Top videos

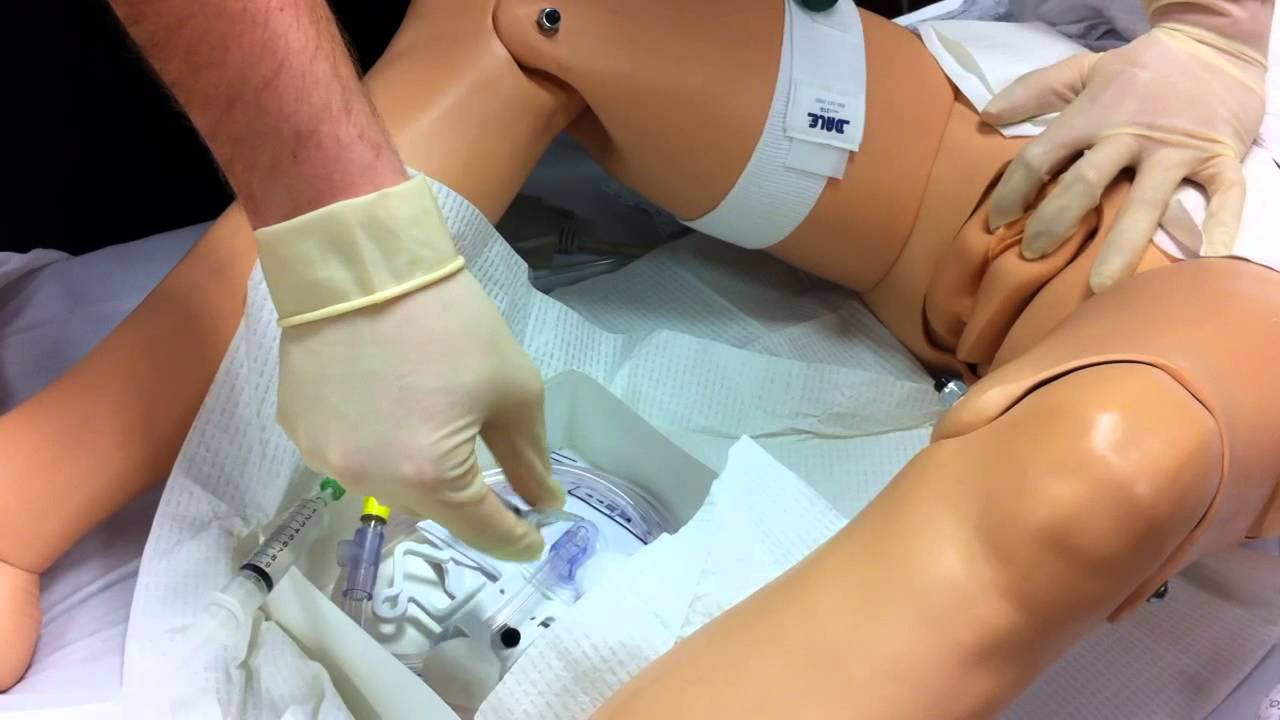
During the examination, the doctor gently puts a lubricated, gloved finger of one hand into the rectum. He or she may use the other hand to press on the lower belly or pelvic area. A digital rectal exam is done for men as part of a complete physical examination to check the prostate gland .
