Top videos

This multi award winning video talks about a time of increased demands on our healthcare system and healthcare providers, ensuring that each and every patient and their family members are provided with compassionate care is a massive goal, but one that the staff at the Royal Alexandra Hospital are pursuing every day. Good quality care is always important, but caring for our patients is what they will really remember.

Ellis demonstrates how to perform good hand hygiene with soap and water.
Our Critical Nursing Skills video tutorial series is taught by Ellis Parker MSN, RN-BC, CNE, CHS and intended to help RN and PN nursing students study for your nursing school exams, including the ATI, HESI and NCLEX.
#NCLEX #ClinicalSkills #HandHygiene #HESI #Kaplan #ATI #NursingSchool #NursingStudent #Nurse #RN #PN #Education #LVN #LPN #nurseeducator
00:00 What Is Good Hand Hygiene?
00:27 Prepping to wash hands
01:01 Proper hand washing technique
01:53 How to dry hands
02:14 Proper technique to turn off faucet
🚨 Reminder: shipping deadlines are looming 👀
🎁 Regular Shipping: Order by Friday, December 15
🚀 Expedited Shipping: Order by Monday, December 18
🔍 Still searching for last-minute gifts? Consider a Level Up RN Gift Card! 💌 It’s not only a thoughtful present but also the perfect way to share treasures like Pharmacology Flashcards OR digital treasures like Flashables Digital Nursing Flashcards & the Level Up RN membership. Give the gift of knowledge this holiday season! 🧠⚡️💖 bit.ly/LevelUpRNGC
🚪 Access our Cram Courses, Quizzes and Videos all in one ad free space with Level Up RN Membership https://bit.ly/LevelUpRNMembership
Want more ways to MASTER Clinical Skills? Check out our flashcards & videos!
👇👇👇👇👇👇👇👇👇👇
👉 https://bit.ly/clinicalnursingskills 👈
☝️👆☝️👆☝️👆☝️👆☝️👆
This is your one-stop-shop for materials to help you LEARN & REVIEW so you can PASS Nursing School.
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our resources are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of ⭐️⭐️⭐️⭐️⭐️ reviews from nurses who passed their exams and the NCLEX with Level Up RN.
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
L👀king for EVEN MORE resources to survive Nursing School? Make your Nursing School experience your own! Life’s difficult enough—learning shouldn’t be.
🪅 Games https://nursesquad.com
💻 Digital resources https://bit.ly/NursingStudyCourses
📅 Organizational tools https://bit.ly/OrganizingSchool
✨Want perks? Join our channel!
https://youtube.com/leveluprn/join
🏷 Head to https://leveluprn.com/specials for all our latest deals!🥳️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://leveluprn.com/signup ⬅️
⚕ 👩 LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.00:00 Good Hand Hygiene?

I talk about 5 Essential Skills you need as a nurse. These skills are timeless in the fat that you will always need to use them at some level. Of course specific skills are good to have as well but these skills are universal and can help you in other areas of life as well.
NURSING SCHOOL STUDY RESOURCES: https://sellfy.com/nursingschoolstudyNURSING
PHARMACOLOGY: https://sellfy.com/p/fnoy/
INSTAGRAM:https://www.instagram.com/your_mentor_rn/?hl=en
PERSONAL INSTAGRAM: https://www.instagram.com/crosby_steen/
MEDIUM ARTICLES: https://medium.com/@rnacademy1..../7-tips-for-nursing-
AMAZON PRIME STUDENT DISCOUNT: https://amzn.to/2OIleAe
VIDEO GEAR
Camera: G7X Markii - https://amzn.to/2na3OR8
Phone: Galaxy Note 8- https://amzn.to/2nboHM3
Audio: Zoom H4NPro Audio Recorder- https://amzn.to/2vktlf8
Computer: 13 inch Macbook Pro- https://amzn.to/2ndhISw
INSTAGRAM TV https://www.instagram.com/crosby_steen/
Hi Guys! My name is Crosby Steen. I am a Nursing Educator, and ER Travel Nurse. I do videos on daily science based news and travel, with the goal of providing value for you in science based education and travel nursing. Any questions hit me up in the comments or Email below.....
