Top videos

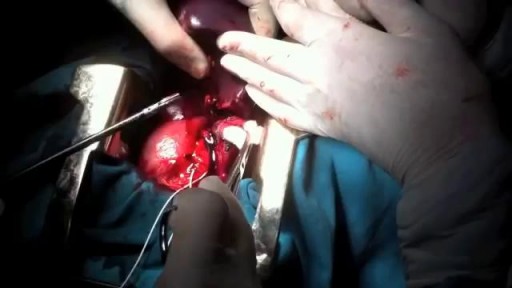
Rare condition disorder known as Diprosopus, also known as craniofacial duplication. Diprosopus is a congenital defect also known as craniofacial duplication. The exact description of diprosopus refers to a fetus with a single trunk, normal limbs, and facial features that are duplicated to a certain degree. A less severe instance is when the fetus has a duplicated nose and the eyes are spaced far apart. In the most extreme instances, the entire face is duplicated, hence the name diprosopus, which is Greek for two-faced. Fetuses with diprosopus often also lack brains (anencephaly), have neural tube defects, or heart malformations. In some cases, if the brain is formed, it may have duplicated structures. Most infants with diprosopus are stillborn and there are fewer than fifty cases documented since 1864.
Identify the anatomy and explain the physiology of the breast on diagrams and sonograms.
Describe and demonstrate the protocol for sonographic scanning of the breast, including the clock and quadrant methods, and targeted examinations based on mammographic findings.
Describe the various diagnostic pathways that may lead to a sonographic breast examination, and explain how the ultrasound findings are correlated with other imaging modalities.
Identify and describe sonographic images of benign and malignant features and common breast pathologies.
Explain biopsy techniques for breast tumors.
Define and use related medical terminology.
Explain the Patient Privacy Rule (HIPAA) and Patient Safety Act (see reference

Breast reconstruction 3D Animation
on Friday, December 17, 2010
The primary part of the procedure can often be carried out immediately following the mastectomy. As with many other surgeries, patients with significant medical comorbidities (high blood pressure, obesity, diabetes) and smokers are higher-risk candidates. Surgeons may choose to perform delayed reconstruction to decrease this risk. Patients expected to receive external beam radiation as part of their adjuvant treatment are also commonly considered for delayed autologous reconstruction due to significantly higher complication rates with tissue expander-implant techniques in those patients. Breast reconstruction is a large undertaking that usually takes multiple operations. Sometimes these follow-up surgeries are spread out over weeks or months. If an implant is used, the individual runs the same risks and complications as those who use them for breast augmentation but has higher rates of capsular contracture (tightening or hardening of the scar tissue around the implant) and revisional surgeries. Outcomes based research on quality of life improvements and psychosocial benefits associated with breast reconstruction served as the stimulus in the United States for the 1998 Women's Health and Cancer Rights Act which mandated health care payer coverage for breast and nipple reconstruction, contralateral procedures to achieve symmetry, and treatment for the sequelae of mastectomy. This was followed in 2001 by additional legislation imposing penalties on noncompliant insurers. Similar provisions for coverage exist in most countries worldwide through national health care programs. There are many methods for breast reconstruction. The two most common are: * Tissue Expander - Breast implants This is the most common technique used in worldwide. The surgeon inserts a tissue expander, a temporary silastic implant, beneath a pocket under the pectoralis major muscle of the chest wall. The pectoral muscles may be released along its inferior edge to allow a larger, more supple pocket for the expander at the expense of thinner lower pole soft tissue coverage. The use of acellular human or animal dermal grafts have been described as an onlay patch to increase coverage of the implant when the pectoral muscle is released, which purports to improve both functional and aesthtic outcomes of implant-expander breast reconstruction. o In a process that can take weeks or months, saline solution is percutaneously injected to progressively expand the overlaying tissue. Once the expander has reached an acceptable size, it may be removed and replaced with a more permanent implant. Reconstruction of the areola and nipple are usually performed in a separate operation after the skin has stretched to its final size. * Flap reconstruction The second most common procedure uses tissue from other parts of the patient's body, such as the back, buttocks, thigh or abdomen. This procedure may be performed by leaving the donor tissue connected to the original site to retain its blood supply (the vessels are tunnelled beneath the skin surface to the new site) or it may be cut off and new blood supply may be connected. o The latissimus dorsi muscle flap is the donor tissue available on the back. It is a large flat muscle which can be employed without significant loss of function. It can be moved into the breast defect still attached to its blood supply under the arm pit (axilla). A latissimus flap is usually used to recruit soft-tissue coverage over an underlying implant. Enough volume can be recruited occasionally to reconstruct small breasts without an implant. o Abdominal flaps The abdominal flap for breast reconstruction is the TRAM flap or its technically distinct variants of microvascular "perforator flaps" like the DIEP/SIEP flaps. Both use the abdominal tissue between the umbilicus and the