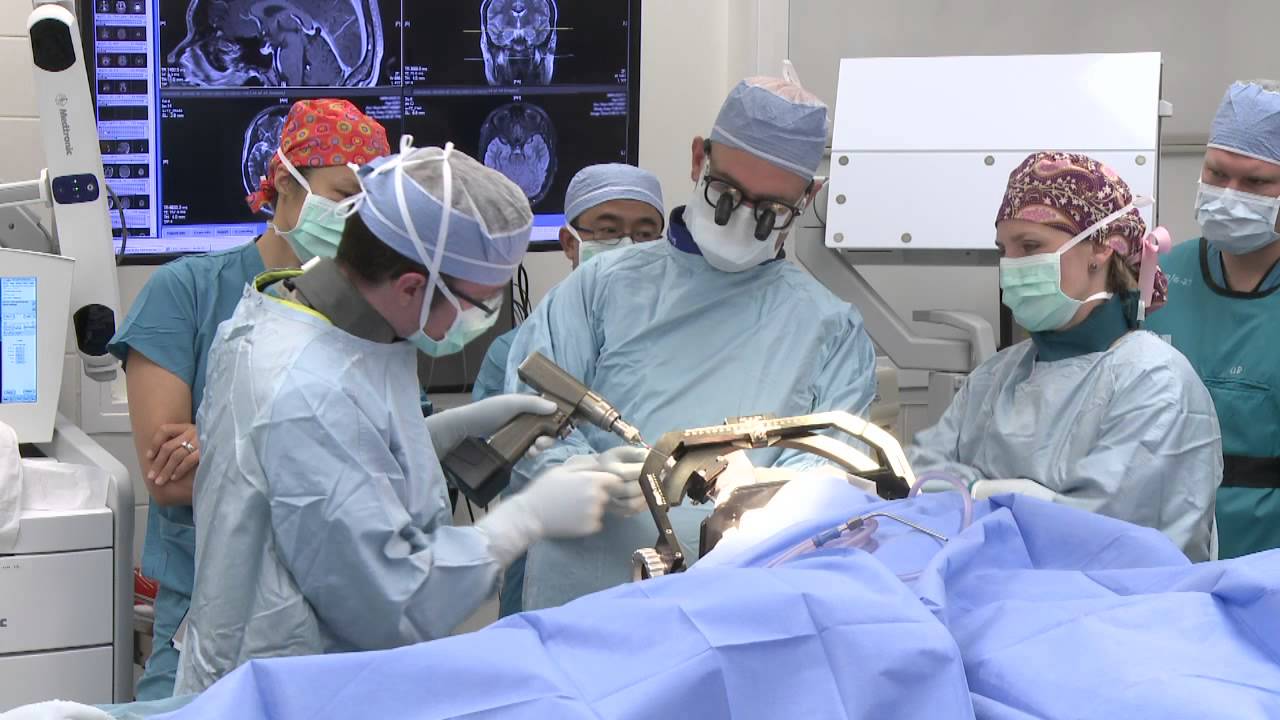
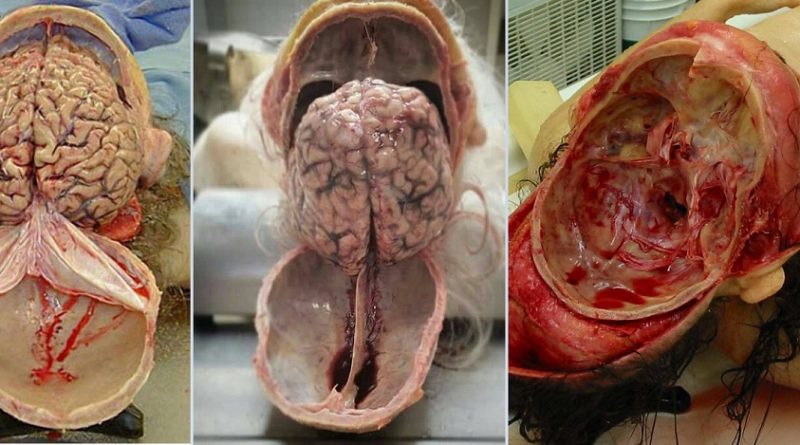
Dr. Jeffrey Ojemann, director of epilepsy surgery at Seattle Children's Hospital, explains a cutting-edge treatment for epilepsy: minimally invasive MRI-guided laser ablation surgery. Laser ablation surgery is much safer and more precise than other treatments, with fewer side effects.
A special thanks to patient Keoni Giauque.
