Top videos

A tummy tuck is a surgical process that removes excess fat and skin. Learn more about the procedure by watching this video!
Looking to book a consultation? Call Zuri Plastic Surgery now at 786-804-1603 or DM us today to schedule a complimentary consultation with Dr. Z.
Un tummy tuck es un procedimiento quirúrgico que elimina el exceso de grasa y piel. ¡Aprenda más sobre este procedimiento viendo este video!
¿Quiere agendar una consulta? Llame a Zuri Plastic Surgery ahora al 786-804-1603 o envíenos un DM hoy para programar una consulta gratuita con el Dr. Z.

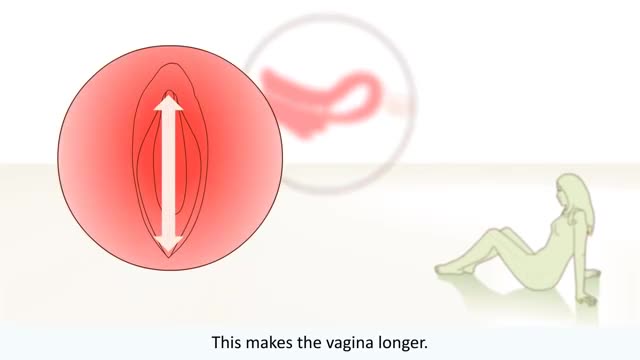
A Pap smear (Papanicolau smear; also known as the Pap test) is a screening test for cervical cancer. The test itself involves collection of a sample of cells from a woman's cervix (the end of the uterus that extends into the vagina) during a routine pelvic exam

This is how Paraumbilical hernia looks like and how it is examined although it looks very simple but in exam it can be very difficult to perform all steps in small amount of time. This can be short case or even long of #cpsp #fcps #mbbs #medicalstudent #mbbsexams #plab2 #plab #plab1 and MS #genernalknowledge #surgery exams
#para-umbilical hernia
#umbilical hernia #paraumbilical #hernia repair#laparoscopic paraumbilical hernia repair. #umbilical defect, #vetral hernia surgery. #herniatreatment #herniatreatment #ventral hernia hernia,#laparoscopic ventral hernia repair,umbilicus,carl lowe jr,hernia repair,training,north carolina,hernia repair surgery,charlotte,operation,laparoscopic,bulge,surgery,surgeon,dr. lowe,ipom repair,live surgery,mesh,
#mesh #ipom repair

Morning erections have colloquially been termed as “morning wood” while scientifically it is called nocturnal penile tumescence. It is a normal and healthy physiological reaction and response that most men experience in their lives. Morning erections are really the ending of a series of erections that happen to men during the night. Healthy men can, on average, have anywhere between three to five erections in a full night of sleep, each of which lasts from 25-35 minutes.

This 3D animation of brain surgery, shows how a ventriculostomy is performed, which is a neurosurgical procedure of creating a hole within a cerebral ventricle for drainage. It is most commonly performed on those with hydrocephalus, an abnormal buildup of fluid in the ventricles (cavities) deep within the brain. It's done by surgically penetrating the skull, dura mater, and brain such that the ventricular system ventricle of the brain is accessed.
When catheter drainage is temporary, it is commonly referred to as an external ventricular drain (EVD). When catheter drainage is permanent, it is usually referred to as a shunt.
There are many catheter-based ventricular shunts that are named for where they terminate, for example, a ventriculi-peritoneal shunt terminates in the peritoneal cavity, a ventriculoarterial shunt terminates within the atrium of the heart, etc. The most common entry point on the skull is called Kocher's point. An EVD ventriculostomy is done primarily to monitor the intracranial pressure as well as to drain cerebrospinal fluid (CSF), primarily, or blood to relieve pressure from the central nervous system (CNS).
For more information about custom medical animation, please visit https://www.amerra.com/.
Watch additional medical animations:
Craniectomy brain surgery - 3D animation: https://youtu.be/1RkseDeYS9g
Accessing an implantable port training - 3D animation: https://youtu.be/xSTpxjyv4O4
Open Suctioning with a Tracheostomy Tube - 3D animation: https://youtu.be/wamB7jpWCiQ
Suctioning the endotracheal tube - medical animation: https://youtu.be/pN6-EYoeh3g
Functional endoscopic sinus surgery (FESS) - 3D animation: https://youtu.be/qKTRyowwaLA
How to insert a nasogastric tube for NG intubation - 3d animation: https://youtu.be/Abf3Gd6AaZQ
Oral airway insertion - oropharyngeal airway technique - 3D animation: https://youtu.be/caxUdNwjt34
Nasotracheal suctioning (NTS) - 3D animation: https://youtu.be/979jWMsF62c
Learn about hemorrhoids with #3d #animation: https://youtu.be/R6NqlMpsiiY
LASIK eye surgery - 3D animation: https://youtu.be/Bb8bnjnEM00
CPR cardiopulmonary resuscitation - 3D animation: https://youtu.be/G87knTZnhks
What are warts (HPV)? - 3D animation: https://youtu.be/guJ1J7rRs1w
How Macular Degeneration Affects Your Vision - 3D animation: https://youtu.be/ozZQIZ_52YY
NeoGraft hair transplant procedure – animation: https://youtu.be/C-eTdH2UPXI

