Top videos

Shut the front door: Scientists have finally found the perfect breasts. No, they weren't hiding in the Amazon or roving solo across the Sahara (although we have no doubt there are women in both the Amazon and the Sahara who have magnificent mammaries); it turns out these perfect breasts were hiding in a plastic surgeon's office this whole time! Now, before you get all worked up, the American Society of Plastic Surgeons (ASPS) would like you to know that the super-fake looking plastic breasts of yore are not actually what people think are most attractive now. According to a study published in the Journal of Plastic and Reconstructive Surgery—which involved asking over 1,300 people to look at pictures of naked boobies and rank them by hotness (stop laughing, this is serious research!)—people preferred a more "real" and "normal" look from their silicone, with the ideal breast shape having a 45:55 ratio. People said the best chests have 45 percent of the fullness above the nipple line and 55 percent of the fullness below, in a slightly teardrop shape. Researchers noted this preference remained consistent across gender, racial, and ethnic groups with the 45:55 ratio favored by 87 percent of women in their 30s, 90 percent of men, and 94 percent of plastic surgeons.
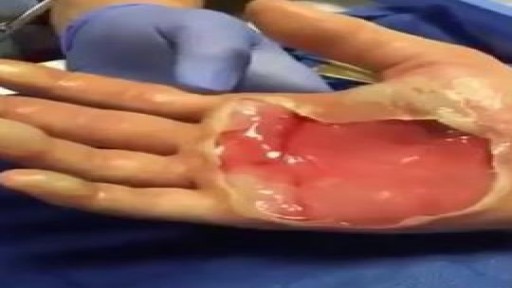
What is a mole? Many people refer to a mole as any dark spot or irregularity in the skin. Doctors use different terms. But the following types of skin marks such as these are not treated the same way moles are and are not discussed here: Birthmarks Abnormal formations of blood vessels (hemangiomas) Keratoses (benign or precancerous spots, which appear after about age 30 years)
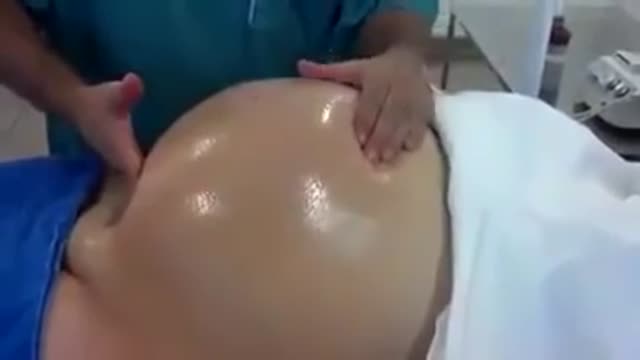
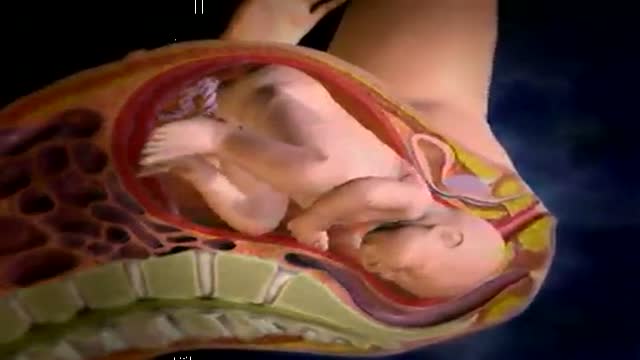
The baby will move head down if there is room or if there is tone in the support to the uterus to direct baby head down. Before 24-26 weeks most babies lie diagonal or sideways in the Transverse Lie position. Between 24-29 weeks most babies turn vertical and some will be breech.

A new well designed randomized study has suggested that long term baby aspirin usage may aid in fight against cancer. The suggested mechanism is that cancers induce inflammatory responses so the anti-inflammatory mechanism of prostaglandins inhibitors may cease the progress of many cancers. There are some concerns about the study because despite the well-designed randomized study; the study didn't include a satisfying number of female participants. The study was also conducted on esophageal, colorectal and lung cancers.

