Top videos

🔥 Multivitamins for Men: https://lynxshort.com/Multivitamins-for-Men
✨ Multivitamins for Women: https://lynxshort.com/Multivitamins-for-Women
⭐ Multivitamins for Kids: https://lynxshort.com/Multivitamins-for-Kids
📙 Book of the Day 📚 https://lynxshort.com/Book-of-the-Day
This is one of the most interesting medical topics to discuss. What are the responsibilities of a doctor? What are the basic skills a doctor needs to have? and what are the responsibilities of a doctor?
**** CONNECT ****
- " Medical Videos " Android application on Google Play store:
https://play.google.com/store/....apps/details?id=com.
https://healthusher.com
https://www.facebook.com/MedicalVideosAnimated
https://www.instagram.com/medical_videos1
👉 Support Us to Help Us Continue Making Videos.. Thanks in Advance :)
- Via PayPal: https://www.paypal.me/medicalvideos
- Via Patreon: https://www.patreon.com/medicalvideosanimated
- The creator:
Pharmacist. Alaa Nasr
#MedicalVideosAnimated
Affiliate Disclaimer: This video and description contains affiliate links, which means that if you click on one of the product links, I'll receive a small commission. This is at no extra cost to you and in many cases include exclusive discounts where applicable. This helps support the channel and allows me to continue to make free videos like this. Thank you for the support!
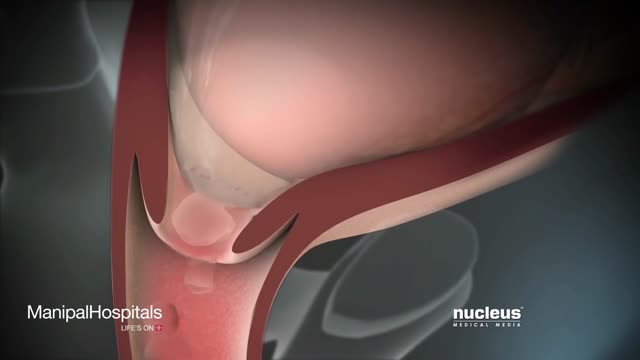
An intrauterine device (IUD), also known as intrauterine contraceptive device (IUCD or ICD) or coil, is a small, often T-shaped birth control device that is inserted into a woman's uterus to prevent pregnancy. IUDs are one form of long-acting reversible birth control (LARC).

