Top videos

If you're pregnant, you're likely paying extra close attention to your body. If you happen to feel a cramp you may worry that it is a sign of a miscarriage. While the first trimester is the most common time for miscarriages, there are other reasons for cramps. Whether it signals a miscarriage depends on when it occurs, the severity of the cramping, and whether you're experiencing other symptoms alongside it.

Having surgery can be frightening for anyone, but it's especially scary for kids who don't always understand what's going on, or what the grown-ups are saying. We're here to help!
Join Avrie, who had surgery at the Sacred Heart Children's Hospital pediatric surgery center in Spokane, WA. Maybe after watching and hearing her story, you and your kiddo will feel better about having surgery in the hospital.
Follow Avrie's trip - from check-in, vital signs and pre-op checks; meeting the doctor who will do his surgery, along with the anesthesiologist, surgery nurse and the Child Life Specialist; the trip to the Operating Room; waking up in the recovery room with his mom by his side; and getting ready to go home.
To learn more about the pediatric surgery center at Sacred Heart Children's Hospital, visit https://washington.providence.....org/locations-direct
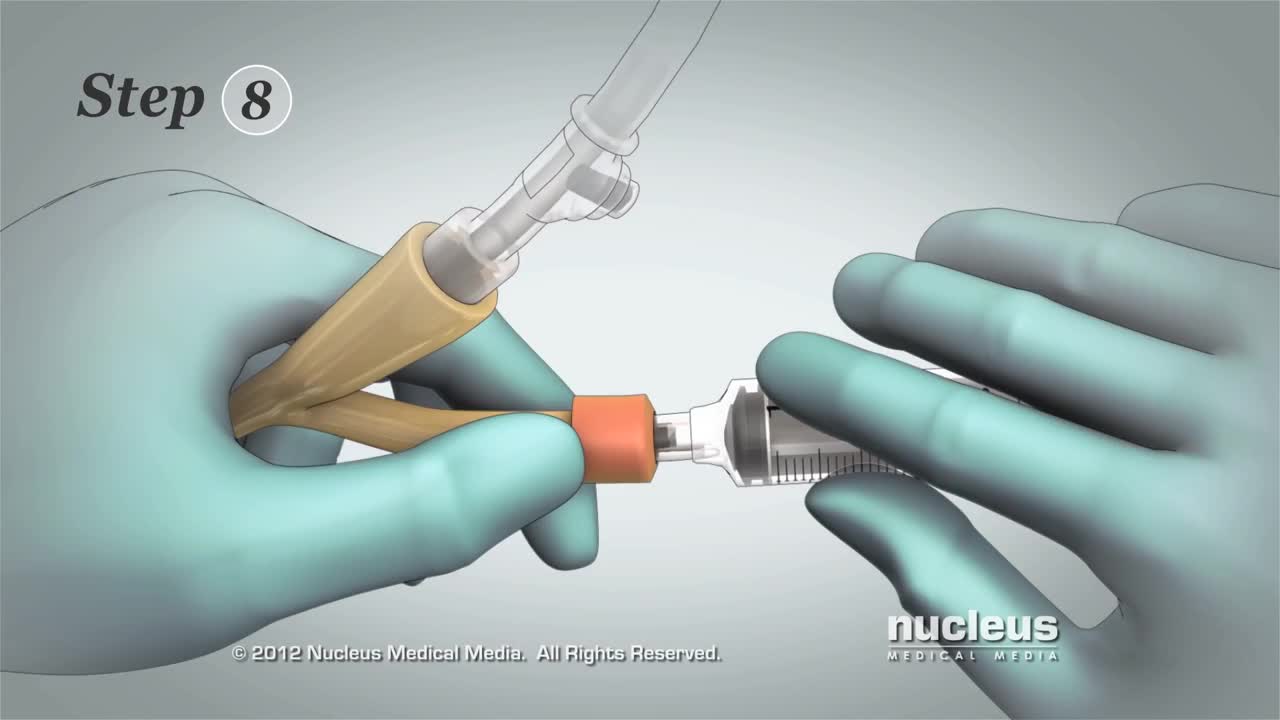
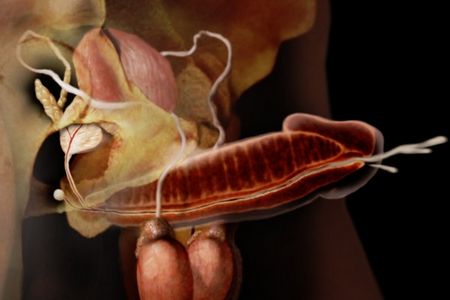
This 3D medical animation contains the discharge instructions for removal of a Foley catheter from a man. The step-by-step procedures for emptying the Foley bag and removing the Foley catheter are shown. Symptoms requiring a follow-up call to the surgeon are listed.

Our mission: Empower you with the tools and support you need for weight loss and live a healthier life. Get started on your weight loss journey today: https://bit.ly/2Ms4JaX
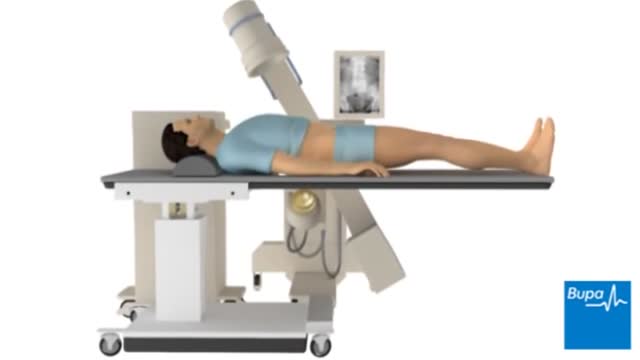
Extracorporeal shock wave lithotripsy (ESWL) uses shock waves to break a kidney stone into small pieces that can more easily travel through the urinary tract camera.gif and pass from the body. See a picture of ESWL camera.gif. You lie on a water-filled cushion, and the surgeon uses X-rays or ultrasound tests to precisely locate the stone. High-energy sound waves pass through your body without injuring it and break the stone into small pieces. These small pieces move through the urinary tract and out of the body more easily than a large stone. The process takes about an hour. You may receive sedatives or local anesthesia. Your surgeon may use a stent if you have a large stone. A stent is a small, short tube of flexible plastic mesh that holds the ureter open. This helps the small stone pieces to pass without blocking the ureter.

This video shows you how to conduct a clinical examination of the foot and how to identify common causes of foot pain.
This video clip is part of the FIFA Diploma in Football Medicine and the FIFA Medical Network. To enrol or to find our more click on the following link http://www.fifamedicalnetwork.com
The Diploma is a free online course designed to help clinicians learn how to diagnose and manage common football-related injuries and illnesses. There are a total of 42 modules created by football medicine experts. Visit a single page, complete individual modules or finish the entire course.
The network provides the opportunity for clinicians around the world to meet and share ideas relating to football medicine. Ask about an interesting case, debate current practice and discuss treatment strategies. Create a profile and log on to interact with other health professionals from around the globe.
This is not medical advice. The content is intended as educational content for health care professionals and students. If you are a patient, seek care of a health care professional.

Atrial fibrillation (also called AFib or AF) is a quivering or irregular heartbeat (arrhythmia) that can lead to blood clots, stroke, heart failure and other heart-related complications. Some people refer to AF as a quivering heart. An estimated 2.7 million Americans are living with AF.