Warren Pettaway of Detroit knew he needed to have his left knee checked out when he could no longer keep up while officiating basketball. The pain got so bad that running up and down the court or quickly changing directions was too much for him to continue doing what he loved.Only three weeks post-surgery, Warren is ready to get back in the game. He is able to move without issue and is getting things done around the house. He makes sure to do his therapy as directed and is exercising on his own in the gym. To learn more visit https://www.henryford.com/serv....ices/joint-replaceme
Identify the anatomy and explain the physiology of the breast on diagrams and sonograms.
Describe and demonstrate the protocol for sonographic scanning of the breast, including the clock and quadrant methods, and targeted examinations based on mammographic findings.
Describe the various diagnostic pathways that may lead to a sonographic breast examination, and explain how the ultrasound findings are correlated with other imaging modalities.
Identify and describe sonographic images of benign and malignant features and common breast pathologies.
Explain biopsy techniques for breast tumors.
Define and use related medical terminology.
Explain the Patient Privacy Rule (HIPAA) and Patient Safety Act (see reference

Breast reconstruction 3D Animation
on Friday, December 17, 2010
The primary part of the procedure can often be carried out immediately following the mastectomy. As with many other surgeries, patients with significant medical comorbidities (high blood pressure, obesity, diabetes) and smokers are higher-risk candidates. Surgeons may choose to perform delayed reconstruction to decrease this risk. Patients expected to receive external beam radiation as part of their adjuvant treatment are also commonly considered for delayed autologous reconstruction due to significantly higher complication rates with tissue expander-implant techniques in those patients. Breast reconstruction is a large undertaking that usually takes multiple operations. Sometimes these follow-up surgeries are spread out over weeks or months. If an implant is used, the individual runs the same risks and complications as those who use them for breast augmentation but has higher rates of capsular contracture (tightening or hardening of the scar tissue around the implant) and revisional surgeries. Outcomes based research on quality of life improvements and psychosocial benefits associated with breast reconstruction served as the stimulus in the United States for the 1998 Women's Health and Cancer Rights Act which mandated health care payer coverage for breast and nipple reconstruction, contralateral procedures to achieve symmetry, and treatment for the sequelae of mastectomy. This was followed in 2001 by additional legislation imposing penalties on noncompliant insurers. Similar provisions for coverage exist in most countries worldwide through national health care programs. There are many methods for breast reconstruction. The two most common are: * Tissue Expander - Breast implants This is the most common technique used in worldwide. The surgeon inserts a tissue expander, a temporary silastic implant, beneath a pocket under the pectoralis major muscle of the chest wall. The pectoral muscles may be released along its inferior edge to allow a larger, more supple pocket for the expander at the expense of thinner lower pole soft tissue coverage. The use of acellular human or animal dermal grafts have been described as an onlay patch to increase coverage of the implant when the pectoral muscle is released, which purports to improve both functional and aesthtic outcomes of implant-expander breast reconstruction. o In a process that can take weeks or months, saline solution is percutaneously injected to progressively expand the overlaying tissue. Once the expander has reached an acceptable size, it may be removed and replaced with a more permanent implant. Reconstruction of the areola and nipple are usually performed in a separate operation after the skin has stretched to its final size. * Flap reconstruction The second most common procedure uses tissue from other parts of the patient's body, such as the back, buttocks, thigh or abdomen. This procedure may be performed by leaving the donor tissue connected to the original site to retain its blood supply (the vessels are tunnelled beneath the skin surface to the new site) or it may be cut off and new blood supply may be connected. o The latissimus dorsi muscle flap is the donor tissue available on the back. It is a large flat muscle which can be employed without significant loss of function. It can be moved into the breast defect still attached to its blood supply under the arm pit (axilla). A latissimus flap is usually used to recruit soft-tissue coverage over an underlying implant. Enough volume can be recruited occasionally to reconstruct small breasts without an implant. o Abdominal flaps The abdominal flap for breast reconstruction is the TRAM flap or its technically distinct variants of microvascular "perforator flaps" like the DIEP/SIEP flaps. Both use the abdominal tissue between the umbilicus and the

The pain is frequently severe and is described as throbbing or pulsating. Nausea is common, and many migraine patients have a watering eye, a running nose, or congestion. If these symptoms are prominent, they may lead to a misdiagnosis of sinus headaches.