For more information, visit: http://www.seattlechildrens.or....g/clinics-programs/n
"One Last Look" music rights via RoyaltyFreeMusic.com

Lupus is an autoimmune disease that can affect almost any part of your body, most often your joints, skin, kidneys, heart, lungs, blood, or brain. Your two kidneys are part of your renal system, which also includes two ureters, the bladder, and the urethra. As the primary organs of the renal system, your kidneys are responsible for: Maintaining the correct amount and type of body fluids Removing waste products and toxic substances Regulating the hormones (chemical messengers) that help control blood pressure and blood volume

Watch as Dr. Diaz performs a tummy tuck procedure on one of our patients!
A tummy tuck, also known as abdominoplasty, removes excess fat and skin and restores weakened muscles to create a smoother, firmer abdominal profile.
This patient as well wanted to receive liposuction in conjunction with the abdominoplasty. Liposuction sometimes referred to as "lipo" by patients, slims and reshapes specific areas of the body by removing excess fat deposits and improving your body contours and proportions.
The recovery time for a tummy tuck ranges anywhere from two to six weeks. The amount of recovery time you need depends on several factors of your surgery.
If you're interested in a consultation, contact us today! 424.235.6608
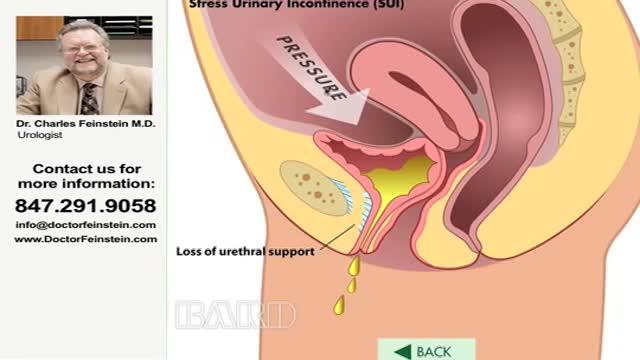
Urinary incontinence — the loss of bladder control — is a common and often embarrassing problem. The severity ranges from occasionally leaking urine when you cough or sneeze to having an urge to urinate that's so sudden and strong you don't get to a toilet in time. If urinary incontinence affects your daily activities, don't hesitate to see your doctor. For most people, simple lifestyle changes or medical treatment can ease discomfort or stop urinary incontinence
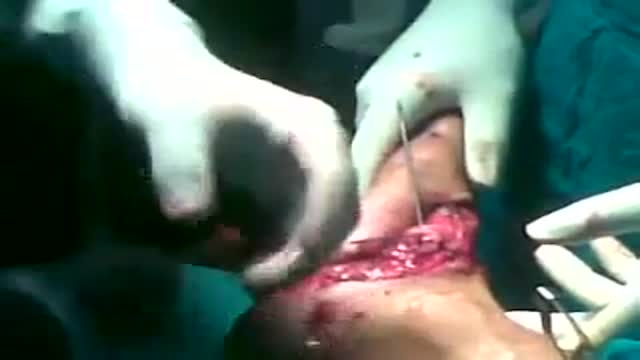
Kirschner wires or K-wires or pins are sterilized, sharpened, smooth stainless steel pins. Introduced in 1909 by Martin Kirschner, the wires are now widely used in orthopaedics and other types of medical and veterinary surgery. They come in different sizes and are used to hold bone fragments together (pin fixation) or to provide an anchor for skeletal traction. The pins are often driven into the bone through the skin (percutaneous pin fixation) using a power or hand drill. They also form part of the Ilizarov apparatus.