Ejaculating into a partner’s mouth is a common practice during oral sex/fellatio. In a safe situation (where there is no danger of catching an STD), the semen-receiving partner may choose to spit the semen out, or to swallow it. Before you engage in fellatio, I’d recommend that you and your partner both get tested for sexually transmitted infections (STIs). If not, please use barriers for oral sex and abstaining from making contact with ejaculate. Semen is mostly water, but also contains amino acids and protein, sugars such as fructose and glucose, minerals such as zinc and calcium, vitamin C, and a few other nutrients. Sperm cells themselves make up less than one percent of semen. Semen is edible, and if swallowed, will travel down the esophagus and into the stomach, where it will be digested in the same way that food is. You can never get pregnant by swallowing semen. Some people accept the taste of semen, but others complain that swallowing semen can give them an upset stomach. In rare cases, you may have an allergy to the proteins found in semen. What does It Taste Like? The taste of semen varies. Bitter, sweet, metallic. So, one may expect to find the taste of semen anywhere from enjoyable to tasteless to disgusting. But there is a way of controlling the taste of semen, which is through diet. Keep track of the diet, and communicate with the partner about when it tastes better or worse.

In most cases, your body's immune system defeats an HPV infection before it creates warts. When warts do appear, they vary in appearance depending on which variety of HPV is involved: Genital warts. These appear as flat lesions, small cauliflower-like bumps or tiny stem-like protrusions. In women, genital warts appear mostly on the vulva but can also occur near the anus, on the cervix or in the vagina. In men, genital warts appear on the penis and scrotum or around the anus. Genital warts rarely cause discomfort or pain, though they may itch. Common warts. Common warts appear as rough, raised bumps and usually occur on the hands, fingers or elbows. In most cases, common warts are simply unsightly, but they can also be painful or susceptible to injury or bleeding.

UPDATE 2/6/15: A new version of this animation is now available! https://www.youtube.com/watch?v=E1ljClS0DhM
This 3D medical animation depicts the surgical removal of the appendix (appendectomy) using laparoscopic instruments. The surgery animation begins by showing an inflamed appendix (appendicitis), followed by the placement of the laparoscope. Afterward, one can see the surgical device staple, cut and remove the inflamed appendix. Following the removal of the appendix the abdomen is flushed with a sterile saline solution to ensure all traces of infection have been removed.
ANCE00183

If you look at someone’s back, you’ll see that the spine runs straight down the middle. When a person has scoliosis, their backbone curves to the side. The angle of the curve may be small, large or somewhere in between. But anything that measures more than 10 degrees is considered scoliosis. Doctors may use the letters “C” and “S” to describe the curve of the backbone. You probably don’t look directly at too many spines, but what you might notice about someone with scoliosis is the way they stand. They may lean a little or have shoulders or hips that look uneven. What Causes Scoliosis? In as many as 80% of cases, doctors don’t find the exact reason for a curved spine. Scoliosis without a known cause is what doctors call “idiopathic.” Some kinds of scoliosis do have clear causes. Doctors divide those curves into two types -- structural and nonstructural. In nonstructural scoliosis, the spine works normally, but looks curved. Why does this happen? There are a number of reasons, such as one leg’s being longer than the other, muscle spasms, and inflammations like appendicitis. When these problems are treated, this type of scoliosis often goes away. In structural scoliosis, the curve of the spine is rigid and can’t be reversed
Thigh pain is most often caused by injuries to bones, joints, muscles, tendons, ligaments, and other soft tissues or blood vessels. These injuries are often caused during sports competition, or strain from overuse, obesity, or pregnancy.