Renal artery stenosis is the narrowing of one or more arteries that carry blood to your kidneys (renal arteries). Narrowing of the arteries prevents normal amounts of oxygen-rich blood from reaching your kidneys. Your kidneys need adequate blood flow to help filter waste products and remove excess fluids. Reduced blood flow may increase blood pressure in your whole body (systemic blood pressure) and injure kidney tissue.
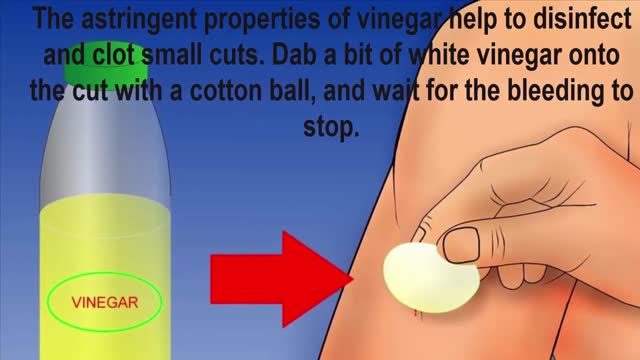
Injuries and certain medical conditions can result in bleeding. This can trigger anxiety and fear, but bleeding has a healing purpose. Still, you need to understand how to treat common bleeding incidents, like cuts and bloody noses, as well as when to seek medical help.

The Epley Maneuver for Vertigo can be very effective at relieving vertigo symptoms, but it’s a procedure that should be performed by a physical therapist or other health care professional. This video is for demonstration purposes only. See Doctor Jo’s blog post about the Epley
Screening is looking for cancer before a person has any symptoms. This can help find cancer at an early stage when it may be easier to treat. Lung cancer may have spread by the time a person has symptoms. One reason lung cancer is so serious is because it usually is not found until it has spread and is more difficult to treat. Screening may provide new hope for early detection and treatment of lung cancer. Scientists study screening tests to find those with the fewest risks and most benefits. They look at results over time to see if finding the cancer early decreases a person's chance of dying from the disease.
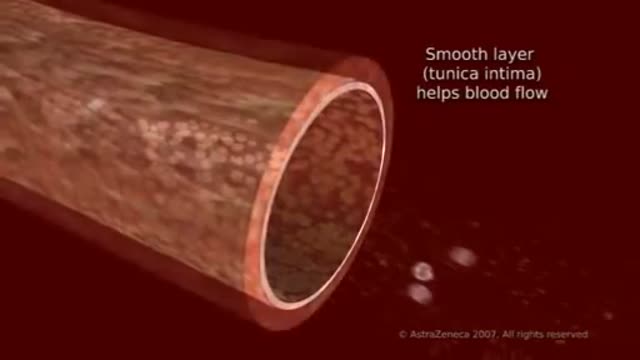
To understand high blood cholesterol (ko-LES-ter-ol), it helps to learn about cholesterol. Cholesterol is a waxy, fat-like substance that’s found in all cells of the body. Your body needs some cholesterol to make hormones, vitamin D, and substances that help you digest foods. Your body makes all the cholesterol it needs. However, cholesterol also is found in some of the foods you eat. Cholesterol travels through your bloodstream in small packages called lipoproteins (lip-o-PRO-teens). These packages are made of fat (lipid) on the inside and proteins on the outside. Two kinds of lipoproteins carry cholesterol throughout your body: low-density lipoproteins (LDL) and high-density lipoproteins (HDL). Having healthy levels of both types of lipoproteins is important. LDL cholesterol sometimes is called “bad” cholesterol. A high LDL level leads to a buildup of cholesterol in your arteries. (Arteries are blood vessels that carry blood from your heart to your body.) HDL cholesterol sometimes is called “good” cholesterol. This is because it carries cholesterol from other parts of your body back to your liver. Your liver removes the cholesterol from your body.

