Top videos
A pneumothorax occurs when some of the tiny air sacs (alveoli) in a baby's lung become overinflated and burst. This causes air to leak into the space between the lung and chest wall (pleural space). The most common cause of pneumothorax is respiratory distress syndrome. This is a condition that occurs in babies who are born too early (premature). The baby's lungs lack the slippery substance (surfactant) that helps them stay open. Therefore, the tiny air sacs are not able to expand as easily. If the baby is put on a breathing machine (mechanical ventilator), there is extra pressure on the baby's lungs, which can sometimes burst the air sacs.
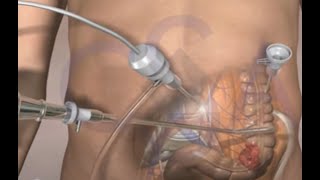
This surgical animation is for patient education and describes a laparoscopic colectomy, which is a type of minimally invasive surgery for colon cancer. Laparoscopic colectomy, also called minimally invasive colectomy, involves several small incisions in your abdomen. Instead of a big incision, the surgeon makes a few small cuts (0.5-1 centimeters) in the abdominal cavity to insert a surgical camera and instruments and perform the operation. A slightly bigger incision, about 3.5 centimeters wide, is made to remove the tumor.
When compared to traditional open surgery, laparoscopic colectomy can result in much less pain and swifter recovery. Depending on the procedure, most laparoscopic colectomy patients leave the hospital and return to normal activities more quickly than patients recovering from open surgery.
Colorectal cancer is the second leading cause of cancer death in the United States.
For more information about 3d animation videos, please visit https://www.amerra.com

Learn what's working for other Nursing Students! Check out our Top 10 Most Popular Lessons Here: https://bit.ly/3nda5u3
Get the full lesson here: https://nursing.com/lesson/ski....lls-03-04-trach-care
Welcome to the NURSING Family, we call it the most supportive nursing cohort on the planet.
At NURSING.com, we want to help you remove the stress and overwhelm of nursing school so that you can focus on becoming an amazing nurse.
Check out our freebies and learn more at: (http://www.nursing.com)
Trach Care Overview (Nursing Skills):
In this video we’re going to look at trach care. Remember you should always suction the patient before trach care, so if you haven’t watched that skill video yet, make sure you watch it!
Click here: https://nursing.com/lesson/ski....lls-03-03-trach-suct
And remember as you’re doing this, you want to be assessing the stoma for signs of infection or skin breakdown.
Bookmarks:
0:00 Introduction
0:30 Set up sterile field
1:00 Apply gloves
1:12 Remove inner canula and dressing
1:30 Apply sterile gloves
2:05 Clean secretions
2:56 Clean stoma
3:48 Replace inner canula
4:14 Change trach ties
5:50 Apply dressing
Visit us at https://nursing.com/medical-disclaimer/ for disclaimer information.
NCLEX®, NCLEX-RN® are registered trademarks of the National Council of State Boards of Nursing, INC. and hold no affiliation with NURSING.com.
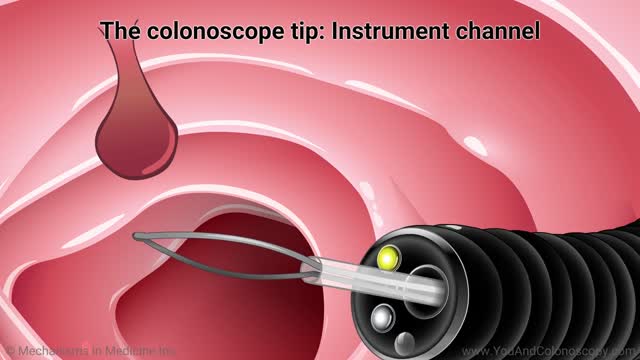
A colonoscope is the special tool used to perform a colonoscopy. It is a thin, flexible, tubular ‘telescope’ with a light and video camera that your doctor carefully guides through your colon in order to see and determine the health of your colon. Watch this animation to learn about the features of the colonoscope, how the colonoscopy procedure is performed and how polyps are removed, and the follow-up care you and your doctor should talk about after your procedure.
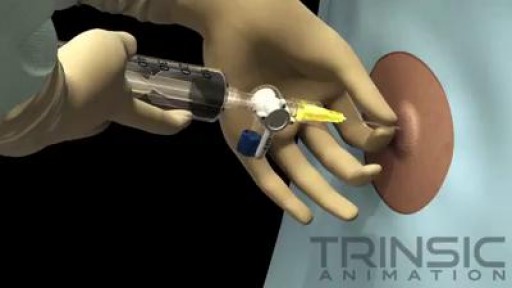
Thoracentesis is a procedure in which a needle is inserted into the pleural space between the lungs and the chest wall. This procedure is done to remove excess fluid, known as a pleural effusion, from the pleural space to help you breathe easier. It may be done to determine the cause of your pleural effusion. Some conditions such as heart failure, lung infections, and tumors can cause pleural effusions.

Bell's palsy is a form of facial paralysis resulting from damage or trauma to the facial nerves. The facial nerve-also called the 7th cranial nerve-travels through a narrow, bony canal (called the Fallopian canal) in the skull, beneath the ear, to the muscles on each side of the face. For most of its journey, the nerve is encased in this bony shell. Each facial nerve directs the muscles on one side of the face, including those that control eye blinking and closing, and facial expressions such as smiling and frowning. Additionally, the facial nerve carries nerve impulses to the lacrimal or tear glands, the saliva glands, and the muscles of a small bone in the middle of the ear called the stapes. The facial nerve also transmits taste sensations from the tongue. When Bell's palsy occurs, the function of the facial nerve is disrupted, causing an interruption in the messages the brain sends to the facial muscles. This interruption results in facial weakness or paralysis. Bell's palsy is named for Sir Charles Bell, a 19th century Scottish surgeon who described the facial nerve and its connection to the condition. The disorder, which is not related to stroke, is the most common cause of facial paralysis. Generally, Bell's palsy affects only one of the paired facial nerves and one side of the face, however, in rare cases, it can affect both sides.