In this video, I have covered Inguinal hernia under the following headings: Definition, Parts of Hernia, Surgical anatomy, Types of inguinal hernia, Aetiology of hernia, Clinical features of hernia, complications of hernia, Clinical examination, Surgical principles, and explanation of a few surgeries (Herniotomy, Bassini suture repair, Shouldice repair, Lichtenstein tension-free open meshplasty, hernia plugs, Laparoscopic techniques like TEP(Totally extraperitoneal approach) and TAPP(Transabdominal preperitoneal approach) surgical procedures).
SUBSCRIBE FOR MORE VIDEOS!
How to study General Surgery in med school: (Tips and Tricks)
https://youtu.be/_tad4i2Kdes
1-minute hernia videos: (Complete playlist by Skeleton)
https://www.youtube.com/watch?v=GsmAPYMiK_s&list=PL-dMZTUxuTxAi7rFqOy9o0pv1g-aZ1GXz
(includes femoral hernia, obturator hernia, epigastric hernia, umbilical hernia, Spigelian hernia, Richter hernia, lumbar hernia, incisional hernia, Hiatal hernia, congenital diaphragmatic hernia, contents of spermatic cord, triangles of hernia)
Study with me:
https://www.youtube.com/watch?v=lBkmmYcUBDo&t=291s
Hydrocele video:
https://www.youtube.com/watch?v=s6ICxMMtpYk&t=65s
You can support my channel by buying me a coffee here:
https://www.buymeacoffee.com/medvids
(Lecture slides will be available in the "EXTRAS" section of this link)
Instagram: @medvidsmadesimple
Check out my other works: linktr.ee/doctorcool
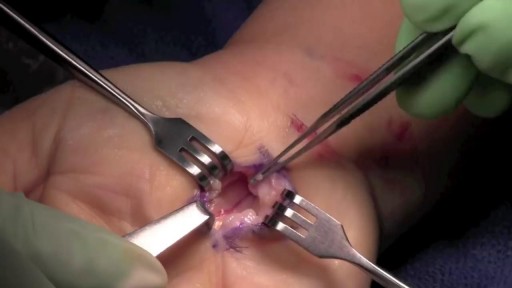
During open carpal tunnel release surgery, the transverse carpal ligament is cut, which releases pressure on the median nerve and relieves the symptoms of carpal tunnel syndrome. An incision is made at the base of the palm of the hand. This allows the doctor to see the transverse carpal ligament.
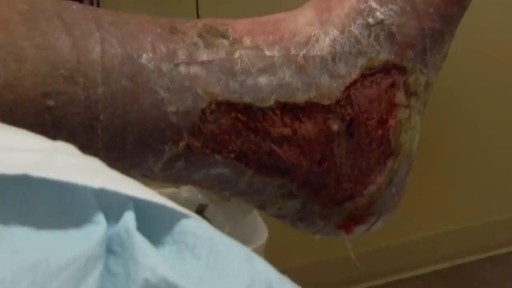
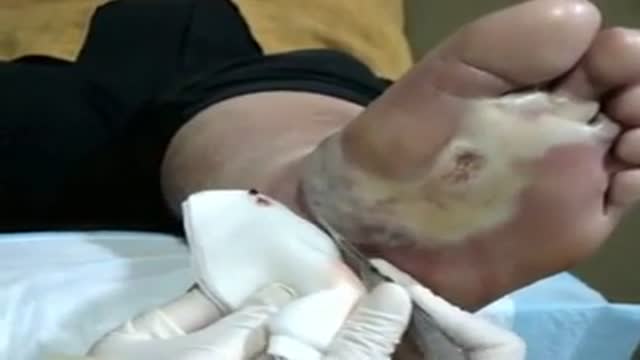
Debridement is the removal of necrotic tissue, foreign debris, bacterial growth, callus, wound edge, and wound bed tissue from chronic wounds in order to stimulate the wound healing process. Stimulation of wound healing mediated by debridement is thought to occur by the conversion of a chronic non-healing wound environment to an acute healing environment through the removal of cells that are not responsive to endogenous healing stimuli. Debridement is used commonly in standard wound treatment of diabetic foot ulcers (DFUs). Methods of debridement include surgery (sharp debridement), chemical debridement (antiseptics, polysaccharide beads, pastes), autolytic (hydrogels, hydrocolloids and transparent films), biosurgery (maggots), mechanical (hydrodebridement), and biochemical debridement (enzyme preparations). Callus is a buildup of keratinized skin formed under conditions of repeated pressure or friction and may contribute to ulcer formation by creating focal areas of high plantar pressure. The debridement of callus has been proposed to be relevant for both treatment and prevention of DFU. The purpose of this report is to retrieve and review existing evidence of comparative clinical effectiveness of different methods of debridement for the treatment of DFUs. Additionally examined in this report is the clinical effectiveness for treatment and prevention of DFU using callus debridement. Cost-effectiveness, and existing debridement guidelines for the treatment of DFUs will also be reviewed.

With help from Trisolt Video Productions. We created a video to help payer sources, caregivers, and Healthcare Profesionals relate to the concept of not recycling Intermttent Catheters. Take a look and let us know what you think. If you would like to learn more about our Service Plus Program. Please call 800-747-0246 or visit www.colonialmed.com

The goal of COPD management is to improve a patient’s functional status and quality of life by preserving optimal lung function, improving symptoms, and preventing the recurrence of exacerbations. Currently, no treatments aside from lung transplantation have been shown to significantly improve lung function or decrease mortality; however, oxygen therapy (when appropriate) and smoking cessation may reduce mortality. Once the diagnosis of COPD is established, it is important to educate the patient about the disease and to encourage his or her active participation in therapy.