Varicose veins are caused by weakened valves and veins in your legs. Normally, one-way valves in your veins keep blood flowing from your legs up toward your heart. When these valves do not work as they should, blood collects in your legs, and pressure builds up. The veins become weak, large, and twisted.
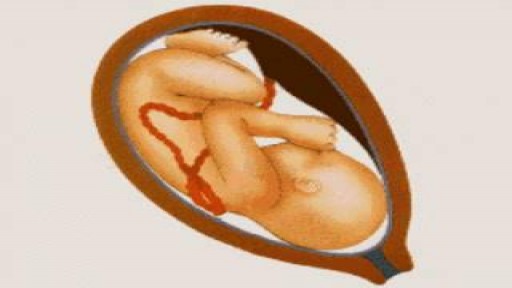
This video: Patent ductus arteriosus (PDA) is a persistent opening between two major blood vessels leading from the heart. The opening, called the ductus arteriosus, is a normal part of a baby's circulatory system before birth that usually closes shortly after birth. If it remains open, however, it's called a patent ductus arteriosus. A small patent ductus arteriosus often doesn't cause problems and might never need treatment. However, a large patent ductus arteriosus left untreated can allow poorly oxygenated blood to flow in the wrong direction, weakening the heart muscle and causing heart failure and other complications. Treatment options for a patent ductus arteriosus include monitoring, medications and closure by cardiac catheterization or surgery.

During the examination, the doctor gently puts a lubricated, gloved finger of one hand into the rectum. He or she may use the other hand to press on the lower belly or pelvic area. A digital rectal exam is done for men as part of a complete physical examination to check the prostate gland .

Patient Greg Grindley communicates with host Bryant Gumbel and his wife for the first time while undergoing deep brain stimulation surgery at University Hospital's Case Medical Center in Cleveland, Ohio.
➡ Subscribe: http://bit.ly/NatGeoSubscribe
About National Geographic:
National Geographic is the world's premium destination for science, exploration, and adventure. Through their world-class scientists, photographers, journalists, and filmmakers, Nat Geo gets you closer to the stories that matter and past the edge of what's possible.
Get More National Geographic:
Official Site: http://bit.ly/NatGeoOfficialSite
Facebook: http://bit.ly/FBNatGeo
Twitter: http://bit.ly/NatGeoTwitter
Instagram: http://bit.ly/NatGeoInsta
Greg's First In-Surgery Conversation | Brain Surgery Live
https://youtu.be/zvqV_2zncNU
National Geographic
https://www.youtube.com/natgeo
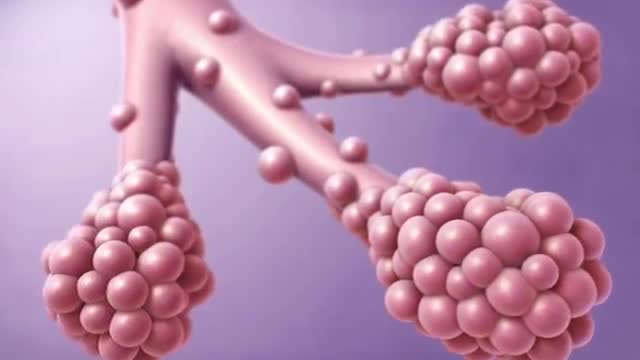
Idiopathic pulmonary fibrosis (IPF) is defined as a specific form of chronic, progressive fibrosing interstitial pneumonia of unknown cause, primarily occurring in older adults, limited to the lungs, and associated with the histopathologic and/or radiologic pattern of usual interstitial pneumonia (UIP).[1] Signs and symptoms The clinical symptoms of idiopathic pulmonary fibrosis are nonspecific and can be shared with many pulmonary and cardiac diseases. Most patients present with a gradual onset (often >6 mo) of exertional dyspnea and/or a nonproductive cough. Approximately 5% of patients have no presenting symptoms when idiopathic pulmonary fibrosis is serendipitously diagnosed.