Top videos
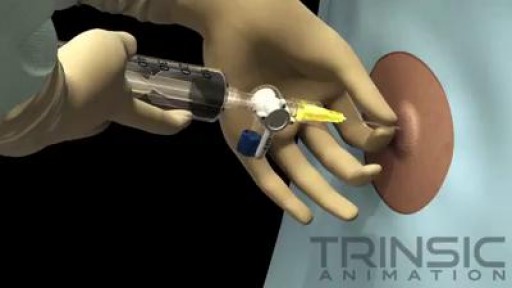
Thoracentesis is a procedure in which a needle is inserted into the pleural space between the lungs and the chest wall. This procedure is done to remove excess fluid, known as a pleural effusion, from the pleural space to help you breathe easier. It may be done to determine the cause of your pleural effusion. Some conditions such as heart failure, lung infections, and tumors can cause pleural effusions.

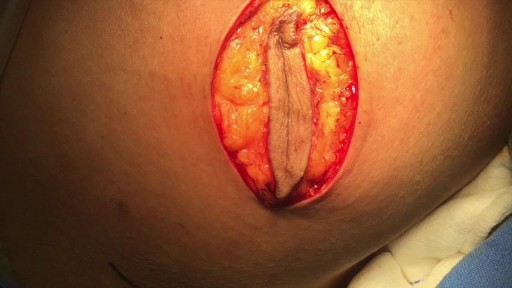
plantar fasciitis and calcaneal spur can be treated by EPFR with calcanean drilling - endoscopic plantar fascia release علاج الشوكة العظمية للكعب بالمنظار د. أسامة الشاذلي مدرس جراحة العظام واستشاري جراحات و مناظير القدم والكاحل كلية الطب جامعة عين شمس
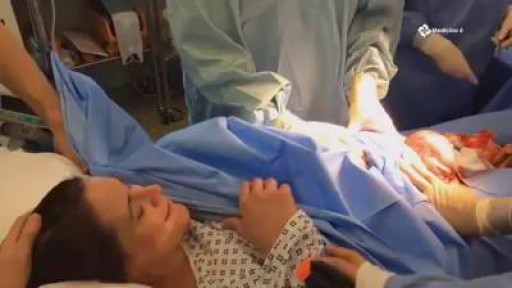
Most C-sections are done under regional anesthesia, which numbs only the lower part of your body — allowing you to remain awake during the procedure. A common choice is a spinal block, in which pain medication is injected directly into the sac surrounding your spinal cord
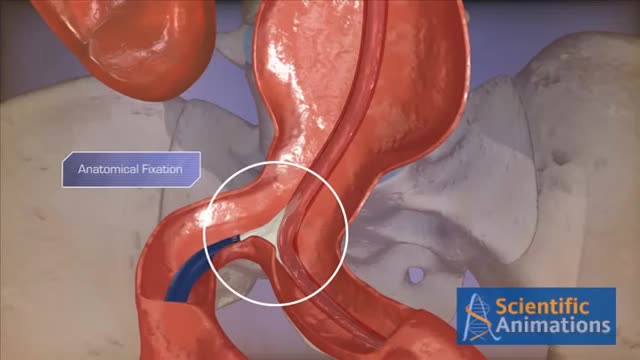
Abdominal aortic aneurysms can weaken the aorta, your body’s largest blood vessel. This can develop into a potentially serious heath problem that can be fatal if the aneurysm bursts, causing massive internal bleeding. Endovascular stent grafting, or endovascular aneurysm repair (EVAR), is a newer form of treatment for abdominal aortic aneurysm that is less invasive than open surgery. Endovascular stent grafting uses an endovascular stent graft to reinforce the wall of the aorta and to help keep the damaged area from rupturing.

Learn what's working for other Nursing Students! Check out our Top 10 Most Popular Lessons Here: https://bit.ly/3nda5u3
Get the full lesson here: https://nursing.com/lesson/ski....lls-03-04-trach-care
Welcome to the NURSING Family, we call it the most supportive nursing cohort on the planet.
At NURSING.com, we want to help you remove the stress and overwhelm of nursing school so that you can focus on becoming an amazing nurse.
Check out our freebies and learn more at: (http://www.nursing.com)
Trach Care Overview (Nursing Skills):
In this video we’re going to look at trach care. Remember you should always suction the patient before trach care, so if you haven’t watched that skill video yet, make sure you watch it!
Click here: https://nursing.com/lesson/ski....lls-03-03-trach-suct
And remember as you’re doing this, you want to be assessing the stoma for signs of infection or skin breakdown.