How To Deal With Anxiety, How To Not Be Depressed, Natural Remedies For Anxiety, Help For Depression---- http://depression-help.info-pro.co --- Treatments for Depression, Depression is a mental disorder which affects about 350 million people worldwide. Its symptoms include, but are not limited to; Feelings of helplessness and hopelessness. loss of interest in daily activities, appetite or weight changes, insomnia or oversleeping, anger or irritability, loss of energy. self-loathing, reckless behavior, concentration problems, unexplained aches and pains and also suicidal thoughts. Current popular treatments for depression include antidepressant medications and talk therapy such as counselling or psychotherapy. Unfortunately, these treatments have many drawbacks. AD medication is associated with a high risk of side effects and a low success rate, while therapy sessions are notoriously expensive. And often unaffordable or unobtainable for most people. Medical Treatments. Medication for depression comes in the form of antidepressants. There are typically 4 classes of AD medication, SSRIs (selective serotonin reuptake inhibitors), atypical antidepressants, tricyclics antidepressants and MAOIs (monoamine oxidase inhibitors). step-by-step guide on exactly what you need to do to naturally and safely cure your depression in just a few weeks - without any medication or expensive therapy sessions. For more information. click here. http://depression-help.info-pro.co

Erectile dysfunction (ED) is the inability to get or keep an erection firm enough for sexual function. It’s a common sexual problem, affecting as many as 30 million men in the United States. Most cases of ED have a physical cause, such as heart disease, diabetes, and obesity. Lifestyle choices like smoking and drinking excessive amounts of alcohol can also lead to ED. But for some men, psychological issues are the root of the problem.

#tummytucksurgery #tummytuckcost #tummytuckresult #drprashantyadav #dezireclinicindia #cosmeticsurgery #plasticsurgery #weightloss #tummytuck #abdominoplasty
Tummy tuck surgery | Weight Loss
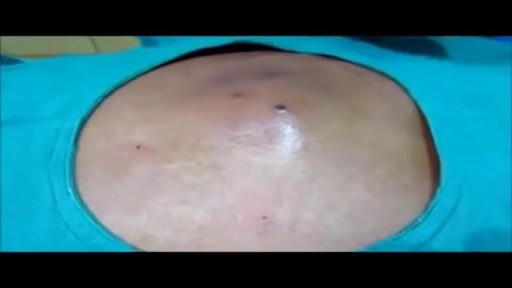
Tummy Tuck Marking before surgery
Tummy Tuck Surgery , Tummy Tuck Surgery Cost, Weight Loss with Tummy tuck surgery, tummy tuck surgery result , tummy tuck cost, Abdominoplasty
📞 Delhi - +91 8956880644 | Pune - +91 9222122122 | Bangalore- 8971224700 | Gurugram - 9272007896 | Ahmedabad - 9711162746
Subscribe to our Channel https://www.youtube.com/dezireclinic
💸Cost: call for free consultation | Zero % interest finance options
Subscribe on YouTube : https://youtube.com/dezireplas....ticsurgerycenter?sub
Subscribe on YouTube https://youtube.com/dezireclin....ic?sub_confirmation=
📸 https://www.instagram.com/drprashantdezireclinic/
🌐 http://dezireclinic.in/
Facebook: https://www.facebook.com/drprashantmch/
Twitter: https://twitter.com/drprashantmch
Email: dezireclinicindia@gmail.com
WHY choose Dezire plastic surgery center?
We are leading cosmetic surgery centre in India leading by Dr Prashant Yadav . See hundreds of various cosmetic surgery and real feedback videos. Watch live surgery to gain confidence before deciding surgery
Dr. Prashant Yadav
M.S., M.Ch. (Plastic & Cosmetic Surgery)
#plasticsurgery #cosmeticsurgery #dezireclinicindia #drprashantyadav #dezireplasticsurgerycenter
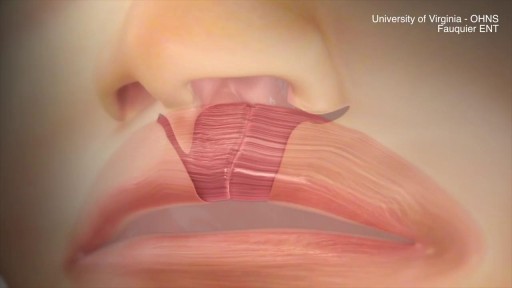
This animation demonstrates how a unilateral complete cleft lip repair is performed. This video is meant for educational purposes for patients and families. There are many ways to fix a complete cleft lip, but the technique shown here is the most common known as the Millard Rotation Advancement Repair.