PRIVATE TUTORING OR VIDEO REQUESTS CONTACT:
crosby.steen@gmail.com
MUSIC BY: https://andrewapplepie.com/ and copyrighted by Epidemic Sound
Music by Joakim Karud http://youtube.com/joakimkarud
Music by DJ Quads
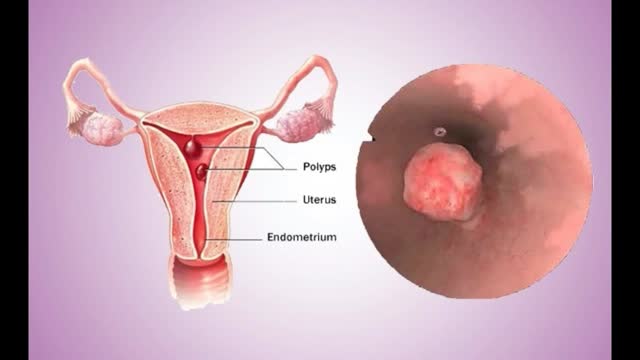
Uterine polyps are growths attached to the inner wall of the uterus that extend into the uterine cavity. Overgrowth of cells in the lining of the uterus (endometrium) leads to the formation of uterine polyps, also known as endometrial polyps. These polyps are usually noncancerous (benign), although some can be cancerous or can eventually turn into cancer (precancerous polyps). Uterine polyps range in size from a few millimeters — no larger than a sesame seed — to several centimeters — golf-ball-size or larger. They attach to the uterine wall by a large base or a thin stalk.
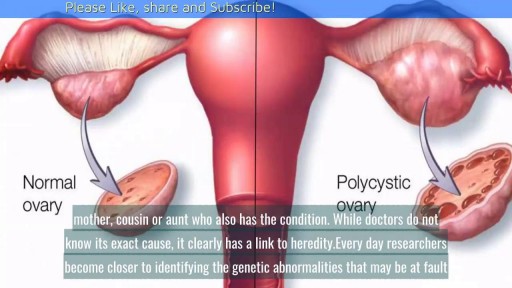
Causes of Polycystic Ovarian Syndrome|| Common gynaecological problems in women Polycystic ovarian syndrome, or PCOS, is a condition where a woman's ovaries and adrenal glands produce more androgens than normal, resulting in increased body hair, acne and irregular periods. While researchers are not certain of the exact cause of PCOS, it is known that an imbalance of the endocrine system is responsible for many of the changes associated with it. However, it is still not known exactly what causes those changes.
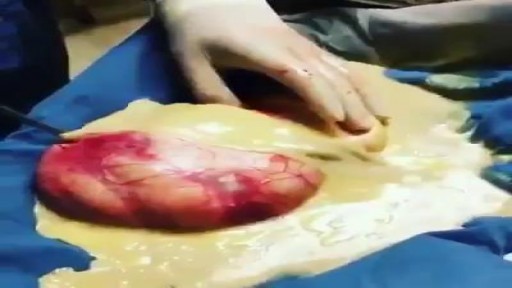
Teratomas are tumors made up of tissues, such as hair, muscle, and bone. They occur most often in the ovaries in women, and the testicles in men. They may be benign or malignant. Symptoms vary depending on the location. A painful lump or swelling may be apparent. Some babies have a mass that can be seen on an ultrasound before birth. Treatment often involves surgery. In rare cases when a teratoma is malignant, chemotherapy or radiation may be needed.