#HerniaRepair #HerniaSurgery #LaparoscopicHerniaRepair #OpenHerniaRepair #InguinalHernia #UmbilicalHernia #VentralHernia #MeshRepair #HerniaRecovery #HerniaComplications
hernia operation
hernia treatment
hernia
hernia treatment at home
hernia operation and recovery
hernia surgery and recovery
terapi hernia
inguinal hernia treatment without surgery
harnia
hernia surgery
hernia surgery animation
harniya operation
hernia symptoms men
harniya
hernia ka ilaj
hernia laparoscopic surgery animation
abdominal hernia treatment without sur...
hernia symptoms
turun berok
abdominal hernia
hernia exercises without surgery
hernia operation in 3d animation
inguinal hernia surgery
umbilical hernia symptoms and treatment
harnia operation
harniya ka ilaj
hernia animation
hernia belt
hernias
how to treat hernia without surgery
inguinal hernia recovery after surgery
ngiri
open hernia surgery
skates
turun bero
3d surgery
after hernia surgery recovery
appam kaise banate hain
hernia belt for men
hernia belt how to use
hernia exam
hernia inguinal sintomas
hernia ka operation kaisa hota hai
hernia operation ke baad exercise
hernia operation video
hernia repair
hernia repair mesh complications
hernia repair surgery animation
hernia surgery recovery tips
hernie abdominale
herniya
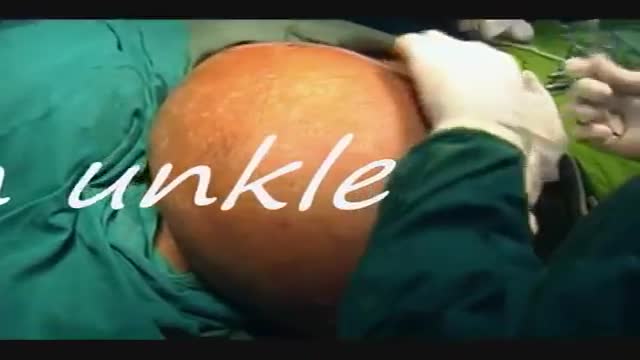
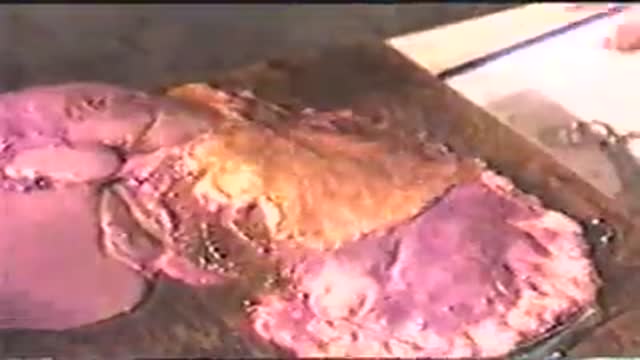
Lipomas are slow-growing soft tissue tumours that rarely reach a size larger than 2 cm. Lesions larger than 5 cm, so-called giant lipomas, can occur anywhere in the body but are seldom found in the upper extremities. The authors present their experiences with eight patients having giant lipomas of the upper extremity. In addition, a review of the literature, and a discussion of the appropriate evaluation and management are included.

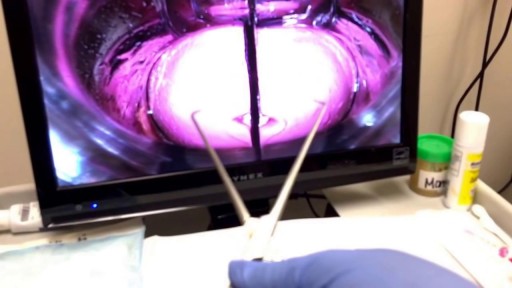
Shane Shapiro, M.D., orthopedic physician at Mayo Clinic in Florida, performs a bone marrow aspiration and concentration for BMAC/stem cell injection into arthritic knees. This procedure is part of a Mayo Clinic IRB approved, FDA monitored clinical research trial which can be searched on at http://ClinicalTrials.gov.
Mayo Clinic and the Mayo Center for Regenerative Biotherapeutics is studying biologically based non-surgical treatments for osteoarthritis. One such treatment is the harvesting of the patient's own stem cells from their bone marrow.
"In our procedure we draw cellular rich bone marrow from both sides of the pelvis. We then filter the resulting product and concentrate the stem cells and their corresponding growth factors. Using an ultrasound to image the knee joint, we are then able to precisely inject the cells into the arthritic knee. We are currently demonstrating that this procedure is safe and can relieve pain. We also hope to be able to slow the progression of the degenerative joint disease and perhaps one day regrow cartilage in the arthritic joint."
------
Hear Dr. Shapiro discus this procedure in detail here: http://youtu.be/8Djpsc66hKI
Learn more about the Mayo Clinic Center for Regenerative Biotherapeutics here: http://goo.gl/rnRdtU
------
Mayo Clinic...
On Facebook: http://Facebook.com/MayoClinic
On Twitter: http://twitter.com/MayoClinic
On Google+: http://google.com/+MayoClinic
On Instagram: http://instagram.com/MayoClinic
On Pinterest: http://Pinterest.com/MayoClinic
On YouTube: http://YouTube.com/MayoClinic
On the blogs: http://connect.MayoClinic.org