Top videos

Morning erections have colloquially been termed as “morning wood” while scientifically it is called nocturnal penile tumescence. It is a normal and healthy physiological reaction and response that most men experience in their lives. Morning erections are really the ending of a series of erections that happen to men during the night. Healthy men can, on average, have anywhere between three to five erections in a full night of sleep, each of which lasts from 25-35 minutes.

The Epley Maneuver for Vertigo can be very effective at relieving vertigo symptoms, but it’s a procedure that should be performed by a physical therapist or other health care professional. This video is for demonstration purposes only. See Doctor Jo’s blog post about the Epley

Cancer starts when cells in a part of the body begins to grow out of control and can spread to other areas of the body. There are many kinds of cancer. Cells in nearly any part of the body can become cancer. To learn more about how cancers start and spread, see What Is Cancer? Leukemias are cancers that start in cells that would normally develop into different types of blood cells. Here we will talk about acute myeloid leukemia (AML). Acute myeloid leukemia (AML) has many other names, including acute myelocytic leukemia, acute myelogenous leukemia, acute granulocytic leukemia, and acute non-lymphocytic leukemia. “Acute” means that this leukemia can progress quickly if not treated, and would probably be fatal in a few months. “Myeloid” refers to the type of cell this leukemia starts from. Most cases of AML develop from cells that would turn into white blood cells (other than lymphocytes), but some cases of AML develop in other types of blood-forming cells. The different types of AML are listed in “ How is acute myeloid leukemia classified?” AML starts in the bone marrow (the soft inner part of certain bones, where new blood cells are made), but in most cases it quickly moves into the blood. It can sometimes spread to other parts of the body including the lymph nodes, liver, spleen, central nervous system (brain and spinal cord), and testicles. Other types of cancer can start in these organs and then spread to the bone marrow. But these cancers that start elsewhere and then spread to the bone marrow are not leukemias. Normal bone marrow, blood, and lymphoid tissue To understand the different types of leukemia, it helps to know about the blood and lymph systems.

In this video a real case of the extremely rare disease "Fibrodysplasia ossificans progressiva" or what is called the "FOP" This disease is commonly misdiagnosed and usually end up by unnecessary surgery which exaggerate the disease. Children born with FOP characteristically have deformed great toes, possibly missing a joint or simply presenting with a notable lump at the minor joint. The first "flare-up" that leads to the formation of FOP bones usually occurs before the age of 10. FOP is a genetic disease. The bone growth progresses from the top downward, just as bones grow in fetuses. A child with FOP will typically develop bones starting at the neck, then on the shoulders, arms, chest area and finally on the feet. However it does not necessarily occur in this order due to injury-caused flare-ups. Often, the tumor-like lumps that characterize the disease appear suddenly. The gene that causes ossification is normally deactivated after a fetus' bones are formed in the womb, but in patients with FOP, the gene keeps working. Aberrant bone formation in patients with FOP occurs when injured connective tissue or muscle cells at the sites of injury or growth incorrectly express an enzyme for bone repair during apoptosis (self-regulated cell death), resulting in lymphocytes containing excess bone morphogenetic protein 4 (BMP4) provided during the immune system response. Since the incorrect enzyme remains unresolved within the immune response, the body continues providing the incorrect BMP4-containing lymphocytes. BMP4 is a product that contributes to the development of the skeleton in the normal embryo.
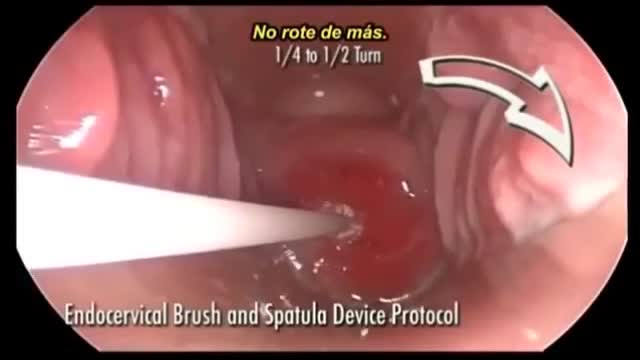
In patients age ;::25, HPV DNA testing is the preferred next step in management if the initial cytology shows ASC-US. In this method, samples are collected for both cytology and reflex HPV DNA. If cytology results are positive, HPV DNA testing is performed. If cytology results are negative, the sample for HPV DNA is discarded. HPV DNA testing along with Pap smear at 3 years is recommended if initial cytology shows ASC-US but HPV DNA testing is negative

Men need to know that breast cancer is not limited to women. Possible symptoms of breast cancer to watch for include: A lump or swelling, which is usually (but not always) painless Skin dimpling or puckering Nipple retraction (turning inward) Redness or scaling of the nipple or breast skin Discharge from the nipple Sometimes a breast cancer can spread to lymph nodes under the arm or around the collar bone and cause a lump or swelling there, even before the original tumor in the breast tissue is large enough to be felt. These changes aren't always caused by cancer. For example, most breast lumps in men are caused by gynecomastia (a harmless enlargement of breast tissue). Still, if you notice any breast changes, you should see a health care professional as soon as possible.
How do you know if you have pneumonia? They may include: Cough. You will likely cough up mucus (sputum) from your lungs. ... Fever. Fast breathing and feeling short of breath. Shaking and "teeth-chattering" chills. Chest pain that often feels worse when you cough or breathe in. Fast heartbeat. Feeling very tired or very weak. Nausea and vomiting.

Renal artery stenosis is the narrowing of one or more arteries that carry blood to your kidneys (renal arteries). Narrowing of the arteries prevents normal amounts of oxygen-rich blood from reaching your kidneys. Your kidneys need adequate blood flow to help filter waste products and remove excess fluids. Reduced blood flow may increase blood pressure in your whole body (systemic blood pressure) and injure kidney tissue.