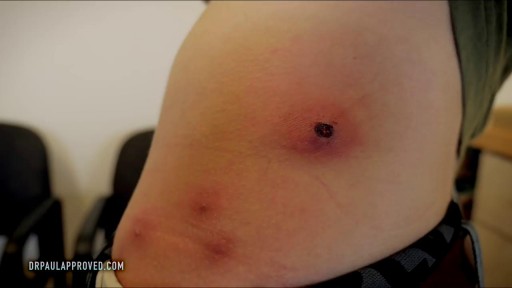
Are most spiders poisonous? The majority of the 3,000 spiders in the United States aren’t poisonous. Even if most spiders did bite, their fangs are too small or weak to puncture human skin. Their bites may leave itchy, red wounds that heal within a week or so. The spiders that do manage to bite through our skin and insert toxic venom can cause serious health complications. Read on to learn what spider bites look like, what spider varieties leave certain bites, and how to treat spider bites. What do spider bites look like? Identifying a spider bite is easier if you saw the spider that bit you, but it’s possible that you won’t notice the wound until hours later. Look for things like: swelling a red welt skin damage any troubling symptoms that accompany the bite Other possible symptoms that may accompany a spider bite include: itching or rash pain around the area of the bite muscle pain or cramping blister that’s red or purple in color sweating difficulty breathing headache nausea and vomiting fever chills anxiety or restlessness rashes swollen lymph glands high blood pressure Spider bites often take longer to heal than other insect bites, and they may affect skin tissues. It’s important to keep the bite clean to reduce the risk of infection. How to treat a spider bite at home In some cases, you can treat spider bites at home. For nonvenomous spider bites, follow these steps: Apply an ice pack on and off the bite for 10 minutes at a time. Elevate the area to reduce swelling. Take an antihistamine, such as diphenhydramine (Benadryl), to help with itching. Clean the area with soap and water to prevent infection. Apply antibiotic ointment to the area if blisters develop. Seek medical attention if you’re showing symptoms of a spider bite or if the symptoms don’t go away over time. Always seek medical attention if you suspect you’ve been bitten by one of the following species: brown recluse black widow hobo spider tarantula Brazilian wandering spider

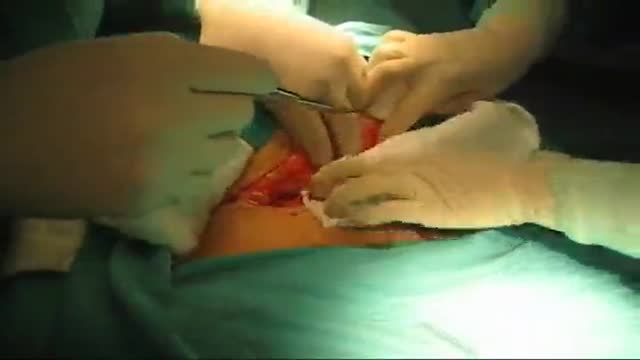
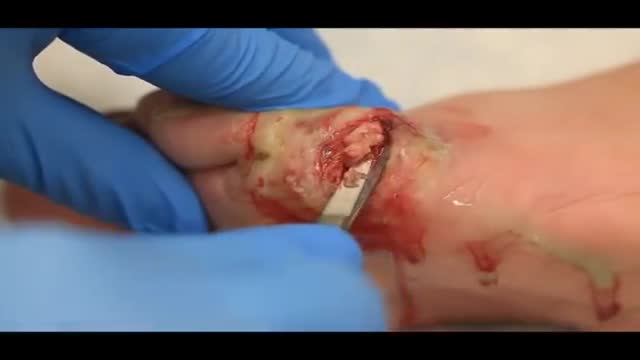
LIS Closed done at 5 O clock position, using Scalpel blade 15. After feeling the groove between internal and external anal sphincter, the blade is passed in and the lower 1/2 of Internal anal sphincter is cut. Remain below dentate line. If anal mucosa is accidently cut suture with 4-0 rapid vicryl. In event of bleeding, pinchcock for 5 minutes.
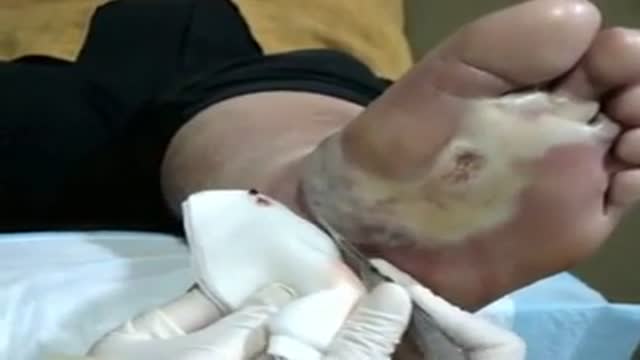
Treatment may not be needed for an eschar if it is part of the natural healing process. However, if an eschar looks like it may have a wound infection – symptoms can include oozing fluid such as pus or blood, your clinician will likely recommend topical treatment or debridement to help control and remove the infection.