other complications. Treatment options for a patent ductus arteriosus include monitoring, medications and closure by cardiac catheterization or surgery.
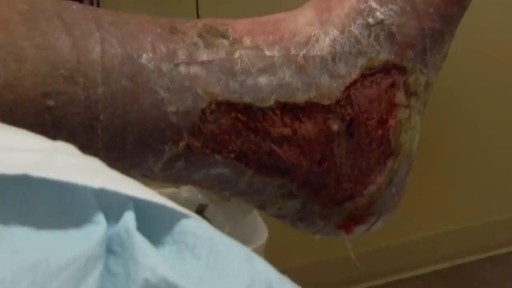
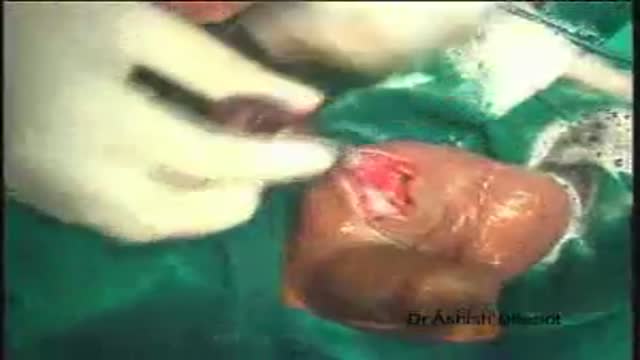
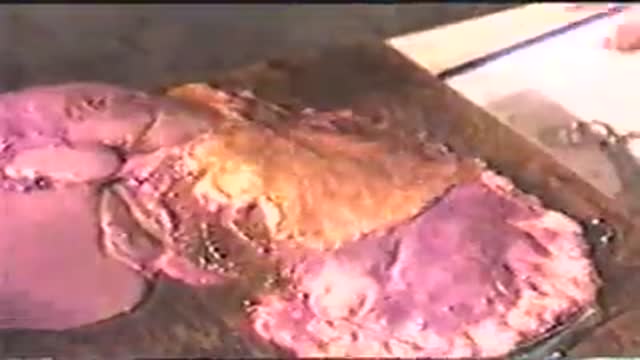
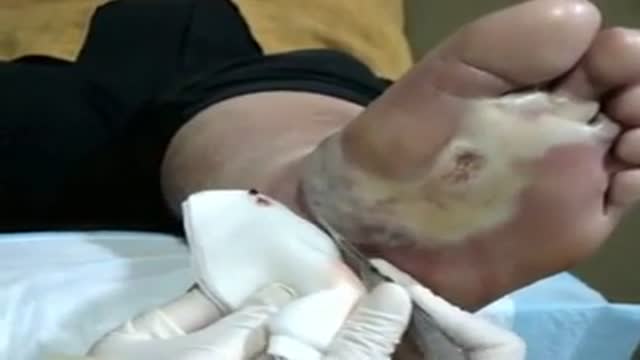
Debridement is the removal of necrotic tissue, foreign debris, bacterial growth, callus, wound edge, and wound bed tissue from chronic wounds in order to stimulate the wound healing process. Stimulation of wound healing mediated by debridement is thought to occur by the conversion of a chronic non-healing wound environment to an acute healing environment through the removal of cells that are not responsive to endogenous healing stimuli. Debridement is used commonly in standard wound treatment of diabetic foot ulcers (DFUs). Methods of debridement include surgery (sharp debridement), chemical debridement (antiseptics, polysaccharide beads, pastes), autolytic (hydrogels, hydrocolloids and transparent films), biosurgery (maggots), mechanical (hydrodebridement), and biochemical debridement (enzyme preparations). Callus is a buildup of keratinized skin formed under conditions of repeated pressure or friction and may contribute to ulcer formation by creating focal areas of high plantar pressure. The debridement of callus has been proposed to be relevant for both treatment and prevention of DFU. The purpose of this report is to retrieve and review existing evidence of comparative clinical effectiveness of different methods of debridement for the treatment of DFUs. Additionally examined in this report is the clinical effectiveness for treatment and prevention of DFU using callus debridement. Cost-effectiveness, and existing debridement guidelines for the treatment of DFUs will also be reviewed.