Top videos

What are the disadvantages of male condoms? a moderately high failure rate when used improperly or inconsistently. the potential for diminished sensation. skin irritation, such as contact dermatitis, due to latex sensitivity or allergy. allergic reactions to spermicides, lubes, scents, and other chemicals in the condoms.
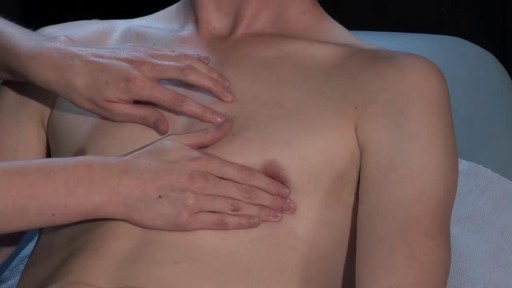
The major elements of the cardiac exam include observation, palpation and, most importantly, auscultation (percussion is omitted). As with all other areas of the physical exam, establishing adequate exposure and a quiet environment are critical. Initially, the patient should rest supine with the upper body elevated 30 to 45 degrees. Most exam tables have an adjustable top. If not, use 2 or 3 pillows. Remember that although assessment of pulse and blood pressure are discussed in the vital signs section they are actually important elements of the cardiac exam.
Heavy period blood can be especially alarming if it contains clots. In most cases, though, red, brown, or even black menstrual blood clots are normal—just bits of the endometrium (the lining of the uterus) that are shed during menstruation.

A flail chest occurs when a segment of the thoracic cage is separated from the rest of the chest wall. This is usually defined as at least two fractures per rib (producing a free segment), in at least two ribs. A segment of the chest wall that is flail is unable to contribute to lung expansion. Large flail segments will involve a much greater proportion of the chest wall and may extend bilaterally or involve the sternum. In these cases the disruption of normal pulmonary mechanics may be large enough to require mechanical ventilation.
Ever considered getting laser eye surgery, but didn’t know how it worked? Allow us to help!
There are three different main types of laser eye surgery: LASIK, SMILE, and Surface Laser Treatments, and each can be explained pretty easily.
LASIK uses two lasers to open up a thin flap on the surface of the cornea, and then reshapes the cornea underneath. The flap is then placed back over the reshaped cornea, and heals independently with time.
SMILE uses one laser to reshape the cornea through a small, self-healing hole.
And Surface Eye Treatments remove the clear skin over the eye, to then reshape the cornea underneath with - you guessed it - a laser!
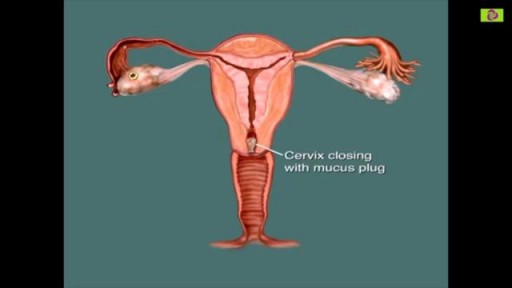
You are most fertile at the time of ovulation, (when an egg is released from your ovaries) which usually occurs 12-14 days before your next period starts. This is the time of the month when you are most likely to get pregnant. It is unlikely that you will get pregnant just after your period, although it can happen.

-Tibial stress fractures are common in athletes and nonathletes who suddenly increase their physical activity. Clinical features include pain, localized tenderness, and swelling. Plain x-ray is <50% sensitive for stress fractures, especially in the first 2-3 weeks after the onset of symptoms. MRI is preferred over bone scan or ultrasound as it can show the fracture line that extends through the cortex into the medullary line. MRI can also identify ligament, muscle, and cartilage injuries. However, MRI findings may be persistently abnormal for up to 1 year after the stress fracture has healed.

The Combitube is a twin lumen device designed for use in emergency situations and difficult airways. It can be inserted without the need for visualization into the oropharynx, and usually enters the esophagus. It has a low volume inflatable distal cuff and a much larger proximal cuff designed to occlude the oro- and nasopharynx.
If the tube has entered the trachea, ventilation is achieved through the distal lumen as with a standard ETT. More commonly the device enters the esophagus and ventilation is achieved through multiple proximal apertures situated above the distal cuff. In the latter case the proximal and distal cuffs have to be inflated to prevent air from escaping through the esophagus or back out of the oro- and nasopharynx.