Bookmarks:
0:00 Introduction
0:30 Set up sterile field
1:00 Apply gloves
1:12 Remove inner canula and dressing
1:30 Apply sterile gloves
2:05 Clean secretions
2:56 Clean stoma
3:48 Replace inner canula
4:14 Change trach ties
5:50 Apply dressing
Visit us at https://nursing.com/medical-disclaimer/ for disclaimer information.
NCLEX®, NCLEX-RN® are registered trademarks of the National Council of State Boards of Nursing, INC. and hold no affiliation with NURSING.com.
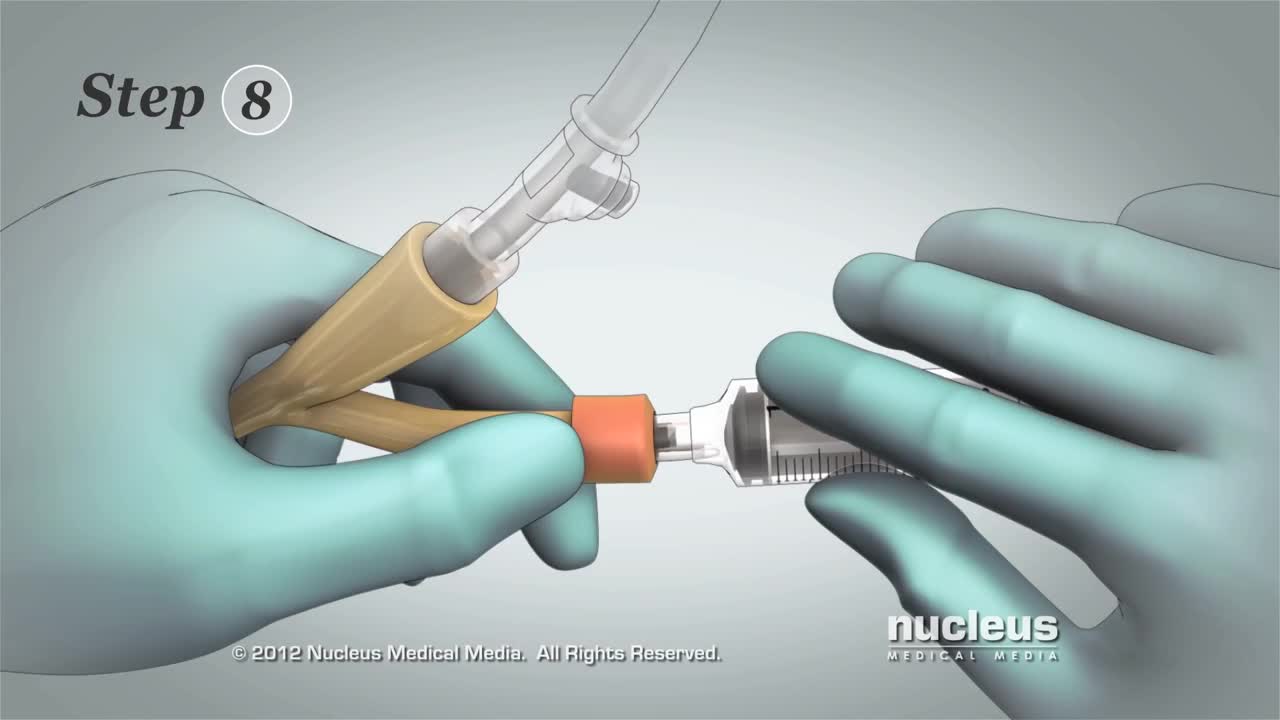
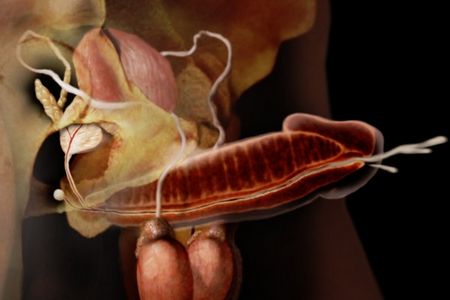
This 3D medical animation contains the discharge instructions for removal of a Foley catheter from a man. The step-by-step procedures for emptying the Foley bag and removing the Foley catheter are shown. Symptoms requiring a follow-up call to the surgeon are listed.
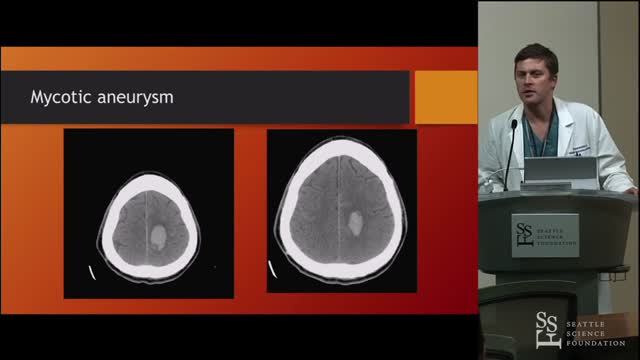
The headache, lethargy, and neck stiffness suggest subarachnoid hemorrhage secondary to rupture of a mycotic aneurysm. Mycotic or infected arterial aneurysms can develop due to metastatic infection from IE, with septic embolization and localized vessel wall destruction in the cerebral (or systemic) circulation. Intracerebral mycotic aneurysms can present as an expanding mass with focal neurologic findings or may not be apparent until aneurysm rupture with stroke or subarachnoid hemorrhage. The diagnosis of mycotic cerebral aneurysm can usually be confirmed with computed tomography angiography. Management includes broad-spectrum antibiotics (tailored to blood culture results) and surgical intervention (open or endovascular).

http://www.nucleushealth.com/ - This 3D medical animation shows the cause and laparoscopic treatment of a ventral incisional hernia. If you have had abdominal surgery in the past, a ventral incisional hernia may appear at the site of your surgical scar. Your intestine may push through a weakened spot in the tissue between your abdominal muscles creating a bulge beneath your skin. If your hernia is not repaired, complications may occur.
#VentralHernia #VentralIncisionalHernia #IncisionalHernia
ANH11053
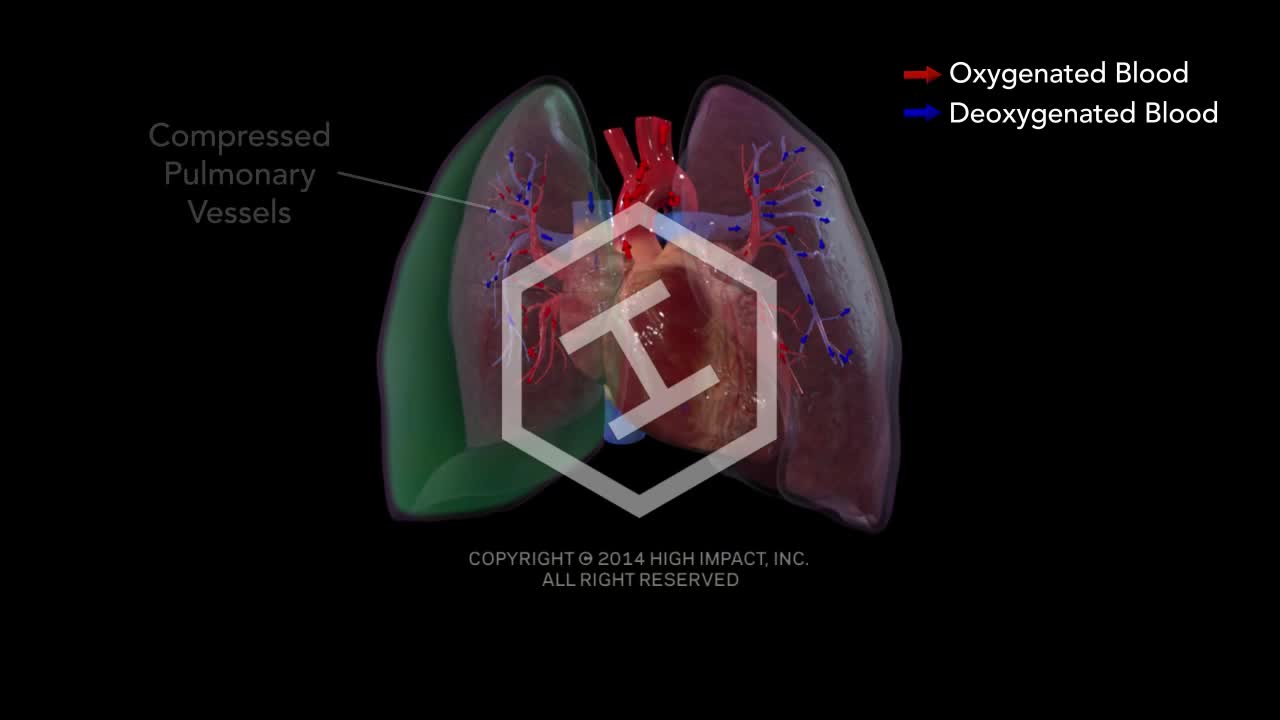
Tension pneumothorax develops when a lung or chest wall injury is such that it allows air into the pleural space but not out of it (a one-way valve). As a result, air accumulates and compresses the lung, eventually shifting the mediastinum, compressing the contralateral lung, and increasing intrathoracic pressure enough to decrease venous return to the heart, causing shock. These effects can develop rapidly, particularly in patients undergoing positive pressure ventilation.

Our mission: Empower you with the tools and support you need for weight loss and live a healthier life. Get started on your weight loss journey today: https://bit.ly/2Ms4JaX